Gemfibrozil - Gemfibrozil tablet prescribing information
INDICATIONS & USAGE
Gemfibrozil tablets, USP are indicated as adjunctive therapy to diet for:
1. Treatment of adult patients with very high elevations of serum triglyceride levels (Types IV and V hyperlipidemia) who present a risk of pancreatitis and who do not respond adequately to a determined dietary effort to control them. Patients who present such risk typically have serum triglycerides over 2000 mg/dL and have elevations of VLDL-cholesterol as well as fasting chylomicrons (Type V hyperlipidemia). Subjects who consistently have total serum or plasma triglycerides below 1000 mg/dL are unlikely to present a risk of pancreatitis. Gemfibrozil therapy may be considered for those subjects with triglyceride elevations between 1000 and 2000 mg/dL who have a history of pancreatitis or of recurrent abdominal pain typical of pancreatitis. It is recognized that some Type IV patients with triglycerides under 1000 mg/dL may, through dietary or alcoholic indiscretion, convert to a Type V pattern with massive triglyceride elevations accompanying fasting chylomicronemia, but the influence of Gemfibrozil therapy on the risk of pancreatitis in such situations has not been adequately studied. Drug therapy is not indicated for patients with Type I hyperlipoproteinemia, who have elevations of chylomicrons and plasma triglycerides, but who have normal levels of very low density lipoprotein (VLDL). Inspection of plasma refrigerated for 14 hours is helpful in distinguishing Types I, IV, and V hyperlipoproteinemia.
2. Reducing the risk of developing coronary heart disease only in Type IIb patients without history of or symptoms of existing coronary heart disease who have had an inadequate response to weight loss, dietary therapy, exercise, and other pharmacologic agents (such as bile acid sequestrants and nicotinic acid, known to reduce LDL-and raise HDL-cholesterol) and who have the following triad of lipid abnormalities: low HDL-cholesterol levels in addition to elevated LDL-cholesterol and elevated triglycerides (see WARNINGS , PRECAUTIONS , and CLINICAL PHARMACOLOGY ). The National Cholesterol Education Program has defined a serum HDL-cholesterol value that is consistently below 35 mg/dL as constituting an independent risk factor for coronary heart disease. Patients with significantly elevated triglycerides should be closely observed when treated with gemfibrozil. In some patients with high triglyceride levels, treatment with gemfibrozil is associated with a significant increase in LDL-cholesterol. BECAUSE OF POTENTIAL TOXICITY SUCH AS MALIGNANCY, GALLBLADDER DISEASE, ABDOMINAL PAIN LEADING TO APPENDECTOMY AND OTHER ABDOMINAL SURGERIES, AN INCREASED INCIDENCE IN NON-CORONARY MORTALITY, AND THE 44% RELATIVE INCREASE DURING THE TRIAL PERIOD IN AGE-ADJUSTED ALL-CAUSE MORTALITY SEEN WITH THE CHEMICALLY AND PHARMACOLOGICALLY RELATED DRUG, CLOFIBRATE, THE POTENTIAL BENEFIT OF GEMFIBROZIL IN TREATING TYPE IIA PATIENTS WITH ELEVATIONS OF LDL-CHOLESTEROL ONLY IS NOT LIKELY TO OUTWEIGH THE RISKS. GEMFIBROZIL IS ALSO NOT INDICATED FOR THE TREATMENT OF PATIENTS WITH LOW HDL-CHOLESTEROLAS THEIR ONLY LIPID ABNORMALITY.
In a subgroup analysis of patients in the Helsinki Heart Study with above-median HDL-cholesterol values at baseline (greater than 46.4 mg/dL), the incidence of serious coronary events was similar for gemfibrozil and placebo subgroups (see Table I). The initial treatment for dyslipidemia is dietary therapy specific for the type of lipoprotein abnormality. Excess body weight and excess alcohol intake may be important factors in hypertriglyceridemia and should be managed prior to any drug therapy. Physical exercise can be an important ancillary measure, and has been associated with rises in HDL-cholesterol. Diseases contributory to hyperlipidemia such as hypothyroidism or diabetes mellitus should be looked for and adequately treated. Estrogen therapy is sometimes associated with massive rises in plasma triglycerides, especially in subjects with familial hypertriglyceridemia. In such cases, discontinuation of estrogen therapy may obviate the need for specific drug therapy of hypertriglyceridemia. The use of drugs should be considered only when reasonable attempts have been made to obtain satisfactory results with nondrug methods. If the decision is made to use drugs, the patient should be instructed that this does not reduce the importance of adhering to diet.
DOSAGE & ADMINISTRATION
The recommended dose for adults is 1200 mg administered in two divided doses 30 minutes before the morning and evening meals (see CLINICAL PHARMACOLOGY ).
CONTRAINDICATIONS
1.Hepatic or severe renal dysfunction, including primary biliary cirrhosis. 2.Preexisting gallbladder disease (see WARNINGS ). 3.Hypersensitivity to gemfibrozil. 4.Combination therapy of gemfibrozil with simvastatin (see WARNINGS and PRECAUTIONS ). 5.Combination therapy of gemfibrozil with repaglinide (see PRECAUTIONS ). 6.Combination therapy of gemfibrozil with dasabuvir (see PRECAUTIONS ). 7. Combination therapy of gemfibrozil with selexipag (see PRECAUTIONS ).
ADVERSE REACTIONS
In the double-blind controlled phase of the primary prevention component of the Helsinki Heart Study, 2046 patients received gemfibrozil for up to five years. In that study, the following adverse reactions were statistically more frequent in subjects in the gemfibrozil group:
| Gemfibrozil (N=2046) | PLACEBO (N=2035) | |
| Frequency in percent of subjects | ||
| Gastrointestinal reactions | 34.2 | 23.8 |
| Dyspepsia | 19.6 | 11.9 |
| Abdominal pain | 9.8 | 5.6 |
| Acute appendicitis (histologically confirmed in most cases where data were available) | 1.2 | 0.6 |
| Atrial fibrillation | 0.7 | 0.1 |
| Adverse events reported by more than 1% of subjects, but without a significant difference between groups: | ||
| Diarrhea | 7.2 | 6.5 |
| Fatigue | 3.8 | 3.5 |
| Nausea/Vomiting | 2.5 | 2.1 |
| Eczema | 1.9 | 1.2 |
| Rash | 1.7 | 1.3 |
| Vertigo | 1.5 | 1.3 |
| Constipation | 1.4 | 1.3 |
| Headache | 1.2 | 1.1 |
Gallbladder surgery was performed in 0.9% of gemfibrozil and 0.5% of placebo subjects in the primary prevention component, a 64% excess, which is not statistically different from the excess of gallbladder surgery observed in the clofibrate group compared to the placebo group of the WHO study. Gallbladder surgery was also performed more frequently in the gemfibrozil group compared to the placebo group (1.9% versus 0.3%, p=0.07) in the secondary prevention component. A statistically significant increase in appendectomy in the gemfibrozil group was seen also in the secondary prevention component (6 on gemfibrozil versus 0 on placebo, p=0.014).
Nervous system and special senses adverse reactions were more common in the gemfibrozil group. These included hypesthesia, paresthesias, and taste perversion. Other adverse reactions that were more common among gemfibrozil treatment group subjects but where a causal relationship was not established include cataracts, peripheral vascular disease, and intracerebral hemorrhage. From other studies it seems probable that gemfibrozil is causally related to the occurrence of MUSCULOSKELETAL SYMPTOMS (see WARNINGS ), and to ABNORMAL LIVER FUNCTION TESTS and HEMATOLOGIC CHANGES (see PRECAUTIONS ). Reports of viral and bacterial infections (common cold, cough, urinary tract infections) were more common in gemfibrozil treated patients in other controlled clinical trials of 805 patients. Additional adverse reactions that have been reported for gemfibrozil are listed below by system. These are categorized according to whether a causal relationship to treatment with gemfibrozil is probable or not established:
| CAUSAL RELATIONSHIP PROBABLE | CAUSAL RELATIONSHIP NOT ESTABLISHED | |
| General: Cardiac: | weight loss extrasystoles | |
| Gastrointestinal: | cholestatic jaundice | pancreatitis hepatoma colitis |
| Central Nervous System: | ||
| dizziness somnolence paresthesia peripheral neuritis decreased libido depression headache | confusion convulsions syncope | |
| Eye: | blurred vision | retinal edema |
| Genitourinary: | impotence | decreased male fertility renal dysfunction |
| Musculoskeletal: | myopathy myasthenia myalgia painful extremities arthralgia synovitis rhabdomyolysis (see WARNINGS and Drug Interactions under PRECAUTIONS ) | |
| Clinical | ||
| Laboratory: | increased creatine phosphokinase increased bilirubin increased liver transaminases (AST, ALT) increased alkaline phosphatase | positive antinuclear antibody |
| Hematopoietic: | anemia leukopenia bone marrow hypoplasia eosinophilia | thrombocytopenia |
| Immunologic: | angioedema laryngeal edema urticaria | anaphylaxis Lupus-like syndrome vasculitis |
| Integumentary: | exfoliative dermatitis rash dermatitis pruritus | alopecia photosensitivity |
Additional adverse reactions that have been reported include cholecystitis and cholelithiasis (see WARNINGS ).
Drug Interactions
( A) HMG-CoA Reductase Inhibitors: The concomitant administration of gemfibrozil with simvastatin is contraindicated (see CONTRAINDICATIONS and WARNINGS ). Avoid concomitant use of gemfibrozil with rosuvastatin. If concomitant use cannot be avoided, initiate rosuvastatin at 5 mg once daily. The dose of rosuvastatin should not exceed 10 mg once daily. The risk of myopathy and rhabdomyolysis is increased with combined gemfibrozil and HMG-CoA reductase inhibitor therapy. Myopathy or rhabdomyolysis with or without acute renal failure have been reported as early as three weeks after initiation of combined therapy or after several months (see WARNINGS ). There is no assurance that periodic monitoring of creatine kinase will prevent the occurrence of severe myopathy and kidney damage.
(B) Anticoagulants: CAUTION SHOULD BE EXERCISED WHEN WARFARIN IS GIVEN IN CONJUNCTION WITH GEMFIBROZIL. THE DOSAGE OF WARFARIN SHOULD BE REDUCED TO MAINTAIN THE PROTHROMBIN TIME AT THE DESIRED LEVEL TO PREVENT BLEEDING COMPLICATIONS. FREQUENT PROTHROMBIN DETERMINATIONS ARE ADVISABLE UNTIL IT HAS BEEN DEFINITELY DETERMINED THAT THE PROTHROMBIN LEVEL HAS STABILIZED.
(C) CYP2C8 Substrates: Gemfibrozil is a strong inhibitor of CYP2C8 and may increase exposure of drugs mainly metabolized by CYP2C8 (e.g., dabrafenib, enzalutamide, loperamide, montelukast, paclitaxel, pioglitazone, rosiglitazone). Therefore, dosing reduction of drugs that are mainly metabolized by CYP2C8 enzyme may be required when gemfibrozil is used concomitantly (see WARNINGS ). Repaglinide: In healthy volunteers, co-administration with gemfibrozil (600 mg twice daily for 3 days) resulted in an 8.1-fold (range 5.5-to 15.0fold) higher repaglinide AUC and a 28.6-fold (range 18.5- to 80.1- fold) higher repaglinide plasma concentration 7 hours after the dose. In the same study, gemfibrozil (600 mg twice daily for 3 days) + itraconazole (200 mg in the morning and 100 mg in the evening at Day 1, then 100 mg twice daily at Day 2–3) resulted in a 19.4-(range 12.9- to 24.7-fold) higher repaglinide AUC and a 70.4 fold (range 42.9-to 119.2-fold) higher repaglinide plasma concentration 7 hours after the dose. In addition, gemfibrozil alone or gemfibrozil + itraconazole prolonged the hypoglycemic effects of repaglinide. Co-administration of gemfibrozil and repaglinide increases the risk of severe hypoglycemia and is contraindicated (see CONTRAINDICATIONS ). Dasabuvir: Co-administration of gemfibrozil with dasabuvir increased dasabuvir AUC and C max (ratios: 11.3 and 2.01, respectively) due to CYP2C8 inhibition. Increased dasabuvir exposure may increase the risk of QT prolongation, therefore, co-administration of gemfibrozil with dasabuvir is contraindicated (see CONTRAINDICATIONS ). Selexipag: Co-administration of gemfibrozil with selexipag doubled exposure to selexipag and increased exposure to the active metabolite by approximately 11-fold. Concomitant administration of gemfibrozil with selexipag is contraindicated (see CONTRAINDICATIONS ). Enzalutamide: In healthy volunteers given a single 160 mg dose of enzalutamide after gemfibrozil 600 mg twice daily, the AUC of enzalutamide plus active metabolite (N-desmethyl enzalutamide) was increased by 2.2 fold and corresponding C max was decreased by 16%. Increased enzalutamide exposure may increase the risk of seizures. If co-administration is considered necessary, the dose of enzalutamide should be reduced (see WARNINGS ). (D) OATP1B1 substrates: Gemfibrozil is an inhibitor of OATP1B1 transporter and may increase exposure of drugs that are substrates of OATP1B1 (e.g., atrasentan, atorvastatin, bosentan, ezetimibe, fluvastatin, glyburide, SN-38 [active metabolite of irinotecan], rosuvastatin, pitavastatin, pravastatin, rifampin, valsartan, olmesartan). Therefore, dosing reductions of drugs that are substrates of OATP1B1 may be required when gemfibrozil is used concomitantly (see WARNINGS ). Combination therapy of gemfibrozil with simvastatin or with repaglinide, which are OATP1B1 substrates, is contraindicated (see CONTRAINDICATIONS ). (E) In vitro studies of CYP enzymes, UGTA enzymes and OATP1B1 transporter: In vitro studies have shown that gemfibrozil is an inhibitor of CYP1A2, CYP2C8, CYP2C9, CYP2C19, OATP1B1, and UDP-glucuronosyltransferase (UGT) 1A1 and 1A3 (see WARNINGS ). (F) Bile Acid-Binding Resins: Gemfibrozil AUC was reduced by 30% when gemfibrozil was given (600 mg) simultaneously with resin-granule drugs such as colestipol (5 g). Administration of the drugs two hours or more apart is recommended because gemfibrozil exposure was not significantly affected when it was administered two hours apart from colestipol. (G) Colchicine: Myopathy, including rhabdomyolysis, has been reported with chronic administration of colchicine at therapeutic doses. Concomitant use of gemfibrozil may potentiate the development of myopathy. Patients with renal dysfunction and elderly patients are at increased risk. Caution should be exercised when prescribing gemfibrozil with colchicine, especially in elderly patients or patients with renal dysfunction.
DESCRIPTION
Gemfibrozil tablets, USP 600 mg is a lipid regulating agent. It is available as tablets for oral administration. Each tablet contains 600 mg gemfibrozil. Each tablet also contains calcium stearate, NF; microcrystalline cellulose, NF; hydroxypropyl cellulose, NF; polysorbate 80, NF; colloidal silicon dioxide, NF; pregelatinized starch (maize starch), NF; croscarmellose sodium, NF; opadry white; opacode Blue. opadry white contains hypromellose, titanium dioxide, polyethylene glycol 400 and opacode blue contains shellac, FD&C Blue #1, N-butyl alcohol, titanium dioxide, propylene glycol, isopropyl alcohol. The chemical name is 5-(2,5-dimethylphenoxy)-2,2 dimethylpentanoic acid, with the following structural formula:
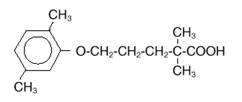
The empirical formula is C 15 H 22 O 3 and the molecular weight is 250.35; the solubility in water and acid is 0.0019% and in dilute base it is greater than 1%. The melting point is 58°–61° C. Gemfibrozil, USP is a white solid which is stable under ordinary conditions.
CLINICAL PHARMACOLOGY
Gemfibrozil is a lipid regulating agent which decreases serum triglycerides and very low density lipoprotein (VLDL) cholesterol, and increases high density lipoprotein (HDL) cholesterol. While modest decreases in total and low density lipoprotein (LDL) cholesterol may be observed with gemfibrozil therapy, treatment of patients with elevated triglycerides due to Type IV hyperlipoproteinemia often results in a rise in LDL-cholesterol. LDL-cholesterol levels in Type IIb patients with elevations of both serum LDL-cholesterol and triglycerides are, in general, minimally affected by gemfibrozil treatment; however, gemfibrozil usually raises HDL-cholesterol significantly in this group. Gemfibrozil increases levels of high density lipoprotein (HDL) subfractions HDL 2 and HDL 3 , as well as apolipoproteins AI and AII. Epidemiological studies have shown that both low HDL-cholesterol and high LDL-cholesterol are independent risk factors for coronary heart disease. In the primary prevention component of the Helsinki Heart Study, in which 4081 male patients between the ages of 40 and 55 were studied in a randomized, double-blind, placebo-controlled fashion, gemfibrozil therapy was associated with significant reductions in total plasma triglycerides and a significant increase in high density lipoprotein cholesterol. Moderate reductions in total plasma cholesterol and low density lipoprotein cholesterol were observed for the gemfibrozil treatment group as a whole, but the lipid response was heterogeneous, especially among different Fredrickson types. The study involved subjects with serum non-HDL-cholesterol of over 200 mg/dL and no previous history of coronary heart disease. Over the five-year study period, the gemfibrozil group experienced a 1.4% absolute (34% relative) reduction in the rate of serious coronary events (sudden cardiac deaths plus fatal and nonfatal myocardial infarctions) compared to placebo, p=0.04 (see Table I). There was a 37% relative reduction in the rate of nonfatal myocardial infarction compared to placebo, equivalent to a treatment-related difference of 13.1 events per thousand persons. Deaths from any cause during the double-blind portion of the study totaled 44(2.2%) in the gemfibrozil randomization group and 43 (2.1% )in the placebo group. Table I Reduction in CHD Rates (events per 1000 patients) by Baseline Lipids 1 in the Helsinki Heart Study, Years 0–5 2
| Incidence of Events 4 | All Patients | LDL-C>175; HDL-C>46.4 | LDL-C>175; TG>177 | LDL-C>175; TG>200; HDL-C<35 | ||||||||
| P | L | Dif 3 | P | L | Dif | P | L | Dif | P | L | Dif | |
| 41 | 27 | 14 | 32 | 29 | 3 | 71 | 44 | 27 | 149 | 64 | 85 | |
1 lipid values in mg/dL at baseline 2 P = placebo group; L= Gemfibrozil group 3 difference in rates between placebo and Gemfibrozil groups 4 fatal and nonfatal myocardial infarctions plus sudden cardiac deaths (events per 1000 patients over 5 years) Among Fredrickson types, during the 5-year double-blind portion of the primary prevention component of the Helsinki Heart Study, the greatest reduction in the incidence of serious coronary events occurred in Type IIb patients who had elevations of both LDL-cholesterol and total plasma triglycerides. This subgroup of Type IIb gemfibrozil group patients had a lower mean HDL-cholesterol level at baseline than the Type IIa subgroup that had elevations of LDL-cholesterol and normal plasma triglycerides. The mean increase in HDL-cholesterol among the Type IIb patients in this study was 12.6% compared to placebo. The mean change in LDL-cholesterol among Type IIb patients was –4.1% with gemfibrozil compared to a rise of 3.9% in the placebo subgroup. The Type IIb subjects in the Helsinki Heart Study had 26 fewer coronary events per thousand persons over five years in the gemfibrozil group compared to placebo. The difference in coronary events was substantially greater between gemfibrozil and placebo for that subgroup of patients with the triad of LDL-cholesterol >175 mg/dL (>4.5 mmol), triglycerides >200 mg/dL(>2.2 mmol),and HDL-cholesterol <35 mg/dL (<0.90 mmol)(see Table I). Further information is available from a 3.5 year (8.5 year cumulative) follow-up of all subjects who had participated in the Helsinki Heart Study. At the completion of the Helsinki Heart Study, subjects could choose to start, stop, or continue to receive gemfibrozil; without knowledge of their own lipid values or double-blind treatment, 60% of patients originally randomized to placebo began therapy with gemfibrozil and 60% of patients originally randomized to gemfibrozil continued medication. After approximately 6.5 years following randomization, all patients were informed of their original treatment group and lipid values during the five years of the double-blind treatment. After further elective changes in gemfibrozil treatment status, 61% of patients in the group originally randomized to gemfibrozil were taking drug; in the group originally randomized to placebo, 65% were taking gemfibrozil. The event rate per 1000 occurring during the open-label follow-up period is detailed in Table II. Table II Cardiac Events and All-Cause Mortality (events per 1000 patients) Occurring During the 3.5 Year Open-Label Follow-up to the Helsinki Heart Study 1
| Group | PDrop | PN | PL | LDrop | LN | LL |
| N=215 | N=494 | N=1283 | N=221 | N=574 | N=1207 | |
| Cardiac Events | 38.8 | 22.9 | 22.5 | 37.2 | 28.3 | 25.4 |
| All-Cause Mortality | 41.9 | 22.3 | 15.6 | 72.3 | 19.2 | 24.9 |
1 The six open-label groups are designated first by the original randomization (P = placebo, L = Gemfibrozil) and then by the drug taken in the follow-up period (N = Attend clinic but took no drug, L = Gemfibrozil, Drop = No attendance at clinic during open-label). Cumulative mortality through 8.5 years showed a 20% relative excess of deaths in the group originally randomized to gemfibrozil versus the originally randomized placebo group and a 20% relative decrease in cardiac events in the group originally randomized to gemfibrozil versus the originally randomized placebo group (see Table III). This analysis of the originally randomized "intent-to-treat'' population neglects the possible complicating effects of treatment switching during the open-label phase. Adjustment of hazard ratios taking into account open-label treatment status from years 6.5 to 8.5, could change the reported hazard ratios for mortality toward unity. Table III Cardiac Events, Cardiac Deaths, Non-Cardiac Deaths, and All-Cause Mortality in the Helsinki Heart Study, Years 0–8.5 1
| Event | Gemfibrozil at Study Start | Placebo at Study Start | Gemfibrozil: Placebo Hazard Ratio 2 | CI Hazard Ratio 3 |
| Cardiac Events 4 | 110 | 131 | 0.80 | 0.62-1.03 |
| Cardiac Deaths | 36 | 38 | 0.98 | 0.63-1.54 |
| Non-Cardiac Deaths | 65 | 45 | 1.40 | 0.95-2.05 |
| All-Cause Mortality | 101 | 83 | 1.20 | 0.90-1.61 |
1 Intention-to-Treat Analysis of originally randomized patients neglecting the open-label treatment switches and exposure to study conditions. 2 Hazard ratio for risk event in the group originally randomized to gemfibrozil compared to the group originally randomized to placebo neglecting open-label treatment switch and exposure to study conditions. 3 95% confidence intervals of gemfibrozil: placebo group hazard ratio 4 Fatal and non-fatal myocardial infarctions plus sudden cardiac deaths over the 8.5 year period. It is not clear to what extent the findings of the primary prevention component of the Helsinki Heart Study can be extrapolated to other segments of the dyslipidemic population not studied (such as women, younger or older males, or those with lipid abnormalities limited solely to HDL-cholesterol) or to other lipid-altering drugs.
The secondary prevention component of the Helsinki Heart Study was conducted over five years in parallel and at the same centers in Finland in 628 middle-aged males excluded from the primary prevention component of the Helsinki Heart Study because of a history of angina, myocardial infarction, or unexplained ECG changes. The primary efficacy endpoint of the study was cardiac events (the sum of fatal and non-fatal myocardial infarctions and sudden cardiac deaths). The hazard ratio (gemfibrozil: placebo) for cardiac events was 1.47 (95% confidence limits 0.88–2.48, p=0.14). Of the 35 patients in the gemfibrozil group who experienced cardiac events, 12 patients suffered events after discontinuation from the study. Of the 24 patients in the placebo group with cardiac events, 4 patients suffered events after discontinuation from the study. There were 17 cardiac deaths in the gemfibrozil group and 8 in the placebo group (hazard ratio 2.18; 95% confidence limits 0.94–5.05, p=0.06). Ten of these deaths in the gemfibrozil group and 3 in the placebo group occurred after discontinuation from therapy. In this study of patients with known or suspected coronary heart disease, no benefit from gemfibrozil treatment was observed in reducing cardiac events or cardiac deaths. Thus, gemfibrozil has shown benefit only in selected dyslipidemic patients without suspected or established coronary heart disease. Even in patients with coronary heart disease and the triad of elevated LDL-cholesterol, elevated triglycerides, plus low HDL-cholesterol, the possible effect of gemfibrozil on coronary events has not been adequately studied. No efficacy in the patients with established coronary heart disease was observed during the Coronary Drug Project with the chemically and pharmacologically related drug, clofibrate. The Coronary Drug Project was a 6-year randomized, double-blind study involving 1000 clofibrate, 1000 nicotinic acid, and 3000 placebo patients with known coronary heart disease. A clinically and statistically significant reduction in myocardial infarctions was seen in the concurrent nicotinic acid group compared to placebo; no reduction was seen with clofibrate.
The mechanism of action of gemfibrozil has not been definitely established. In man, gemfibrozil has been shown to inhibit peripheral lipolysis and to decrease the hepatic extraction of free fatty acids, thus reducing hepatic triglyceride production. Gemfibrozil inhibits synthesis and increases clearance of VLDL carrier apolipoprotein B, leading to a decrease in VLDL production. Animal studies suggest that gemfibrozil may, in addition to elevating HDL-cholesterol, reduce incorporation of long-chain fatty acids into newly formed triglycerides, accelerate turnover and removal of cholesterol from the liver, and increase excretion of cholesterol in the feces. Gemfibrozil is well absorbed from the gastrointestinal tract after oral administration. Peak plasma levels occur in 1 to 2 hours with a plasma half-life of 1.5 hours following multiple doses.
Gemfibrozil is completely absorbed after oral administration of gemfibrozil tablets, reaching peak plasma concentrations 1 to 2 hours after dosing. Gemfibrozil pharmacokinetics are affected by the timing of meals relative to time of dosing. In one study (ref. 4), both the rate and extent of absorption of the drug were significantly increased when administered 0.5 hour before meals. Average AUC was reduced by 14–44% when gemfibrozil was administered after meals compared to 0.5 hour before meals. In a subsequent study, rate of absorption of gemfibrozil was maximum when administered 0.5 hour before meals with the C max 50–60% greater than when given either with meals or fasting. In this study, there were no significant effects on AUC of timing of dose relative to meals (see DOSAGE AND ADMINISTRATION ). Gemfibrozil mainly undergoes oxidation of a ring methyl group to successively form a hydroxymethyl and a carboxyl metabolite. Approximately seventy percent of the administered human dose is excreted in the urine, mostly as the glucuronide conjugate, with less than 2% excreted as unchanged gemfibrozil. Six percent of the dose is accounted for in the feces. Gemfibrozil is highly bound to plasma proteins and there is potential for displacement interactions with other drugs (see PRECAUTIONS ).
HOW SUPPLIED
Gemfibrozil Tablets, USP 600 mg: White, elliptical, film-coated, scored tablets, imprinted 'C17' on one side,are available as follows:
NDC 71209-008-03: Bottles of 60
NDC 71209-008-08: Bottles of 180
NDC 71209-008-10: Bottles of 500
Store at controlled room temperature 20° – 25°C (68° – 77°F) [see USP]. Protect from light and humidity. R x only Manufactured by: Cadila Pharmaceuticals Limited, 1389 Trasad Road, Dholka, District - Ahmedabad, Gujarat, INDIA Revised: January 2021