Get your patient on Itraconazole - Itraconazole capsule (Itraconazole)
Itraconazole - Itraconazole capsule prescribing information
BOXED WARNING
Congestive Heart Failure, Cardiac Effects and Drug Interactions
Congestive Heart Failure and Cardiac Effects
- Itraconazole Capsules should not be administered for the treatment of onychomycosis in patients with evidence of ventricular dysfunction such as congestive heart failure (CHF) or a history of CHF. If signs or symptoms of congestive heart failure occur during administration of Itraconazole Capsules, discontinue administration.
- When itraconazole was administered intravenously to dogs and healthy human volunteers, negative inotropic effects were seen. (See CONTRAINDICATIONS , WARNINGS , PRECAUTIONS: Drug Interactions , ADVERSE REACTIONS: Postmarketing Experience , and CLINICAL PHARMACOLOGY: Special Populations for more information.)
Drug Interactions:
- Coadministration of a number of CYP3A4 substrates are contraindicated with Itraconazole Capsules. Some examples of drugs that are contraindicated for coadministration with Itraconazole Capsules are: methadone, disopyramide, dofetilide, dronedarone, quinidine, isavuconazole, ergot alkaloids (such as dihydroergotamine, ergometrine (ergonovine), ergotamine, methylergometrine (methylergonovine)), irinotecan, lurasidone, oral midazolam, pimozide, triazolam, felodipine, nisoldipine, ivabradine, ranolazine, eplerenone, cisapride, naloxegol, lomitapide, lovastatin, simvastatin, avanafil, ticagrelor, finerenone, voclosporin.
- Coadministration with colchicine, fesoterodine and solifenacin is contraindicated in subjects with varying degrees of renal or hepatic impairment.
- Coadministration with eliglustat is contraindicated in subjects that are poor or intermediate metabolizers of CYP2D6 and in subjects taking strong or moderate CYP2D6 inhibitors.
- Coadministration with venetoclax is contraindicated in patients with chronic lymphocytic leukemia (CLL)/small lymphocytic lymphoma (SLL) during the dose initiation and ramp-up phase of venetoclax. See PRECAUTIONS: Drug Interactions Section for specific examples.
- Coadministration with itraconazole can cause elevated plasma concentrations of these drugs and may increase or prolong both the pharmacologic effects and/or adverse reactions to these drugs. For example, increased plasma concentrations of some of these drugs can lead to QT prolongation and ventricular tachyarrhythmias including occurrences of torsade de pointes, a potentially fatal arrhythmia. See CONTRAINDICATIONS and WARNINGS Sections, and PRECAUTIONS: Drug Interactions Section for specific examples.
INDICATIONS AND USAGE
Itraconazole Capsules are indicated for the treatment of the following fungal infections in immunocompromised and non-immunocompromised patients:
- Blastomycosis, pulmonary and extrapulmonary
- Histoplasmosis, including chronic cavitary pulmonary disease and disseminated, non-meningeal histoplasmosis, and
- Aspergillosis, pulmonary and extrapulmonary, in patients who are intolerant of or who are refractory to amphotericin B therapy.
Specimens for fungal cultures and other relevant laboratory studies (wet mount, histopathology, serology) should be obtained before therapy to isolate and identify causative organisms. Therapy may be instituted before the results of the cultures and other laboratory studies are known; however, once these results become available, antiinfective therapy should be adjusted accordingly.
Itraconazole Capsules are also indicated for the treatment of the following fungal infections in non-immunocompromised patients:
- Onychomycosis of the toenail, with or without fingernail involvement, due to dermatophytes (tinea unguium), and
- Onychomycosis of the fingernail due to dermatophytes (tinea unguium).
Prior to initiating treatment, appropriate nail specimens for laboratory testing (KOH preparation, fungal culture, or nail biopsy) should be obtained to confirm the diagnosis of onychomycosis.
(See CLINICAL PHARMACOLOGY: Special Populations , CONTRAINDICATIONS , WARNINGS , and ADVERSE REACTIONS: Postmarketing Experience for more information.)
Description of Clinical Studies
Blastomycosis
Analyses were conducted on data from two open-label, non-concurrently controlled studies (N=73 combined) in patients with normal or abnormal immune status. The median dose was 200 mg/day. A response for most signs and symptoms was observed within the first 2 weeks, and all signs and symptoms cleared between 3 and 6 months. Results of these two studies demonstrated substantial evidence of the effectiveness of itraconazole for the treatment of blastomycosis compared with the natural history of untreated cases.
Histoplasmosis
Analyses were conducted on data from two open-label, non-concurrently controlled studies (N=34 combined) in patients with normal or abnormal immune status (not including HIV-infected patients). The median dose was 200 mg/day. A response for most signs and symptoms was observed within the first 2 weeks, and all signs and symptoms cleared between 3 and 12 months. Results of these two studies demonstrated substantial evidence of the effectiveness of itraconazole for the treatment of histoplasmosis, compared with the natural history of untreated cases.
Histoplasmosis in HIV-infected patients
Data from a small number of HIV-infected patients suggested that the response rate of histoplasmosis in HIV-infected patients is similar to that of non-HIV-infected patients. The clinical course of histoplasmosis in HIV-infected patients is more severe and usually requires maintenance therapy to prevent relapse.
Aspergillosis
Analyses were conducted on data from an open-label, "single-patient-use" protocol designed to make itraconazole available in the U.S. for patients who either failed or were intolerant of amphotericin B therapy (N=190). The findings were corroborated by two smaller open-label studies (N=31 combined) in the same patient population. Most adult patients were treated with a daily dose of 200 to 400 mg, with a median duration of 3 months. Results of these studies demonstrated substantial evidence of effectiveness of itraconazole as a second-line therapy for the treatment of aspergillosis compared with the natural history of the disease in patients who either failed or were intolerant of amphotericin B therapy.
Onychomycosis of the toenail
Analyses were conducted on data from three double-blind, placebo-controlled studies (N=214 total; 110 given Itraconazole Capsules) in which patients with onychomycosis of the toenails received 200 mg of Itraconazole Capsules once daily for 12 consecutive weeks. Results of these studies demonstrated mycologic cure, defined as simultaneous occurrence of negative KOH plus negative culture, in 54% of patients. Thirty-five percent (35%) of patients were considered an overall success (mycologic cure plus clear or minimal nail involvement with significantly decreased signs) and 14% of patients demonstrated mycologic cure plus clinical cure (clearance of all signs, with or without residual nail deformity). The mean time to overall success was approximately 10 months. Twenty-one percent (21%) of the overall success group had a relapse (worsening of the global score or conversion of KOH or culture from negative to positive).
Onychomycosis of the fingernail
Analyses were conducted on data from a double-blind, placebo-controlled study (N=73 total; 37 given Itraconazole Capsules) in which patients with onychomycosis of the fingernails received a 1-week course (pulse) of 200 mg of Itraconazole Capsules b.i.d., followed by a 3-week period without Itraconazole Capsules, which was followed by a second 1-week pulse of 200 mg of Itraconazole Capsules b.i.d. Results demonstrated mycologic cure in 61% of patients. Fifty-six percent (56%) of patients were considered an overall success and 47% of patients demonstrated mycologic cure plus clinical cure. The mean time to overall success was approximately 5 months. None of the patients who achieved overall success relapsed.
DOSAGE AND ADMINISTRATION
Itraconazole Capsules should be taken with a full meal to ensure maximal absorption. Itraconazole Capsules must be swallowed whole.
Itraconazole Capsules are a different preparation than SPORANOX ® (itraconazole) Oral Solution and should not be used interchangeably.
Treatment of Blastomycosis and Histoplasmosis
The recommended dose is 200 mg once daily (2 capsules). If there is no obvious improvement, or there is evidence of progressive fungal disease, the dose should be increased in 100-mg increments to a maximum of 400 mg daily. Doses above 200 mg/day should be given in two divided doses.
Treatment of Aspergillosis
A daily dose of 200 to 400 mg is recommended.
Treatment in Life-Threatening Situations
In life-threatening situations, a loading dose should be used.
Although clinical studies did not provide for a loading dose, it is recommended, based on pharmacokinetic data, that a loading dose of 200 mg (2 capsules) three times daily (600 mg/day) be given for the first 3 days of treatment.
Treatment should be continued for a minimum of three months and until clinical parameters and laboratory tests indicate that the active fungal infection has subsided. An inadequate period of treatment may lead to recurrence of active infection.
Itraconazole Capsules and SPORANOX ® (itraconazole) Oral Solution should not be used interchangeably. Only the Oral Solution has been demonstrated effective for oral and/or esophageal candidiasis.
Treatment of Onychomycosis
Toenails with or without fingernail involvement
The recommended dose is 200 mg (2 capsules) once daily for 12 consecutive weeks.
Treatment of Onychomycosis
Fingernails only
The recommended dosing regimen is 2 treatment pulses, each consisting of 200 mg (2 capsules) b.i.d. (400 mg/day) for 1 week. The pulses are separated by a 3-week period without itraconazole.
Use in Patients with Renal Impairment
Limited data are available on the use of oral itraconazole in patients with renal impairment. Caution should be exercised when this drug is administered in this patient population. (See CLINICAL PHARMACOLOGY: Special Populations and PRECAUTIONS .)
Use in Patients with Hepatic Impairment
Limited data are available on the use of oral itraconazole in patients with hepatic impairment. Caution should be exercised when this drug is administered in this patient population. (See CLINICAL PHARMACOLOGY: Special Populations , WARNINGS , and PRECAUTIONS .)
CONTRAINDICATIONS
Congestive Heart Failure
Itraconazole Capsules should not be administered for the treatment of onychomycosis in patients with evidence of ventricular dysfunction such as congestive heart failure (CHF) or a history of CHF. (See BOXED WARNING , WARNINGS , PRECAUTIONS: Drug Interactions-Calcium Channel Blockers, ADVERSE REACTIONS: Postmarketing Experience , and CLINICAL PHARMACOLOGY: Special Populations .)
Drug Interactions
Coadministration of a number of CYP3A4 substrates are contraindicated with itraconazole. Some examples of drugs for which plasma concentrations increase are: methadone, disopyramide, dofetilide, dronedarone, quinidine, isavuconazole, ergot alkaloids (such as dihydroergotamine, ergometrine (ergonovine), ergotamine, methylergometrine (methylergonovine)), irinotecan, lurasidone, oral midazolam, pimozide, triazolam, felodipine, nisoldipine, ivabradine, ranolazine, eplerenone, cisapride, naloxegol, lomitapide, lovastatin, simvastatin, avanafil, ticagrelor, finerenone, voclosporin. In addition, coadministration with colchicine, fesoterodine and solifenacin is contraindicated in subjects with varying degrees of renal or hepatic impairment, and coadministration with eliglustat is contraindicated in subjects that are poor or intermediate metabolizers of CYP2D6 and in subjects taking strong or moderate CYP2D6 inhibitors. (See PRECAUTIONS: Drug Interactions Section for specific examples.) This increase in drug concentrations caused by coadministration with itraconazole may increase or prolong both the pharmacologic effects and/or adverse reactions to these drugs. For example, increased plasma concentrations of some of these drugs can lead to QT prolongation and ventricular tachyarrhythmias including occurrences of torsade de pointes, a potentially fatal arrhythmia. Some specific examples are listed in PRECAUTIONS: Drug Interactions.
Coadministration with venetoclax is contraindicated in patients with CLL/SLL during the dose initiation and ramp-up phase of venetoclax due to the potential for an increased risk of tumor lysis syndrome.
Itraconazole should not be administered for the treatment of onychomycosis to pregnant patients or to women contemplating pregnancy.
Itraconazole is contraindicated for patients who have shown hypersensitivity to itraconazole. There is limited information regarding cross-hypersensitivity between itraconazole and other azole antifungal agents. Caution should be used when prescribing itraconazole to patients with hypersensitivity to other azoles.
ADVERSE REACTIONS
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
Itraconazole has been associated with rare cases of serious hepatotoxicity, including liver failure and death. Some of these cases had neither pre-existing liver disease nor a serious underlying medical condition. If clinical signs or symptoms develop that are consistent with liver disease, treatment should be discontinued and liver function testing performed. The risks and benefits of itraconazole use should be reassessed. (See WARNINGS: Hepatic Effects and PRECAUTIONS: Hepatotoxicity and Information for Patients .)
Adverse Events in the Treatment of Systemic Fungal Infections
Adverse event data were derived from 602 patients treated for systemic fungal disease in U.S. clinical trials who were immunocompromised or receiving multiple concomitant medications. Treatment was discontinued in 10.5% of patients due to adverse events. The median duration before discontinuation of therapy was 81 days (range: 2 to 776 days). The table lists adverse events reported by at least 1% of patients.
| Body System/Adverse Event | Incidence (%) (N=602) |
|---|---|
| Gastrointestinal | |
| Nausea | 11 |
| Vomiting | 5 |
| Diarrhea | 3 |
| Abdominal Pain | 2 |
| Anorexia | 1 |
| Body as a Whole | |
| Edema | 4 |
| Fatigue | 3 |
| Fever | 3 |
| Malaise | 1 |
| Skin and Appendages | |
| Rash Rash tends to occur more frequently in immunocompromised patients receiving immunosuppressive medications. | 9 |
| Pruritus | 3 |
| Central/Peripheral Nervous System | |
| Headache | 4 |
| Dizziness | 2 |
| Psychiatric | |
| Libido Decreased | 1 |
| Somnolence | 1 |
| Cardiovascular | |
| Hypertension | 3 |
| Metabolic/Nutritional | |
| Hypokalemia | 2 |
| Urinary System | |
| Albuminuria | 1 |
| Liver and Biliary System | |
| Hepatic Function Abnormal | 3 |
| Reproductive System, Male | |
| Impotence | 1 |
Adverse events infrequently reported in all studies included constipation, gastritis, depression, insomnia, tinnitus, menstrual disorder, adrenal insufficiency, gynecomastia, and male breast pain.
Adverse Events Reported in Toenail Onychomycosis Clinical Trials
Patients in these trials were on a continuous dosing regimen of 200 mg once daily for 12 consecutive weeks.
The following adverse events led to temporary or permanent discontinuation of therapy.
| Adverse Event | Incidence (%) Itraconazole (N=112) |
|---|---|
| Elevated Liver Enzymes (greater than twice the upper limit of normal) | 4 |
| Gastrointestinal Disorders | 4 |
| Rash | 3 |
| Hypertension | 2 |
| Orthostatic Hypotension | 1 |
| Headache | 1 |
| Malaise | 1 |
| Myalgia | 1 |
| Vasculitis | 1 |
| Vertigo | 1 |
The following adverse events occurred with an incidence of greater than or equal to 1% (N=112): headache: 10%; rhinitis: 9%; upper respiratory tract infection: 8%; sinusitis, injury: 7%; diarrhea, dyspepsia, flatulence, abdominal pain, dizziness, rash: 4%; cystitis, urinary tract infection, liver function abnormality, myalgia, nausea: 3%; appetite increased, constipation, gastritis, gastroenteritis, pharyngitis, asthenia, fever, pain, tremor, herpes zoster, abnormal dreaming: 2%.
Adverse Events Reported in Fingernail Onychomycosis Clinical Trials
Patients in these trials were on a pulse regimen consisting of two 1-week treatment periods of 200 mg twice daily, separated by a 3-week period without drug.
The following adverse events led to temporary or permanent discontinuation of therapy.
| Adverse Event | Incidence (%) Itraconazole (N=37) |
|---|---|
| Rash/Pruritus | 3 |
| Hypertriglyceridemia | 3 |
The following adverse events occurred with an incidence of greater than or equal to 1% (N=37): headache: 8%; pruritus, nausea, rhinitis: 5%; rash, bursitis, anxiety, depression, constipation, abdominal pain, dyspepsia, ulcerative stomatitis, gingivitis, hypertriglyceridemia, sinusitis, fatigue, malaise, pain, injury: 3%.
Adverse Events Reported from Other Clinical Trials
In addition, the following adverse drug reaction was reported in patients who participated in Itraconazole Capsules clinical trials: Hepatobiliary Disorders: hyperbilirubinemia.
The following is a list of additional adverse drug reactions associated with itraconazole that have been reported in clinical trials of SPORANOX ® Oral Solution and itraconazole IV excluding the adverse reaction term "Injection site inflammation" which is specific to the injection route of administration:
Cardiac Disorders: cardiac failure, left ventricular failure, tachycardia;
General Disorders and Administration Site Conditions: face edema, chest pain, chills;
Hepatobiliary Disorders: hepatic failure, jaundice;
Investigations: alanine aminotransferase increased, aspartate aminotransferase increased, blood alkaline phosphatase increased, blood lactate dehydrogenase increased, blood urea increased, gamma-glutamyltransferase increased, urine analysis abnormal;
Metabolism and Nutrition Disorders: hyperglycemia, hyperkalemia, hypomagnesemia;
Psychiatric Disorders: confusional state;
Renal and Urinary Disorders: renal impairment;
Respiratory, Thoracic and Mediastinal Disorders: dysphonia, cough;
Skin and Subcutaneous Tissue Disorders: rash erythematous, hyperhidrosis;
Vascular Disorders: hypotension
Postmarketing Experience
Adverse drug reactions that have been first identified during postmarketing experience with itraconazole (all formulations) are listed in the table below. Because these reactions are reported voluntarily from a population of uncertain size, reliably estimating their frequency or establishing a causal relationship to drug exposure is not always possible.
| Blood and Lymphatic System Disorders: | Leukopenia, neutropenia, thrombocytopenia |
| Immune System Disorders: | Anaphylaxis; anaphylactic, anaphylactoid and allergic reactions; serum sickness; angioneurotic edema |
| Endocrine Disorders: | Pseudoaldosteronism |
| Nervous System Disorders: | Peripheral neuropathy, paresthesia, hypoesthesia, tremor |
| Eye Disorders: | Visual disturbances, including vision blurred and diplopia |
| Ear and Labyrinth Disorders: | Transient or permanent hearing loss |
| Cardiac Disorders: | Congestive heart failure, bradycardia |
| Respiratory, Thoracic and Mediastinal Disorders: | Pulmonary edema, dyspnea |
| Gastrointestinal Disorders: | Pancreatitis, dysgeusia |
| Hepatobiliary Disorders: | Serious hepatotoxicity (including some cases of fatal acute liver failure), hepatitis |
| Skin and Subcutaneous Tissue Disorders: | Toxic epidermal necrolysis, Stevens-Johnson syndrome, acute generalized exanthematous pustulosis, erythema multiforme, exfoliative dermatitis, leukocytoclastic vasculitis, alopecia, photosensitivity, urticaria |
| Musculoskeletal and Connective Tissue Disorders: | Arthralgia |
| Renal and Urinary Disorders: | Urinary incontinence, pollakiuria |
| Reproductive System and Breast Disorders: | Erectile dysfunction |
| General Disorders and Administration Site Conditions: | Peripheral edema |
| Investigations: | Blood creatine phosphokinase increased |
There is limited information on the use of itraconazole during pregnancy. Cases of congenital abnormalities including skeletal, genitourinary tract, cardiovascular and ophthalmic malformations as well as chromosomal and multiple malformations have been reported during postmarketing experience. A causal relationship with itraconazole has not been established. (See CLINICAL PHARMACOLOGY: Special Populations , CONTRAINDICATIONS , WARNINGS , and PRECAUTIONS: Drug Interactions for more information.)
Drug Interactions:
Effect of Itraconazole Capsules on Other Drugs
Itraconazole and its major metabolite, hydroxy-itraconazole, are potent CYP3A4 inhibitors. Itraconazole is an inhibitor of the drug transporters P-glycoprotein and breast cancer resistance protein (BCRP). Consequently, Itraconazole Capsules has the potential to interact with many concomitant drugs resulting in either increased or sometimes decreased concentrations of the concomitant drugs. Increased concentrations may increase the risk of adverse reactions associated with the concomitant drug which can be severe or life-threatening in some cases (e.g., QT prolongation, torsade de pointes, respiratory depression, hepatic adverse reactions, hypersensitivity reactions, myelosuppression, hypotension, seizures, angioedema, atrial fibrillation, bradycardia, priapism). Reduced concentrations of concomitant drugs may reduce their efficacy. Table 1 lists examples of drugs that may have their concentrations affected by itraconazole, but it is not a comprehensive list.
Refer to the approved product labeling to become familiar with the interaction pathways, risk potential, and specific actions to be taken with regards to each concomitant drug prior to initiating therapy with Itraconazole Capsules.
Although many of the clinical drug interactions in Table 1 are based on information with a similar azole antifungal, ketoconazole, these interactions are expected to occur with Itraconazole Capsules.
| Examples of Concomitant Drugs Within Class | Prevention or Management | |
|---|---|---|
| Drug Interactions with Itraconazole Capsules that Increase Concomitant Drug Concentrations and May Increase Risk of Adverse Reactions Associated with the Concomitant Drug | ||
| Alpha Blockers | ||
| Alfuzosin Silodosin Tamsulosin | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Analgesics | ||
| Methadone | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Fentanyl | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Alfentanil Buprenorphine (IV and sublingual) Oxycodone Based on clinical drug interaction information with itraconazole. Sufentanil | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Antiarrhythmics | ||
| Disopyramide Dofetilide Dronedarone Quinidine | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Digoxin | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Antibacterials | ||
| Bedaquiline Based on 400 mg bedaquiline once daily for 2 weeks. | Concomitant Itraconazole Capsules not recommended for more than 2 weeks at any time during bedaquiline treatment. | |
| Rifabutin | Not recommended 2 weeks before, during, and 2 weeks after Itraconazole Capsules treatment. See also Table 2 . | |
| Clarithromycin | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. See also Table 2 . | |
| Trimetrexate | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Anticoagulants and Antiplatelets | ||
| Ticagrelor | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Apixaban Rivaroxaban Vorapaxar | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Cilostazol Dabigatran Warfarin | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Anticonvulsants | ||
| Carbamazepine | Not recommended 2 weeks before, during, and 2 weeks after Itraconazole Capsules treatment. See also Table 2 . | |
| Antidiabetic Drugs | ||
| Repaglinide Saxagliptin | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Antihelminthics, Antifungals and Antiprotozoals | ||
| Isavuconazonium | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Praziquantel | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Artemether-lumefantrine Quinine | Monitor for adverse reactions. | |
| Antimigraine Drugs | ||
| Ergot alkaloids (e.g., dihydroergotamine, ergotamine) | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Eletriptan | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Antineoplastics | ||
| Irinotecan | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Venetoclax | Contraindicated during the dose initiation and ramp-up phase in patients with CLL/SLL. Refer to the venetoclax prescribing information for dosing and safety monitoring instructions. | |
| Mobocertinib | Avoid use during and 2 weeks after Itraconazole Capsules treatment. | |
| Axitinib Bosutinib Cabazitaxel Cabozantinib Ceritinib Cobimetinib Crizotinib Dabrafenib Dasatinib Docetaxel | Ibrutinib Lapatinib Nilotinib Olaparib Pazopanib Sunitinib Trabectedin Trastuzumab- emtansine Vinca alkaloids | Avoid use during and 2 weeks after Itraconazole Capsules treatment. |
| Entrectinib Pemigatinib Talazoparib | Refer to the entrectinib, pemigatinib and talazoparib prescribing information for dosing instructions if concomitant use cannot be avoided. | |
| Glasdegib | Refer to the glasdegib prescribing information for safety monitoring if concomitant use cannot be avoided. | |
| Bortezomib Brentuximab- vedotin Busulfan Erlotinib Gefitinib Idelalisib Imatinib Ixabepilone | Nintedanib Panobinostat Ponatinib Ruxolitinib Sonidegib Tretinoin (oral) Vandetanib | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. For idelalisib, see also Table 2 . |
| Antipsychotics, Anxiolytics and Hypnotics | ||
| Alprazolam Aripiprazole Buspirone Cariprazine Diazepam Haloperidol | Midazolam (IV) Quetiapine Ramelteon Risperidone Suvorexant | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. |
| Zopiclone | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Lurasidone Midazolam (oral) Pimozide Triazolam | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Antivirals | ||
| Daclatasvir Indinavir Maraviroc | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. For indinavir, see also Table 2 . | |
| Cobicistat Elvitegravir (ritonavir-boosted) Ombitasvir/Paritaprevir/Ritonavir with or without Dasabuvir Ritonavir Saquinavir (unboosted) | Monitor for adverse reactions. See also Table 2 . | |
| Elbasvir/grazoprevir | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Glecaprevir/pibrentasvir | Monitor for adverse reactions. | |
| Tenofovir disoproxil fumarate | Monitor for adverse reactions. | |
| Beta Blockers | ||
| Nadolol | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Calcium Channel Blockers | ||
| Felodipine Nisoldipine | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Diltiazem Other dihydropyridines Verapamil | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. For diltiazem, see also Table 2 . | |
| Cardiovascular Drugs, Miscellaneous | ||
| Ivabradine Ranolazine | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Aliskiren Riociguat Sildenafil (for pulmonary hypertension) Tadalafil (for pulmonary hypertension) | Not recommended during and 2 weeks after Itraconazole Capsules treatment. For sildenafil and tadalafil, see also Urologic Drugs below. | |
| Bosentan Guanfacine | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Contraceptives CYP3A4 inhibitors (including itraconazole) may increase systemic contraceptive hormone concentrations. | ||
| Dienogest Ulipristal | Monitor for adverse reactions. | |
| Diuretics | ||
| Eplerenone Finerenone | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Gastrointestinal Drugs | ||
| Cisapride Naloxegol | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Aprepitant Loperamide | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Netupitant | Monitor for adverse reactions. | |
| Immunosuppressants | ||
| Voclosporin | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Everolimus Sirolimus Temsirolimus (IV) | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Budesonide (inhalation) Budesonide (non-inhalation) Ciclesonide (inhalation) Cyclosporine (IV) Cyclosporine (non-IV) Dexamethasone | Fluticasone (inhalation) Fluticasone (nasal) Methylprednisolone Tacrolimus (IV) Tacrolimus (oral) | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. |
| Lipid-Lowering Drugs | ||
| Lomitapide Lovastatin Simvastatin | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Atorvastatin | Monitor for drug adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Respiratory Drugs | ||
| Salmeterol | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| SSRIs, Tricyclics and Related Antidepressants | ||
| Venlafaxine | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Urologic Drugs | ||
| Avanafil | Contraindicated during and 2 weeks after Itraconazole Capsules treatment. | |
| Fesoterodine | Patients with moderate to severe renal or hepatic impairment : Contraindicated during and 2 weeks after Itraconazole Capsules treatment. Other patients : Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Solifenacin | Patients with severe renal or moderate to severe hepatic impairment : Contraindicated during and 2 weeks after Itraconazole Capsules treatment. Other patients : Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Darifenacin Vardenafil | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Dutasteride Oxybutynin Sildenafil (for erectile dysfunction) Tadalafil (for erectile dysfunction and benign prostatic hyperplasia) Tolterodine | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. For sildenafil and tadalafil, see also Cardiovascular Drugs above. | |
| Miscellaneous Drugs and Other Substances | ||
| Colchicine | Patients with renal or hepatic impairment: Contraindicated during and 2 weeks after Itraconazole Capsules treatment. Other patients : Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Eliglustat | CYP2D6 EMs EMs: extensive metabolizers; IMs: intermediate metabolizers, PMs: poor metabolizers taking a strong or moderate CYP2D6 inhibitor, CYP2D6 IMs, or CYP2D6 PMs : Contraindicated during and 2 weeks after Itraconazole Capsules treatment. CYP2D6 EMsnot taking a strong or moderate CYP2D6 inhibitor : Monitor for adverse reactions. Eliglustat dose reduction may be necessary. | |
| Lumacaftor/Ivacaftor | Not recommended 2 weeks before, during, and 2 weeks after Itraconazole Capsules treatment. | |
| Alitretinoin (oral) Cabergoline Cannabinoids Cinacalcet Galantamine Ivacaftor | Monitor for adverse reactions. Concomitant drug dose reduction may be necessary. | |
| Valbenazine | Concomitant drug dose reduction is necessary. Refer to the valbenazine prescribing information for dosing instructions. | |
| Vasopressin Receptor Antagonists | ||
| Conivaptan Tolvaptan | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Drug Interactions with Itraconazole Capsules that Decrease Concomitant Drug Concentrations and May Reduce Efficacy of the Concomitant Drug | ||
| Antineoplastics | ||
| Regorafenib | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Gastrointestinal Drugs | ||
| Saccharomyces boulardii | Not recommended during and 2 weeks after Itraconazole Capsules treatment. | |
| Nonsteroidal Anti-Inflammatory Drugs | ||
| Meloxicam | Concomitant drug dose increase may be necessary. | |
Effect of Other Drugs on Itraconazole Capsules
Itraconazole is mainly metabolized through CYP3A4. Other substances that either share this metabolic pathway or modify CYP3A4 activity may influence the pharmacokinetics of itraconazole. Some concomitant drugs have the potential to interact with Itraconazole Capsules resulting in either increased or sometimes decreased concentrations of Itraconazole Capsules. Increased concentrations may increase the risk of adverse reactions associated with Itraconazole Capsules. Decreased concentrations may reduce Itraconazole Capsules efficacy.
Table 2 lists examples of drugs that may affect itraconazole concentrations, but is not a comprehensive list. Refer to the approved product labeling to become familiar with the interaction pathways, risk potential and specific actions to be taken with regards to each concomitant drug prior to initiating therapy with Itraconazole Capsules.
Although many of the clinical drug interactions in Table 2 are based on information with a similar azole antifungal, ketoconazole, these interactions are expected to occur with Itraconazole Capsules.
| Examples of Concomitant Drugs Within Class | Prevention or Management |
|---|---|
| Drug Interactions with Other Drugs that Increase Itraconazole Capsules Concentrations and May Increase Risk of Adverse Reactions Associated with Itraconazole Capsules | |
| Antibacterials | |
| Ciprofloxacin Based on clinical drug interaction information with itraconazole. Erythromycin Clarithromycin | Monitor for adverse reactions. Itraconazole Capsules dose reduction may be necessary. |
| Antineoplastics | |
| Idelalisib | Monitor for adverse reactions. Itraconazole Capsules dose reduction may be necessary. See also Table 1 . |
| Antivirals | |
| Cobicistat Darunavir (ritonavir-boosted) Elvitegravir (ritonavir-boosted) Fosamprenavir (ritonavir-boosted) Indinavir Ombitasvir/ Paritaprevir/ Ritonavir with or without Dasabuvir Ritonavir Saquinavir | Monitor for adverse reactions. Itraconazole Capsules dose reduction may be necessary. For, cobicistat, elvitegravir, indinavir, ombitasvir/ paritaprevir/ ritonavir with or without dasabuvir, ritonavir, and saquinavir, see also Table 1 . |
| Calcium Channel Blockers | |
| Diltiazem | Monitor for adverse reactions. Itraconazole Capsules dose reduction may be necessary. See also Table 1 . |
| Drug Interactions with Other Drugs that Decrease Itraconazole Capsules Concentrations and May Reduce Efficacy of Itraconazole Capsules | |
| Antibacterials | |
| Isoniazid Rifampicin | Not recommended 2 weeks before and during Itraconazole Capsules treatment. |
| Rifabutin | Not recommended 2 weeks before, during, and 2 weeks after Itraconazole Capsules treatment. See also Table 1 . |
| Anticonvulsants | |
| Phenobarbital Phenytoin | Not recommended 2 weeks before and during Itraconazole Capsules treatment. |
| Carbamazepine | Not recommended 2 weeks before, during, and 2 weeks after Itraconazole Capsules treatment. See also Table 1 . |
| Antivirals | |
| Efavirenz Nevirapine | Not recommended 2 weeks before and during Itraconazole Capsules treatment. |
| Gastrointestinal Drugs | |
| Drugs that reduce gastric acidity e.g. acid neutralizing medicines such as aluminum hydroxide, or acid secretion suppressors such as H 2 - receptor antagonists and proton pump inhibitors. | Use with caution. Administer acid neutralizing medicines at least 2 hours before or 2 hours after the intake of Itraconazole Capsules. |
| Miscellaneous Drugs and Other Substances | |
| Lumacaftor/Ivacaftor | Not recommended 2 weeks before, during, and 2 weeks after Itraconazole Capsules treatment. |
Pediatric Population
Interaction studies have only been performed in adults.
DESCRIPTION
Itraconazole is an azole antifungal agent. Itraconazole is a 1:1:1:1 racemic mixture of four diastereomers (two enantiomeric pairs), each possessing three chiral centers. It may be represented by the following structural formula and nomenclature:
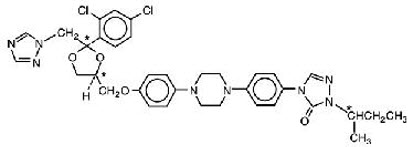
(±)-1-[( R •)- sec -butyl]-4-[ p -[4-[ p -[[(2 R •,4 S •)-2-(2,4-dichlorophenyl)-2-(1 H -1,2,4-triazol-1-ylmethyl)-1,3-dioxolan-4-yl]methoxy]phenyl]-1-piperazinyl]phenyl]-Δ 2 -1,2,4-triazolin-5-one mixture with (±)-1-[( R •)- sec -butyl]-4-[ p -[4-[ p -[[(2 S •,4 R •)-2-(2,4-dichlorophenyl)-2-(1 H -1,2,4-triazol-1-ylmethyl)-1,3-dioxolan-4-yl]methoxy]phenyl]-1-piperazinyl]phenyl]-Δ 2 -1,2,4-triazolin-5-one
or
(±)-1-[( RS )- sec -butyl]-4-[ p -[4-[ p -[[(2 R ,4 S )-2-(2,4-dichlorophenyl)-2-(1 H -1,2,4-triazol-1-ylmethyl)-1,3-dioxolan-4-yl]methoxy]phenyl]-1-piperazinyl]phenyl]-Δ 2 -1,2,4-triazolin-5-one
Itraconazole has a molecular formula of C 35 H 38 Cl 2 N 8 O 4 and a molecular weight of 705.64. It is a white to slightly yellowish powder. It is insoluble in water, very slightly soluble in alcohols, and freely soluble in dichloromethane. It has a pKa of 3.70 (based on extrapolation of values obtained from methanolic solutions) and a log (n-octanol/water) partition coefficient of 5.66 at pH 8.1.
Itraconazole Capsules contain 100 mg of itraconazole coated on sugar spheres (composed of sucrose, maize starch, and purified water). Inactive ingredients are hard gelatin capsule, hypromellose, polyethylene glycol (PEG) 20,000, titanium dioxide, FD&C Blue No. 1, FD&C Blue No. 2, D&C Red No. 22 and D&C Red No. 28.
Meets USP Dissolution Test 2.
CLINICAL PHARMACOLOGY
Pharmacokinetics and Metabolism
General Pharmacokinetic Characteristics
Peak plasma concentrations of itraconazole are reached within 2 to 5 hours following oral administration. As a consequence of non-linear pharmacokinetics, itraconazole accumulates in plasma during multiple dosing. Steady-state concentrations are generally reached within about 15 days, with C max values of 0.5 μg/mL, 1.1 μg/mL and 2.0 μg/mL after oral administration of 100 mg once daily, 200 mg once daily and 200 mg b.i.d., respectively. The terminal half-life of itraconazole generally ranges from 16 to 28 hours after single dose and increases to 34 to 42 hours with repeated dosing. Once treatment is stopped, itraconazole plasma concentrations decrease to an almost undetectable concentration within 7 to 14 days, depending on the dose and duration of treatment. Itraconazole mean total plasma clearance following intravenous administration is 278 mL/min. Itraconazole clearance decreases at higher doses due to saturable hepatic metabolism.
Absorption
Itraconazole is rapidly absorbed after oral administration. Peak plasma concentrations of itraconazole are reached within 2 to 5 hours following an oral capsule dose. The observed absolute oral bioavailability of itraconazole is about 55%.
The oral bioavailability of itraconazole is maximal when Itraconazole Capsules are taken immediately after a full meal.
Absorption of itraconazole capsules is reduced in subjects with reduced gastric acidity, such as subjects taking medications known as gastric acid secretion suppressors (e.g., H 2 -receptor antagonists, proton pump inhibitors) or subjects with achlorhydria caused by certain diseases. (See PRECAUTIONS: Drug Interactions .) Absorption of itraconazole under fasted conditions in these subjects is increased when Itraconazole Capsules are administered with an acidic beverage (such as a non-diet cola). When Itraconazole Capsules were administered as a single 200-mg dose under fasted conditions with non-diet cola after ranitidine pretreatment, a H 2 -receptor antagonist, itraconazole absorption was comparable to that observed when Itraconazole Capsules were administered alone. (See PRECAUTIONS: Drug Interactions .)
Itraconazole exposure is lower with the Capsule formulation than with the Oral Solution when the same dose of drug is given. (See WARNINGS .)
Distribution
Most of the itraconazole in plasma is bound to protein (99.8%), with albumin being the main binding component (99.6% for the hydroxy-metabolite). It has also a marked affinity for lipids. Only 0.2% of the itraconazole in plasma is present as free drug. Itraconazole is distributed in a large apparent volume in the body (>700 L), suggesting extensive distribution into tissues. Concentrations in lung, kidney, liver, bone, stomach, spleen and muscle were found to be two to three times higher than corresponding concentrations in plasma, and the uptake into keratinous tissues, skin in particular, up to four times higher. Concentrations in the cerebrospinal fluid are much lower than in plasma.
Metabolism
Itraconazole is extensively metabolized by the liver into a large number of metabolites. In vitro studies have shown that CYP3A4 is the major enzyme involved in the metabolism of itraconazole. The main metabolite is hydroxy-itraconazole, which has in vitro antifungal activity comparable to itraconazole; trough plasma concentrations of this metabolite are about twice those of itraconazole.
Excretion
Itraconazole is excreted mainly as inactive metabolites in urine (35%) and in feces (54%) within one week of an oral solution dose. Renal excretion of itraconazole and the active metabolite hydroxy-itraconazole account for less than 1% of an intravenous dose. Based on an oral radiolabeled dose, fecal excretion of unchanged drug ranges from 3% to 18% of the dose.
As re-distribution of itraconazole from keratinous tissues appears to be negligible, elimination of itraconazole from these tissues is related to epidermal regeneration. Contrary to plasma, the concentration in skin persists for 2 to 4 weeks after discontinuation of a 4-week treatment and in nail keratin – where itraconazole can be detected as early as 1 week after start of treatment – for at least six months after the end of a 3-month treatment period.
Special Populations
Renal Impairment
Limited data are available on the use of oral itraconazole in patients with renal impairment. A pharmacokinetic study using a single 200 mg oral dose of itraconazole was conducted in three groups of patients with renal impairment (uremia: n=7; hemodialysis: n=7; and continuous ambulatory peritoneal dialysis: n=5). In uremic subjects with a mean creatinine clearance of 13 mL/min. × 1.73 m 2 , the exposure, based on AUC, was slightly reduced compared with normal population parameters. This study did not demonstrate any significant effect of hemodialysis or continuous ambulatory peritoneal dialysis on the pharmacokinetics of itraconazole (T max , C max , and AUC 0–8h ). Plasma concentration-versus-time profiles showed wide intersubject variation in all three groups. After a single intravenous dose, the mean terminal half-lives of itraconazole in patients with mild (defined in this study as CrCl 50–79 mL/min), moderate (defined in this study as CrCl 20–49 mL/min), and severe renal impairment (defined in this study as CrCl <20 mL/min) were similar to that in healthy subjects (range of means 42–49 hours vs 48 hours in renally impaired patients and healthy subjects, respectively). Overall exposure to itraconazole, based on AUC, was decreased in patients with moderate and severe renal impairment by approximately 30% and 40%, respectively, as compared with subjects with normal renal function. Data are not available in renally impaired patients during long-term use of itraconazole. Dialysis has no effect on the half-life or clearance of itraconazole or hydroxy-itraconazole. (See PRECAUTIONS and DOSAGE AND ADMINISTRATION .)
Hepatic Impairment
Itraconazole is predominantly metabolized in the liver. A pharmacokinetic study was conducted in 6 healthy and 12 cirrhotic subjects who were administered a single 100 mg dose of itraconazole as capsule. A statistically significant reduction in mean C max (47%) and a twofold increase in the elimination half-life (37±17 hours vs. 16±5 hours) of itraconazole were noted in cirrhotic subjects compared with healthy subjects. However, overall exposure to itraconazole, based on AUC, was similar in cirrhotic patients and in healthy subjects. Data are not available in cirrhotic patients during long-term use of itraconazole. (See CONTRAINDICATIONS , PRECAUTIONS: Drug Interactions and DOSAGE AND ADMINISTRATION .)
Decreased Cardiac Contractility
When itraconazole was administered intravenously to anesthetized dogs, a dose-related negative inotropic effect was documented. In a healthy volunteer study of itraconazole intravenous infusion, transient, asymptomatic decreases in left ventricular ejection fraction were observed using gated SPECT imaging; these resolved before the next infusion, 12 hours later. If signs or symptoms of congestive heart failure appear during administration of Itraconazole Capsules, itraconazole should be discontinued. (See BOXED WARNING , CONTRAINDICATIONS , WARNINGS , PRECAUTIONS: Drug Interactions and ADVERSE REACTIONS: Postmarketing Experience for more information.)
MICROBIOLOGY
Mechanism of Action
In vitro studies have demonstrated that itraconazole inhibits the cytochrome P450-dependent synthesis of ergosterol, which is a vital component of fungal cell membranes.
Antimicrobial Activity
Itraconazole exhibits in vitro activity against Blastomyces dermatitidis, Histoplasma capsulatum, Histoplasma duboisii, Aspergillus flavus, Aspergillus fumigatus, and Trichophyton species (See INDICATIONS AND USAGE: Description of Clinical Studies ).
Susceptibility Testing Methods
For specific information regarding susceptibility test interpretive criteria and associated test methods and quality control standards recognized by FDA for this drug, please see: https://www.fda.gov/STIC.
Resistance
Isolates from several fungal species with decreased susceptibility to itraconazole have been isolated in vitro and from patients receiving prolonged therapy.
Itraconazole is not active against Zygomycetes (e.g., Rhizopus spp., Rhizomucor spp., Mucor spp. and Absidia spp.), Fusarium spp., Scedosporium spp. and Scopulariopsis spp.
Cross-Resistance
Several in vitro studies have reported that some fungal clinical isolates with reduced susceptibility to one azole antifungal agent may also be less susceptible to other azole derivatives. The finding of cross-resistance is dependent on a number of factors, including the species evaluated, its clinical history, the particular azole compounds compared, and the type of susceptibility test that is performed.
Studies (both in vitro and in vivo ) suggest that the activity of amphotericin B may be suppressed by prior azole antifungal therapy. As with other azoles, itraconazole inhibits the 14 C-demethylation step in the synthesis of ergosterol, a cell wall component of fungi. Ergosterol is the active site for amphotericin B. In one study the antifungal activity of amphotericin B against Aspergillus fumigatus infections in mice was inhibited by ketoconazole therapy. The clinical significance of test results obtained in this study is unknown.
Description of Clinical Studies
Blastomycosis
Analyses were conducted on data from two open-label, non-concurrently controlled studies (N=73 combined) in patients with normal or abnormal immune status. The median dose was 200 mg/day. A response for most signs and symptoms was observed within the first 2 weeks, and all signs and symptoms cleared between 3 and 6 months. Results of these two studies demonstrated substantial evidence of the effectiveness of itraconazole for the treatment of blastomycosis compared with the natural history of untreated cases.
Histoplasmosis
Analyses were conducted on data from two open-label, non-concurrently controlled studies (N=34 combined) in patients with normal or abnormal immune status (not including HIV-infected patients). The median dose was 200 mg/day. A response for most signs and symptoms was observed within the first 2 weeks, and all signs and symptoms cleared between 3 and 12 months. Results of these two studies demonstrated substantial evidence of the effectiveness of itraconazole for the treatment of histoplasmosis, compared with the natural history of untreated cases.
Histoplasmosis in HIV-infected patients
Data from a small number of HIV-infected patients suggested that the response rate of histoplasmosis in HIV-infected patients is similar to that of non-HIV-infected patients. The clinical course of histoplasmosis in HIV-infected patients is more severe and usually requires maintenance therapy to prevent relapse.
Aspergillosis
Analyses were conducted on data from an open-label, "single-patient-use" protocol designed to make itraconazole available in the U.S. for patients who either failed or were intolerant of amphotericin B therapy (N=190). The findings were corroborated by two smaller open-label studies (N=31 combined) in the same patient population. Most adult patients were treated with a daily dose of 200 to 400 mg, with a median duration of 3 months. Results of these studies demonstrated substantial evidence of effectiveness of itraconazole as a second-line therapy for the treatment of aspergillosis compared with the natural history of the disease in patients who either failed or were intolerant of amphotericin B therapy.
Onychomycosis of the toenail
Analyses were conducted on data from three double-blind, placebo-controlled studies (N=214 total; 110 given Itraconazole Capsules) in which patients with onychomycosis of the toenails received 200 mg of Itraconazole Capsules once daily for 12 consecutive weeks. Results of these studies demonstrated mycologic cure, defined as simultaneous occurrence of negative KOH plus negative culture, in 54% of patients. Thirty-five percent (35%) of patients were considered an overall success (mycologic cure plus clear or minimal nail involvement with significantly decreased signs) and 14% of patients demonstrated mycologic cure plus clinical cure (clearance of all signs, with or without residual nail deformity). The mean time to overall success was approximately 10 months. Twenty-one percent (21%) of the overall success group had a relapse (worsening of the global score or conversion of KOH or culture from negative to positive).
Onychomycosis of the fingernail
Analyses were conducted on data from a double-blind, placebo-controlled study (N=73 total; 37 given Itraconazole Capsules) in which patients with onychomycosis of the fingernails received a 1-week course (pulse) of 200 mg of Itraconazole Capsules b.i.d., followed by a 3-week period without Itraconazole Capsules, which was followed by a second 1-week pulse of 200 mg of Itraconazole Capsules b.i.d. Results demonstrated mycologic cure in 61% of patients. Fifty-six percent (56%) of patients were considered an overall success and 47% of patients demonstrated mycologic cure plus clinical cure. The mean time to overall success was approximately 5 months. None of the patients who achieved overall success relapsed.
HOW SUPPLIED
Itraconazole Capsules are available containing 100 mg of itraconazole, with a blue opaque cap and pink transparent body, imprinted with "PP 100." The capsules are supplied in bottles of 30 capsules (NDC 10147-1700-3).
Store at controlled room temperature 15°–25°C (59°–77°F). Protect from light and moisture.
Mechanism of Action
In vitro studies have demonstrated that itraconazole inhibits the cytochrome P450-dependent synthesis of ergosterol, which is a vital component of fungal cell membranes.
Itraconazole - Itraconazole capsule PubMed™ news
- Journal Article • 2026 MayAssessing the Potential Clinical Drug-Drug Interactions Between D-1553 (Garsorasib) and CYP450 Enzymes/Transporters via a Cocktail Approach.
- Journal Article • 2026 MayEvaluation of Sensititre YeastOne for antifungal susceptibility testing of Candida (Candidozyma) auris: misclassification of FKS1 mutants and overestimation of caspofungin resistance in a global collection of isolates.
- Journal Article • 2026 MayNiemann-Pick C1 maintains cholesterol homeostasis in late endosomes to drive hepatitis B virus endosomal escape.
- Journal Article • 2026 MayResponse to Letter to the Editor Regarding "The Effect of Itraconazole on the Pharmacokinetics of Vepdegestrant, a PROteolysis TArgeting Chimera Estrogen Receptor Degrader, in Healthy Adult Participants".
- Journal Article • 2026 MayPharmacokinetic drug-drug interaction between the COVID-19 3CL protease inhibitor GST-HG171 and itraconazole in healthy subjects.