Brimonidine Tartrate - Brimonidine Tartrate solution prescribing information
INDICATIONS AND USAGE
Brimonidine tartrate ophthalmic solution, 0.15% is indicated for the lowering of intraocular pressure in patients with open-angle glaucoma or ocular hypertension.
DOSAGE AND ADMINISTRATION
The recommended dosage is one drop of brimonidine tartrate ophthalmic solution, 0.15% in the affected eye(s) three-times daily, approximately 8 hours apart.
Brimonidine tartrate ophthalmic solution, 0.15% may be used concomitantly with other topical ophthalmic drug products to lower intraocular pressure. If more than one topical ophthalmic product is being used, the products should be administered at least 5 minutes apart.
DOSAGE FORMS AND STRENGTHS
Ophthalmic solution containing 0.15% (1.5 mg/mL) brimonidine tartrate.
USE IN SPECIFIC POPULATIONS
Use with caution in pediatric patients aged 2 years and older (8.4 ).
Pregnancy
Risk Summary
There are no adequate and well-controlled studies with brimonidine tartrate ophthalmic solution, 0.15% in pregnant women. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
In animal studies, brimonidine crossed the placenta and entered into the fetal circulation to a limited extent (see Data). Because animal reproduction studies are not always predictive of human response, brimonidine tartrate ophthalmic solution, 0.15% should be used during pregnancy only if the potential benefit to the mother justifies the potential risk to the fetus.
Data
Human Data
Limited available data from postmarketing safety reports and published literature with topical use of brimonidine tartrate ophthalmic solution in pregnant women are insufficient to inform a drug-associated risk of pregnancy-related adverse outcomes including miscarriage, stillbirth, congenital anomaly, and events experiences by offspring while breastfeeding.
Animal Data
Embryofetal studies were conducted in pregnant rabbits administered brimonidine tartrate by daily oral gavage on gestation days 6 to 18, to target the period of organogenesis. Brimonidine caused miscarriage at 5 mg/kg/day (approximately 50-times the recommended human ophthalmic dose (RHOD) based on AUC). The no observed adverse effect level (NOAEL) for developmental toxicity in rabbits was 1 mg/kg/day (approximately 6-fold the RHOD based on AUC). No treatment-related malformations were observed in rabbits. Signs of maternal sedation and fatigue were observed at all dose levels; the lowest observed adverse effect level (LOAEL) for maternal toxicity was 5 mg/kg/day, based on the dose-response for these signs.
Embryofetal studies were conducted in pregnant rats administered brimonidine tartrate by daily oral gavage on gestation days 6 to 15, to target the period of organogenesis. The NOAEL for developmental toxicity was 2.5 mg/kg/day (approximately 750-fold the RHOD based on AUC). No treatment-related malformations were observed in rats. The LOAEL for maternal toxicity was 2.5 mg/kg/day, based on signs of sedation and fatigue. The maternal NOAEL was 1 mg/kg/day (180-fold the RHOD based on AUC).
After pregnant rats received a single oral dose of 14 C-brimonidine tartrate, brimonidine and metabolites crossed the placenta and were detectable in fetal blood and organs.
Lactation
Risk Summary
It is not known whether brimonidine tartrate is excreted in human milk. In animal studies, brimonidine has been shown to cross the blood-brain barrier and is excreted into breast milk after oral administration to lactating rats (see Data) . Because of the potential for serious adverse reactions, including central nervous system depression and apnea, from brimonidine tartrate ophthalmic solution, 0.15% in nursing infants, brimonidine tartrate ophthalmic solution, 0.15% is not recommended for use during lactation.
Data
Animal Data
After a single oral dose of 14 C-labeled brimonidine tartrate to lactating rats, brimonidine and metabolites were detected in milk. After male and female rats received a single oral dose of 14 C-brimonidine tartrate, brimonidine crossed the blood:brain barrier. Radiolabel was detected in the cerebellum, cerebrum, and spinal cord.
Pediatric Use
Brimonidine tartrate ophthalmic solution, 0.15% is contraindicated in pediatric patients younger than 2 years old [see Contraindications (4.1 )] . During postmarketing surveillance, apnea, bradycardia, coma, hypotension, hypothermia, hypotonia, lethargy, pallor, respiratory depression, and somnolence have been reported in infants receiving brimonidine.
In a well-controlled clinical study conducted in pediatric glaucoma patients aged 2 to 7 years old, the most commonly observed adverse events with brimonidine tartrate ophthalmic solution 0.2% dosed three-times-daily were somnolence (50% to 83% in pediatric patients aged 2 to 6 years old) and decreased alertness. In pediatric patients aged 7 years and older (>20 kg), somnolence appears to occur less frequently (25%). Approximately 16% of pediatric patients on brimonidine tartrate ophthalmic solution discontinued from the study due to somnolence.
Geriatric Use
No overall differences in safety or effectiveness have been observed between elderly and other adult patients.
CONTRAINDICATIONS
Neonates and Infants (Pediatric Patients Younger than 2 Years Old)
Brimonidine tartrate ophthalmic solution, 0.15% is contraindicated in neonates and infants (pediatric patients younger than 2 years old) [see Use in Specific Populations (8.4 ) ].
Hypersensitivity Reactions
WARNINGS AND PRECAUTIONS
- Potentiation of vascular insufficiency (5.1 )
Potentiation of Vascular Insufficiency
Brimonidine tartrate ophthalmic solution, 0.15% may potentiate syndromes associated with vascular insufficiency. Brimonidine tartrate ophthalmic solution, 0.15% should be used with caution in patients with depression, cerebral or coronary insufficiency, Raynaud's phenomenon, orthostatic hypotension, or thromboangiitis obliterans.
5.2 Severe Cardiovascular Disease
Although brimonidine tartrate ophthalmic solution had minimal effect on the blood pressure of patients in clinical studies, caution should be exercised in treating patients with severe cardiovascular disease.
5.3 Contamination of Topical Ophthalmic Products After Use
There have been reports of bacterial keratitis associated with the use of multiple-dose containers of topical ophthalmic products. These containers had been inadvertently contaminated by patients who, in most cases, had a concurrent corneal disease or a disruption of the ocular epithelial surface.
ADVERSE REACTIONS
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Neonates and Infants (Pediatric Patients Younger than 2 Years Old) [see Contraindications (4.1 )]
- Potentiation of Vascular Insufficiency [see Warnings and Precautions (5.1 )]
- Severe Cardiovascular Disease [see Warnings and Precautions (5.2 )]
- Contamination of Topical Ophthalmic Products After Use [see Warnings and Precautions (5.3 )]
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Adverse reactions occurring in approximately 10 to 20% of the subjects included: allergic conjunctivitis, conjunctival hyperemia, and eye pruritis.
Adverse reactions occurring in approximately 5 to 9% of the subjects included: burning sensation, conjunctival folliculosis, hypertension, ocular allergic reaction, oral dryness, and visual disturbance.
Adverse reactions occurring in approximately 1 to 4% of subjects included: allergic reaction, arthralgia, arthritis, asthenia, blepharitis, blepharoconjunctivitis, blurred vision, bronchitis, cataract, chest pain, conjunctival edema, conjunctival hemorrhage, conjunctivitis, cough, dizziness, diabetes mellitus, dyspepsia, dyspnea, epiphora, eye discharge, eye dryness, eye irritation, eye pain, eyelid edema, eyelid erythema, fatigue, flu syndrome, follicular conjunctivitis, foreign body sensation, gastrointestinal disorder, headache, hypercholesterolemia, hypotension, infection, insomnia, joint disorder, keratitis, lid disorder, osteoporosis, pharyngitis, photophobia, rash, rhinitis, sinus infection, sinusitis, somnolence, stinging, superficial punctate keratopathy, tearing, visual field defect, vitreous detachment, vitreous disorder, vitreous floaters, and worsened visual acuity.
The following adverse reactions were reported in less than 1% of subjects: corneal erosion, nasal dryness, and taste perversion.
Postmarketing Experience
The following adverse reactions have been identified during postapproval use of brimonidine tartrate ophthalmic solution. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Bradycardia, iritis, miosis, skin reactions (including erythema, eyelid pruritis, rash, and vasodilation), and tachycardia.
- Apnea, bradycardia, hypotension, hypothermia, hypotonia, and somnolence have been reported in infants receiving brimonidine tartrate ophthalmic solutions.
DRUG INTERACTIONS
- Concomitant use with systemic beta-blockers may potentiate systemic beta-blockade (7.1 ).
- Use with CNS depressants may result in an additive or potentiating effect (7.2 ).
- Tricyclic antidepressants may potentially blunt the hypotensive effect of systemic clonidine (7.3 ).
- Monoamine oxidase inhibitors may result in increased hypotension (7.4 ).
Anti-hypertensives / Cardiac Glycosides
Alpha-2 agonists, as a class, may reduce blood pressure. Caution in using drugs such as beta-blockers (ophthalmic and systemic), anti-hypertensives and/or cardiac glycosides is advised.
CNS Depressants
Although specific drug interaction studies have not been conducted with brimonidine tartrate ophthalmic solution, 0.15%, the possibility of an additive or potentiating effect with CNS depressants (alcohol, barbiturates, opiates, sedatives, or anesthetics) should be considered.
Tricyclic Antidepressants
Tricyclic antidepressants have been reported to blunt the hypotensive effect of systemic clonidine. It is not known whether the concurrent use of these agents with brimonidine tartrate ophthalmic solution, 0.15% in humans can lead to resulting interference with its IOP-lowering effect. Caution, however, is advised in patients taking tricyclic antidepressants, which can affect the metabolism and uptake of circulating amines.
Monoamine Oxidase Inhibitors
Monoamine oxidase (MAO) inhibitors may theoretically interfere with the metabolism of brimonidine and potentially result in an increased systemic side-effect such as hypotension. Caution is advised in patients taking MAO inhibitors which can affect the metabolism and uptake of circulating amines.
DESCRIPTION
Brimonidine tartrate ophthalmic solution, 0.15% (1.5 mg brimonidine tartrate per mL equivalent to 1.0 mg brimonidine free base per mL) is a relatively selective alpha-2-adrenergic agonist for topical ophthalmic use. The chemical name of brimonidine tartrate is 5-bromo-6-(2-imidazolidinylideneamino) quinoxaline L-tartrate. It is a white to off-white,
pale yellow to yellow powder. It has a molecular weight of 442.24 as the tartrate salt, and is both soluble in water (1.5 mg/mL) and in the product vehicle (3.0 mg/mL) at pH 7.2. The structural formula is:
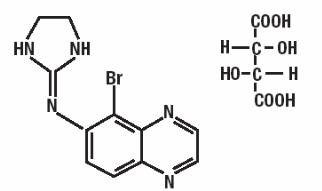
Formula: C 11 H 10 BrN 5 • C 4 H 6 O 6
CAS Number: 59803-98-4
In solution, brimonidine tartrate ophthalmic solution, 0.15% has a clear, pale yellow to greenish yellow color. It has an osmolality of 250 - 350 mOsmol/kg and a pH of 6.6 to 7.4.
Contains: Active ingredient: brimonidine tartrate 1.5 mg/mL (1.5 mg/mL), Preservative: Polyquad (polyquaternium-1) 0.001% (0.01 mg/mL), Inactives: boric acid, calcium chloride, magnesium chloride, mannitol, potassium chloride, povidone, purified water, sodium borate, sodium chloride, with hydrochloric acid and/or sodium hydroxide to adjust pH.
CLINICAL PHARMACOLOGY
Mechanism of Action
Brimonidine tartrate ophthalmic solution, 0.15% is an alpha-2 adrenergic receptor agonist. Fluorophotometric studies in animals and humans suggest that brimonidine tartrate has a dual mechanism of action by reducing aqueous humor production and increasing uveoscleral outflow.
Pharmacodynamics
Brimonidine tartrate ophthalmic solution, 0.15% has a peak ocular hypotensive effect occurring at two hours post-dosing.
Elevated IOP presents a major risk factor in glaucomatous field loss. The higher the level of IOP, the greater the likelihood of optic nerve damage and visual field loss. Brimonidine tartrate has the action of lowering intraocular pressure with minimal effect on cardiovascular and pulmonary parameters.
Pharmacokinetics
Absorption
In a pharmacokinetic study, 14 healthy subjects (4 males and 10 females) received a single topical ocular administration of brimonidine tartrate ophthalmic solution, 0.15%, one drop per eye. The peak plasma concentrations (C max ) and AUC 0-inf were 73 ± 19 pg/mL and 375 ± 89 pg•hr/mL, respectively. T max was 1.7 ± 0.7 hours after dosing. The systemic half-life was approximately 2.1 hours.
Distribution
Brimonidine was approximately 29% bound to plasma proteins in healthy subjects.
Elimination
Metabolism
In humans, brimonidine is extensively metabolized by the liver.
Excretion
Urinary excretion is the major route of elimination of brimonidine and its metabolites. Approximately 87% of an orally administered radioactive dose of brimonidine was eliminated within 120 hours, with 74% of the radioactivity recovered in the urine.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
No compound-related carcinogenic effects were observed in either mice or rats following a 21-month and a 24-month study, respectively. In these studies, dietary administration of brimonidine tartrate at doses up to 2.5 mg/kg/day in mice and 1.0 mg/kg/day in rats achieved 120 and 76 times the recommended human ophthalmic dose (RHOD) based on C max .
Mutagenesis
Brimonidine tartrate was not mutagenic or cytogenic in a series of in vitro and in vivo studies including the Ames test, chromosomal aberration assay in Chinese hamster ovary (CHO) cells, a host-mediated assay and cytogenic studies in mice, and dominant lethal assay.
Impairment of Fertility
A reproduction and fertility study in rats with brimonidine tartrate demonstrated no adverse effect on male or female fertility at oral doses up to 1 mg/kg (approximately 180 times the recommended human ophthalmic dose (RHOD) based on estimated AUC).
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Adverse reactions occurring in approximately 10 to 20% of the subjects included: allergic conjunctivitis, conjunctival hyperemia, and eye pruritis.
Adverse reactions occurring in approximately 5 to 9% of the subjects included: burning sensation, conjunctival folliculosis, hypertension, ocular allergic reaction, oral dryness, and visual disturbance.
Adverse reactions occurring in approximately 1 to 4% of subjects included: allergic reaction, arthralgia, arthritis, asthenia, blepharitis, blepharoconjunctivitis, blurred vision, bronchitis, cataract, chest pain, conjunctival edema, conjunctival hemorrhage, conjunctivitis, cough, dizziness, diabetes mellitus, dyspepsia, dyspnea, epiphora, eye discharge, eye dryness, eye irritation, eye pain, eyelid edema, eyelid erythema, fatigue, flu syndrome, follicular conjunctivitis, foreign body sensation, gastrointestinal disorder, headache, hypercholesterolemia, hypotension, infection, insomnia, joint disorder, keratitis, lid disorder, osteoporosis, pharyngitis, photophobia, rash, rhinitis, sinus infection, sinusitis, somnolence, stinging, superficial punctate keratopathy, tearing, visual field defect, vitreous detachment, vitreous disorder, vitreous floaters, and worsened visual acuity.
The following adverse reactions were reported in less than 1% of subjects: corneal erosion, nasal dryness, and taste perversion.
HOW SUPPLIED/STORAGE AND HANDLING
Brimonidine tartrate ophthalmic solution, 0.15% is supplied sterile in opaque white LDPE plastic bottles and natural tips with purple polypropylene caps as follows:
5 mL in 8 mL bottle NDC 61314-144-05
10 mL in 10 mL bottle NDC 61314-144-10
15 mL in 15 mL bottle NDC 61314-144-15
Storage: Store at 15°C to 25° C (59°F to 77°F). After opening, Brimonidine tartrate ophthalmic solution, 0.15% can be used until the expiration date on the bottle.
Mechanism of Action
Brimonidine tartrate ophthalmic solution, 0.15% is an alpha-2 adrenergic receptor agonist. Fluorophotometric studies in animals and humans suggest that brimonidine tartrate has a dual mechanism of action by reducing aqueous humor production and increasing uveoscleral outflow.