Get your patient on Ancobon - Flucytosine capsule (Flucytosine)
Ancobon - Flucytosine capsule prescribing information
WARNING
Use with extreme caution in patients with impaired renal function. Close monitoring of hematologic, renal and hepatic status of all patients is essential. These instructions should be thoroughly reviewed before administration of ANCOBON.
INDICATIONS AND USAGE
ANCOBON is indicated only in the treatment of serious infections caused by susceptible strains of Candida and/or Cryptococcus .
Candida: Septicemia, endocarditis and urinary system infections have been effectively treated with flucytosine. Limited trials in pulmonary infections justify the use of flucytosine.
Cryptococcus: Meningitis and pulmonary infections have been treated effectively. Studies in septicemias and urinary tract infections are limited, but good responses have been reported.
ANCOBON should be used in combination with amphotericin B for the treatment of systemic candidiasis and cryptococcosis because of the emergence of resistance to ANCOBON (see MICROBIOLOGY ).
DOSAGE AND ADMINISTRATION
The usual dosage of ANCOBON is 50 to 150 mg/kg/day administered in divided doses at 6-hour intervals. Nausea or vomiting may be reduced or avoided if the capsules are given a few at a time over a 15-minute period. If the BUN or the serum creatinine is elevated, or if there are other signs of renal impairment, the initial dose should be at the lower level (see WARNINGS ).
ANCOBON should be used in combination with amphotericin B for the treatment of systemic candidiasis and cryptococcosis because of the emergence of resistance to ANCOBON (see MICROBIOLOGY ).
CONTRAINDICATIONS
ANCOBON is contraindicated in patients with a known hypersensitivity to the drug.
ANCOBON is contraindicated in patients with known complete dihydropyrimidine dehydrogenase (DPD) enzyme deficiency (see WARNINGS ).
ADVERSE REACTIONS
The adverse reactions which have occurred during treatment with ANCOBON are grouped according to organ system affected.
Cardiovascular: Cardiac arrest, myocardial toxicity, ventricular dysfunction.
Respiratory: Respiratory arrest, chest pain, dyspnea.
Dermatologic: Rash, pruritus, urticaria, photosensitivity.
Gastrointestinal: Nausea, emesis, abdominal pain, diarrhea, anorexia, dry mouth, duodenal ulcer, gastrointestinal hemorrhage, acute hepatic injury including hepatic necrosis with possible fatal outcome in debilitated patients, hepatic dysfunction, jaundice, ulcerative colitis, enterocolitis, bilirubin elevation, increased hepatic enzymes.
Genitourinary: Azotemia, creatinine and BUN elevation, crystalluria, renal failure.
Hematologic: Anemia, agranulocytosis, aplastic anemia, eosinophilia, leukopenia, pancytopenia, thrombocytopenia, and fatal cases of bone marrow aplasia.
Neurologic: Ataxia, hearing loss, headache, paresthesia, parkinsonism, peripheral neuropathy, pyrexia, vertigo, sedation, convulsions.
Psychiatric: Confusion, hallucinations, psychosis.
Miscellaneous: Fatigue, hypoglycemia, hypokalemia, weakness, allergic reactions, Lyell’s syndrome.
To report SUSPECTED ADVERSE REACTIONS, contact Bausch Health US, LLC at 1-800-321-4576 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
Cytosine arabinoside, a cytostatic agent, has been reported to inactivate the antifungal activity of ANCOBON by competitive inhibition. Drugs which impair glomerular filtration may prolong the biological half-life of flucytosine.
DESCRIPTION
ANCOBON (flucytosine), an antifungal agent, is available as 250 mg and 500 mg capsules for oral administration. In addition to the active ingredient of flucytosine, each capsule contains corn starch, lactose and talc. The 250 mg capsule shell contains black iron oxide, D&C Yellow No. 10, FD&C Blue No. 1, FD&C Yellow No. 6, gelatin and titanium dioxide. The 500 mg capsule shell contains black iron oxide, gelatin and titanium dioxide.
Chemically, flucytosine is 5-fluorocytosine, a fluorinated pyrimidine which is related to fluorouracil and floxuridine. It is a white to off-white crystalline powder with a molecular weight of 129.09 and the following structural formula:
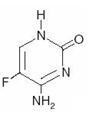
CLINICAL PHARMACOLOGY
Flucytosine is rapidly and virtually completely absorbed following oral administration. ANCOBON is not metabolized significantly when given orally to man. Bioavailability estimated by comparing the area under the curve of serum concentrations after oral and intravenous administration showed 78% to 89% absorption of the oral dose. Peak serum concentrations of 30 to 40 mcg/mL were reached within 2 hours of administration of a 2 g oral dose to normal subjects. Other studies revealed mean serum concentrations of approximately 70 to 80 mcg/mL 1 to 2 hours after a dose in patients with normal renal function receiving a 6-week regimen of flucytosine (150 mg/kg/day given in divided doses every 6 hours) in combination with amphotericin B. The half-life in the majority of healthy subjects ranged between 2.4 and 4.8 hours. Flucytosine is excreted via the kidneys by means of glomerular filtration without significant tubular reabsorption. More than 90% of the total radioactivity after oral administration was recovered in the urine as intact drug. Flucytosine is deaminated (probably by gut bacteria) to 5-fluorouracil. The area under the curve (AUC) ratio of 5-fluorouracil to flucytosine is 4%. Approximately 1% of the dose is present in the urine as the α-fluoro-β-ureido-propionic acid metabolite. A small portion of the dose is excreted in the feces.
The half-life of flucytosine is prolonged in patients with renal insufficiency; the average half-life in nephrectomized or anuric patients was 85 hours (range: 29.9 to 250 hours). A linear correlation was found between the elimination rate constant of flucytosine and creatinine clearance.
In vitro studies have shown that 2.9% to 4% of flucytosine is protein-bound over the range of therapeutic concentrations found in the blood. Flucytosine readily penetrates the blood-brain barrier, achieving clinically significant concentrations in cerebrospinal fluid.
Pharmacokinetics in Pediatric Patients
Limited data are available regarding the pharmacokinetics of ANCOBON administered to neonatal patients being treated for systemic candidiasis. After five days of continuous therapy, median peak levels in infants were 19.6 mcg/mL, 27.7 mcg/mL, and 83.9 mcg/mL at doses of 25 mg/kg (N=3), 50 mg/kg (N=4), and 100 mg/kg (N=3), respectively. Mean time to peak serum levels was of 2.5 ± 1.3 hours, similar to that observed in adult patients. A good deal of interindividual variability was noted, which did not correlate with gestational age. Some patients had serum levels > 100 mcg/mL, suggesting a need for drug level monitoring during therapy. In another study, serum concentrations were determined during flucytosine therapy in two patients (total assays performed =10). Median serum flucytosine concentrations at steady state were calculated to be 57 ± 10 mcg/mL (doses of 50 to 125 mg/kg/day, normalized to 25 mg/kg per dose for comparison). In three infants receiving flucytosine 25 mg/kg/day (four divided doses), a median flucytosine half-life of 7.4 hours was observed, approximately double that seen in adult patients. The concentration of flucytosine in the cerebrospinal fluid of one infant was 43 mcg/mL 3 hours after a 25 mg oral dose, and ranged from 20 to 67 mg/L in another neonate receiving oral doses of 120 to 150 mg/kg/day.
MICROBIOLOGY
Mechanism of Action
Flucytosine is taken up by fungal organisms via the enzyme cytosine permease. Inside the fungal cell, flucytosine is rapidly converted to fluorouracil by the enzyme cytosine deaminase. Fluorouracil exerts its antifungal activity through the subsequent conversion into several active metabolites, which inhibit protein synthesis by being falsely incorporated into fungal RNA or interfere with the biosynthesis of fungal DNA through the inhibition of the enzyme thymidylate synthetase.
Activity In Vitro
Flucytosine has been shown to be active against most strains of the following microorganisms both in vitro and in clinical infections.
Candida albicans
Cryptococcus neoformans
Susceptibility Testing
For specific information regarding susceptibility test interpretive criteria and associated test methods and quality control standards recognized by FDA for this drug, please see: https://www.fda.gov/STIC .
Drug Resistance
Flucytosine resistance may arise from a mutation of an enzyme necessary for the cellular uptake or metabolism of flucytosine or from an increased synthesis of pyrimidines, which compete with the active metabolites of flucytosine (fluorinated antimetabolites). Resistance to flucytosine has been shown to develop during monotherapy after prolonged exposure to the drug.
Drug Combination
Antifungal synergism between flucytosine and polyene antibiotics, particularly amphotericin B has been reported in vitro. ANCOBON is usually administered in combination with amphotericin B due to lack of cross-resistance and reported synergistic activity of both drugs.
HOW SUPPLIED ANCOBON ® (flucytosine) Capsules are supplied as capsules containing 250 mg and 500 mg flucytosine as follows:
NDC | Strength | Package Configuration | Description |
0187‑3554‑10 | 250 mg | Bottles of 100 | Gray and green capsules imprinted with “ANCOBON ® 250 ICN” |
0187‑3555‑10 | 500 mg | Bottles of 100 | Gray and white capsules imprinted with “ANCOBON ® 500 ICN” |
- Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F).
Distributed by:
Bausch Health US, LLC
Bridgewater, NJ 08807 USA
Manufactured by:
Bausch Health Companies Inc.
Steinbach, MB R5G 1Z7, Canada
ANCOBON is a trademark of Bausch Health Companies Inc. or its affiliates.
© 2022 Bausch Health Companies Inc. or its affiliates
Rev. 02/2022 9578603 20005061
Ancobon - Flucytosine capsule PubMed™ news
- Journal Article • 2026 MayEvaluation of Sensititre YeastOne for antifungal susceptibility testing of Candida (Candidozyma) auris: misclassification of FKS1 mutants and overestimation of caspofungin resistance in a global collection of isolates.
- Journal Article • 2026 MayPhenotypic and Molecular Characterization of Naganishia uzbekistanensis: Diagnostic Challenges and Antifungal Resistance Profile.
- Journal Article • 2026 AprEpidemiology, clinical and microbiologic aspects of Rhodotorula fungemia: A review of reported cases over the past 16 years.
- Journal Article • 2026 AprCandida urinary tract infections, antifungal susceptibility and factors associated with candiduria among pregnant women seeking antenatal care at Murang'a County Referral Hospital, Kenya.
- Journal Article • 2026 AprRefractory Candidozyma (Candida) auris-associated central nervous system infection in a postoperative neurosurgical patient.