Lidocan prescribing information
INDICATIONS AND USAGE
LIDOCAN™ is indicated for relief of pain associated with post-herpetic neuralgia. It should be applied only to intact skin.
DOSAGE AND ADMINISTRATION
Apply LIDOCAN™ to intact skin to cover the most painful area. Apply the prescribed number of patches (maximum of 3), only once for up to 12 hours within a 24-hour period. Patches may be cut into smaller sizes with scissors prior to removal of the release liner (see HANDLING AND DISPOSAL). Clothing may be worn over the area of application. Smaller areas of treatment are recommended in a debilitated patient, or a patient with impaired elimination.
If irritation or a burning sensation occurs during application, remove the patch(es) and do not reapply until the irritation subsides.
When LIDOCAN™ is used concomitantly with other products containing local anesthetic agents, the amount absorbed from all formulations must be considered.
LIDOCAN™ may not stick if it gets wet. Avoid contact with water, such as bathing, swimming, or showering.
CONTRAINDICATIONS
LIDOCAN™ is contraindicated in patients with a known history of sensitivity to local anesthetics of the amide type, or to any other component of the product.
ADVERSE REACTIONS
Application Site Reactions
During or immediately after treatment with LIDOCAN™ , the skin at the site of application may develop blisters, bruising, burning sensation, depigmentation, dermatitis, discoloration, edema, erythema, exfoliation, irritation, papules, petechia, pruritus, vesicles, or may be the locus of abnormal sensation. These reactions are generally mild and transient, resolving spontaneously within a few minutes to hours.
Allergic Reactions
Allergic and anaphylactoid reactions associated with lidocaine, although rare, can occur. They are characterized by angioedema, bronchospasm, dermatitis, dyspnea, hypersensitivity, laryngospasm, pruritus, shock, and urticaria. If they occur, they should be managed by conventional means. The detection of sensitivity by skin testing is of doubtful value.
Other Adverse Events
Due to the nature and limitation of spontaneous reports in postmarketing surveillance, causality has not been established for additional reported adverse events including:
Asthenia, confusion, disorientation, dizziness, headache, hyperesthesia, hypoesthesia, lightheadedness, metallic taste, nausea, nervousness, pain exacerbated, paresthesia, somnolence, taste alteration, vomiting, visual disturbances such as blurred vision, flushing, tinnitus, and tremor.
Systemic (Dose-Related) Reactions
Systemic adverse reactions following appropriate use of LIDOCAN™ are unlikely, due to the small dose absorbed (see CLINICAL PHARMACOLOGY, Pharmacokinetics). Systemic adverse effects of lidocaine are similar in nature to those observed with other amide local anesthetic agents, including CNS excitation and/or depression (lightheadedness, nervousness, apprehension, euphoria, confusion, dizziness, drowsiness, tinnitus, blurred or double vision, vomiting, sensations of heat, cold, or numbness, twitching, tremors, convulsions, unconsciousness, respiratory depression and arrest). Excitatory CNS reactions may be brief or not occur at all, in which case the first manifestation may be drowsiness merging into unconsciousness. Cardiovascular manifestations may include bradycardia, hypotension, and cardiovascular collapse leading to arrest.
Drug Interactions
Antiarrhythmic Drugs
LIDOCAN™ should be used with caution in patients receiving Class I antiarrhythmic drugs (such as tocainide and mexiletine) since the toxic effects are additive and potentially synergistic.
Local Anesthetics When LIDOCAN™ is used concomitantly with other products containing local anesthetic agents, the amount absorbed from all formulations must be considered.
Drugs That May Cause Methemoglobinemia When Used with LIDOCAN™
Patients who are administered local anesthetics are at increased risk of developing methemoglobinemia when concurrently exposed to the following drugs, which could include other local anesthetics:
Examples of Drugs Associated with Methemoglobinemia:
| Class | Example |
| Nitrates/Nitrites | nitric oxide, nitroglycerin, nitroprusside, nitrous oxide |
| Local anesthetics | articaine, benzocaine, bupivacaine, lidocaine, mepivacaine, prilocaine, procaine, ropivacaine, tetracaine |
| Antineoplastic agents | cyclophosphamide, flutamide, hydroxyurea, ifosfamide, rasburicase |
| Antibiotics | dapsone, nitrofurantoin, para-aminosalicylic acid, sulfonamides |
| Antimalarials | chloroquine, primaquine |
| Anticonvulsants | Phenobarbital, phenytoin, sodium valproate |
| Other drugs | acetaminophen, metoclopramide, quinine, sulfasalazine |
DESCRIPTION
LIDOCAN™ is comprised of an adhesive material containing 5% lidocaine, which is applied to a non-woven polyester felt backing and covered with a polyethylene terephthalate (PET) film release liner. The release liner is removed prior to application to the skin. The size of the patch is 10 cm x 14 cm. Lidocaine is chemically designated as acetamide, 2-(diethylamino)-N-(2,6-dimethylphenyl), has an octanol:water partition ratio of 43 at pH 7.4, and has the following structure:
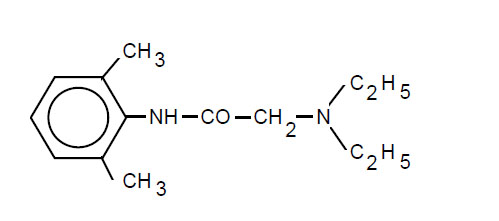
Each adhesive patch contains 700 mg of lidocaine (50 mg per gram adhesive) in an aqueous base. It also contains the following inactive ingredients: purified water, glycerin, sorbitol, polyacrylic acid, sodium carboxymethylcellulose, sodium polyacrylate, propylene glycol, urea, kaolin, tartaric acid, gelatin, polyvinyl alcohol, dihydroxyaluminum aminoacetate, edetate disodium, methylparaben, and propylparaben.
CLINICAL PHARMACOLOGY
Pharmacodynamics
Lidocaine is an amide-type local anesthetic agent and is suggested to stabilize neuronal membranes by inhibiting the ionic fluxes required for the initiation and conduction of impulses.
The penetration of lidocaine into intact skin after application of a lidocaine patch 5% is sufficient to produce an analgesic effect, but less than the amount necessary to produce a complete sensory block.
Pharmacokinetics
Absorption The amount of lidocaine systemically absorbed from lidocaine patch 5% is directly related to both the duration of application and the surface area over which it is applied. In a pharmacokinetic study, three lidocaine patches were applied over an area of 420 cm 2 of intact skin on the back of normal volunteers for 12 hours. Blood samples were withdrawn for determination of lidocaine concentration during the application and for 12 hours after removal of patches. The results are summarized in Table 1.
Table 1
Absorption of lidocaine from Lidocaine Patch 5%
| Lidocaine Patch 5% | Application Site | Area (cm 2 ) | Dose Absorbed (mg) | C max (mcg/mL) | T max (hr) |
| 3 patches (2100 mg) | Back | 420 | 64 ± 32 | 0.13 ± 0.06 | 11 hr |
When LIDOCAN™ is used according to the recommended dosing instructions, only 3 ± 2% of the dose applied is expected to be absorbed. At least 95% (665 mg) of lidocaine will remain in a used patch. Mean peak blood concentration of lidocaine is about 0.13 mcg/mL (about 1/10 of the therapeutic concentration required to treat cardiac arrhythmias). Repeated application of three patches simultaneously for 12 hours (recommended maximum daily dose), once per day for three days, indicated that the lidocaine concentration does not increase with daily use. The mean plasma pharmacokinetic profile for the 15 healthy volunteers is shown in Figure 1.
Figure 1
Mean lidocaine blood concentrations after three consecutive daily applications of three lidocaine patches simultaneously for 12 hours per day in healthy volunteers (n = 15).
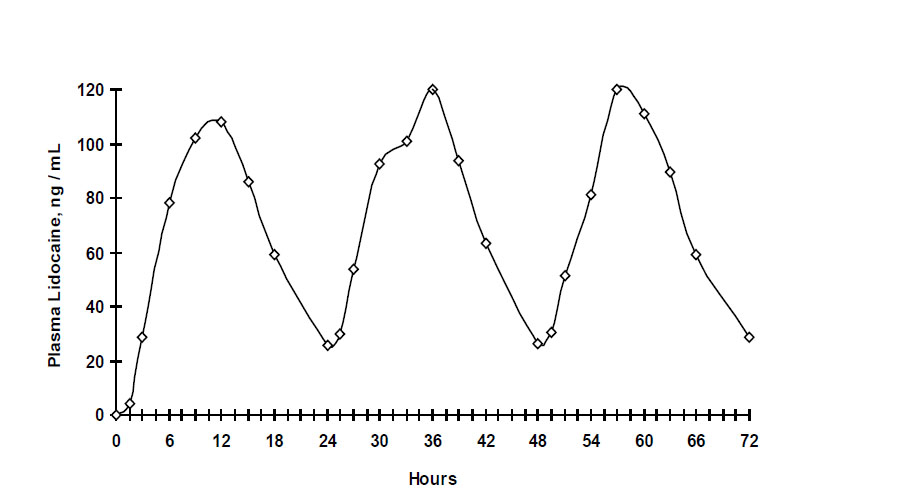
Distribution When lidocaine is administered intravenously to healthy volunteers, the volume of distribution is 0.7 to 2.7 L/kg (mean 1.5 ± 0.6 SD, n = 15). At concentrations produced by application of lidocaine patch 5%, lidocaine is approximately 70% bound to plasma proteins, primarily alpha-1-acid glycoprotein. At much higher plasma concentrations (1 to 4 mcg/mL of free base), the plasma protein binding of lidocaine is concentration dependent. Lidocaine crosses the placental and blood brain barriers, presumably by passive diffusion.
Metabolism It is not known if lidocaine is metabolized in the skin. Lidocaine is metabolized rapidly by the liver to a number of metabolites, including monoethylglycinexylidide (MEGX) and glycinexylidide (GX), both of which have pharmacologic activity similar to, but less potent than that of lidocaine. A minor metabolite, 2,6-xylidine, has unknown pharmacologic activity but is carcinogenic in rats. The blood concentration of this metabolite is negligible following application of lidocaine patch 5%. Following intravenous administration, MEGX and GX concentrations in serum range from 11 to 36% and from 5 to 11% of lidocaine concentrations, respectively.
Excretion Lidocaine and its metabolites are excreted by the kidneys. Less than 10% of lidocaine is excreted unchanged. The half-life of lidocaine elimination from the plasma following IV administration is 81 to 149 minutes (mean 107 ± 22 SD, n = 15). The systemic clearance is 0.33 to 0.90 L/min (mean 0.64 ± 0.18 SD, n = 15).
CLINICAL STUDIES
Single-dose treatment with lidocaine patch 5% was compared to treatment with vehicle patch (without lidocaine), and to no treatment (observation only) in a double-blind, crossover clinical trial with 35 post-herpetic neuralgia patients. Pain intensity and pain relief scores were evaluated periodically for 12 hours. Lidocaine patch 5% performed statistically better than vehicle patch in terms of pain intensity from 4 to 12 hours.
Multiple-dose, two-week treatment with lidocaine patch 5%, was compared to vehicle patch (without lidocaine) in a double-blind, crossover clinical trial of withdrawal-type design conducted in 32 patients, who were considered as responders to the open-label use of lidocaine patch 5% prior to the study. The constant type of pain was evaluated but not the pain induced by sensory stimuli (dysesthesia). Statistically significant differences favoring lidocaine patch 5% were observed in terms of time to exit from the trial (14 versus 3.8 days at p-value <0.001), daily average pain relief, and patient's preference of treatment. About half of the patients also took oral medication commonly used in the treatment of post-herpetic neuralgia. The extent of use of concomitant medication was similar in the two treatment groups.
HOW SUPPLIED
LIDOCAN™ is available as the following:
Carton of 30 patches....................................................................................NDC 5 9088-905-54
(packaged into individual child-resistant envelope)
Carton of 15 patches....................................................................................NDC 59088-905-82
(packaged into individual child-resistant envelope)
Single patch............................................................................................. NDC 59088-905-84
(packaged into individual child-resistant envelope)
Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature].
KEEP THIS AND All MEDICATIONS OUT OF THE REACH OF CHILDREN. Call your doctor about side effects. To report side effects, call PureTek Corporation at 1-877-921-7873 .
Distributed by: PureTek Corporation Panorama City, CA 91402 For questions or information call toll-free: 877-921-7873