Get your patient on Favlyxa (Fluorouracil)
Favlyxa prescribing information
WARNING: SERIOUS ADVERSE REACTIONS OR DEATH IN PATIENTS WITH COMPLETE DPD DEFICIENCY
- Increased risk of serious adverse reactions or death in patients with complete DPD deficiency.
- Test patients for genetic variants of DPYD prior to initiating FAVLYXA unless immediate treatment is necessary. Avoid use of FAVLYXA in patients with certain homozygous or compound heterozygous DPYD variants that result in complete DPD deficiency [see Warnings and Precautions (5.1) ].
INDICATIONS AND USAGE
FAVLYXA is indicated for the treatment of patients with:
1.1 Adenocarcinoma of the Colon and Rectum
1.2 Adenocarcinoma of the Breast
1.3 Gastric Adenocarcinoma
1.4 Pancreatic Adenocarcinoma
2 DOSAGE AND ADMINISTRATION
- FAVLYXA is recommended for administration either as an intravenous bolus or as an intravenous infusion. (2.1 )
- Adenocarcinoma of the Colon and Rectum
- In combination with leucovorin or as a component of a multidrug chemotherapy regimen that includes leucovorin (infusional regimen): 400 mg/m 2 for one dose, followed by 2,400 mg/m 2 to 3,000 mg/m 2 over 46 hours on day 1 of each 2-week cycle or
- In combination with leucovorin (bolus regimen): 500 mg/m 2 on days 1, 8, 15, 22, 29 and 36 of each 8-week cycle. (2.2 )
- Adenocarcinoma of the Breast in combination with a cyclophosphamide-based multidrug regimen: 500 mg/m 2 or 600 mg/m 2 on days 1 and 8 of each 28-day cycle (bolus regimen). (2.2 )
- Gastric Adenocarcinoma in combination with a platinum-containing multidrug regimen: 200 mg/m 2 to 1,000 mg/m 2 over 24 hours (infusional regimen). (2.2 )
- Pancreatic Adenocarcinoma in combination with leucovorin or as a component of a multidrug chemotherapy regimen that includes leucovorin: 400 mg/m 2 on day 1, followed by 2,400 mg/m 2 over 46 hours every 2 weeks (infusional regimen). (2.2 )
- Refer to Section 2.3 for dosage modifications due to adverse reactions.
Evaluation and Testing for DPD Deficiency Before Initiating FAVLYXA
Prior to initiating FAVLYXA, test patients for genetic variants of the DPYD gene unless immediate treatment is necessary. An FDA-authorized test for the detection of the DPYD gene to identify patients at risk of serious adverse reactions with FAVLYXA is not currently available. Currently available tests used to identify DPYD variants may vary in accuracy and design (e.g., which DPYD variant(s) they identify).
Avoid use of FAVLYXA in patients known to have certain homozygous or compound heterozygous DPYD variants that result in complete DPD deficiency . No FAVLYXA dose has been proven safe for patients with complete DPD deficiency. For patients with partial DPD deficiency, individualize the dosage and modify based on tolerability and intent of treatment [see Warnings and Precautions (5.1) ] .
Recommended Dosage
FAVLYXA is recommended for administration either as an intravenous bolus or as an intravenous infusion. Dosage recommendations are in Table 1.
| Indication | Recommended Dosage | Duration of Treatment |
| Adenocarcinoma of the Colon and Rectum | ||
| In combination with leucovorin or as a component of a multidrug chemotherapy regimen that includes leucovorin | 400 mg/m 2 for one dose, followed by 2,400 mg/m 2 to 3,000 mg/m 2 over 46 hours on day 1 of each 2-week cycle | Until disease progression or unacceptable toxicity. |
| In combination with leucovorin alone (bolus regimen) | 500 mg/m 2 on days 1, 8, 15, 22, 29 and 36 of each 8-week cycle | Until disease progression or unacceptable toxicity. |
| Adenocarcinoma of the Breast | ||
| In combination with cyclophosphamide-based multidrug regimen (bolus regimen) | 500 mg/m 2 or 600 mg/m 2 on days 1 and 8 of each 28-day cycle | Until disease progression or unacceptable toxicity or 6 cycles |
| Gastric Adenocarcinoma | ||
| In combination with a platinum-containing multidrug regimen | 200 mg/m 2 to 1,000 mg/m 2 over 24 hours | Frequency in each cycle and length of each cycle depend on dose of FAVLYXA and specific regimen |
| Pancreatic Adenocarcinoma | ||
| In combination with leucovorin or as a component of a multidrug chemotherapy regimen that includes leucovorin | 400 mg/m 2 on day 1, followed by 2,400 mg/m 2 over 46 hours every 2 weeks | Until disease progression or unacceptable toxicity. |
Dosage Modifications for Adverse Reactions
Withhold FAVLYXA for the following adverse reactions. Depending on the severity of the adverse reaction, either discontinue or resume FAVLYXA at a reduced dosage upon resolution or improvement to Grade 1:
- Grade 3 or 4 diarrhea [see Warnings and Precautions (5.5) ]
- Grade 2 or 3 palmar-plantar erythrodysesthesia (hand-foot syndrome) [see Warnings and Precautions (5.6) ]
- Grade 3 or 4 mucositis [see Warnings and Precautions (5.8) ]
- Grade 4 myelosuppression [see Warnings and Precautions (5.7) ]
There is no recommended dose for resumption of FAVLYXA administration following development of any of the following adverse reactions; consider permanent discontinuation of FAVLYXA following:
- Development of angina, myocardial infarction/ischemia, arrhythmia, or heart failure in patients with no history of coronary artery disease or myocardial dysfunction [see Warnings and Precautions (5.2) ]
- Hyperammonemic encephalopathy [see Warnings and Precautions (5.3) ]
- Neurologic toxicity including acute cerebellar syndrome [see Warnings and Precautions (5.4) ]
Preparation and Administration
FAVLYXA is a hazardous drug. Follow applicable special handling and disposal procedures 1 .
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit.
For Direct Intravenous Bolus Injection
Preparation
- Select the appropriate number of vial(s) based on the prescribed dose.
- Withdraw the calculated dose into a sterile syringe.
- Discard partially used or empty vials of FAVLYXA.
Administration
- Administer FAVLYXA as an intravenous bolus through an established intravenous line over 2 to 5 minutes.
- Do not administer in the same intravenous line concomitantly with other medicinal products.
Storage
- If the dose is not administered, attach a tip cap to the syringe prior to storage. The syringe can be stored at room temperature 20°C to 25°C (68°F to 77°F) for up to 4 hours.
For Intravenous Infusion
Preparation
- Select the appropriate number of vial(s) based on the prescribed dose.
- Withdraw the calculated dose into a sterile syringe.
- Dilute the calculated dose in an appropriate amount of 0.9% Sodium Chloride Injection, or 5% Dextrose Injection, to prepare an infusion solution with a final concentration ranging from 1.5 mg/mL to 10 mg/mL.
Administration
- Do not administer in the same intravenous line concomitantly with other medicinal products.
- For intravenous infusion regimens, administer through a central venous line using an infusion pump.
Storage
- If not used immediately, the diluted FAVLYXA can be stored at room temperature 20°C to 25°C (68°F to 77°F) for up to 24 hours.
DOSAGE FORMS AND STRENGTHS
Injection: FAVLYXA contains 250 mg/10 mL (25 mg/mL) fluorouracil as colorless to light yellow clear solution in a single-dose vial.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary
Based on mechanism of action and animal reproduction studies, FAVLYXA can cause fetal harm when administered during pregnancy [see Clinical Pharmacology (12.1) ]. Available data from observational studies with intravenous administration of fluorouracil during pregnancy are insufficient to identify a drug-associated risk of major birth defects, miscarriage or adverse maternal or fetal outcomes.
Administration of fluorouracil to rats and mice during selected periods of organogenesis, at doses lower than a human dose of 12 mg/kg, caused embryolethality and teratogenicity. Malformations included cleft palate and skeletal defects. In monkeys, maternal doses of fluorouracil higher than an approximate human dose of 12 mg/kg resulted in abortion (see Data).
In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2–4% and 15–20%, respectively.
Data
Animal Data
Malformations including cleft palate, skeletal defects and deformed appendages (paws and tails) were observed when fluorouracil was administered by intraperitoneal injection to mice at doses at or above 10 mg/kg (approximately 0.06 times a human dose of 12 mg/kg on a mg/m 2 basis) for 4 days during the period of organogenesis. Similar results were observed in hamsters administered fluorouracil intramuscularly at doses lower than those administered in commonly used clinical treatment regimens. In rats, administration of fluorouracil by intraperitoneal injection at doses greater than 15 mg/kg (approximately 0.2 times a human dose of 12 mg/kg on a mg/m 2 basis) for a single day during organogenesis resulted in delays in growth and malformations including micro-anophthalmos. In monkeys, administration of fluorouracil during organogenesis at doses approximately equal to a human dose of 12 mg/kg on a mg/m 2 basis resulted in abortion; at a 50% lower dose, resorptions and decreased fetal body weights were reported.
Lactation
Risk Summary
There are no data on the presence of fluorouracil or its metabolites in human milk, the effects on the breastfed child, or the effects on milk production. Because of the potential for serious adverse reactions in the breastfed child, advise patients not to breastfeed during treatment with FAVLYXA and for 1 week after the last dose.
Females and Males of Reproductive Potential
FAVLYXA can cause fetal harm when administered to a pregnant woman [see Use in Specific Populations (8.1 ) ] .
Pregnancy Testing
Verify that females of reproductive potential are not pregnant prior to initiating FAVLYXA [see Warnings and Precautions (5.10) , Use in Specific Populations (8.1 , 8.3) ].
Contraception
Females
Advise females of reproductive potential to use effective contraception during treatment with FAVLYXA and for 6 months after the last dose.
Males
Based on genotoxicity findings, advise males with female partners of reproductive potential to use effective contraception during treatment with FAVLYXA and for 3 months after the last dose [see Nonclinical Toxicology (13.1) ].
Infertility
Based on animal studies, FAVLYXA may impair fertility in females and males of reproductive potential [see Nonclinical Toxicology (13.1) ].
Pediatric Use
The safety and effectiveness of FAVLYXA in pediatric patients have not been established.
Geriatric Use
Reported clinical experience has not identified differences in safety or effectiveness between the elderly and younger patients.
CONTRAINDICATIONS
None.
WARNINGS AND PRECAUTIONS
- Cardiotoxicity: FAVLYXA can cause cardiotoxicity, including angina, myocardial infarction/ischemia, arrhythmia, and heart failure. Withhold FAVLYXA for cardiac toxicity. (5.2 )
- Hyperammonemic Encephalopathy: Altered mental status, confusion, disorientation, coma, or ataxia with elevated serum ammonia level can occur within 72 hours of initiation of FAVLYXA. Withhold FAVLYXA and initiate ammonia-lowering therapy. (5.3 )
- Neurologic Toxicity: FAVLYXA can cause acute cerebellar syndrome, confusion, disorientation, ataxia, or visual disturbances. Withhold FAVLYXA for neurologic toxicity. (5.4 )
- Diarrhea: FAVLYXA can cause severe diarrhea. Withhold FAVLYXA for severe diarrhea until resolved. (5.5 )
- Palmar-Plantar Erythrodysesthesia Syndrome: Based on severity, withhold FAVLYXA until resolved or decreased to Grade 1, then resume at a reduced dose. (5.6 )
- Myelosuppression: FAVLYXA can cause severe and fatal myelosuppression. Withhold FAVLYXA until severe myelosuppression resolves, then resume at a reduced dose. (5.7 )
- Mucositis: FAVLYXA can cause severe mucositis. Withhold FAVLYXA until resolved or decreased to Grade 1, then resume at a reduced dose. (5.8 )
- Increased Risk of Bleeding with Concomitant Use of Warfarin: Concurrent administration with warfarin can result in clinically significant increases in coagulation parameters: Closely monitor INR and prothrombin time. (5.9 )
- Embryofetal Toxicity: Can cause fetal harm. Advise females and males of reproductive potential of the potential risk to a fetus and to use effective contraception. (5.10 , 8.1 , 8.3 )
Serious Adverse Reactions or Death from Dihydropyrimidine Dehydrogenase (DPD) Deficiency
Patients with certain homozygous or compound heterozygous variants in the DPYD gene known to result in complete or near complete absence of DPD activity (complete DPD deficiency) are at increased risk for acute early-onset toxicity and serious, including fatal adverse reactions due to FAVLYXA (e.g., mucositis, diarrhea, neutropenia, and neurotoxicity). Patients with partial DPD activity (partial DPD deficiency) may also have increased risk of serious or fatal adverse reactions.
Prior to initiating FAVLYXA, test patients for genetic variants of the DPYD gene unless immediate treatment is necessary [see Clinical Pharmacology (12.5) ] . Serious adverse reactions may still occur even if no DPYD variants are identified.
Avoid use of FAVLYXA in patients with certain homozygous or compound heterozygous DPYD variants that result in complete DPD deficiency.
Withhold or permanently discontinue FAVLYXA based on clinical assessment of the onset, duration, and severity of adverse events in patients with evidence of acute early-onset or unusually severe reactions. No fluorouracil dose has been proven safe for patients with complete DPD deficiency. For patients with partial DPD deficiency, individualize the dosage and modify based on tolerability and intent of treatment.
An FDA-authorized test for the detection of genetic variants of the DPYD gene to identify patients at risk of serious adverse reactions with FAVLYXA treatment is not currently available. Currently available tests used to identify DPYD variants may vary in accuracy and design (e.g., which DPYD variant(s) they identify).
Cardiotoxicity
FAVLYXA can cause cardiotoxicity, including angina, myocardial infarction/ischemia, arrhythmia, and heart failure, based on postmarketing reports. Reported risk factors for cardiotoxicity are administration by continuous infusion rather than intravenous bolus and presence of coronary artery disease. Withhold FAVLYXA for cardiotoxicity. The risks of resumption of FAVLYXA in patients with cardiotoxicity that has resolved have not been established [see Dosage and Administration (2.3) ].
Hyperammonemic Encephalopathy
FAVLYXA can cause hyperammonemic encephalopathy in the absence of liver disease or other identifiable cause, based on postmarketing reports. Signs or symptoms of hyperammonemic encephalopathy began within 72 hours after initiation of FAVLYXA infusion; these included altered mental status, confusion, disorientation, coma, or ataxia, in the presence of concomitant elevated serum ammonia level. Withhold FAVLYXA for hyperammonemic encephalopathy and initiate ammonia-lowering therapy. The risks of resumption of FAVLYXA in patients with hyperammonemic encephalopathy that has resolved have not been established [see Dosage and Administration (2.3) ] .
Neurologic Toxicity
FAVLYXA can cause neurologic toxicity, including acute cerebellar syndrome and other neurologic events, based on postmarketing reports. Neurologic symptoms included confusion, disorientation, ataxia, or visual disturbances. Withhold FAVLYXA for neurologic toxicity. There are insufficient data on the risks of resumption of FAVLYXA in patients with neurologic toxicity that has resolved [see Dosage and Administration (2.3) ] .
Diarrhea
FAVLYXA can cause severe diarrhea. Withhold FAVLYXA for Grade 3 or 4 diarrhea until resolved or decreased in intensity to Grade 1, then resume FAVLYXA at a reduced dose. Administer fluids, electrolyte replacement, or antidiarrheal treatments as necessary [see Dosage and Administration (2.3) ] .
Palmar-Plantar Erythrodysesthesia (Hand-Foot Syndrome)
FAVLYXA can cause palmar-plantar erythrodysesthesia, also known as hand-foot syndrome (HFS). Symptoms of HFS include a tingling sensation, pain, swelling, and erythema with tenderness, and desquamation. HFS occurs more commonly when fluorouracil is administered as a continuous infusion than when fluorouracil is administered as a bolus injection, and has been reported to occur more frequently in patients with previous exposure to chemotherapy. HFS is generally observed after 8 to 9 weeks of fluorouracil administration but may occur earlier. Institute supportive measures for symptomatic relief of HFS. Withhold FAVLYXA administration for Grade 2 or 3 HFS; resume FAVLYXA at a reduced dose when HFS is completely resolved or decreased in severity to Grade 1 [see Dosage and Administration (2.3) ] .
Myelosuppression
FAVLYXA can cause severe and fatal myelosuppression which may include neutropenia, thrombocytopenia, and anemia. The nadir in neutrophil counts commonly occurs between 9 and 14 days after fluorouracil administration. Obtain complete blood counts prior to each treatment cycle, weekly if administered on a weekly or similar schedule, and as needed. Withhold FAVLYXA until Grade 4 myelosuppression resolves; resume FAVLYXA at a reduced dose when myelosuppression has resolved or improved to Grade 1 in severity [see Dosage and Administration (2.3) ] .
Mucositis
FAVLYXA can cause mucositis, stomatitis or esophagopharyngitis, which may lead to mucosal sloughing or ulceration.
The incidence is reported to be higher with administration of fluorouracil by intravenous bolus compared with administration by continuous infusion. Withhold FAVLYXA administration for Grade 3 or 4 mucositis; resume FAVLYXA at a reduced dose once mucositis has resolved or decreased in severity to Grade 1 [see Dosage and Administration (2.3) ] .
Increased Risk of Bleeding with Concomitant Use of Warfarin
Altered coagulation parameters and/or bleeding, including death, have been reported during concomitant use of warfarin and fluorouracil. Monitor INR more frequently and adjust the dose of warfarin in patients receiving concomitant warfarin [see Drug Interactions (7) ] .
Embryofetal Toxicity
Based on its mechanism of action and animal reproduction studies, FAVLYXA can cause fetal harm when administered during pregnancy [see Use in Specific Populations (8.1) , and Clinical Pharmacology (12.1) ] . Advise females of reproductive potential to use effective contraception during treatment with FAVLYXA and for 6 months after the last dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with FAVLYXA and for 3 months after the last dose [see Use in Specific Populations (8.3) ] .
ADVERSE REACTIONS
The following adverse reactions are discussed in more detail in other sections of the labeling:
- Serious adverse reactions or death from Dihydropyrimidine Dehydrogenase (DPD) deficiency [see Warnings and Precautions (5.1) ]
- Cardiotoxicity [see Warnings and Precautions (5.2) ]
- Hyperammonemic encephalopathy [see Warnings and Precautions (5.3) ]
- Neurologic toxicity [see Warnings and Precautions (5.4) ]
- Diarrhea [see Warnings and Precautions (5.5) ]
- Palmar-plantar erythrodysesthesia (hand-foot syndrome) [see Warnings and Precautions (5.6) ]
- Myelosuppression [see Warnings and Precautions (5.7) ]
- Mucositis [see Warnings and Precautions (5.8) ]
- Increased risk of bleeding with concomitant use of warfarin [see Warnings and Precautions (5.9) ]
Postmarketing Experience
The following adverse reactions have been identified during postapproval use of fluorouracil. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Hematologic: pancytopenia [see Warnings and Precautions (5.7) ]
Gastrointestinal: gastrointestinal ulceration, nausea, vomiting
Allergic Reactions: anaphylaxis and generalized allergic reactions
Neurologic: nystagmus, headache
Dermatologic: dry skin; fissuring; photosensitivity, as manifested by erythema or increased pigmentation of the skin; vein pigmentation
Ophthalmic: lacrimal duct stenosis, visual changes, lacrimation, photophobia
Psychiatric: euphoria
Miscellaneous: thrombophlebitis, epistaxis, nail changes (including loss of nails)
DRUG INTERACTIONS
Effect of FAVLYXA on Other Drugs
Vitamin K Antagonists
Monitor INR and PT more frequently in patients receiving FAVLYXA and warfarin. Elevated INR and PT have been reported in patients taking fluorouracil concomitantly with warfarin.
DESCRIPTION
FAVLYXA injection contains fluorouracil, a nucleoside metabolic inhibitor. Fluorouracil, a fluorinated pyrimidine, has a chemical name of 5-fluoro-2,4 (1 H ,3 H )-pyrimidinedione. Its structural formula is:
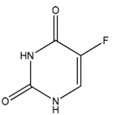
Molecular formula: C 4 H 3 FN 2 O 2
Molecular weight: 130.08 g/mole
FAVLYXA injection 250 mg/10 mL is a sterile, colorless to light yellow clear solution available in single-dose vials for intravenous bolus or infusion administration. Each mL contains 25 mg fluorouracil in water for injection. Sodium hydroxide is added to adjust the pH to 8.6 to 9.4.
CLINICAL PHARMACOLOGY
Mechanism of Action
Fluorouracil is a nucleoside metabolic inhibitor that interferes with the synthesis of deoxyribonucleic acid (DNA) and to a lesser extent inhibits the formation of ribonucleic acid (RNA); these affect rapidly growing cells and may lead to cell death. Fluorouracil is converted to three main active metabolites: 5-fluoro-2′-deoxyuridine-5′-monophosphate (FdUMP), 5-fluorouridine-5′triphosphate (FUTP) and 5-fluoro-2′-deoxyuridine-5′-triphosphate (FdUTP). These metabolites have several effects including the inhibition of thymidylate synthase by FdUMP, incorporation of FUTP into RNA and incorporation of FdUTP into DNA.
Pharmacodynamics
Fluorouracil exposure-response relationships and the time course of the pharmacodynamic response are unknown.
Pharmacokinetics
Distribution
Following bolus intravenous injection, fluorouracil distributes throughout the body including the intestinal mucosa, bone marrow, liver, cerebrospinal fluid and brain tissue.
Elimination
Following bolus intravenous injection, 5 to 20% of the parent drug is excreted unchanged in the urine in six hours. The remaining percentage of the administered dose is metabolized, primarily in the liver. The metabolites of fluorouracil (e.g., urea and α-fluoro-ßalanine) are excreted in the urine over 3 to 4 hours.
Following bolus intravenous injection of fluorouracil, as a single agent, the elimination half-life increased with dose from 8 to 20 minutes.
Pharmacogenomics
The DPYD gene encodes the enzyme DPD, which is responsible for the catabolism of >80% of fluorouracil. Approximately 3 to 5% of White populations have partial DPD deficiency and 0.2% of White populations have complete DPD deficiency, which may be due to certain genetic no function or decreased function variants in DPYD resulting in partial to complete or near complete absence of enzyme activity. DPD deficiency is estimated to be more prevalent in Black or African American populations compared to White populations. Insufficient information is available to estimate the prevalence of DPD deficiency in other populations.
Patients who are homozygous or compound heterozygous for no function DPYD variants (i.e., carry two DPYD variants that result in no DPD enzyme activity) or are compound heterozygous for a no function DPYD variant plus a decreased function DPYD variant have complete DPD deficiency and are at increased risk for acute early-onset of toxicity and serious life-threatening, or fatal adverse reactions due to increased systemic exposure to fluorouracil. Partial DPD deficiency can result from the presence of either two decreased function DPYD variants or one normal function plus either a decreased function or a no function DPYD variant. Patients with partial DPD deficiency may also be at an increased risk for toxicity from fluorouracil.
Several DPYD variants observed with variability across populations have been associated with reduced or no DPD activity, especially when present as homozygous or compound heterozygous variants. These include c.1905+1G>A ( DPYD •2A), c.1679T>G ( DPYD •13), c.2846A>T, and c.1129-5923C>G (Haplotype B3). DPYD •2A and DPYD •13 are no function variants, and c.2846A>T, c.1129-5923C>G, and c557A>G are decreased function variants. This is not a complete listing of all DPYD variants that may result in DPD deficiency [see Warnings and Precautions (5.1) ] .
NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies have not been performed with fluorouracil. Fluorouracil was mutagenic in vitro in the bacterial reverse mutation (Ames) assay and induced chromosomal aberrations in hamster fibroblasts in vitro and in mouse bone marrow in the in vivo mouse micronucleus assay.
Administration of fluorouracil intraperitoneally to male rats at dose levels equal to or greater than 1.7-fold the human dose of 12 mg/kg induced chromosomal aberrations in spermatogonia and inhibition of spermatogonia differentiation resulting in transient infertility. In female rats, intraperitoneal administration of fluorouracil during the pre-ovulatory phases of oogenesis at dose levels equal to or greater than 0.33 times a human dose of 12 mg/kg resulted in decreased incidence of fertile matings, increased pre-implantation loss, and fetotoxicity.
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
FAVLYXA TM Injection is a sterile colorless to light yellow clear solution available in single-dose vials individually packaged in a carton as follows:
| NDC Number | Strength | Package |
| 83831-143-01 | 250 mg/10 mL (25 mg/mL) | 1 single-dose vial in 1 carton |
Storage
Store at 20°C to 25°C (68°F to 77°F); excursions permitted from 15°C to 30°C (59°F to 86°F). [see USP Controlled Room Temperature]. Protect from light. Retain in carton until time of use.
Fluorouracil is a hazardous drug. Follow applicable special handling and disposable procedures [see References (15) ] .
Mechanism of Action
Fluorouracil is a nucleoside metabolic inhibitor that interferes with the synthesis of deoxyribonucleic acid (DNA) and to a lesser extent inhibits the formation of ribonucleic acid (RNA); these affect rapidly growing cells and may lead to cell death. Fluorouracil is converted to three main active metabolites: 5-fluoro-2′-deoxyuridine-5′-monophosphate (FdUMP), 5-fluorouridine-5′triphosphate (FUTP) and 5-fluoro-2′-deoxyuridine-5′-triphosphate (FdUTP). These metabolites have several effects including the inhibition of thymidylate synthase by FdUMP, incorporation of FUTP into RNA and incorporation of FdUTP into DNA.