Get your patient on Desmoda (Desmopressin Acetate Oral Solution)
Desmoda prescribing information
INDICATIONS AND USAGE
DESMODA is indicated for the management of central diabetes insipidus as antidiuretic replacement therapy for adults and pediatric patients. Limitations of Use • DESMODA is not indicated for the treatment of nephrogenic diabetes insipidus.
DOSAGE AND ADMINISTRATION
2.1 Recommended Dosage for Central Diabetes Insipidus
• Instruct patients about appropriate fluid restriction during DESMODA treatment due to risk of hyponatremia [see Warnings and Precautions (5.1)]. • Individualize the dosage of DESMODA for each patient and adjust the dosage according to the diurnal pattern of response. Estimate patient response by adequate duration of sleep and water turnover. • Recommended starting dosage of DESMODA for adults and pediatric patients is 0.05 mg orally twice daily. • Titrate the daily dosage as needed to obtain an adequate antidiuretic response. • Administer DESMODA on an empty stomach, at least 1 hour prior to or 2 hours after food. • Administer DESMODA using an oral syringe provided by the pharmacy. • Monitor response by measuring urine volume and osmolarity. Monitoring measurements of plasma osmolarity may also be useful.
2.2 Switching Patients with Central Diabetes Insipidus to DESMODA From Desmopressin Acetate Nasal Spray
• For patients with central diabetes insipidus switching to DESMODA from desmopressin acetate nasal spray, wait twelve hours after the last dose. • Monitor patients closely during the initial dose titration period.
DOSAGE FORMS AND STRENGTHS
Oral solution: 0.05 mg desmopressin acetate in 1 mL (0.05 mg/mL)
USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Risk Summary Available data on the use of desmopressin acetate during pregnancy over decades of use have not identified a drug associated risk of major birth defects, miscarriage or adverse maternal or fetal outcomes. There are risks associated with untreated central diabetes insipidus during pregnancy (see Clinical Considerations). In vitro studies with human placenta demonstrate poor placental transfer of desmopressin. No adverse developmental outcomes were observed in animal reproduction studies with administration of desmopressin during organogenesis to pregnant rats and rabbits at doses approximately <1 to 38 times, respectively, the maximum recommended human dose based on body surface areas (mg/m2) (see Data). The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Clinical Considerations Disease Associated Maternal and Embryo-Fetal Risk There are risks associated with untreated central diabetes insipidus during pregnancy such as dehydration, preterm birth and oligohydramnios. Pregnant patients with diabetes insipidus should be monitored for electrolyte imbalance, maternal hypotension, and low amniotic fluid levels.
Data Animal Data In a developmental toxicity study in rats, desmopressin acetate was administered intravenously at doses of 9.68, 48.4, or 241 mcg/kg/day during the period of organogenesis (gestations days 7 to 17). Laparohysterectomy for fetal examinations were conducted on gestation day 20 for twenty females in each group; the remaining 10 females were allowed to litter in order to determine any postnatal effects that might be attributable to pre-natal treatment. No effects were seen on maternal and fetal survival, growth and morphology or post-natal offspring survival, growth, development, behavior and reproductive performance up to 241 mcg/kg/day (4 times a 0.6 mg dose received by a 60 kg patient based on body surface area).
In an embryo-fetal development study and a pre- and postnatal development study in rabbits, desmopressin acetate was administered subcutaneously at doses of 2, 20 or 200 mcg/kg/day (embryo-fetal development) and 0.1, 1 or 10 mcg/kg/day (pre- and postnatal development) during the period of organogenesis (gestation days 6 to 18). No effects on maternal and fetal survival or morphology were observed in both studies at doses of up to 200 mcg/kg/day (6.5 times a 0.6 mg dose received by a 60 kg patient based on body surface area) nor were there effects in the pre- and postnatal development study on parturition, postnatal survival, growth, development or behavior, up to the highest dose tested of 10 mcg/kg/day (0.3 times a 0.6 mg dose received by a 60 kg patient, based on body surface area).
8.2 Lactation
Risk Summary Breastfeeding is not expected to result in clinically relevant exposure of the infant to desmopressin following maternal administration. Desmopressin is transferred into human breastmilk at negligible amounts (see Data). There is no information on the effects of desmopressin on the breastfed infant or on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for DESMODA and any potential adverse effects on the breastfed infant from DESMODA or from the underlying maternal condition.
Data A trial was conducted in six healthy lactating women, at greater than 4 months postpartum, to evaluate intranasal administration of 300 mcg single dose of desmopressin acetate. Samples of maternal plasma and breastmilk were obtained at 0, 30, 60, 120, 240, 360 and 480 min after the drug administration. At 8 hours after dose intake, the levels in the milk ranged between 4.16 and 101 pg/ml, and the plasma levels ranged between 40 and 242 pg/ml. The total amount of desmopressin present in the milk over the 8 hours ranged between 491 pg and 16 ng, which corresponds to 0.0001 to 0.005% of the administered dose to the breastfeeding mother.
8.4 Pediatric Use
Desmopressin acetate is indicated for the management of central diabetes insipidus as antidiuretic replacement therapy in pediatric patients. Use in pediatric patients requires careful fluid intake restriction to prevent possible water intoxication with hyponatremia. In younger pediatric patients, the dose must be individually adjusted to prevent an excessive decrease in plasma osmolality leading to hyponatremia and possible convulsions. Fluid restriction should be discussed with the patient and/or guardian [see Warnings and Precautions (5.2)].
DESMODA contains benzoic acid, a metabolite of benzyl alcohol. Serious adverse reactions, including fatal reactions, of new onset or worsening metabolic acidosis that progressed to neurotoxicity, and in some cases gasping syndrome, have been reported in low-birth weight neonates and preterm neonates who received benzyl alcohol-containing drugs intravenously (DESMODA is not approved for intravenous use [see Dosage and Administration (2.1)]). Gasping syndrome is a life-threatening condition in neonates caused by benzyl alcohol toxicity that is characterized by new onset or worsening metabolic acidosis with gradual neurological deterioration, seizures, intracranial hemorrhage, hematologic abnormalities, skin breakdown, hepatic and kidney failure, hypotension, bradycardia, and gasping respirations followed by death. In reported cases, benzyl alcohol in amounts of 99 to 234 mg/kg/day produced blood BA levels of 6.6 to 14.9 mg/dL, but the minimum amount of benzyl alcohol at which gasping syndrome may occur in neonates is not known [see Warnings and Precautions (5.4)]. The rate at which benzyl alcohol is metabolized to benzoic acid cannot be reliably predicted, and the relationship between systemic levels of benzoic acid and toxicity is not well-characterized.
DESMODA contains 2.74 mg of benzoic acid per mL [see Warnings and Precautions (5.4)].
8.5 Geriatric Use
Because geriatric patients are more likely to have decreased renal function, care should be taken in dose selection and monitoring renal function is recommended [see Clinical Pharmacology (12.3)].
Use of DESMODA in geriatric patients requires careful fluid intake restriction to prevent possible water intoxication with hyponatremia [see Warnings and Precautions (5.1)].
8.6 Renal Impairment
Desmopressin acetate is substantially excreted by the kidney, and the risk of adverse events may be greater in patients with renal impairment than patients with normal renal function. Desmopressin acetate is contraindicated in patients with estimated CLcr by Cockcroft Gault equation less than 50 mL/min [see Contraindications (4), Clinical Pharmacology (12.3)].
CONTRAINDICATIONS
DESMODA is contraindicated in patients with: •Hyponatremia or a history of hyponatremia [see Warnings and Precautions (5.1)]. •Hypersensitivity to desmopressin acetate or any of the inactive ingredients of DESMODA.Reactions have included anaphylaxis [see Warnings and Precautions (5.3)]. •Moderate to severe renal impairment (defined as creatinine clearance (CLcr) less than 50 mL/min)[see Use in Specific Populations (8.6)].
WARNINGS AND PRECAUTIONS
5.1 Hyponatremia
Excessive fluid intake when urine output is limited by the antidiuretic effect of desmopressin may lead to water intoxication with hyponatremia. Cases of hyponatremia have been reported from postmarketing experience in patients treated with desmopressin acetate. Unless properly diagnosed and treated hyponatremia can be fatal.
Observe all patients receiving DESMODA for the following signs or symptoms associated with hyponatremia: headache, nausea/vomiting, decreased serum sodium, weight gain, restlessness, fatigue, lethargy, disorientation, depressed reflexes, loss of appetite, irritability, muscle weakness, muscle spasms or cramps and abnormal mental status such as hallucinations, decreased consciousness and confusion. Severe symptoms due to an extreme decrease in serum sodium and plasma osmolality may include one or a combination of the following: seizure, coma and/or respiratory arrest.
In order to decrease the risk of water intoxication with hyponatremia, fluid restriction is recommended. Careful fluid intake is particularly important in pediatric and geriatric patients because these patients are at greater risk of developing hyponatremia [see Use in Specific Populations (8.4, 8.5)]. More frequent monitoring of serum sodium levels is recommended in the following patients: those with conditions associated with fluid and electrolyte imbalance, such as cystic fibrosis, heart failure, renal disorders, habitual or psychogenic polydipsia or those taking concomitant drugs that may cause hyponatremia [see Drug Interactions (7.1)].
Temporarily stop treatment with DESMODA during acute intercurrent illness characterized by fluid and/or electrolyte imbalance (e.g., systemic infections, fever, recurrent vomiting or diarrhea) or under conditions of extremely hot weather, vigorous exercise or other conditions associated with increased water intake.
5.2 Fluid Retention
Desmopressin acetate can cause fluid retention, which can worsen underlying conditions that are susceptible to volume status. Closely monitor patients with heart failure or uncontrolled hypertension. DESMODA is not recommended in patients at risk for increased intracranial pressure or those with a history of urinary retention.
5.3 Hypersensitivity Reactions
Hypersensitivity reactions including anaphylaxis have been reported with intravenous and nasal administration of desmopressin acetate, including cases of fatal anaphylaxis with intravenous desmopressin acetate [see Adverse Reactions (6)]. DESMODA is contraindicated in patients with a history of hypersensitivity to desmopressin acetate or any of the inactive ingredients of DESMODA [see Contraindications (4)]. If signs or symptoms of hypersensitivity reactions occur, discontinue DESMODA and initiate appropriate supportive care.
5.4 Risk of Benzyl Alcohol Toxicity in Neonates DESMODA contains 2.74 mg/mL of benzoic acid, a metabolite of benzyl alcohol. Serious adverse reactions of metabolic acidosis, including fatalities, have been reported in low-birth-weight neonates (less than 2,500 grams) and preterm neonates (gestational age less than 34 weeks) who received benzyl alcohol-containing drugs intravenously. The relationship between systemic levels of benzoic acid and toxicity is not well-characterized [see Use in Specific Populations (8.4)]. Use DESMODA with caution in low-birth-weight neonates or preterm neonates and monitor for signs and symptoms of metabolic acidosis.
ADVERSE REACTIONS
The following serious adverse reactions are described below and elsewhere in the labeling: •Hyponatremia [see Warnings and Precautions (5.1)]
•Fluid Retention [see Warnings and Precautions (5.2)]
•Hypersensitivity [see Warnings and Precautions (5.3)]
•Risk of Benzyl Alcohol Toxicity in Neonates [see Warnings and Precautions (5.4)]
The following adverse reactions associated with the use of desmopressin acetate were identified in clinical studies or postmarketing reports. Because some of these reactions were reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Cardiac disorders: hypertension Gastrointestinal disorders: nausea, vomiting, diarrhea, constipation, abdominal cramps General disorders: headache, malaise, drug ineffective, edema, fatigue Hepatobiliary disorders: transient increases in AST (1.5 times the upper limit of normal) Immune system disorders: severe allergic reactions, anaphylaxis has occurred with other formulations of desmopressin Metabolism and nutrition: dehydration, hyponatremia, water intoxication with hyponatremia Nervous system disorders: hyponatremic convulsions, hyponatremic convulsions associated with concomitant use of the following medications: oxybutynin and imipramine [see Drug Interactions (7.1)], asthenia, coma, disturbance in attention, psychomotor hyperactivity, dizziness, somnolence, depressed level of consciousness, falls. Psychiatric disorders: confusional state, abnormal behavior, emotional disorder, depression, hallucination, insomnia Renal and urinary disorders: bladder and urethral symptoms, including urinary retention, urine flow decreased, dysuria Skin and subcutaneous tissue disorders: rash, dermatitis allergic, sweating, flushing, urticaria Respiratory, thoracic and mediastinal disorders: dyspnea, epistaxis
In long-term clinical studies in which patients with diabetes insipidus were followed for periods up to 44 months of desmopressin acetate oral therapy, transient increases in AST (SGOT) no higher than 1.5 times the upper limit of normal were occasionally observed. Elevated AST (SGOT) returned to the normal range despite the continued use of desmopressin acetate oral therapy.
DRUG INTERACTIONS
7.1 Other Drugs that may Increase Risk of Hyponatremia Concomitant administration of DESMODA with other drugs that may increase the risk of water intoxication with hyponatremia, (e.g., tricyclic antidepressants, selective serotonin re-uptake inhibitors, chlorpromazine, opiate analgesics, thiazide diuretics, NSAIDs, lamotrigine, sulfonylureas, particularly chlorpropamide, oxybutynin and carbamazepine). Monitor serum sodium more frequently in patients taking DESMODA concomitantly with these drugs and when doses of these drugs are increased [see Warnings and Precautions (5.1), Adverse Reactions (6)].
7.2 Other Vasoconstrictors Desmopressin acetate can elevate blood pressure. Use of large doses of DESMODA with other vasoconstrictors may require a reduction of the DESMODA dosage [see Adverse Reactions (6)].
DESCRIPTION
DESMODA oral solution contains active moiety desmopressin, an analog of natural pituitary hormone 8-arginine vasopressin (antidiuretic hormone), in the form of acetate salt. The chemical name of desmopressin acetate is 1-desamino-8-D-arginine vasopressin acetate. Desmopressin acetate has a molecular weight of 1129.30 g/mol, an empirical formula of C 46 H 64 N 14 O 12 S 2 ·C 2 H 4 O 2 , and structural formula:
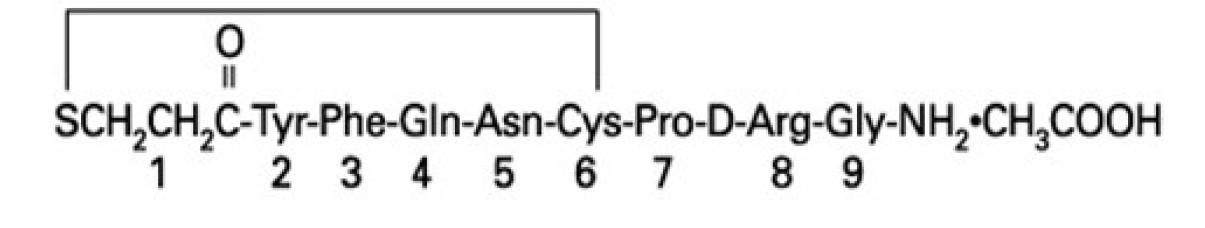
Desmopressin acetate is white amorphous powder and is soluble in water.
DESMODA oral solution: Each mL contains 0.05 mg of desmopressin acetate (equivalent to 0.047 mg of desmopressin free base) as active ingredient. The inactive ingredients include benzoic acid and sodium benzoate as buffering agents and antimicrobial agents, and purified water. The pH of the oral solution is 4.8 to 5.2.
CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Desmopressin acetate’s primary pharmacodynamic action involves its binding to vasopressin 2 (V2) receptors. V2 receptors are primarily located in the distal convoluted tubule and collecting ducts of the nephron in the kidneys. These receptors play a crucial role in regulating water reabsorption and urine concentration. By influencing the permeability of the renal tubules, V2 receptors help maintain the body’s water balance and overall homeostasis.
12.2 Pharmacodynamics
Dose response studies in patients with diabetes insipidus following desmopressin acetate tablets 0.025 mg to 0.4 mg produced clinically significant antidiuretic effects. In most patients, doses of 0.1 mg to 0.2 mg produced optimal antidiuretic effects lasting up to eight hours. With doses of 0.4 mg, antidiuretic effects were observed for up to 12 hours; measurements beyond 12 hours were not recorded.
Following administration of desmopressin acetate tablets, the onset of antidiuretic effect occurs at around 1 hour, and it reaches a maximum at about 4 to 7 hours based on the measurement of increased urine osmolality.
12.3 Pharmacokinetics
Following a single oral administration of DESMODA in healthy subjects at 0.6 mg, mean maximum concentration (SD) is 82 (33) pg/mL, and mean total systemic exposure (SD) is 314 (138) (hrs∙pg/mL).
Absorption Desmopressin absolute oral bioavailability is 0.16%. Desmopressin area under the plasma drug concentration time curve (AUC) is reduced by 95% following administration of the oral solution compared to the intranasal formulation.
Effect of Food DESMODA Cmax was decreased 72% and the AUC was decreased 64% following administration of 0.6 mg DESMODA with a high-fat meal (1000 calories, 50% fat).
Distribution DESMODA mean apparent (oral) volume of distribution (SD) is 11717 (5086) L.
Elimination Desmopressin is mainly excreted in the urine. Desmopressin estimated elimination half-life is 3.6 hours. DESMODA mean apparent (oral) clearance (SD) is 2264 (940) L/hr.
Specific Populations Renal Impairment A pharmacokinetic study was conducted in subjects with normal renal function and patients with mild, moderate, and severe renal impairment (n=24, 6 subjects each group) with a single dose of 2 mcg desmopressin acetate intravenous injection. The geometric mean terminal half-life was 2.8 hours in subjects with normal renal function, and 4, 6.6, and 8.7 hours in patients with mild, moderate, and severe renal impairment, respectively. In patients with mild, moderate and severe renal impairment, mean desmopressin AUC was 1.5-fold, 2.4-fold and 3.6-fold higher, respectively, compared to that of subjects with normal renal function.
NONCLINICAL TOXICOLOGY
Long-term carcinogenicity studies with DESMODA in animals to evaluate the carcinogenic potential of desmopressin acetate have not been performed. Desmopressin was not mutagenic in bacterial mutagenicity (AMES) and mouse lymphoma assays. Studies to evaluate animal fertility have not been performed.
CLINICAL STUDIES
The effectiveness of DESMODA was supported by dose response studies of desmopressin acetate tablets in patients with diabetes insipidus. These studies demonstrated that oral doses of 0.025 mg to 0.4 mg of desmopressin acetate tablets produced clinically significant antidiuretic effects. In patients treated with desmopressin acetate tablets, doses of 0.1 mg to 0.2 mg produced optimal antidiuretic effects lasting up to eight hours [see Clinical Pharmacology (12.2)].
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied DESMODA (desmopressin acetate) oral solution is a clear, colorless to slightly yellow colored solution supplied in an amber glass bottle:
| Strength | Volume in Bottle | NDC |
| 0.05 mg/mL | 145 mL | 71863-123-14 |
Storage and Handling Store at 2°C to 25°C (36°F to 77°F). Excursions permitted to 30°C (86°F) [see USP refrigerated and controlled room temperature]. Do not freeze. Discard any unused DESMODA oral solution after 120 days after first opening the bottle.
12.1 Mechanism of Action
Desmopressin acetate’s primary pharmacodynamic action involves its binding to vasopressin 2 (V2) receptors. V2 receptors are primarily located in the distal convoluted tubule and collecting ducts of the nephron in the kidneys. These receptors play a crucial role in regulating water reabsorption and urine concentration. By influencing the permeability of the renal tubules, V2 receptors help maintain the body’s water balance and overall homeostasis.