Midodrine Hydrochloride - Midodrine Hydrochloride tablet prescribing information
Warning: Because Midodrine hydrochloride can cause marked elevation of supine blood pressure, it should be used in patients whose lives are considerably impaired despite standard clinical care. The indication for use of Midodrine hydrochloride in the treatment of symptomatic orthostatic hypotension is based primarily on a change in a surrogate marker of effectiveness, an increase in systolic blood pressure measured one minute after standing, a surrogate marker considered likely to correspond to a clinical benefit. At present, however, clinical benefits of Midodrine hydrochloride, principally improved ability to carry out activities of daily living, have not been verified.
INDICATIONS AND USAGE
Midodrine Hydrochloride Tablets, USP are indicated for the treatment of symptomatic orthostatic hypotension (OH). Because Midodrine Hydrochloride Tablets, USP can cause marked elevation of supine blood pressure (BP>200 mmHg systolic), it should be used in patients whose lives are considerably impaired despite standard clinical care, including non-pharmacologic treatment (such as support stockings), fluid expansion, and lifestyle alterations. The indication is based on Midodrine Hydrochloride Tablets, USP effect on increases in 1-minute standing systolic blood pressure, a surrogate marker considered likely to correspond to a clinical benefit. At present, however, clinical benefits of Midodrine Hydrochloride Tablets, USP principally improved ability to perform life activities, have not been established. Further clinical trials are underway to verify and describe the clinical benefits of Midodrine Hydrochloride Tablets, USP.
After initiation of treatment, Midodrine Hydrochloride Tablets, USP should be continued only for patients who report significant symptomatic improvement.
DOSAGE AND ADMINISTRATION
The recommended dose of Midodrine Hydrochloride Tablets, USP is 10 mg, 3 times daily.Dosing should take place during the daytime hours when the patient needs to be upright, pursuing the activities of daily living. A suggested dosing schedule of approximately 4-hour intervals is as follows: shortly before, or upon arising in the morning, midday and late afternoon (not later than 6 P.M.). Doses may be given in 3-hour intervals, if required, to control symptoms, but not more frequently. Single doses as high as 20 mg have been given to patients, but severe and persistent systolic supine hypertension occurs at a high rate (about 45%) at this dose. In order to reduce the potential for supine hypertension during sleep, Midodrine Hydrochloride Tablets, USP should not be given after the evening meal or less than 4 hours before bedtime. Total daily doses greater than 30 mg have been tolerated by some patients, but their safety and usefulness have not been studied systematically or established. Because of the risk of supine hypertension, Midodrine Hydrochloride Tablets, USP should be continued only in patients who appear to attain symptomatic improvement during initial treatment.
The supine and standing blood pressure should be monitored regularly, and the administration of Midodrine Hydrochloride Tablets, USP should be stopped if supine blood pressure increases excessively.
Because desglymidodrine is excreted renally, dosing in patients with abnormal renal function should be cautious; although this has not been systematically studied, it is recommended that treatment of these patients be initiated using 2.5-mg doses.
Dosing in children has not been adequately studied.
Blood levels of midodrine and desglymidodrine were similar when comparing levels in patients 65 or older vs. younger than 65 and when comparing males vs. females, suggesting dose modifications for these groups are not necessary.
CONTRAINDICATIONS
Midodrine hydrochloride is contraindicated in patients with severe organic heart disease, acute renal disease, urinary retention, pheochromocytoma or thyrotoxicosis. Midodrine hydrochloride should not be used in patients with persistent and excessive supine hypertension.
ADVERSE REACTIONS
The most frequent adverse reactions seen in controlled trials were supine and sitting hypertension; paresthesia and pruritus, mainly of the scalp; goosebumps; chills; urinary urge; urinary retention and urinary frequency.
The frequency of these events in a 3-week placebo-controlled trial is shown in the following table:
1 Includes hyperesthesia and scalp paresthesia | ||||
2 Includes dysuria (1), increased urinary frequency (2), impaired urination (1), urinary retention (5), urinary urgency (2) | ||||
3 Includes scalp pruritus | ||||
4 Includes patients who experienced an increase in supine hypertension | ||||
5 Includes abdominal pain and pain increase | ||||
| Placebo n=88 | Midodrine n=82 | |||
| Event | #of reports | % of patients | #of reports | % of patients |
| Total #of reports | 22 | 77 | ||
| Paresthesia 1 | 4 | 4.5 | 15 | 18.3 |
| Piloerection | 0 | 0 | 11 | 13.4 |
| Dysuria 2 | 0 | 0 | 11 | 13.4 |
| Pruritis 3 | 2 | 2.3 | 10 | 12.2 |
| Supine hypertension 4 | 0 | 0 | 6 | 7.3 |
| Chills | 0 | 0 | 4 | 4.9 |
| Pain 5 | 0 | 0 | 4 | 4.9 |
| Rash | 1 | 1.1 | 2 | 2.4 |
Less frequent adverse reactions were headache; feeling of pressure/fullness in the head; vasodilation/flushing face; confusion/thinking abnormality; dry mouth; nervousness/anxiety and rash. Other adverse reactions that occurred rarely were visual field defect; dizziness; skin hyperesthesia; insomnia; somnolence; erythema multiforme; canker sore; dry skin; dysuria; impaired urination; asthenia; backache; pyrosis; nausea; gastrointestinal distress; flatulence and leg cramps.
The most potentially serious adverse reaction associated with Midodrine hydrochloride therapy is supine hypertension. The feelings of paresthesia, pruritus, piloerection and chills are pilomotor reactions associated with the action of midodrine on the alpha-adrenergic receptors of the hair follicles. Feelings of urinary urgency, retention and frequency are associated with the action of midodrine on the alpha-receptors of the bladder neck.
DESCRIPTION
Name: Midodrine Hydrochloride Tablets, USP
Dosage Form: 2.5 mg, 5 mg and 10 mg tablets for oral administration
Active Ingredient: Midodrine hydrochloride, 2.5 mg, 5 mg and 10 mg
Inactive Ingredients: Colloidal Silicone Dioxide, Croscarmellose sodium, Magnesium Stearate, Microcrystalline Cellulose, Pregelatinised Starch, Sodium Lauryl Sulphate
Pharmacological Classification: Vasopressor/Antihypotensive
Chemical Names (USAN: Midodrine Hydrochloride): (1) Acetamide, 2-amino-N-[2-(2,5- dimethoxyphenyl)-2-hydroxyethyl]-monohydrochloride, (±)-; (2) (±)-2-amino-N-(ß-hydroxy-2,5-dimethoxyphenethyl)acetamide monohydrochloride BAN, INN, JAN: Midodrine
Structural formula:
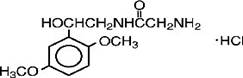
Molecular formula: C 12 H 18 N 2 O 4 HCl;
Molecular Weight: 290.7
Organoleptic Properties: Odorless, white crystalline powder
Solubility: Water:Soluble Methanol: Sparingly soluble
pKa: 7.8 (0.3% aqueous solution)
pH: 3.5 to 5.5 (5% aqueous solution)
Melting Range: 200 to 203°C
CLINICAL PHARMACOLOGY
Mechanism of Action: Midodrine hydrochloride forms an active metabolite, desglymidodrine, that is an alpha1-agonist, and exerts its actions via activation of the alpha-adrenergic receptors of the arteriolar and venous vasculature, producing an increase in vascular tone and elevation of blood pressure. Desglymidodrine does not stimulate cardiac beta-adrenergic receptors. Desglymidodrine diffuses poorly across the blood-brain barrier, and is therefore not associated with effects on the central nervous system.
Administration of Midodrine hydrochloride results in a rise in standing, sitting, and supine systolic and diastolic blood pressure in patients with orthostatic hypotension of various etiologies. Standing systolic blood pressure is elevated by approximately 15 to 30 mmHg at 1 hour after a 10-mg dose of midodrine, with some effect persisting for 2 to 3 hours. Midodrine hydrochloride has no clinically significant effect on standing or supine pulse rates in patients with autonomic failure.
Pharmacokinetics: Midodrine hydrochloride is a prodrug, i.e., the therapeutic effect of orally administered midodrine is due to the major metabolite desglymidodrine, formed by deglycination of midodrine. After oral administration, Midodrine hydrochloride is rapidly absorbed. The plasma levels of the prodrug peak after about half an hour, and decline with a half- life of approximately 25 minutes, while the metabolite reaches peak blood concentrations about 1 to 2 hours after a dose of midodrine and has a half-life of about 3 to 4 hours. The absolute bioavailability of midodrine (measured as desglymidodrine) is 93%. The bioavailability of desglymidodrine is not affected by food. Approximately the same amount of desglymidodrine is formed after intravenous and oral administration of midodrine. Neither midodrine nor desglymidodrine is bound to plasma proteins to any significant extent.
Metabolism and Excretion: Thorough metabolic studies have not been conducted, but it appears that deglycination of midodrine to desglymidodrine takes place in many tissues, and both compounds are metabolized in part by the liver. Neither midodrine nor desglymidodrine is a substrate for monoamine oxidase.
Renal elimination of midodrine is insignificant. The renal clearance of desglymidodrine is of the order of 385 mL/minute, most, about 80%, by active renal secretion. The actual mechanism of active secretion has not been studied, but it is possible that it occurs by the base-secreting pathway responsible for the secretion of several other drugs that are bases (see also Potential for Drug Interactions ).
Clinical Studies
Midodrine has been studied in 3 principal controlled trials, one of 3-weeks duration and 2 of 1 to 2 days duration. All studies were randomized, double-blind and parallel-design trials in patients with orthostatic hypotension of any etiology and supine-to-standing fall of systolic blood pressure of at least 15 mmHg accompanied by at least moderate dizziness/lightheadedness. Patients with pre-existing sustained supine hypertension above 180/110 mmHg were routinely excluded. In a 3-week study in 170 patients, most previously untreated with midodrine, the midodrine-treated patients (10 mg t.i.d., with the last dose not later than 6 P.M.) had significantly higher (by about 20 mmHg) 1-minute standing systolic pressure 1 hour after dosing (blood pressures were not measured at other times) for all 3 weeks. After week 1, midodrine-treated patients had small improvements in dizziness/lightheadedness/unsteadiness scores and global evaluations, but these effects were made difficult to interpret by a high early drop-out rate (about 25% vs 5% on placebo). Supine and sitting blood pressure rose 16/8 and 20/10 mmHg, respectively, on average.
In a 2-day study, after open-label midodrine, known midodrine responders received midodrine 10 mg or placebo at 0, 3, and 6 hours. One-minute standing systolic blood pressures were increased 1 hour after each dose by about 15 mmHg and 3 hours after each dose by about 12mmHg; 3-minute standing pressures were increased also at 1, but not 3, hours after dosing. There were increases in standing time seen intermittently 1 hour after dosing, but not at 3 hours.
In a 1-day, dose-response trial, single doses of 0, 2.5, 10, and 20 mg of midodrine were given to 25 patients. The 10- and 20-mg doses produced increases in standing 1- minute systolic pressure of about 30 mmHg at 1 hour; the increase was sustained in part for 2 hours after 10 mg and 4 hours after 20 mg. Supine systolic pressure was ≥200 mmHg in 22% of patients on 10mg and 45% of patients on 20 mg; elevated pressures often lasted 6 hours or more.
Special Populations
A study with 16 patients undergoing hemodialysis demonstrated that Midodrine hydrochloride is removed by dialysis.
HOW SUPPLIED
Midodrine Hydrochloride Tablets, USP 2.5mg, 5mg and 10mg tablets for oral administration.
Midodrine Hydrochloride Tablets, USP 2.5mg are white to off white, round beveled edge, scored tablets debossed with " ^ " above the score line on one side and "040" on other side.
Bottles of 100 tablets: NDC 72888-112-01
Midodrine Hydrochloride Tablets, USP 5mg are white to off white, round beveled edge, scored tablets debossed with " ^ " above the score line on one side and "041" on other side.
Bottles of 100 tablets: 72888-113-01
Midodrine Hydrochloride Tablets, USP 10mg are white to off white, round beveled edge, scored tablets debossed with " ^ " above the score line on one side and "042" on other side.
Bottles of 100 tablets: NDC 72888-114-01
Store at 20° to 25°C (68° to 77°F) excursions permitted between 15° to 30° C (59° to 86°F) [see USP Controlled Room Temperature].
Dispense in a tight, light-resistant container as defined in the USP, using a child-resistant closure.
To report SUSPECTED ADVERSE REACTIONS, contact FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Distributed By Advagen Pharma Ltd East Windsor, NJ 08520, USA
Manufactured by: Rubicon Research Ltd, Thane 421506, India
Rx Only
Rev. 12/2025