Get your patient on Loperamide Hydrochloride - Loperamide Hydrochloride capsule (Loperamide Hydrochloride)
Loperamide Hydrochloride - Loperamide Hydrochloride capsule prescribing information
BOXED WARNING
WARNING: TORSADES DE POINTES AND SUDDEN DEATH
- Cases of Torsades de Pointes, cardiac arrest, and death have been reported with the use of a higher than recommended dosages of Loperamide Hydrochloride Capsules (see WARNINGS and OVERDOSAGE).
- Loperamide Hydrochloride Capsules is contraindicated in pediatric patients less than 2 years of age (see CONTRAINDICATIONS).
- Avoid Loperamide Hydrochloride Capsules dosages higher than recommended in adults and pediatric patients 2 years of age and older due to the risk of serious cardiac adverse reactions (see DOSAGE AND ADMINISTRATION).
INDICATIONS & USAGE
Loperamide Hydrochloride Capsules (loperamide hydrochloride) is indicated for the control and symptomatic relief of acute nonspecific diarrhea in patients 2 years of age and older and of chronic diarrhea in adults associated with inflammatory bowel disease. Loperamide Hydrochloride Capsules is also indicated for reducing the volume of discharge from ileostomies.
DOSAGE & ADMINISTRATION
Loperamide Hydrochloride Capsules is contraindicated in pediatric patients less than 2 years of age due to the risks of respiratory depression and serious cardiac adverse reactions (see CONTRAINDICATIONS ).
Avoid Loperamide Hydrochloride Capsules dosages higher than recommended in adult or pediatric patients 2 years of age and older due to the risk of serious cardiac adverse reactions (See WARNINGS, OVERDOSAGE ).
(1 capsule = 2 mg)
Patients should receive appropriate fluid and electrolyte replacement as needed.
Acute Diarrhea
Adults and Pediatric Patients 13 Years and Older: The recommended initial dose is 4mg (two capsules) followed by 2 mg (one capsule) after each unformed stool. The maximum daily dose is 16mg (eight capsules). Clinical improvement is usually observed within 48 hours.
Pediatric Patients 2 to 12 Years of Age : In pediatric patients 2 to 5 years of age (20 kg or less), the non-prescription liquid formulation of loperamide (1 mg/5 mL) should be used; for ages 6-12, either loperamide hydrochloride capsules or the non-prescription liquid formulation of loperamide may be used. For pediatric patients 2 to 12 years of age, the following schedule for capsules or liquid will usually fulfill initial dosage requirements:
Recommended First Day Dosage Schedule
Two to five years (13 to 20 kg): 1 mg three times daily (3 mg total daily dosage) Six to eight years (20 to 30 kg): 2 mg twice daily. (4 mg total daily dosage)
Eight to twelve years (greater than 30kg): 2 mg three times daily (6 mg total daily dosage)
Recommended Subsequent Daily Dosage
Following the first treatment day, it is recommended that subsequent Loperamide Hydrochloride Capsules doses (1 mg/10 kg body weight) be administered only after a loose stool. The total daily dosage should not exceed recommended dosages for the first day.
Chronic Diarrhea
Adults
'The recommended initial dose is 4 mg (two capsules) followed by 2 mg (one capsule) after each unformed stool until diarrhea is controlled, after which the dosage of Loperamide Hydrochloride Capsules should be reduced to meet individual requirements. When the optimal daily dosage has been established, this amount may then be administered as a single dose or in divided doses. The average daily maintenance dosage in clinical trials was 4 to 8 mg (two to four capsules per day). The maximum daily dosage is 16 mg (eight capsules per day). If clinical improvement is not observed after treatment with 16 mg per day for at least 10 days, symptoms are unlikely to be controlled by further administration. Loperamide Hydrochloride Capsules administration may be continued if diarrhea cannot be adequately controlled with diet or specific treatment.
Elderly
No formal pharmacokinetic studies were conducted in elderly subjects. However, there were no major differences reported in the drug disposition in elderly patients with diarrhea relative to young patients. No dose adjustment is required for the elderly.
In general, elderly patients may be more susceptible to drug-associated effects of the QT interval. Avoid Loperamide Hydrochloride Capsules in elderly patients taking drugs that can result in prolongation of the QT interval (for example, Class IA or III antiarrhythmics) or in patients with risk factors for Torsades de Pointes (see WARNINGS ).
Renal Impairment
No pharmacokinetic data are available in patients with renal impairment. Since the metabolites and the unchanged drug are mainly excreted in the feces, no dosage adjustment is required for patients with renal impairment (see PRECAUTIONS ).
Hepatic Impairment
The pharmacokinetics of loperamide have not been studied in patients with hepatic impairment.
Use Loperamide Hydrochloride Capsules with caution in such patients because the systemic exposure may be increased due to reduced metabolism (see PRECAUTIONS ).
CONTRAINDICATIONS
Loperamide Hydrochloride Capsules is contraindicated in:
- pediatric patients less than 2 years of age due to the risks of respiratory depression and serious cardiac adverse reactions (see WARNINGS ).
- patients with a known hypersensitivity to loperamide hydrochloride or to any of the excipients.
- patients with abdominal pain in the absence of diarrhea.
- patients with acute dysentery, which is characterized by blood in stools and high fever.
- patients with acute ulcerative colitis.
- patients with bacterial enterocolitis caused by invasive organisms including Salmonella , Shigella , and Campylobacter .
- patients with pseudomembranous colitis (e.g., Clostridium difficle ) associated with the use of broad-spectrum antibiotics.
ADVERSE REACTIONS
Clinical Trial Experience
The adverse effects reported during clinical investigations of Loperamide Hydrochloride Capsules (loperamide hydrochloride) are difficult to distinguish from symptoms associated with the diarrheal syndrome. Adverse experiences recorded during clinical studies with Loperamide Hydrochloride Capsules were generally of a minor and self-limiting nature. They were more commonly observed during the treatment of chronic diarrhea.
The adverse events reported are summarized irrespective of the causality assessment of the investigators.
1) Adverse events from 4 placebo-controlled studies in patients with acute diarrhea The adverse events with an incidence of 1.0% or greater, which were reported at least as often in patients on loperamide hydrochloride as on placebo, are presented in the table below.
| Acute Diarrhea | ||
| Loperamide Hydrochloride | Placebo | |
| No. of treated patients | 231 | 236 |
| Gastrointestinal AE% Constipation | 2.6% | 0.8% |
The adverse events with an incidence of 1.0% or greater, which were more frequently reported in patients on placebo than on loperamide hydrochloride, were: dry mouth, flatulence, abdominal cramp and colic.
2) Adverse events from 20 placebo-controlled studies in patients with chronic diarrhea The adverse events with an incidence of 1.0% or greater, which were reported at least as often in patients on loperamide hydrochloride as on placebo, are presented below in the table below.
| Chronic Diarrhea | ||
| Loperamide Hydrochloride | Placebo | |
| No. of treated patients | 285 | 277 |
| Gastrointestinal AE% Constipation | 5.3% | 0.0% |
| Central and peripheral nervous system AE% Dizziness | 1.4% | 0.7% |
The adverse events with an incidence of 1.0% or greater, which were more frequently reported in patients on placebo than on loperamide hydrochloride were: nausea, vomiting, headache, meteorism, abdominal pain, abdominal cramp and colic.
3) Adverse events from seventy-six controlled and uncontrolled studies in patients with acute or chronic diarrhea The adverse events with an incidence of 1.0% or greater in patients from all studies are given in the table below.
| Acute Diarrhea | Chronic Diarrhea | All Studies a | |
| No. of treated patients | 1913 | 1371 | 3740 |
| Gastrointestinal AE% Nausea Constipation Abdominal cramps | 0.7% 1.6% 0.5% | 3.2% 1.9% 3.0% | 1.8% 1.7% 1.4% |
a. All patients in all studies, including those in which it was not specified if the adverse events occurred in patients with acute or chronic diarrhea.
Postmarketing Experience
The following adverse events have been reported:
Cardiac disorders
QT/QTc interval prolongation, Torsades de Pointes, other ventricular arrhythmias, cardiac arrest, syncope, and death (see WARNINGS, OVERDOSAGE ).
Skin and subcutaneous tissue disorders
Rash, pruritus, urticaria, and angioedema and extremely rare cases bullous eruption including erythema multiforme, Stevens-Johnson syndrome and Toxic Epidermal Necrolysis have been reported with use of Loperamide Hydrochloride Capsules.
Immune system disorders
Isolated occurrences of allergic reactions and in some cases severe hypersensitivity reactions including anaphylactic shock and anaphylactoid reactions have been reported with the use of Loperamide Hydrochloride Capsules.
Gastrointestinal disorders
Dry mouth, abdominal pain, distention or discomfort, nausea, vomiting, flatulence, dyspepsia, constipation, paralytic ileus, megacolon; including toxic megacolon (see CONTRAINDICATIONS, WARNINGS ).
Renal and urinary disorders
Urinary retention
Nervous system disorders
Drowsiness, dizziness
General disorders and administrative site conditions
Tiredness
A number of the adverse events reported during the clinical investigations and post-marketing experience with loperamide are frequent symptoms of the underlying diarrheal syndrome (abdominal pain/discomfort, nausea, vomiting, dry mouth, tiredness, drowsiness, dizziness, constipation, and flatulence). These symptoms are often difficult to distinguish from undesirable drug effects.
DRUG INTERACTIONS
Effects of Other Drugs on Loperamide
Concomitant use of Loperamide Hydrochloride Capsules with inhibitors of CYP3A4 (e.g., itraconazole) or CYP2C8 (e.g., gemfibrozil) or inhibitors of P-glycoprotein (e.g., quinidine, ritonavir) can increase exposure to loperamide. The increased systemic exposure to loperamide may increase a risk for cardiac adverse reactions especially in patients who are taking multiple CYP enzyme inhibitors, or in patients with underlying cardiac conditions (see WARNINGS ). Monitor patients for cardiac adverse reactions.
CYP3A4 Inhibitors
Itraconazole
Concomitant administration of multiple doses of 100 mg itraconazole twice daily, an inhibitor of both CYP3A4 and P-glycoprotein, with a single 4-mg dose of loperamide hydrochloride increased the peak plasma concentration and the systemic exposure to loperamide by 2.9-fold and 3.8-fold, respectively.
CYP2C8 Inhibitors
Gemfibrozil
When a single 4-mg dose of loperamide hydrochloride was co-administered with 600 mg gemfibrozil, a strong inhibitor of CYP2C8, on day 3 of a 5-day treatment with gemfibrozil twice daily, the mean peak plasma concentration and the systemic exposure to loperamide was increased by 1.6-fold and 2.2-fold, respectively.
CYP3A4 and CYP2C8 Inhibitors
When multiple doses of both 100 mg itraconazole and 600 mg gemfibrozil twice daily were administered with a single 4-mg dose of loperamide hydrochloride, the mean peak plasma concentration and the systemic exposure to loperamide was increased by 4.2-fold and 12.6-fold, respectively.
P-glycoprotein Inhibitors
Concomitant administration of a 16 mg single dose of loperamide hydrochloride with a 600 mg single dose of quinidine or ritonavir, both of which are P-glycoprotein inhibitors, resulted in a 2- to 3-fold increase in loperamide plasma concentrations. Due to the potential for enhanced CNS adverse reactions when loperamide is co-administered with quinidine and with ritonavir, caution should be exercised when Loperamide Hydrochloride Capsules USP, 2 mg is administered at the recommended dosages (2 mg, up to 16 mg maximum daily dose) with P-glycoprotein inhibitors.
Effects of Loperamide on Other Drugs
Saquinavir
When a single 16-mg dose of loperamide hydrochloride is coadministered with a 600 mg single dose of saquinavir, loperamide decreased saquinavir exposure by 54%, which may be of clinical relevance due to reduction of therapeutic efficacy of saquinavir. The effect of saquinavir on loperamide is of less clinical significance. Therefore, when Loperamide Hydrochloride Capsules is given with saquinavir, the therapeutic efficacy of saquinavir should be closely monitored.
DESCRIPTION
Loperamide Hydrochloride Capsules USP (loperamide hydrochloride), 4-(p-chlorophenyl)-4-hydroxy-N,N-dimethyl- a,a- diphenyl-1-piperidinebutyramide monohydrochloride, is a synthetic antidiarrheal for oral use.
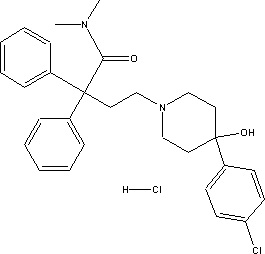
Loperamide Hydrochloride Capsules USP is available in 2mg capsules.
The inactive ingredients are: Magnesium stearate, microcrystalline cellulose, sodium starch glycolate, lactose monohydrate, colloidal silicon dioxide. In addition, the hard gelatin capsule also contains gelatin, black iron oxide, red iron oxide, titanium dioxide and yellow iron oxide. The black printing ink contains black iron oxide, propylene glycol, shellac, and potassium hydroxide.
CLINICAL PHARMACOLOGY
Mechanism of Action
In vitro and animal studies show that Loperamide Hydrochloride Capsules (loperamide hydrochloride) acts by slowing intestinal motility and by affecting water and electrolyte movement through the bowel.
Loperamide binds to the opiate receptor in the gut wall. Consequently, it inhibits the release of acetylcholine and prostaglandins, thereby reducing propulsive peristalsis, and increasing intestinal transit time. Loperamide increases the tone of the anal sphincter, thereby reducing incontinence and urgency.
Pharmacodynamics
Loperamide prolongs the transit time of the intestinal contents. It reduces daily fecal volume, increases the viscosity and bulk density, and diminishes the loss of fluid and electrolytes.
Tolerance to the antidiarrheal effect has not been observed.
Pharmacokinetics
Absorption
Plasma concentrations of unchanged drug remain below 2 ng/mL after the intake of a 2 mg capsule of Loperamide Hydrochloride Capsules. Plasma loperamide concentrations are highest approximately 5 hours after administration of the capsule and 2.5 hours after the liquid. The peak plasma concentrations of loperamide were similar for both formulations.
Distribution
Based on literature information, the plasma protein binding of loperamide is about 95%. Loperamide is a P-glycoprotein substrate.
Elimination
The apparent elimination half-life of loperamide is 10.8 hours with a range of 9.1 to 14.4 hours. Elimination of loperamide mainly occurs by oxidative N-demethylation.
Metabolism
In vitro loperamide is metabolized mainly by cytochrome P450 (CYP450) isozymes, CYP2C8 and CYP3A4, to form- N-demethyl loperamide. In an in vitro study quercetin (CYP2C8 inhibitor) and ketoconazole (CYP3A4 inhibitor) significantly inhibited the N-demethylation process by 40% and 90%, respectively. In addition, CYP2B6 and CYP2D6 appear to play a minor role in loperamide N-demethylation.
Concomitant use of Loperamide Hydrochloride Capsules with inhibitors of CYP3A4 (e.g., itraconazole) or CYP2C8 (e.g., gemfibrozil) or inhibitors of P-glycoprotein (e.g., quinidine, ritonavir) can increase exposure to loperamide (see PRECAUTIONS, Drug Interactions ).
Excretion
Excretion of the unchanged loperamide and its metabolites mainly occurs through the feces.
HOW SUPPLIED
Capsules - each capsule contains 2 mg of loperamide hydrochloride. The capsules have a light brown opaque cap and a light brown opaque body with an “^" over “605” imprinted radially on one segment.
NDC 42799-605-03
(30 CAPSULES)
NDC 42799-605-01
(100 CAPSULES)
NDC 42799-605-02
(500 CAPSULES)
Store at 20° to 25°C (68° to 77°F) [See USP Controlled Room Temperature].
Revised October 2021
Edenbridge Pharmaceuticals, LLC
Parsippany, NJ 07054
877-381-3336
Rx Only
Printed in USA
Loperamide Hydrochloride - Loperamide Hydrochloride capsule PubMed™ news
- Journal Article • 2026 MayAGA Clinical Practice Update on Management of Clostridioides difficile Infection in Inflammatory Bowel Disease: Expert Review.
- Journal Article • 2026 MayAntidiarrheal activity of the 80% methanol extract and solvent fractions of the leaves of Thymus schimperi (Lamiaceae) in mice.
- Journal Article • 2026 MayLactobacillus plantarum RG-034 colonic soluble capsules alleviate functional constipation in rats by promoting short-chain fatty acid generation.
- Journal Article • 2026 MayIntestinal transit time phenotype is not transferred through gut microbiota transplantation.
- Journal Article • 2026 MayStudy on the preparation of postbiotic elements by fermentation of wheat by-products and their role in improving constipation.