Get your patient on Clonidine - Clonidine injection, Solution (Clonidine)
Clonidine - Clonidine injection, Solution prescribing information
The 500 mcg/mL strength product should be diluted prior to use in an appropriate solution.
INDICATIONS AND USAGE
Clonidine hydrochloride injection is indicated in combination with opiates for the treatment of severe pain in cancer patients that is not adequately relieved by opioid analgesics alone. Epidural clonidine is more likely to be effective in patients with neuropathic pain than somatic or visceral pain (see Clinical Trials ).
The safety of this drug product has only been established in a highly selected group of cancer patients, and only after an adequate trial of opioid analgesia. Other use is of unproven safety and is not recommended. In a rare patient, the potential benefits may outweigh the known risks (see WARNINGS ).
DOSAGE AND ADMINISTRATION
The recommended starting dose of clonidine hydrochloride injection for continuous epidural infusion is 30 mcg/hr. Although dosage may be titrated up or down depending on pain relief and occurrence of adverse events, experience with dosage rates above 40 mcg/hr is limited.
Familiarization with the continuous epidural infusion device is essential. Patients receiving epidural clonidine from a continuous infusion device should be closely monitored for the first few days to assess their response.
The 500 mcg/mL (0.5 mg/mL) strength product must be diluted prior to use in 0.9% Sodium Chloride for Injection, USP, to a final concentration of 100 mcg/mL:
| Volume of Clonidine Hydrochloride 500 mcg/mL | Volume of 0.9% Sodium Chloride for Injection, USP | Resulting Final Clonidine Hydrochloride Injection Concentration (100 mcg/mL) |
| 1 mL | 4 mL | 500 mcg/5 mL |
| 2 mL | 8 mL | 1000 mcg/10 mL |
| 3 mL | 12 mL | 1500 mcg/15 mL |
| 4 mL | 16 mL | 2000 mcg/20 mL |
| 5 mL | 20 mL | 2500 mcg/25 mL |
| 6 mL | 24 mL | 3000 mcg/30 mL |
| 7 mL | 28 mL | 3500 mcg/35 mL |
| 8 mL | 32 mL | 4000 mcg/40 mL |
| 9 mL | 36 mL | 4500 mcg/45 mL |
| 10 mL | 40 mL | 5000 mcg/50 mL |
Renal Impairment
Dosage should be adjusted according to the degree of renal impairment, and patients should be carefully monitored. Since only a minimal amount of clonidine is removed during routine hemodialysis, there is no need to give supplemental clonidine following dialysis.
Clonidine hydrochloride injection must not be used with a preservative.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
Special Populations
The pharmacokinetics of epidurally administered clonidine has not been studied in the pediatric population or in patients with renal or hepatic disease.
CONTRAINDICATIONS
Clonidine hydrochloride injection is contraindicated in patients with a history of sensitization or allergic reactions to clonidine. Epidural administration is contraindicated in the presence of an injection site infection, in patients on anticoagulant therapy, and in those with a bleeding diathesis. Administration of clonidine hydrochloride injection above the C4 dermatome is contraindicated since there are no adequate safety data to support such use (see WARNINGS ).
ADVERSE REACTIONS
Adverse reactions seen during continuous epidural clonidine infusion are dose-dependent and typical for a compound of this pharmacologic class. The adverse events most frequently reported in the pivotal controlled clinical trial of continuous epidural clonidine administration consisted of hypotension, postural hypotension, decreased heart rate, rebound hypertension, dry mouth, nausea, confusion, dizziness, somnolence, and fever. Hypotension is the adverse event that most frequently requires treatment. The hypotension is usually responsive to intravenous fluids and, if necessary, appropriate parenterally-administered pressor agents. Hypotension was observed more frequently in women and in lower weight patients, but no dose-related response was established.
Implantable epidural catheters are associated with a risk of catheter-related infections, including meningitis and/or epidural abscess. The risk depends on the clinical situation and the type of catheter used, but catheter related infections occur in 5% to 20% of patients, depending on the kind of catheter used, catheter placement technique, quality of catheter care, and length of catheter placement.
The inadvertent intrathecal administration of clonidine has not been associated with a significantly increased risk of adverse events, but there are inadequate safety and efficacy data to support the use of intrathecal clonidine.
Epidural clonidine was compared to placebo in a two-week double-blind study of 85 terminal cancer patients with intractable pain receiving epidural morphine. The following adverse events were reported in two or more patients and may be related to administration of either clonidine or morphine:
| Incidence of Adverse Events in the Two-Week Trial | |||
|---|---|---|---|
| Adverse Events | Clonidine N = 38 n (%) | Placebo N = 47 n (%) | |
| Total Number of Patients Who Experienced at Least One Adverse Event | 37 (97.4) | 38 (80.5) | |
| Hypotension | 17 (44.8) | 5 (10.6) | |
| Postural Hypotension | 12 (31.6) | 0 (0) | |
| Dry Mouth | 5 (13.2) | 4 (8.5) | |
| Nausea | 5 (13.2) | 10 (21.3) | |
| Somnolence | 5 (13.2) | 10 (21.3) | |
| Dizziness | 5 (13.2) | 2 (4.3) | |
| Confusion | 5 (13.2) | 5 (10.6) | |
| Vomiting | 4 (10.5) | 7 (14.9) | |
| Nausea/Vomiting | 3 (7.9) | 1 (2.1) | |
| Sweating | 2 (5.3) | 0 (0) | |
| Chest Pain | 2 (5.3) | 0 (0) | |
| Hallucination | 2 (5.3) | 1 (2.1) | |
| Tinnitus | 2 (5.3) | 0 (0) | |
| Constipation | 1 (2.6) | 2 (4.3) | |
| Tachycardia | 1 (2.6) | 2 (4.3) | |
| Hypoventilation | 1 (2.6) | 2 (4.3) | |
An open label long-term extension of the above trial was performed. Thirty-two subjects received epidural clonidine and morphine for up to 94 weeks with a median dosing period of 10 weeks. The following adverse events (and percent incidence) were reported: hypotension/ postural hypotension (47%); nausea (13%); anxiety/confusion (38%); somnolence (25%); urinary tract infection (22%); constipation, dyspnea, fever, infection (6% each); asthenia, hyperaesthesia, pain, skin ulcer, and vomiting (5% each). Eighteen percent of subjects discontinued this study as a result of catheter-related problems (infections, accidental dislodging, etc.), and one subject developed meningitis, possibly as a result of a catheter-related infection. In this study, rebound hypertension was not assessed, and ECG and laboratory data were not systematically sought.
The following adverse reactions have also been reported with the use of any dosage form of clonidine. In many cases patients were receiving concomitant medication and a causal relationship has not been established:
Body as a Whole: Weakness, 10%; fatigue, 4%; headache and withdrawal syndrome, each 1%. Also reported were pallor, a weakly positive Coomb's test, and increased sensitivity to alcohol.
Cardiovascular: Palpitations and tachycardia, and bradycardia, each 0.5%. Syncope, Raynaud’s phenomenon, congestive heart failure, and electrocardiographic abnormalities (i.e., sinus node arrest, functional bradycardia, high degree AV block) have been reported rarely. Rare cases of sinus bradycardia and atrioventricular block have been reported, both with and without the use of concomitant digitalis.
Central Nervous System: Nervousness and agitation, 3%; mental depression, 1%; insomnia, 0.5%. Cerebrovascular accidents, other behavioral changes, vivid dreams or nightmares, restlessness, and delirium have been reported rarely.
Dermatological: Rash, 1%; pruritus, 0.7%; hives, angioneurotic edema and urticaria, 0.5%; alopecia, 0.2%.
Gastrointestinal: Anorexia and malaise, each 1%; mild transient abnormalities in liver function tests, 1%; hepatitis, parotitis, ileus and pseudo obstruction, and abdominal pain, rarely.
Genitourinary: Decreased sexual activity, impotence, and libido, 3%; nocturia, about 1%; difficulty in micturition, about 0.2%; urinary retention, about 0.1%.
Hematologic: Thrombocytopenia, rarely.
Metabolic: Weight gain, 0.1%; gynecomastia, 1%; transient elevation of glucose or serum phosphatase, rarely.
Musculoskeletal: Muscle or joint pain, about 0.6%; leg cramps, 0.3%.
Oro-otolaryngeal: Dryness of the nasal mucosa was rarely reported.
Ophthalmological: Dryness of the eyes, burning of the eyes and blurred vision were rarely reported.
To report SUSPECTED ADVERSE REACTIONS, contact XGen Pharmaceuticals DJB, Inc. at 1-866-390-4411 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch .
Drug Interactions
Clonidine may potentiate the CNS-depressive effect of alcohol, barbiturates or other sedating drugs. Narcotic analgesics may potentiate the hypotensive effects of clonidine. Tricyclic antidepressants may antagonize the hypotensive effects of clonidine. The effects of tricyclic antidepressants on clonidine’s analgesic actions are not known.
Beta-blockers may exacerbate the hypertensive response seen with clonidine withdrawal. Also, due to the potential for additive effects such as bradycardia and AV block, caution is warranted in patients receiving clonidine with agents known to affect sinus node function or AV nodal conduction, e.g., digitalis, calcium channel blockers, and beta-blockers.
There is one reported case of a patient with acute delirium associated with the simultaneous use of fluphenazine and oral clonidine. Symptoms resolved when clonidine was withdrawn and recurred when the patient was rechallenged with clonidine.
Epidural clonidine may prolong the duration of pharmacologic effects of epidural local anesthetics, including both sensory and motor blockade.
DESCRIPTION
Clonidine hydrochloride injection is a centrally-acting analgesic solution for use in continuous epidural infusion devices.
Clonidine Hydrochloride, USP, is an imidazoline derivative and exists as a mesomeric compound. The chemical names are Benzenamine, 2,6-dichloro-N-2-imidazolidinylidene monohydrochloride and 2-[(2,6-dichlorophenyl)imino]imidazolidine monohydrochloride. The following is the structural formula:
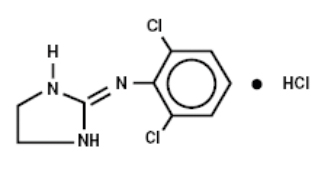
| C 9 H 9 Cl 2 N 3 · HCl | Mol. Wt. 266.56 |
Clonidine hydrochloride injection is supplied as a clear, colorless, preservative-free, pyrogen-free, aqueous sterile solution (pH 5 to 7) in single-dose, 10 mL vials.
Each mL of the 100 mcg/mL (0.1 mg/mL) concentration contains 100 mcg of Clonidine Hydrochloride, USP and 9 mg Sodium Chloride in Water for Injection, USP. Hydrochloric Acid and/or Sodium Hydroxide may have been added for pH adjustment. Each 10 mL vial contains 1 mg (1000 mcg) of clonidine hydrochloride.
Each mL of the 500 mcg/mL (0.5 mg/mL) concentration contains 500 mcg of Clonidine Hydrochloride, USP and 9 mg Sodium Chloride in Water for Injection, USP. Hydrochloric Acid and/or Sodium Hydroxide may have been added for pH adjustment. Each 10 mL vial contains 5 mg (5000 mcg) of clonidine hydrochloride.
CLINICAL PHARMACOLOGY
Mechanism of Action
Epidurally administered clonidine produces dose-dependent analgesia not antagonized by opiate antagonists. The analgesia is limited to the body regions innervated by the spinal segments where analgesic concentrations of clonidine are present. Clonidine is thought to produce analgesia at presynaptic and postjunctional alpha-2-adrenoceptors in the spinal cord by preventing pain signal transmission to the brain.
Pharmacokinetics
Following a 10 minute intravenous infusion of 300 mcg clonidine HCl to five male volunteers, plasma clonidine levels showed an initial rapid distribution phase (mean ± SD t 1⁄2 = 11 ± 9 minutes) followed by a slower elimination phase (t 1⁄2 = 9 ± 2 hours) over 24 hours. Clonidine’s total body clearance (CL) was 219 ± 92 mL/min.
Following a 700 mcg clonidine HCl epidural dose given over five minutes to four male and five female volunteers, peak clonidine plasma levels (4.4 ± 1.4 ng/mL) were obtained in 19 ± 27 minutes. The plasma elimination half-life was determined to be 22 ± 15 hours following sample collection for 24 hours. CL was 190 ± 70 mL/min. In cerebral spinal fluid (CSF), peak clonidine levels (418 ± 255 ng/mL) were achieved in 26 ± 11 minutes. The clonidine CSF elimination half-life was 1.3 ± 0.5 hours when samples were collected for 6 hours. Compared to men, women had a lower mean plasma clearance, longer mean plasma half-life, and higher mean peak level of clonidine in both plasma and CSF.
In cancer patients who received 14 days of clonidine HCl epidural infusion (rate = 30 mcg/hr) plus morphine by patient-controlled analgesia (PCA), steady state clonidine plasma concentrations of 2.2 ± 1.1 and 2.4 ± 1.4 ng/mL were obtained on dosing days 7 and 14, respectively. CL was 279 ± 184 and 272 ± 163 mL/min on these days. CSF concentrations were not determined in these patients.
Distribution
Clonidine is highly lipid soluble and readily distributes into extravascular sites including the central nervous system. Clonidine’s volume of distribution is 2.1 ± 0.4 L/kg. The binding of clonidine to plasma protein is primarily to albumin and varies between 20 and 40% in vitro. Epidurally administered clonidine readily partitions into plasma via the epidural veins and attains systemic concentrations (0.5 to 2 ng/mL) that are associated with a hypotensive effect mediated by the central nervous system.
Excretion
Following an intravenous dose of 14 C-clonidine, 72% of the administered dose was excreted in urine in 96 hours of which 40 to 50% was unchanged clonidine. Renal clearance for clonidine was determined to be 133 ± 66 mL/min. In a study where 14 C-clonidine was given to subjects with varying degrees of kidney function, elimination half-lives varied (17.5 to 41 hours) as a function of creatinine clearance. In subjects undergoing hemodialysis only 5% of body clonidine stores were removed.
Metabolism
In humans, clonidine metabolism follows minor pathways with the major metabolite, p-hydroxy-clonidine, being present at less than 10% of the concentration of unchanged drug in urine.
Special Populations
The pharmacokinetics of epidurally administered clonidine has not been studied in the pediatric population or in patients with renal or hepatic disease.
Clinical Trials
In a double-blind, randomized study of cancer patients with severe intractable pain below the C4 dermatome not controlled by morphine, 38 patients were randomized to an epidural infusion of clonidine hydrochloride injection plus epidural morphine, whereas 47 subjects received epidural placebo plus epidural morphine. Both groups were allowed rescue doses of epidural morphine. Successful analgesia, defined as a decrease in either morphine use or Visual Analog Score (VAS) pain, was significantly more common with epidural clonidine than placebo (45% vs 21%, p=0.016). Only the subgroup of 36 patients with ‘‘neuropathic’’ pain, characterized by the investigator as well-localized, burning, shooting, or electric-like pain in a dermatomal or peripheral nerve distribution had significant analgesic effects relative to placebo in this study.
The most frequent adverse events with clonidine were hypotension (45% vs 11% for placebo, p< 0.001), postural hypotension (32% vs 0%, p< 0.001), dizziness (13% vs 4%, p=0.234), anxiety (11% vs 2%, p=0.168) and dry mouth (13% vs 9%, p=0.505). Both mean blood pressure and heart rate were reduced in the clonidine group. At the conclusion of the two-week study period in the clinical trial, all patients were abruptly withdrawn from study drug or placebo. Four patients of the clonidine group suffered rebound hypertension upon withdrawal of clonidine; one of these patients suffered a cerebrovascular accident. Asymptomatic bradycardia was noted in one clonidine patient.
Clinical Trials
In a double-blind, randomized study of cancer patients with severe intractable pain below the C4 dermatome not controlled by morphine, 38 patients were randomized to an epidural infusion of clonidine hydrochloride injection plus epidural morphine, whereas 47 subjects received epidural placebo plus epidural morphine. Both groups were allowed rescue doses of epidural morphine. Successful analgesia, defined as a decrease in either morphine use or Visual Analog Score (VAS) pain, was significantly more common with epidural clonidine than placebo (45% vs 21%, p=0.016). Only the subgroup of 36 patients with ‘‘neuropathic’’ pain, characterized by the investigator as well-localized, burning, shooting, or electric-like pain in a dermatomal or peripheral nerve distribution had significant analgesic effects relative to placebo in this study.
The most frequent adverse events with clonidine were hypotension (45% vs 11% for placebo, p< 0.001), postural hypotension (32% vs 0%, p< 0.001), dizziness (13% vs 4%, p=0.234), anxiety (11% vs 2%, p=0.168) and dry mouth (13% vs 9%, p=0.505). Both mean blood pressure and heart rate were reduced in the clonidine group. At the conclusion of the two-week study period in the clinical trial, all patients were abruptly withdrawn from study drug or placebo. Four patients of the clonidine group suffered rebound hypertension upon withdrawal of clonidine; one of these patients suffered a cerebrovascular accident. Asymptomatic bradycardia was noted in one clonidine patient.
HOW SUPPLIED
Clonidine hydrochloride injection is supplied as:
100 mcg/mL in cartons containing one 10 mL vial (NDC 39822-2000-1)
500 mcg/mL in cartons containing one 10 mL vial (NDC 39822-2010-1)
Store at 20º to 25ºC (68º to 77ºF) [see USP Controlled Room Temperature].
Preservative Free. Discard unused portion.
Vial stoppers do not contain natural rubber latex.
Manufactured for: XGen Pharmaceuticals DJB, Inc. Big Flats, NY 14814
Rx Only
Revised: December 2022 CLON-AV-PI-00
8021569
Mechanism of Action
Epidurally administered clonidine produces dose-dependent analgesia not antagonized by opiate antagonists. The analgesia is limited to the body regions innervated by the spinal segments where analgesic concentrations of clonidine are present. Clonidine is thought to produce analgesia at presynaptic and postjunctional alpha-2-adrenoceptors in the spinal cord by preventing pain signal transmission to the brain.
Clonidine - Clonidine injection, Solution PubMed™ news
- Journal Article • 2026 MaySafety of clonidine and dexmedetomidine in peripheral nerve blocks: interpreting preclinical safety data. Comment on Br J Anaesth 2026; 136: 255-65.
- Journal Article • 2026 MayActivation of TGF-β/ALK5/SMAD signaling alleviates behavioral and neurochemical deficits in tramadol withdrawal.
- Journal Article • 2026 MayPresentation and management of acute medetomidine withdrawal.
- Journal Article • 2026 MayBeneficial effects of the rapid vs. standard procedure for injection naltrexone initiation operate through increased adjunctive medication use.
- Journal Article • 2026 MayEffects of noradrenergic blockade on emotional working memory and its neural underpinnings: A randomized, double-blind, placebo-controlled trial.