Get your patient on Bisoprolol Fumarate - Bisoprolol Fumarate tablet, Film Coated (Bisoprolol Fumarate)
Bisoprolol Fumarate - Bisoprolol Fumarate tablet, Film Coated prescribing information
INDICATIONS AND USAGE
Bisoprolol fumarate is indicated in the management of hypertension. It may be used alone or in combination with other antihypertensive agents.
DOSAGE AND ADMINISTRATION
The dose of bisoprolol fumarate must be individualized to the needs of the patient. The usual starting dose is 5 mg once daily. In some patients, 2.5 mg may be an appropriate starting dose (see Bronchospastic Disease in WARNINGS ). If the antihypertensive effect of 5 mg is inadequate, the dose may be increased to 10 mg and then, if necessary, to 20 mg once daily. Patients with Renal or Hepatic Impairment In patients with hepatic impairment (hepatitis or cirrhosis) or renal dysfunction (creatinine clearance less than 40 mL/min), the initial daily dose should be 2.5 mg and caution should be used in dose-titration. Since limited data suggest that bisoprolol fumarate is not dialyzable, drug replacement is not necessary in patients undergoing dialysis. Geriatric Patients It is not necessary to adjust the dose in the elderly, unless there is also significant renal or hepatic dysfunction (see above and Geriatric Use in PRECAUTIONS).
Pediatric Patients There is no pediatric experience with bisoprolol fumarate.
CONTRAINDICATIONS
Bisoprolol fumarate is contraindicated in patients with cardiogenic shock, overt cardiac failure, second or third degree AV block, and marked sinus bradycardia.
ADVERSE REACTIONS
Safety data are available in more than 30,000 patients or volunteers. Frequency estimates and rates of withdrawal of therapy for adverse events were derived from two U.S. placebo-controlled studies.
In Study A, doses of 5, 10, and 20 mg bisoprolol fumarate were administered for 4 weeks. In Study B, doses of 2.5, 10, and 40 mg of bisoprolol fumarate were administered for 12 weeks. A total of 273 patients were treated with 5 to 20 mg of bisoprolol fumarate; 132 received placebo. Withdrawal of therapy for adverse events was 3.3% for patients receiving bisoprolol fumarate and 6.8% for patients on placebo. Withdrawals were less than 1% for either bradycardia or fatigue/lack of energy.
The following table presents adverse experiences, whether or not considered drug related, reported in at least 1% of patients in these studies, for all patients studied in placebo-controlled clinical trials (2.5 to 40 mg), as well as for a subgroup that was treated with doses within the recommended dosage range (5 to 20 mg). Of the adverse events listed in the table, bradycardia, diarrhea, asthenia, fatigue, and sinusitis appear to be dose related.
| Body System/Adverse Experience | All Adverse Experiences (% a ) Bisoprolol fumarate | ||
| Placebo (n = 132) % | 5 to 20 mg (n = 273) % | 2.5 to 40 mg (n = 404) % | |
| Skin | |||
| increased sweating | 1.5 | 0.7 | 1.0 |
| Musculoskeletal | |||
| arthralgia | 2.3 | 2.2 | 2.7 |
| Central Nervous System | |||
| dizziness | 3.8 | 2.9 | 3.5 |
| headache | 11.4 | 8.8 | 10.9 |
| hypoaesthesia | 0.8 | 1.1 | 1.5 |
| Autonomic Nervous System | |||
| dry mouth | 1.5 | 0.7 | 1.3 |
| Heart Rate/Rhythm | |||
| bradycardia | 0 | 0.4 | 0.5 |
| Psychiatric | |||
| vivid dreams | 0 | 0 | 0 |
| insomnia | 2.3 | 1.5 | 2.5 |
| depression | 0.8 | 0 | 0.2 |
| Gastrointestinal | |||
| diarrhea | 1.5 | 2.6 | 3.5 |
| nausea | 1.5 | 1.5 | 2.2 |
| vomiting | 0 | 1.1 | 1.5 |
| Respiratory | |||
| bronchospasm | 0 | 0 | 0 |
| cough | 4.5 | 2.6 | 2.5 |
| dyspnea | 0.8 | 1.1 | 1.5 |
| pharyngitis | 2.3 | 2.2 | 2.2 |
| rhinitis | 3.0 | 2.9 | 4.0 |
| sinusitis | 1.5 | 2.2 | 2.2 |
| URI | 3.8 | 4.8 | 5.0 |
| Body as a Whole | |||
| asthenia | 0 | 0.4 | 1.5 |
| chest pain | 0.8 | 1.1 | 1.5 |
| fatigue | 1.5 | 6.6 | 8.2 |
| edema (peripheral) | 3.8 | 3.7 | 3.0 |
a percentage of patients with event
The following is a comprehensive list of adverse experiences reported with bisoprolol fumarate in worldwide studies, or in postmarketing experience (in italics): Central Nervous System Dizziness, unsteadiness, vertigo, syncope, headache, paresthesia, hypoesthesia, hyperesthesia, somnolence, sleep disturbances, anxiety/restlessness, decreased concentration/memory Autonomic Nervous System Dry mouth Cardiovascular Bradycardia, palpitations and other rhythm disturbances, cold extremities, claudication, hypotension, orthostatic hypotension, chest pain, congestive heart failure, dyspnea on exertion Psychiatric Vivid dreams, insomnia, depression. Gastrointestinal Gastric/epigastric/abdominal pain, gastritis, dyspepsia, nausea, vomiting, diarrhea, constipation, peptic ulcer Musculoskeletal Muscle/joint pain, arthralgia, back/neck pain, muscle cramps, twitching/tremor. Skin Rash, acne, eczema, psoriasis, skin irritation, pruritus, flushing, sweating, alopecia, dermatitis, angioedema, exfoliative dermatitis, cutaneous vasculitis Special Senses Visual disturbances, ocular pain/pressure, abnormal lacrimation, tinnitus, decreased hearing, earache, taste abnormalities. Metabolic Gout Respiratory Asthma/bronchospasm, bronchitis, coughing, dyspnea, pharyngitis, rhinitis, sinusitis, URI. Genitourinary Decreased libido/impotence, Peyronie’s disease, cystitis, renal colic, polyuria. Hematologic Purpura. General Fatigue, asthenia, chest pain, malaise, edema, weight gain, angioedema. In addition, a variety of adverse effects have been reported with other beta-adrenergic blocking agents and should be considered potential adverse effects of bisoprolol fumarate: Central Nervous System Reversible mental depression progressing to catatonia, hallucinations, an acute reversible syndrome characterized by disorientation to time and place, emotional lability, slightly clouded sensorium. Allergic Fever, combined with aching and sore throat, laryngospasm, respiratory distress. Hematologic Agranulocytosis, thrombocytopenia, thrombocytopenic purpura. Gastrointestinal Mesenteric arterial thrombosis, ischemic colitis. Miscellaneous The oculomucocutaneous syndrome associated with the beta-blocker practolol has not been reported with bisoprolol fumarate during investigational use or extensive foreign marketing experience. Laboratory Abnormalities In clinical trials, the most frequently reported laboratory change was an increase in serum triglycerides, but this was not a consistent finding. Sporadic liver test abnormalities have been reported. In the U.S. controlled trials experience with bisoprolol fumarate treatment for 4-12 weeks, the incidence of concomitant elevations in SGOT and SGPT from 1 to 2 times normal was 3.9%, compared to 2.5% for placebo. No patient had concomitant elevations greater than twice normal. In the long-term, uncontrolled experience with bisoprolol fumarate treatment for 6-18 months, the incidence of one or more concomitant elevations in SGOT and SGPT from 1 to 2 times normal was 6.2%. The incidence of multiple occurrences was 1.9%. For concomitant elevations in SGOT and SGPT of greater than twice normal, the incidence was 1.5%. The incidence of multiple occurrences was 0.3%. In many cases these elevations were attributed to underlying disorders, or resolved during continued treatment with bisoprolol fumarate. Other laboratory changes included small increases in uric acid, creatinine, BUN, serum potassium, glucose, and phosphorus and decreases in WBC and platelets. These were generally not of clinical importance and rarely resulted in discontinuation of bisoprolol fumarate. As with other beta-blockers, ANA conversions have also been reported on bisoprolol fumarate. About 15% of patients in long-term studies converted to a positive titer, although about one-third of these patients subsequently reconverted to a negative titer while on continued therapy.
Drug Interactions
Bisoprolol fumarate should not be combined with other beta-blocking agents. Patients receiving catecholamine-depleting drugs, such as reserpine or guanethidine, should be closely monitored, because the added beta-adrenergic blocking action of bisoprolol fumarate may produce excessive reduction of sympathetic activity. In patients receiving concurrent therapy with clonidine, if therapy is to be discontinued, it is suggested that bisoprolol fumarate be discontinued for several days before the withdrawal of clonidine. Bisoprolol fumarate should be used with care when myocardial depressants or inhibitors of AV conduction, such as certain calcium antagonists (particularly of the phenylalkylamine [verapamil] and benzothiazepine [diltiazem] classes), or antiarrhythmic agents, such as disopyramide, are used concurrently. Both digitalis glycosides and beta-blockers slow atrioventricular conduction and decrease heart rate. Concomitant use can increase the risk of bradycardia. Concurrent use of rifampin increases the metabolic clearance of bisoprolol fumarate, resulting in a shortened elimination half-life of bisoprolol fumarate. However, initial dose modification is generally not necessary. Pharmacokinetic studies document no clinically relevant interactions with other agents given concomitantly, including thiazide diuretics and cimetidine. There was no effect of bisoprolol fumarate on prothrombin time in patients on stable doses of warfarin. Risk of Anaphylactic Reaction: While taking beta-blockers, patients with a history of severe anaphylactic reaction to a variety of allergens may be more reactive to repeated challenge, either accidental, diagnostic, or therapeutic. Such patients may be unresponsive to the usual doses of epinephrine used to treat allergic reactions.
DESCRIPTION
Bisoprolol fumarate, USP is a synthetic, beta 1 -selective (cardioselective) adrenoceptor blocking agent. The chemical name for bisoprolol fumarate is (±)-1-[4-[[2-(1-Methylethoxy)ethoxy]methyl]phenoxy]-3-[(1-methylethyl)amino]-2-propanol (E)-2-butenedioate (2:1) (salt). It possesses an asymmetric carbon atom in its structure and is provided as a racemic mixture. The S(-) enantiomer is responsible for most of the beta-blocking activity. Its molecular formula is (C 18 H 31 NO 4 ) 2 •C 4 H 4 O 4 and its structure is:
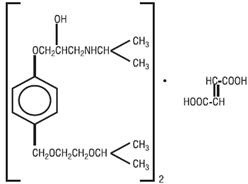
Bisoprolol fumarate has a molecular weight of 766.97. It is a white crystalline powder which is approximately equally hydrophilic and lipophilic, and is readily soluble in water, methanol, ethanol, and chloroform.
Bisoprolol fumarate tablets, USP are available as 5 and 10 mg tablets for oral administration.
Inactive ingredients include microcrystalline cellulose, butylated hydroxy anisole, dibasic calcium phosphate anhydrous, crospovidone, colloidal silicon dioxide, magnesium stearate, hypromellose, hydroxypropyl cellulose and titanium dioxide. The 5 mg tablets also contain talc, FD&C red#40 and FD&C blue #2. FDA approved dissolution test specifications differ from USP.
CLINICAL PHARMACOLOGY
Bisoprolol fumarate is a beta 1 -selective (cardioselective) adrenoceptor blocking agent without significant membrane stabilizing activity or intrinsic sympathomimetic activity in its therapeutic dosage range. Cardioselectivity is not absolute, however, and at higher doses (≥ 20 mg) bisoprolol fumarate also inhibits beta 2 -adrenoceptors, chiefly located in the bronchial and vascular musculature; to retain selectivity it is therefore important to use the lowest effective dose. Pharmacokinetics and Metabolism The absolute bioavailability after a 10 mg oral dose of bisoprolol fumarate is about 80%. Absorption is not affected by the presence of food. The first pass metabolism of bisoprolol fumarate is about 20%. Binding to serum proteins is approximately 30%. Peak plasma concentrations occur within 2-4 hours of dosing with 5 to 20 mg, and mean peak values range from 16 ng/mL at 5 mg to 70 ng/mL at 20 mg. Once daily dosing with bisoprolol fumarate results in less than twofold intersubject variation in peak plasma levels. The plasma elimination half-life is 9-12 hours and is slightly longer in elderly patients, in part because of decreased renal function in that population. Steady state is attained within 5 days of once daily dosing. In both young and elderly populations, plasma accumulation is low; the accumulation factor ranges from 1.1 to 1.3, and is what would be expected from the first order kinetics and once daily dosing. Plasma concentrations are proportional to the administered dose in the range of 5 to 20 mg. Pharmacokinetic characteristics of the two enantiomers are similar. Bisoprolol fumarate is eliminated equally by renal and non-renal pathways with about 50% of the dose appearing unchanged in the urine and the remainder appearing in the form of inactive metabolites. In humans, the known metabolites are labile or have no known pharmacologic activity. Less than 2% of the dose is excreted in the feces. Bisoprolol fumarate is not metabolized by cytochrome P450 II D6 (debrisoquin hydroxylase). In subjects with creatinine clearance less than 40 mL/min, the plasma half-life is increased approximately threefold compared to healthy subjects. In patients with cirrhosis of the liver, the elimination of bisoprolol fumarate is more variable in rate and significantly slower than that in healthy subjects, with plasma half-life ranging from 8.3 to 21.7 hours. Pharmacodynamics The most prominent effect of bisoprolol fumarate is the negative chronotropic effect, resulting in a reduction in resting and exercise heart rate. There is a fall in resting and exercise cardiac output with little observed change in stroke volume, and only a small increase in right atrial pressure, or pulmonary capillary wedge pressure at rest or during exercise. Findings in short-term clinical hemodynamics studies with bisoprolol fumarate are similar to those observed with other beta-blocking agents. The mechanism of action of its antihypertensive effects has not been completely established. Factors which may be involved include: 1. Decreased cardiac output, 2. Inhibition of renin release by the kidneys, 3. Diminution of tonic sympathetic outflow from the vasomotor centers in the brain. In normal volunteers, bisoprolol fumarate therapy resulted in a reduction of exercise- and isoproterenol-induced tachycardia. The maximal effect occurred within 1-4 hours post-dosing. Effects persisted for 24 hours at doses equal to or greater than 5 mg. Electrophysiology studies in man have demonstrated that bisoprolol fumarate significantly decreases heart rate, increases sinus node recovery time, prolongs AV node refractory periods, and, with rapid atrial stimulation, prolongs AV nodal conduction. Beta 1 -selectivity of bisoprolol fumarate has been demonstrated in both animal and human studies. No effects at therapeutic doses on beta 2 -adrenoceptor density have been observed. Pulmonary function studies have been conducted in healthy volunteers, asthmatics, and patients with chronic obstructive pulmonary disease (COPD). Doses of bisoprolol fumarate ranged from 5 to 60 mg, atenolol from 50 to 200 mg, metoprolol from 100 to 200 mg, and propranolol from 40 to 80 mg. In some studies, slight, asymptomatic increases in airways resistance (AWR) and decreases in forced expiratory volume (FEV 1 ) were observed with doses of bisoprolol fumarate 20 mg and higher, similar to the small increases in AWR also noted with the other cardioselective beta-blockers. The changes induced by beta-blockade with all agents were reversed by bronchodilator therapy. Bisoprolol fumarate had minimal effect on serum lipids during antihypertensive studies. In U.S. placebo-controlled trials, changes in total cholesterol averaged +0.8% for bisoprolol fumarate-treated patients, and +0.7% for placebo. Changes in triglycerides averaged +19% for bisoprolol fumarate-treated patients, and +17% for placebo.
Bisoprolol fumarate has also been given concomitantly with thiazide diuretics. Even very low doses of hydrochlorothiazide (6.25 mg) were found to be additive with bisoprolol fumarate in lowering blood pressure in patients with mild-to-moderate hypertension.
HOW SUPPLIED
Bisoprolol fumarate is supplied as 5 mg and 10 mg tablets. The 5 mg tablet is pinkish purple to purple colored, round, biconvex, film-coated tablets, debossed with “H14” on one side and functional scoring on other side. Tablets shall be free from physical defects. Bottles of 30 Unit-of-use: NDC 70095-020-01 Bottles of 100: NDC 70095-020-02 The 10 mg tablet is white to off white colored, round, biconvex, film-coated tablets, debossed with “H16” on one side and plain on other side. Tablets shall be free from physical defects. Bottles of 30 Unit-of-use: NDC 70095-019-01 Bottles of 100: NDC 70095-019-02 Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature]. Protect from moisture. Dispense in tight, light-resistant containers. To report SUSPECTED ADVERSE REACTIONS, contact Sun Pharmaceutical Industries, Inc. at +1 855 963 5151 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Manufactured by: Harman Finochem Limited A-100/1 Finished Dosage Form (FDF), M.I.D.C. Industrial Area, Shendra, Ch. Sambhajinagar, Maharashtra 431154, India (IND) Distributed by: Sun Pharmaceutical Industries, Inc. Cranbury, NJ 08512 Revised: 10/2024