Get your patient on Albuterol Sulfate - Albuterol Sulfate solution (Albuterol Sulfate)
Albuterol Sulfate - Albuterol Sulfate solution prescribing information
INDICATIONS AND USAGE
Albuterol inhalation solution is indicated for the relief of bronchospasm in patients 2 years of age and older with reversible obstructive airway disease and acute attacks of bronchospasm.
DOSAGE AND ADMINISTRATION
Adults and Children 2 to 12 Years of Age: The usual dosage for adults and for children weighing at least 15 kg is 2.5 mg of albuterol (one vial) administered three to four times daily by nebulization.
Children weighing < 15 kg who require < 2.5 mg/dose (i.e., less than a full vial) should use albuterol inhalation solution, 0.5% instead of albuterol inhalation solution, 0.083%. More frequent administration or higher doses are not recommended. To administer 2.5 mg of albuterol, administer the entire contents of one sterile unit-dose vial (3 mL of 0.083% inhalation solution) by nebulization. The flow rate is regulated to suit the particular nebulizer so that albuterol inhalation solution will be delivered over approximately 5 to 15 minutes.
The use of albuterol inhalation solution can be continued as medically indicated to control recurring bouts of bronchospasm. During this time most patients gain optimum benefit from regular use of the inhalation solution.
If a previously effective dosage regimen fails to provide the usual relief, medical advice should be sought immediately, as this is often a sign of seriously worsening asthma that would require reassessment of therapy.
CONTRAINDICATIONS
Albuterol inhalation solution is contraindicated in patients with a history of hypersensitivity to any of its components.
ADVERSE REACTIONS
The results of clinical trials with albuterol inhalation solution in 135 patients showed the following side effects which were considered probably or possibly drug related:
Central Nervous System: tremors (20%), dizziness (7%), nervousness (4%), headache (3%), insomnia (1%).
Gastrointestinal: nausea (4%), dyspepsia (1%).
Ear, Nose and Throat: pharyngitis (<1%), nasal congestion (1%).
Cardiovascular: tachycardia (1%), hypertension (1%).
Respiratory: bronchospasm (8%), cough (4%), bronchitis (4%), wheezing (1%).
No clinically relevant laboratory abnormalities related to albuterol inhalation solution administration were determined in these studies.
In comparing the adverse reactions reported for patients treated with albuterol inhalation solution with those of patients treated with isoproterenol during clinical trials of three months, the following moderate to severe reactions, as judged by the investigators, were reported. This table does not include mild reactions.
| Reaction | Albuterol N=65 | Isoproterenol N=65 |
| Central Nervous System | ||
| Tremors | 10.7% | 13.8% |
| Headache | 3.1% | 1.5% |
| Insomnia | 3.1% | 1.5% |
| Cardiovascular | ||
| Hypertension | 3.1% | 3.1% |
| Arrhythmias | 0% | 3% |
| •Palpitation | 0% | 22% |
| Respiratory | ||
| +Bronchospasm | 15.4% | 18% |
| Cough | 3.1% | 5% |
| Bronchitis | 1.5% | 5% |
| Wheeze | 1.5% | 1.5% |
| Sputum Increase | 1.5% | 1.5% |
| Dyspnea | 1.5% | 1.5% |
| Gastrointestinal | ||
| Nausea | 3.1% | 0% |
| Dyspepsia | 1.5% | 0% |
| Systemic | ||
| Malaise | 1.5% | 0% |
•The finding of no arrhythmias and no palpitations after albuterol administration in the clinical study should not be interpreted as indicating that these adverse effects cannot occur after the administration of inhaled albuterol.
+In most cases of bronchospasm, this term was generally used to describe exacerbations in the underlying pulmonary disease. Cases of urticaria, angioedema, rash, bronchospasm, hoarseness, oropharyngeal edema, arrhythmias (including atrial fibrillations, supraventricular tachycardia, extrasystoles) have been reported after the use of albuterol inhalation solution.
Drug Interactions
Other sympathomimetic aerosol bronchodilators or epinephrine should not be used concomitantly with albuterol.
Albuterol should be administered with extreme caution to patients being treated with monoamine oxidase inhibitors or tricyclic antidepressants, since the action of albuterol on the vascular system may be potentiated.
Beta-receptor blocking agents and albuterol inhibit the effect of each other.
DESCRIPTION
Albuterol inhalation solution, USP is a relatively selective beta 2 -adrenergic bronchodilator (see CLINICAL PHARMACOLOGY section below). Albuterol sulfate USP, the racemic form of albuterol, has the chemical name α 1 -[( tert -Butylamino)methyl]-4-hydroxy- m -xylene-α,α′-diol sulfate (2:1) (salt) and the following structural formula:
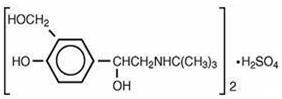
Albuterol sulfate has a molecular weight of 576.7, and the molecular formula is (C 13 H 21 NO 3 ) 2 • H 2 SO 4 . Albuterol sulfate, USP is a white or practically white powder, freely soluble in water and slightly soluble in alcohol. The World Health Organization’s recommended name for albuterol base is salbutamol. Albuterol inhalation solution, USP 0.083% requires no dilution before administration.
Each mL of albuterol inhalation solution, USP (0.083%) contains 0.83 mg of albuterol (as 1 mg of albuterol sulfate USP) in an isotonic, sterile, aqueous solution containing sodium chloride; sulfuric acid is used to adjust the pH to between 3 and 5. Albuterol inhalation solution, USP (0.083%) contains no sulfiting agents. Albuterol inhalation solution, USP is a clear, colorless to light yellow solution.
CLINICAL PHARMACOLOGY
The prime action of beta-adrenergic drugs is to stimulate adenyl cyclase, the enzyme which catalyzes the formation of cyclic-3',5'-adenosine monophosphate (cyclic AMP) from adenosine triphosphate (ATP). The cyclic AMP thus formed mediates the cellular responses.
In vitro studies and in vivo pharmacologic studies have demonstrated that albuterol has a preferential effect on beta 2 -adrenergic receptors compared with isoproterenol. While it is recognized that beta 2 -adrenergic receptors are the predominant receptors in bronchial smooth muscle, data indicate that 10% to 50% of the beta-receptors in the human heart may be beta 2 -receptors. The precise function of these receptors, however, is not yet established.
Albuterol has been shown in most controlled clinical trials to have more effect on the respiratory tract in the form of bronchial smooth muscle relaxation than isoproterenol at comparable doses while producing fewer cardiovascular effects.
Controlled clinical studies and other clinical experience have shown that inhaled albuterol, like other beta-adrenergic agonist drugs, can produce a significant cardiovascular effect in some patients, as measured by pulse rate, blood pressure, symptoms, and/or electrocardiographic changes. Albuterol is longer acting than isoproterenol in most patients by any route of administration because it is not a substrate for the cellular uptake processes for catecholamines nor for catechol- O -methyl transferase.
Studies in asthmatic patients have shown that less than 20% of a single albuterol dose was absorbed following either IPPB (intermittent positive-pressure breathing) or nebulizer administration; the remaining amount was recovered from the nebulizer and apparatus and expired air. Most of the absorbed dose was recovered in the urine 24 hours after drug administration. Following a 3 mg dose of nebulized albuterol, the maximum albuterol plasma level at 0.5 hours was 2.1 ng/mL (range, 1.4 to 3.2 ng/mL). There was a significant dose-related response in FEV 1 (forced expiratory volume in one second) and peak flow rate. It has been demonstrated that following oral administration of 4 mg of albuterol, the elimination half-life was five to six hours.
Animal studies show that albuterol does not pass the blood-brain barrier. Recent studies in laboratory animals (minipigs, rodents, and dogs) recorded the occurrence of cardiac arrhythmias and sudden death (with histologic evidence of myocardial necrosis) when beta-agonists and methylxanthines were administered concurrently. The significance of these findings when applied to humans is currently unknown.
In controlled clinical trials, most patients exhibited an onset of improvement in pulmonary function within 5 minutes as determined by FEV 1 . FEV 1 measurements also showed that the maximum average improvement in pulmonary function usually occurred at approximately 1 hour following inhalation of 2.5 mg of albuterol by compressor-nebulizer and remained close to peak for 2 hours. Clinically significant improvement in pulmonary function (defined as maintenance of a 15% or more increase in FEV 1 over baseline values) continued for 3 to 4 hours in most patients and in some patients continued up to 6 hours.
In repetitive dose studies, continued effectiveness was demonstrated throughout the three-month period of treatment in some patients.
Published reports of trials in asthmatic children aged 3 years or older have demonstrated significant improvement in either FEV 1 or PEFR within 2 to 20 minutes following a single dose of albuterol inhalation solution. An increase of 15% or more in baseline FEV 1 has been observed in children aged 5 to 11 years up to 6 hours after treatment with doses of 0.10 mg/kg or higher of albuterol inhalation solution. Single doses of 3, 4, or 10 mg resulted in improvement in baseline PEFR that was comparable in extent and duration to a 2 mg dose, but doses above 3 mg were associated with heart rate increases of more than 10%.
HOW SUPPLIED
Albuterol Inhalation Solution, USP 0.083% is contained in plastic, sterile, unit dose vials of 3 mL each, supplied in foil pouches:
NDC 0487-9501-25: carton of 25 vials
NDC 0487-9501-03: carton of 30 vials
NDC 0487-9501-60: carton of 60 vials
NDC 0487-9501-01: 30 vials, each in an individual foil pouch.
Storage and Handling
PROTECT FROM LIGHT. Store vials in pouch until time of use. Store between 20°C to 25° C (68°F to 77° F), excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Rx Only
Manufactured By:
Nephron Pharmaceuticals Corporation
West Columbia, SC 29172
For Customer Service,
Call 1-800-443-4313
INSTRUCTIONS FOR USE
- Remove vial from the foil pouch.
- Twist the cap completely off the vial and squeeze the contents into the nebulizer reservoir (Figure 1).
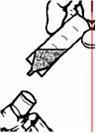
- Connect the nebulizer reservoir to the mouthpiece or face mask (Figure 2).
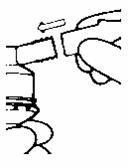
- Connect the nebulizer to the compressor.
- Sit in a comfortable, upright position; place the mouthpiece in your mouth (Figure 3)(or put on the face mask); and turn on the compressor.
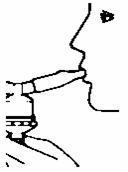
- Breathe as calmly, deeply and evenly as possible until no more mist is formed in the nebulizer chamber (about 5 to 15 minutes). At this point, the treatment is finished.
- Clean the nebulizer (see manufacturer’s instructions).
Note: Use only as directed by your physician. More frequent administration or higher doses are not recommended.
Store Albuterol Inhalation Solution, USP 0.083%• between 20°C to 25° C (68°F to 77° F) [see USP Controlled Room Temperature].
• Potency expressed as albuterol