Get your patient on Famotidine - Famotidine injection, Solution (Famotidine)
Famotidine - Famotidine injection, Solution prescribing information
INDICATIONS AND USAGE
Famotidine Injection, supplied as a concentrated solution for intravenous injection, is intended for intravenous use only. Famotidine Injection is indicated in some hospitalized patients with pathological hypersecretory conditions or intractable ulcers, or as an alternative to the oral dosage forms for short term use in patients who are unable to take oral medication for the following conditions:
- Short term treatment of active duodenal ulcer . Most adult patients heal within 4 weeks; there is rarely reason to use famotidine at full dosage for longer than 6 to 8 weeks. Studies have not assessed the safety of famotidine in uncomplicated active duodenal ulcer for periods of more than 8 weeks.
- Maintenance therapy for duodenal ulcer patients at reduced dosage after healing of an active ulcer. Controlled studies in adults have not extended beyond one year.
- Short term treatment of active benign gastric ulcer. Most adult patients heal within 6 weeks. Studies have not assessed the safety or efficacy of famotidine in uncomplicated active benign gastric ulcer for periods of more than 8 weeks.
- Short term treatment of gastroesophageal reflux disease (GERD). Famotidine is indicated for short term treatment of patients with symptoms of GERD (see CLINICAL PHARMACOLOGY IN ADULTS, Clinical Studies ). Famotidine is also indicated for the short term treatment of esophagitis due to GERD including erosive or ulcerative disease diagnosed by endoscopy (see CLINICAL PHARMACOLOGY IN ADULTS, Clinical Studies ).
- Treatment of pathological hypersecretory conditions (e.g., Zollinger-Ellison Syndrome, multiple endocrine adenomas) (see CLINICAL PHARMACOLOGY IN ADULTS, Clinical Studies ).
DOSAGE AND ADMINISTRATION
In some hospitalized patients with pathological hypersecretory conditions or intractable ulcers, or in patients who are unable to take oral medication, Famotidine Injection may be administered until oral therapy can be instituted.
The recommended dosage for Famotidine Injection in adult patients is 20 mg intravenously q 12 h.
The doses and regimen for parenteral administration in patients with GERD have not been established.
Dosage for Pediatric Patients <1 Year of Age Gastroesophageal Reflux Disease (GERD)
See PRECAUTIONS, Pediatric Patients<1 Year of Age .
The studies described in PRECAUTIONS, Pediatric Patients <1 Year of Age suggest the following starting doses in pediatric patients <1 year of age: Gastroesophageal Reflux Disease (GERD) – 0.5 mg/kg/dose of famotidine oral suspension for the treatment of GERD for up to 8 weeks once daily in patients <3 months of age and 0.5 mg/kg/dose twice daily in patients 3 months to <1 year of age. Patients should also be receiving conservative measures (e.g., thickened feedings). The use of intravenous famotidine in pediatric patients <1 year of age with GERD has not been adequately studied.
Dosage for Pediatric Patients 1 to 16 Years of Age
See PRECAUTIONS, Pediatric Patients 1 to 16 Years of Age .
The studies described in PRECAUTIONS, Pediatric Patients 1 to 16 Years of Age suggest that the starting dose in pediatric patients 1 to 16 years of age is 0.25 mg/kg intravenously (injected over a period of not less than two minutes or as a 15-minute infusion) q 12 h up to 40 mg/day.
While published uncontrolled clinical studies suggest effectiveness of famotidine in the treatment of peptic ulcer, data in pediatric patients are insufficient to establish percent response with dose and duration of therapy. Therefore, treatment duration (initially based on adult duration recommendations) and dose should be individualized based on clinical response and/or gastric pH determination and endoscopy. Published uncontrolled studies in pediatric patients 1 to 16 years of age have demonstrated gastric acid suppression with doses up to 0.5 mg/kg intravenously q 12 h.
Dosage Adjustments for Patients with Moderate or Severe Renal Insufficiency
In adult patients with moderate (creatinine clearance <50 mL/min) or severe (creatinine clearance <10 mL/min) renal insufficiency, the elimination half-life of famotidine is increased. For patients with severe renal insufficiency, it may exceed 20 hours, reaching approximately 24 hours in anuric patients. Since CNS adverse effects have been reported in patients with moderate and severe renal insufficiency, to avoid excess accumulation of the drug in patients with moderate or severe renal insufficiency, the dose of Famotidine Injection may be reduced to half the dose, or the dosing interval may be prolonged to 36 to 48 hours as indicated by the patient's clinical response.
Based on the comparison of pharmacokinetic parameters for famotidine in adults and pediatric patients, dosage adjustment in pediatric patients with moderate or severe renal insufficiency should be considered.
Pathological Hypersecretory Conditions (e.g., Zollinger-Ellison Syndrome, Multiple Endocrine Adenomas)
The dosage of famotidine in patients with pathological hypersecretory conditions varies with the individual patient. The recommended adult intravenous dose is 20 mg q 12 h. Doses should be adjusted to individual patient needs and should continue as long as clinically indicated. In some patients, a higher starting dose may be required. Oral doses up to 160 mg q 6 h have been administered to some adult patients with severe Zollinger-Ellison Syndrome.
To prepare intravenous solutions, aseptically dilute 2 mL of Famotidine Injection (solution containing 10 mg/mL) with Sodium Chloride Injection 0.9% or other compatible intravenous solution (see Stability ) to a total volume of either 5 mL or 10 mL and inject over a period of not less than 2 minutes.
To prepare intravenous infusion solutions, aseptically dilute 2 mL of Famotidine Injection with 100 mL of Dextrose 5% or other compatible solution (see Stability ), and infuse over a 15 to 30 minute period.
Concomitant Use of Antacids
Antacids may be given orally concomitantly if needed.
Stability
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration whenever solution and container permit.
When added to or diluted with most commonly used intravenous solutions, e.g., Water for Injection, Sodium Chloride Injection 0.9%, Dextrose Injection 5% and 10% or Lactated Ringer's Injection, diluted Famotidine Injection is physically and chemically stable (i.e., maintains at least 90% of initial potency) for 7 days at room temperature – see HOW SUPPLIED, Storage .
When added to or diluted with Sodium Bicarbonate Injection 5%, Famotidine Injection at a concentration of 0.2 mg/mL (the recommended concentration of famotidine intravenous infusion solutions) is physically and chemically stable (i.e., maintains at least 90% of initial potency) for 7 days at room temperature – see HOW SUPPLIED, Storage . However, a precipitate may form at higher concentrations of Famotidine Injection (>0.2 mg/mL) in Sodium Bicarbonate Injection 5%.
CONTRAINDICATIONS
Hypersensitivity to any component of these products. Cross sensitivity in this class of compounds has been observed. Therefore, Famotidine Injection should not be administered to patients with a history of hypersensitivity to other H 2 –receptor antagonists.
ADVERSE REACTIONS
To report SUSPECTED ADVERSE REACTIONS, contact Fresenius Kabi USA, LLC at 1-800- 551-7176 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
The adverse reactions listed below have been reported during domestic and international clinical trials in approximately 2,500 patients. In those controlled clinical trials in which famotidine tablets were compared to placebo, the incidence of adverse experiences in the group which received famotidine tablets, 40 mg at bedtime, was similar to that in the placebo group.
The following adverse reactions have been reported to occur in more than 1% of patients on therapy with famotidine in controlled clinical trials, and may be causally related to the drug: headache (4.7%), dizziness (1.3%), constipation (1.2%) and diarrhea (1.7%).
The following other adverse reactions have been reported infrequently in clinical trials or since the drug was marketed. The relationship to therapy with famotidine has been unclear in many cases. Within each category the adverse reactions are listed in order of decreasing severity.
Body as a Whole: fever, asthenia, fatigue
Cardiovascular: arrhythmia, AV block, palpitation, prolonged QT interval
Gastrointestinal: cholestatic jaundice, hepatitis, elevated liver enzyme, vomiting, nausea, abdominal discomfort, anorexia, dry mouth
Hematologic: agranulocytosis, pancytopenia, leukopenia, thrombocytopenia
Hypersensitivity: anaphylaxis, angioedema, orbital or facial edema, urticaria, rash, conjunctival injection, bronchospasm
Musculoskeletal: rhabdomyolysis, musculoskeletal pain, muscle cramps, arthralgia
Nervous System/Psychiatric: seizure, hallucinations, confusion, agitation, depression, anxiety, decreased libido; paresthesia; insomnia; somnolence.
Respiratory: interstitial pneumonia
Skin: toxic epidermal necrolysis/Stevens Johnson syndrome, pruritus, dry skin, flushing
Special Senses: tinnitus, taste disorder
Other: impotence
The adverse reactions reported for Famotidine Tablets may also occur with Famotidine for Oral Suspension or Famotidine Injection. In addition, transient irritation at the injection site has been observed with Famotidine Injection.
Pediatric Patients
In a clinical study in 35 pediatric patients < 1 year of age with GERD symptoms [e.g. vomiting (spitting up), irritability (fussing)], agitation was observed in 5 patients on famotidine that resolved when the medication was discontinued.
Drug Interactions
No drug interactions have been identified. Studies with famotidine in man, in animal models, and in vitro have shown no significant interference with the disposition of compounds metabolized by the hepatic microsomal enzymes, e.g., cytochrome P450 system. Compounds tested in man include warfarin, theophylline, phenytoin, diazepam, aminopyrine and antipyrine. Indocyanine green as an index of hepatic drug extraction has been tested and no significant effects have been found.
DESCRIPTION
The active ingredient in Famotidine Injection, USP is a histamine H 2 –receptor antagonist. Famotidine is [1-Amino-3-[[[2- [(diaminomethylene)amino]-4-thiazolyl] methyl]thio]propylidene] sulfamide. Its structural formula is:
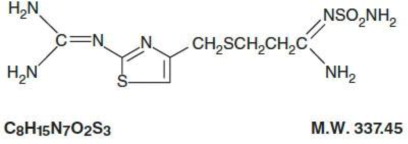
Famotidine is a white to pale yellow crystalline compound that is freely soluble in glacial acetic acid, slightly soluble in methanol, very slightly soluble in water, and practically insoluble in ethanol.
Famotidine Injection, USP is supplied as a sterile concentrated solution for intravenous injection. Each mL of the solution contains 10 mg of famotidine and the following inactive ingredients: L-aspartic acid 4 mg, mannitol 20 mg, Water for Injection q.s. 1 mL.
CLINICAL PHARMACOLOGY IN ADULTS
GI Effects
Famotidine is a competitive inhibitor of histamine H 2 –receptors. The primary clinically important pharmacologic activity of famotidine is inhibition of gastric secretion. Both the acid concentration and volume of gastric secretion are suppressed by famotidine, while changes in pepsin secretion are proportional to volume output.
In normal volunteers and hypersecretors, famotidine inhibited basal and nocturnal gastric secretion, as well as secretion stimulated by food and pentagastrin. After oral administration, the onset of the antisecretory effect occurred within one hour; the maximum effect was dose-dependent, occurring within one to three hours. Duration of inhibition of secretion by doses of 20 and 40 mg was 10 to 12 hours.
After intravenous administration, the maximum effect was achieved within 30 minutes. Single intravenous doses of 10 and 20 mg inhibited nocturnal secretion for a period of 10 to 12 hours. The 20 mg dose was associated with the longest duration of action in most subjects.
Single evening oral doses of 20 and 40 mg inhibited basal and nocturnal acid secretion in all subjects; mean nocturnal gastric acid secretion was inhibited by 86% and 94%, respectively, for a period of at least 10 hours. The same doses given in the morning suppressed food-stimulated acid secretion in all subjects. The mean suppression was 76% and 84%, respectively, 3 to 5 hours after administration, and 25% and 30%, respectively, 8 to 10 hours after administration. In some subjects who received the 20 mg dose, however, the antisecretory effect was dissipated within 6 to 8 hours. There was no cumulative effect with repeated doses. The nocturnal intragastric pH was raised by evening doses of 20 and 40 mg of famotidine to mean values of 5.0 and 6.4, respectively. When famotidine was given after breakfast, the basal daytime interdigestive pH at 3 and 8 hours after 20 or 40 mg of famotidine was raised to about 5.
Famotidine had little or no effect on fasting or postprandial serum gastrin levels. Gastric emptying and exocrine pancreatic function were not affected by famotidine.
Other Effects
Systemic effects of famotidine in the CNS, cardiovascular, respiratory or endocrine systems were not noted in clinical pharmacology studies. Also, no antiandrogenic effects were noted. (See ADVERSE REACTIONS .) Serum hormone levels, including prolactin, cortisol, thyroxine (T 4 ) and testosterone, were not altered after treatment with famotidine.
Pharmacokinetics
Orally administered famotidine is incompletely absorbed, and its bioavailability is 40 to 45%.
Famotidine undergoes minimal first-pass metabolism. After oral doses, peak plasma levels occur in 1 to 3 hours. Plasma levels after multiple doses are similar to those after single doses. Fifteen to 20% of famotidine in plasma is protein bound. Famotidine has an elimination half-life of 2.5 to 3.5 hours.
Famotidine is eliminated by renal (65 to 70%) and metabolic (30 to 35%) routes. Renal clearance is 250 to 450 mL/min, indicating some tubular excretion. Twenty-five to 30% of an oral dose and 65 to 70% of an intravenous dose are recovered in the urine as unchanged compound. The only metabolite identified in man is the S-oxide.
There is a close relationship between creatinine clearance values and the elimination half-life of famotidine. In patients with severe renal insufficiency, i.e., creatinine clearance less than 10 mL/min, the elimination half-life of famotidine may exceed 20 hours and adjustment of dose or dosing intervals in moderate and severe renal insufficiency may be necessary (see PRECAUTIONS , DOSAGE AND ADMINISTRATION ).
In elderly patients, there are no clinically significant age-related changes in the pharmacokinetics of famotidine.
However, in elderly patients with decreased renal function, the clearance of the drug may be decreased (see PRECAUTIONS, Geriatric Use ).
Clinical Studies
The majority of clinical study experience involved oral administration of famotidine tablets, and is provided herein for reference.
Duodenal Ulcer
In a U.S. multicenter, double-blind study in outpatients with endoscopically confirmed duodenal ulcer, orally administered famotidine was compared to placebo. As shown in Table 1 , 70% of patients treated with famotidine 40 mg h.s. were healed by week 4.
•Statistically significantly different than placebo (p<0.001) | |||
| Outpatients with Endoscopically Confirmed Healed Duodenal Ulcers | |||
| Famotidine | Famotidine | Placebo | |
| 40 mg h.s. | 20 mg b.i.d. | h.s. | |
| (N=89) | (N=84) | (N=97) | |
| Week 2 | •32% | • 38% | 17% |
| Week 4 | •70% | • 67% | 31% |
Patients not healed by week 4 were continued in the study. By week 8, 83% of patients treated with famotidine had healed versus 45% of patients treated with placebo. The incidence of ulcer healing with famotidine was significantly higher than with placebo at each time point based on proportion of endoscopically confirmed healed ulcers.
In this study, time to relief of daytime and nocturnal pain was significantly shorter for patients receiving famotidine than for patients receiving placebo; patients receiving famotidine also took less antacid than the patients receiving placebo.
Long-Term Maintenance Treatment of Duodenal Ulcers
Famotidine, 20 mg p.o. h.s. was compared to placebo h.s. as maintenance therapy in two double-blind, multicenter studies of patients with endoscopically confirmed healed duodenal ulcers. In the U.S. study the observed ulcer incidence within 12 months in patients treated with placebo was 2.4 times greater than in the patients treated with famotidine. The 89 patients treated with famotidine had a cumulative observed ulcer incidence of 23.4% compared to an observed ulcer incidence of 56.6% in the 89 patients receiving placebo (p<0.01). These results were confirmed in an international study where the cumulative observed ulcer incidence within 12 months in the 307 patients treated with famotidine was 35.7%, compared to an incidence of 75.5% in the 325 patients treated with placebo (p<0.01).
Gastric Ulcer
In both a U.S. and an international multicenter, double-blind study in patients with endoscopically confirmed active benign gastric ulcer, orally administered famotidine, 40 mg h.s., was compared to placebo h.s. Antacids were permitted during the studies, but consumption was not significantly different between the famotidine and placebo groups. As shown in Table 2 , the incidence of ulcer healing (dropouts counted as unhealed) with famotidine was statistically significantly better than placebo at weeks 6 and 8 in the U.S. study, and at weeks 4, 6 and 8 in the international study, based on the number of ulcers that healed, confirmed by endoscopy.
•••, † Statistically significantly better than placebo (p≤0.05, p≤0.01, respectively) | ||||
| Patients with Endoscopically Confirmed Healed Gastric Ulcers | ||||
| U.S. Study | International Study | |||
| Famotidine | Placebo | Famotidine | Placebo | |
| 40 mg h.s. | h.s. | 40 mg h.s. | h.s. | |
| (N=74) | (N=75) | (N=149) | (N=145) | |
| Week 4 | 45% | 39% | † 47% | 31% |
| Week 6 | † 66% | 44% | † 65% | 46% |
| Week 8 | •••78% | 64% | † 80% | 54% |
Time to complete relief of daytime and nighttime pain was statistically significantly shorter for patients receiving famotidine than for patients receiving placebo; however, in neither study was there a statistically significant difference in the proportion of patients whose pain was relieved by the end of the study (week 8).
Gastroesophageal Reflux Disease (GERD)
Orally administered famotidine was compared to placebo in a U.S. study that enrolled patients with symptoms of GERD and without endoscopic evidence of erosion or ulceration of the esophagus. Famotidine 20 mg b.i.d. was statistically significantly superior to 40 mg h.s. and to placebo in providing a successful symptomatic outcome, defined as moderate or excellent improvement of symptoms (Table 3 ).
†† p≤0.01 vs placebo | |||
| % Successful Symptomatic Outcome | |||
| Famotidine 20 mg b.i.d. | Famotidine 40 mg h.s. | Placebo | |
| (N=154) | (N=149) | (N=73) | |
| Week 6 | 82 †† | 69 | 62 |
By two weeks of treatment, symptomatic success was observed in a greater percentage of patients taking famotidine 20 mg b.i.d. compared to placebo (p≤0.01).
Symptomatic improvement and healing of endoscopically verified erosion and ulceration were studied in two additional trials. Healing was defined as complete resolution of all erosions or ulcerations visible with endoscopy. The U.S. study comparing famotidine 40 mg p.o. b.i.d. to placebo and famotidine 20 mg p.o. b.i.d., showed a significantly greater percentage of healing for famotidine 40 mg b.i.d. at weeks 6 and 12 (Table 4 ).
††† p≤0.01 vs placebo | |||
‡ p ≤ 0.05 vs famotidine 20 mg b.i.d. | |||
‡‡ p≤0.01 vs famotidine 20 mg b.i.d. | |||
| % Endoscopic Healing – U.S. Study | |||
| Famotidine 40 mg b.i.d. | Famotidine 20 mg b.i.d. | Placebo | |
| (N=127) | (N=125) | (N=66) | |
| Week 6 | 48 †††, ‡‡ | 32 | 18 |
| Week 12 | 69 †††, ‡ | 54 ††† | 29 |
As compared to placebo, patients who received famotidine had faster relief of daytime and nighttime heartburn and a greater percentage of patients experienced complete relief of nighttime heartburn.
These differences were statistically significant.
In the international study, when famotidine 40 mg p.o. b.i.d. was compared to ranitidine 150 mg p.o. b.i.d., a statistically significantly greater percentage of healing was observed with famotidine 40 mg b.i.d. at week 12 (Table 5 ). There was, however, no significant difference among treatments in symptom relief.
‡‡‡ p≤0.05 vs Ranitidine 150 mg b.i.d. | |||
| % Endoscopic Healing - International Study | |||
| Famotidine 40 mg b.i.d. | Famotidine 20 mg b.i.d. | Ranitidine 150 mg b.i.d. | |
| (N=175) | (N=93) | (N=172) | |
| Week 6 | 48 | 52 | 42 |
| Week 12 | 71 ‡‡‡ | 68 | 60 |
Pathological Hypersecretory Conditions (e.g., Zollinger-Ellison Syndrome, Multiple Endocrine Adenomas)
In studies of patients with pathological hypersecretory conditions such as Zollinger-Ellison Syndrome with or without multiple endocrine adenomas, famotidine significantly inhibited gastric acid secretion and controlled associated symptoms. Orally administered doses from 20 to 160 mg q 6 h maintained basal acid secretion below 10 mEq/hr; initial doses were titrated to the individual patient need and subsequent adjustments were necessary with time in some patients. Famotidine was well tolerated at these high dose levels for prolonged periods (greater than 12 months) in eight patients, and there were no cases reported of gynecomastia, increased prolactin levels, or impotence which were considered to be due to the drug.
Clinical Studies
The majority of clinical study experience involved oral administration of famotidine tablets, and is provided herein for reference.
Duodenal Ulcer
In a U.S. multicenter, double-blind study in outpatients with endoscopically confirmed duodenal ulcer, orally administered famotidine was compared to placebo. As shown in Table 1 , 70% of patients treated with famotidine 40 mg h.s. were healed by week 4.
•Statistically significantly different than placebo (p<0.001) | |||
| Outpatients with Endoscopically Confirmed Healed Duodenal Ulcers | |||
| Famotidine | Famotidine | Placebo | |
| 40 mg h.s. | 20 mg b.i.d. | h.s. | |
| (N=89) | (N=84) | (N=97) | |
| Week 2 | •32% | • 38% | 17% |
| Week 4 | •70% | • 67% | 31% |
Patients not healed by week 4 were continued in the study. By week 8, 83% of patients treated with famotidine had healed versus 45% of patients treated with placebo. The incidence of ulcer healing with famotidine was significantly higher than with placebo at each time point based on proportion of endoscopically confirmed healed ulcers.
In this study, time to relief of daytime and nocturnal pain was significantly shorter for patients receiving famotidine than for patients receiving placebo; patients receiving famotidine also took less antacid than the patients receiving placebo.
Long-Term Maintenance Treatment of Duodenal Ulcers
Famotidine, 20 mg p.o. h.s. was compared to placebo h.s. as maintenance therapy in two double-blind, multicenter studies of patients with endoscopically confirmed healed duodenal ulcers. In the U.S. study the observed ulcer incidence within 12 months in patients treated with placebo was 2.4 times greater than in the patients treated with famotidine. The 89 patients treated with famotidine had a cumulative observed ulcer incidence of 23.4% compared to an observed ulcer incidence of 56.6% in the 89 patients receiving placebo (p<0.01). These results were confirmed in an international study where the cumulative observed ulcer incidence within 12 months in the 307 patients treated with famotidine was 35.7%, compared to an incidence of 75.5% in the 325 patients treated with placebo (p<0.01).
Gastric Ulcer
In both a U.S. and an international multicenter, double-blind study in patients with endoscopically confirmed active benign gastric ulcer, orally administered famotidine, 40 mg h.s., was compared to placebo h.s. Antacids were permitted during the studies, but consumption was not significantly different between the famotidine and placebo groups. As shown in Table 2 , the incidence of ulcer healing (dropouts counted as unhealed) with famotidine was statistically significantly better than placebo at weeks 6 and 8 in the U.S. study, and at weeks 4, 6 and 8 in the international study, based on the number of ulcers that healed, confirmed by endoscopy.
•••, † Statistically significantly better than placebo (p≤0.05, p≤0.01, respectively) | ||||
| Patients with Endoscopically Confirmed Healed Gastric Ulcers | ||||
| U.S. Study | International Study | |||
| Famotidine | Placebo | Famotidine | Placebo | |
| 40 mg h.s. | h.s. | 40 mg h.s. | h.s. | |
| (N=74) | (N=75) | (N=149) | (N=145) | |
| Week 4 | 45% | 39% | † 47% | 31% |
| Week 6 | † 66% | 44% | † 65% | 46% |
| Week 8 | •••78% | 64% | † 80% | 54% |
Time to complete relief of daytime and nighttime pain was statistically significantly shorter for patients receiving famotidine than for patients receiving placebo; however, in neither study was there a statistically significant difference in the proportion of patients whose pain was relieved by the end of the study (week 8).
Gastroesophageal Reflux Disease (GERD)
Orally administered famotidine was compared to placebo in a U.S. study that enrolled patients with symptoms of GERD and without endoscopic evidence of erosion or ulceration of the esophagus. Famotidine 20 mg b.i.d. was statistically significantly superior to 40 mg h.s. and to placebo in providing a successful symptomatic outcome, defined as moderate or excellent improvement of symptoms (Table 3 ).
†† p≤0.01 vs placebo | |||
| % Successful Symptomatic Outcome | |||
| Famotidine 20 mg b.i.d. | Famotidine 40 mg h.s. | Placebo | |
| (N=154) | (N=149) | (N=73) | |
| Week 6 | 82 †† | 69 | 62 |
By two weeks of treatment, symptomatic success was observed in a greater percentage of patients taking famotidine 20 mg b.i.d. compared to placebo (p≤0.01).
Symptomatic improvement and healing of endoscopically verified erosion and ulceration were studied in two additional trials. Healing was defined as complete resolution of all erosions or ulcerations visible with endoscopy. The U.S. study comparing famotidine 40 mg p.o. b.i.d. to placebo and famotidine 20 mg p.o. b.i.d., showed a significantly greater percentage of healing for famotidine 40 mg b.i.d. at weeks 6 and 12 (Table 4 ).
††† p≤0.01 vs placebo | |||
‡ p ≤ 0.05 vs famotidine 20 mg b.i.d. | |||
‡‡ p≤0.01 vs famotidine 20 mg b.i.d. | |||
| % Endoscopic Healing – U.S. Study | |||
| Famotidine 40 mg b.i.d. | Famotidine 20 mg b.i.d. | Placebo | |
| (N=127) | (N=125) | (N=66) | |
| Week 6 | 48 †††, ‡‡ | 32 | 18 |
| Week 12 | 69 †††, ‡ | 54 ††† | 29 |
As compared to placebo, patients who received famotidine had faster relief of daytime and nighttime heartburn and a greater percentage of patients experienced complete relief of nighttime heartburn.
These differences were statistically significant.
In the international study, when famotidine 40 mg p.o. b.i.d. was compared to ranitidine 150 mg p.o. b.i.d., a statistically significantly greater percentage of healing was observed with famotidine 40 mg b.i.d. at week 12 (Table 5 ). There was, however, no significant difference among treatments in symptom relief.
‡‡‡ p≤0.05 vs Ranitidine 150 mg b.i.d. | |||
| % Endoscopic Healing - International Study | |||
| Famotidine 40 mg b.i.d. | Famotidine 20 mg b.i.d. | Ranitidine 150 mg b.i.d. | |
| (N=175) | (N=93) | (N=172) | |
| Week 6 | 48 | 52 | 42 |
| Week 12 | 71 ‡‡‡ | 68 | 60 |
Pathological Hypersecretory Conditions (e.g., Zollinger-Ellison Syndrome, Multiple Endocrine Adenomas)
In studies of patients with pathological hypersecretory conditions such as Zollinger-Ellison Syndrome with or without multiple endocrine adenomas, famotidine significantly inhibited gastric acid secretion and controlled associated symptoms. Orally administered doses from 20 to 160 mg q 6 h maintained basal acid secretion below 10 mEq/hr; initial doses were titrated to the individual patient need and subsequent adjustments were necessary with time in some patients. Famotidine was well tolerated at these high dose levels for prolonged periods (greater than 12 months) in eight patients, and there were no cases reported of gynecomastia, increased prolactin levels, or impotence which were considered to be due to the drug.
HOW SUPPLIED
FOR INTRAVENOUS USE ONLY
Famotidine Injection, USP 10 mg per mL is a non-preserved, clear, colorless solution and is supplied as:
| Product Code | Unit of Sale | Strength | Each |
| PRX730912 | NDC 63323-739-16 Unit of 25 | 20 mg per 2 mL (10 mg per mL) | NDC 63323-739-41 2 mL Single Dose Vial |
Storage
Store Famotidine Injection at 2° to 8°C (36° to 46°F). If solution freezes, bring to room temperature; allow sufficient time to solubilize all the components
Although diluted Famotidine Injection has been shown to be physically and chemically stable for 7 days at room temperature, there are no data on the maintenance of sterility after dilution. Therefore, it is recommended that if not used immediately after preparation, diluted solutions of Famotidine Injection should be refrigerated and used within 48 hours (see DOSAGE AND ADMINISTRATION ).
This container closure is not made with natural rubber latex.
PREMIERProRx ® is a registered trademark of Premier Healthcare Alliance, L.P., used under license.
Manufactured by:
Fresenius Kabi
Lake Zurich, IL 60047
www.fresenius-kabi.com/us
451450B
Revised: June 2021
