Get your patient on Cefaclor - Cefaclor suspension (Cefaclor)
Cefaclor - Cefaclor suspension prescribing information
INDICATIONS AND USAGE
Cefaclor is indicated in the treatment of the following infections when caused by susceptible strains of the designated microorganisms:
Otitis media caused by Streptococcus pneumoniae, Haemophilus influenzae , staphylococci, and Streptococcus pyogenes
Note: β-lactamase-negative, ampicillin-resistant (BLNAR) strains of Haemophilus influenzae should be considered resistant to cefaclor despite apparent in vitro susceptibility of some BLNAR strains.
Lower respiratory tract infections , including pneumonia, caused by Streptococcus pneumoniae, Haemophilus influenzae , and Streptococcus pyogenes
Note: β-lactamase-negative, ampicillin-resistant (BLNAR) strains of Haemophilus influenzae should be considered resistant to cefaclor despite apparent in vitro susceptibility of some BLNAR strains.
Pharyngitis and Tonsillitis , caused by Streptococcus pyogenes
Note: Penicillin is the usual drug of choice in the treatment and prevention of streptococcal infections, including the prophylaxis of rheumatic fever. Cefaclor is generally effective in the eradication of streptococci from the nasopharynx; however, substantial data establishing the efficacy of cefaclor in the subsequent prevention of rheumatic fever are not available at present.
Urinary tract infections , including pyelonephritis and cystitis, caused by Escherichia coli, Proteus mirabilis, Klebsiella spp., and coagulase-negative staphylococci
Skin and skin structure infections caused by Staphylococcus aureus and Streptococcus pyogenes
Appropriate culture and susceptibility studies should be performed to determine susceptibility of the causative organism to cefaclor.
To reduce the development of drug-resistant bacteria and maintain the effectiveness of Cefaclor for Oral Suspension and other antibacterial drugs, Cefaclor for Oral Suspension should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
DOSAGE AND ADMINISTRATION
Cefaclor is administered orally.
Adults -- The usual adult dosage is 250 mg every 8 hours. For more severe infections (such as pneumonia) or those caused by less susceptible organisms, doses may be doubled.
Pediatric Patients -- The usual recommended daily dosage for pediatric patients is 20 mg/kg/day in divided doses every 8 hours. In more serious infections, otitis media, and infections caused by less susceptible organisms, 40 mg/kg/day are recommended, with a maximum dosage of 1 g/day.
Table 1:
| Cefaclor for Oral Suspension, USP | ||
| 20 mg/kg/day | ||
| Weight | 125 mg/5 mL | 250 mg/5 mL |
| 9 kg | 1/2 tsp t.i.d. | |
| 18 kg | 1 tsp t.i.d. | 1/2 tsp t.i.d. |
| 40 mg/kg/day | ||
| 9 kg | 1 tsp t.i.d. | 1/2 tsp t.i.d. |
| 18 kg | 1 tsp t.i.d. | |
B.I.D. Treatment Option —For the treatment of otitis media and pharyngitis, the total daily dosage may be divided and administered every 12 hours.
Table 2:
| Cefaclor for Oral Suspension, USP | |
| 20 mg/kg/day (Pharyngitis) | |
| Weight | 375 mg/5 mL |
| 18 kg | 1/2 tsp b.i.d. |
| 40 mg/kg/day (Otitis Media) | |
| 9 kg | 1/2 tsp b.i.d. |
| 18 kg | 1 tsp b.i.d. |
Cefaclor may be administered in the presence of impaired renal function. Under such a condition, the dosage usually is unchanged (see PRECAUTIONS ).
In the treatment of β-hemolytic streptococcal infections, a therapeutic dosage of cefaclor should be administered for at least 10 days.
Directions for Mixing:
Add appropriate water volume as indicated in the following table in two portions to dry mixture in the bottle. Shake well after each addition.
Each 5 mL (approximately one teaspoonful) will then contain Cefaclor, USP, monohydrate equivalent to 250 mg anhydrous cefaclor, respectively, as shown in the following table.
Oversize bottle provides extra space for shaking.
Table 3:
| Cefaclor For Oral Suspension, USP | ||
| Strength Package Size (when mixed) | Water Volume to Add | Anhydrous Cefaclor/5 mL (approx. one teaspoonful) |
| 250 mg/5 Ml 150 mL | 106 mL | 250 mg |
CONTRAINDICATIONS
Cefaclor is contraindicated in patients with known allergy to the cephalosporin group of antibiotics.
ADVERSE REACTIONS
Adverse effects considered to be related to therapy with cefaclor are listed below:
Hypersensitivity reactions have been reported in about 1.5% of patients and include morbilliform eruptions (1 in 100). Pruritus, urticaria, and positive Coombs' tests each occur in less than 1 in 200 patients.
Cases of serum-sickness-like reactions have been reported with the use of cefaclor. These are characterized by findings of erythema multiforme, rashes, and other skin manifestations accompanied by arthritis/arthralgia, with or without fever, and differ from classic serum sickness in that there is infrequently associated lymphadenopathy and proteinuria, no circulating immune complexes, and no evidence to date of sequelae of the reaction. Occasionally, solitary symptoms may occur, but do not represent a serum-sickness-like reaction. While further investigation is ongoing, serum-sickness-like reactions appear to be due to hypersensitivity and more often occur during or following a second (or subsequent) course of therapy with cefaclor. Such reactions have been reported more frequently in pediatric patients than in adults with an overall occurrence ranging from 1 in 200 (0.5%) in one focused trial to 2 in 8,346 (0.024%) in overall clinical trials (with an incidence in pediatric patients in clinical trials of 0.055%) to 1 in 38,000 (0.003%) in spontaneous event reports. Signs and symptoms usually occur a few days after initiation of therapy and subside within a few days after cessation of therapy; occasionally these reactions have resulted in hospitalization, usually of short duration (median hospitalization = 2 to 3 days, based on postmarketing surveillance studies). In those requiring hospitalization, the symptoms have ranged from mild to severe at the time of admission with more of the severe reactions occurring in pediatric patients. Antihistamines and glucocorticoids appear to enhance resolution of the signs and symptoms. No serious sequelae have been reported.
More severe hypersensitivity reactions, including Stevens-Johnson syndrome, toxic epidermal necrolysis, and anaphylaxis have been reported rarely.
Anaphylactoid events may be manifested by solitary symptoms, including angioedema, asthenia, edema (including face and limbs), dyspnea, paresthesias, syncope, hypotension, or vasodilatation. Anaphylaxis may be more common in patients with a history of penicillin allergy.
Rarely, hypersensitivity symptoms may persist for several months.
Gastrointestinal symptoms occur in about 2.5% of patients and include diarrhea (1 in 70).
Onset of pseudomembranous colitis symptoms may occur during or after antibiotic treatment. (see WARNINGS ). Nausea and vomiting have been reported rarely. As with some penicillins and some other cephalosporins, transient hepatitis and cholestatic jaundice have been reported rarely.
Other effects considered related to therapy included eosinophilia (1 in 50 patients), genital pruritus, moniliasis or vaginitis (about 1 in 50 patients), and, rarely, thrombocytopenia or reversible interstitial nephritis.
Causal Relationship Uncertain –
CNS -- Rarely, reversible hyperactivity, agitation, nervousness, insomnia, confusion, hypertonia, dizziness, hallucinations, and somnolence have been reported.
Transitory abnormalities in clinical laboratory test results have been reported. Although they were of uncertain etiology, they are listed below to serve as alerting information for the physician.
Hepatic -- Slight elevations of AST, ALT, or alkaline phosphatase values (1 in 40).
Hematopoietic -- As has also been reported with other β-lactam antibiotics, transient lymphocytosis, leukopenia, and, rarely, hemolytic anemia, aplastic anemia, agranulocytosis, and reversible neutropenia of possible clinical significance.
There have been rare reports of increased prothrombin time with or without clinical bleeding in patients receiving cefaclor and Coumadin ® concomitantly.
Renal -- Slight elevations in BUN or serum creatinine (less than 1 in 500) or abnormal urinalysis (less than 1 in 200).
Cephalosporin-class Adverse Reactions
In addition to the adverse reactions listed above that have been observed in patients treated with cefaclor, the following adverse reactions and altered laboratory tests have been reported for cephalosporin-class antibiotics: fever, abdominal pain, superinfection, renal dysfunction, toxic nephropathy, hemorrhage, false-positive test for urinary glucose, elevated bilirubin, elevated LDH, and pancytopenia.
Several cephalosporins have been implicated in triggering seizures, particularly in patients with renal impairment when the dosage was not reduced. If seizures associated with drug therapy occur, the drug should be discontinued. Anticonvulsant therapy can be given if clinically indicated (see DOSAGE AND ADMINISTRATION and OVERDOSAGE sections).
To report SUSPECTED ADVERSE REACTIONS, contact Azorian Pharma at 1- 302-459-8479 or FDA at 1-800-FDA-1088 or www.fda.gov/me. dwatch
DESCRIPTION
Cefaclor, USP, is a semisynthetic cephalosporin antibiotic for oral administration. It is chemically designated as 3-chloro-7-D-(2-phenylglycinamido) -3-cephem-4-carboxylic acid monohydrate. The chemical formula for cefaclor is C 15 H 14 ClN 3 O 4 S•H 2 O and the molecular weight is 385.82.
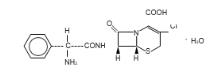
After mixing, each 5 mL of Cefaclor for Oral Suspension will contain cefaclor monohydrate equivalent to 250 mg (0.68 mmol) anhydrous cefaclor. The suspensions also contain methylcellulose, sodium lauryl sulfate, sucrose, and xanthan gum, FD&C Red No. 40, strawberry flavor.
The color of drug powder in the dry powder state is white to off-white. After reconstitution, it turns to a red suspension.
CLINICAL PHARMACOLOGY
Cefaclor is well-absorbed after oral administration to fasting subjects. Total absorption is the same whether the drug is given with or without food; however, when it is taken with food, the peak concentration achieved is 50% to 75% of that observed when the drug is administered to fasting subjects and generally appears from three-fourths to 1 hour later. Following administration of 250 mg, 500 mg, and 1 g doses to fasting subjects, average peak serum levels of approximately 7, 13, and 23 mcg/mL, respectively, were obtained within 30 to 60 minutes. Approximately 60% to 85% of the drug is excreted unchanged in the urine within 8 hours, the greater portion being excreted within the first 2 hours. During this 8-hour period, peak urine concentrations following the 250 mg, 500 mg and 1 g doses were approximately 600, 900 and 1,900 mcg/mL, respectively. The serum half-life in normal subjects is 0.6 to 0.9 hour. In patients with reduced renal function, the serum half-life of cefaclor is slightly prolonged. In those with complete absence of renal function, the plasma half-life of the intact molecule is 2.3 to 2.8 hours. Excretion pathways in patients with markedly impaired renal function have not been determined. Hemodialysis shortens the half-life by 25% to 30%.
Microbiology
Mechanism of Action
As with other cephalosporins, the bactericidal action of cefaclor results from inhibition of cell-wall synthesis.
Mechanism of Resistance
Resistance to cefaclor is primarily through hydrolysis of beta-lactamases, alteration of penicillin-binding proteins (PBPs) and decreased permeability. Pseudomonas spp., Acinetobacter calcoaceticus and most strains of Enterococci (Enterococcus faecalis , group D streptococci), Enterobacter spp., indole-positive Proteus, Morganella morganii (formerly Proteus morganii), Providencia rettgeri (formerly Proteus rettgeri ), and Serratia spp. are resistant to cefaclor. Cefaclor is inactive against methicillin-resistant staphylococci. β-lactamase-negative, ampicillin-resistant strains of H. influenzae should be considered resistant to cefaclor despite apparent in vitro susceptibility to this agent.
Antibacterial Activity
Cefaclor has been shown to be active against most strains of the following microorganisms both in vitro and in clinical infections as described in the INDICATIONS AND USAGE section.
Gram-positive Bacteria
Staphylococcus aureus (methicillin susceptible only)
Coagulase negative staphylococci (methicillin susceptible only)
Streptococcus pneumoniae
Streptococcus pyogenes (group A β-hemolytic streptococci)
Gram-negative Bacteria
Escherichia coli
Haemophilus influenzae (excluding β-lactamase-negative, ampicillin-resistant strains)
Klebsiella spp.
Proteus mirabilis
The following in vitro data are available, but their clinical significance is unknown. At least 90 percent of the following bacteria exhibit an in vitro minimum inhibitory concentrations (MICs) less than or equal to the susceptible breakpoint of cefaclor. However, the safety and effectiveness of cefaclor in treating clinical infections due to these bacteria has not been established in adequate and well-controlled trials.
Gram-negative Bacteria
Citrobacter diversus
Moraxella catarrhalis
Neisseria gonorrhoeae
Anaerobic Bacteria
Bacteroides spp.
Peptococcus spp.
Peptostreptococcus spp.
Propionibacterium acnes
Susceptibility Testing
For specific information regarding susceptibility test interpretive criteria and associated test methods and quality control standards recognized by FDA for this drug, please see: https://www.fda.gov/STIC.
HOW SUPPLIED
Cefaclor Oral Suspension, USP, is supplied in bottles with child-resistant caps as:
250 mg/5 mL strawberry flavor
NDC 81948-6250-1 (150 mL size)
After mixing, store in a refrigerator. Shake well before using. Keep tightly closed. The mixture may be kept for 14 days without significant loss of potency. Discard unused portion after 14 days.
Store dry powder at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
Manufactured by: Yung Shin Pharmaceutical Ind. Co., Ltd. Tachia, Taichung 43769, TAIWAN Manufactured for:

Azorian Pharma, LLC Claymont, DE 19703
Revised: 10/22
KRP50e (Azorian) USA 2150153-001