Get your patient on Rebinyn - Coagulation Factor Ix Recombinant, Glycopegylated (Coagulation Factor Ix Recombinant, Glycopegylated)
Rebinyn - Coagulation Factor Ix Recombinant, Glycopegylated prescribing information
INDICATIONS AND USAGE
REBINYN, Coagulation Factor IX (Recombinant), GlycoPEGylated, is a recombinant DNA-derived coagulation Factor IX concentrate indicated for use in adults and children with hemophilia B (congenital Factor IX deficiency) for:
- On-demand treatment and control of bleeding episodes
- Perioperative management of bleeding
- Routine prophylaxis to reduce the frequency of bleeding episodes
Limitations of Use : REBINYN is not indicated for immune tolerance induction in patients with hemophilia B.
DOSAGE AND ADMINISTRATION
For intravenous infusion after reconstitution only.
Dosing Guidelines
- Dose and duration of treatment depend on the location and extent of bleeding, and the patient’s clinical condition.
- If monitoring of Factor IX activity is performed, use a chromogenic assay or selected one-stage clotting assay validated for use with REBINYN [ see Warnings and Precautions (5.5 ) ].
- Each carton and vial label for REBINYN states the actual Factor IX potency in IU.
On-demand Treatment and Control of Bleeding Episodes
REBINYN dosing for on-demand treatment and control of bleeding episodes is provided in Table 1.
Table 1: Dosing for On-demand Treatment and Control of Bleeding Episodes
Type of bleeding | Recommended dose IU/kg body weight | Additional information |
Minor and moderate For example: Uncomplicated joint bleeds, minor muscular bleeds, mucosal or subcutaneous bleeds | 40 | A single dose should be sufficient for minor and moderate bleeds. Additional doses of 40 IU/kg can be given. |
Major For example: Intracranial, retroperitoneal, iliopsoas and neck bleeds, muscle bleeds with compartment syndrome and bleeds associated with a significant decrease in the hemoglobin level | 80 | Additional doses of 40 IU/kg can be given. |
Perioperative Management
REBINYN dosing for perioperative management is provided in Table 2.
Table 2: Dosing for Perioperative Management
Type of surgical procedure | Recommended dose IU/kg body weight | Additional Information |
Minor For example: Implanting pumps in subcutaneous tissue, skin biopsies or simple dental procedures | 40 | A single pre-operative dose should be sufficient. Additional doses can be given if needed. |
Major For example: Body cavity is entered, mesenchymal barrier is crossed, fascial plane is opened, organ is removed, normal anatomy is operatively altered | 80 | Pre-operative dose |
40 | As clinically needed for the perioperative management of bleeding, repeated doses of 40 IU/kg (in 1-3 day intervals) within the first week after major surgery may be administered.• Due to the long half-life of REBINYN, the frequency of dosing in the post-surgical setting may be extended to once weekly after the first week until bleeding stops and healing is achieved. |
•See 12.3 Pharmacokinetics, Table 8
Routine Prophylaxis
For prophylaxis use, the recommended dose is 40 IU/kg body weight once weekly.
Adjust dosing regimen based on individual patient’s bleeding pattern, and physical activity.
Reconstitution
- Always wash hands and ensure that the area is clean before performing the reconstitution procedures.
- Use aseptic technique during the reconstitution procedures.
- If the patient uses more than one vial of REBINYN per infusion, reconstitute each vial according to the following instructions.
Overview of REBINYN Package
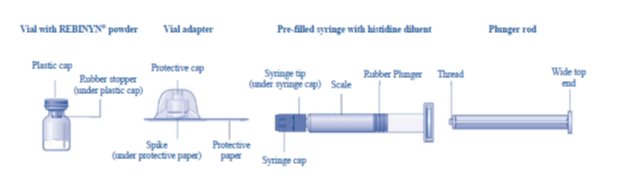
The instructions below serve as a general guideline for reconstitution of REBINYN. For full instructions, refer to the FDA-approved patient information and Instructions for Use.
Reconstitution
- Bring the REBINYN vial and the pre-filled diluent syringe to room temperature.
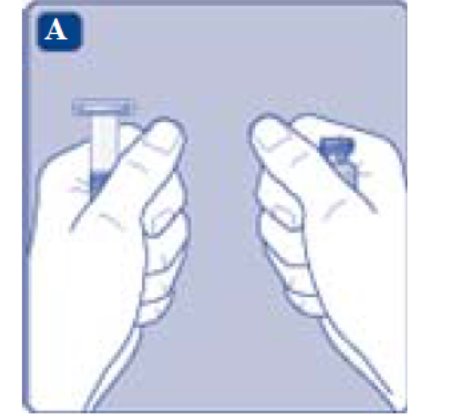
- Remove the plastic cap from the REBINYN vial.

- Wipe the rubber stopper on the vial with a sterile alcohol swab and allow it to dry prior to use.
- Remove the protective paper from the vial adapter. Do not remove the vial adapter from the protective cap.
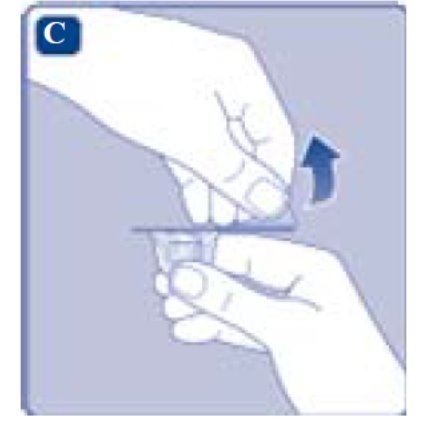
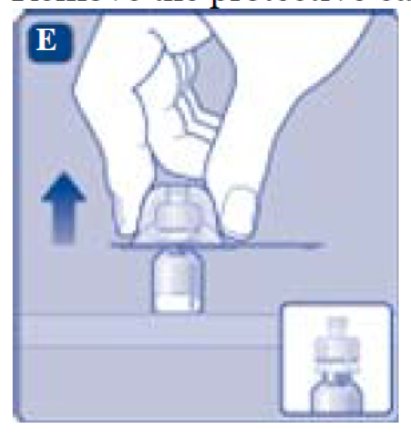
- Place the vial on a flat and solid surface. While holding the protective cap, place the vial adapter over the REBINYN vial and press down firmly on the protective cap until the vial adapter spike penetrates the rubber stopper.
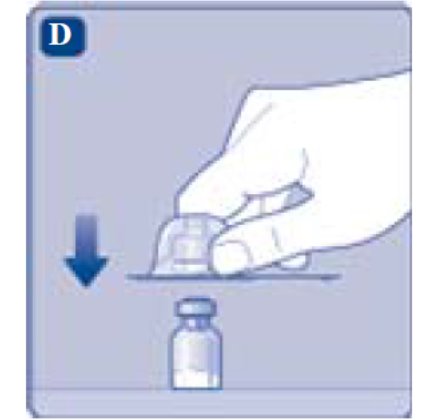
- Remove the protective cap from the vial adapter.
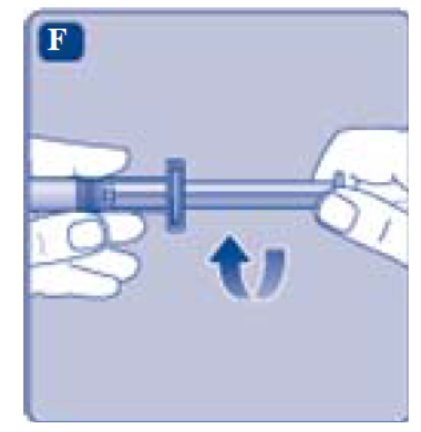
- Grasp the plunger rod as shown in the diagram. Attach the plunger rod to the syringe by holding the plunger rod by the wide top end. Turn the plunger rod clockwise into the rubber plunger inside the pre-filled diluent syringe until resistance is felt.
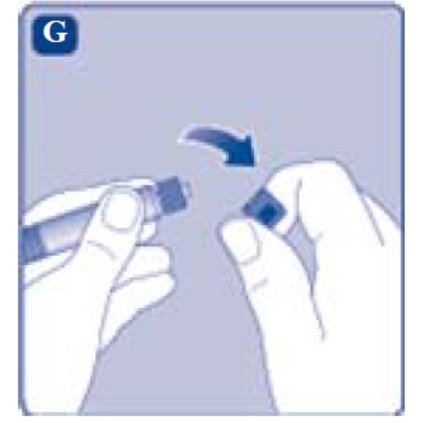
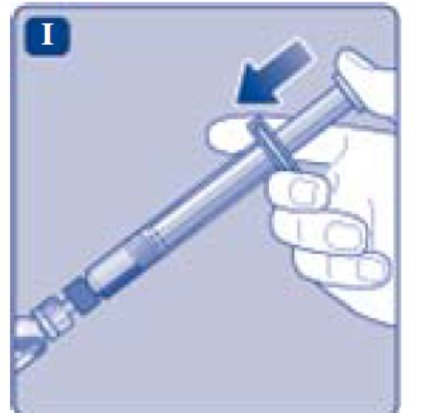
- Break off the syringe cap from the pre-filled diluent syringe by snapping the perforation of the cap.
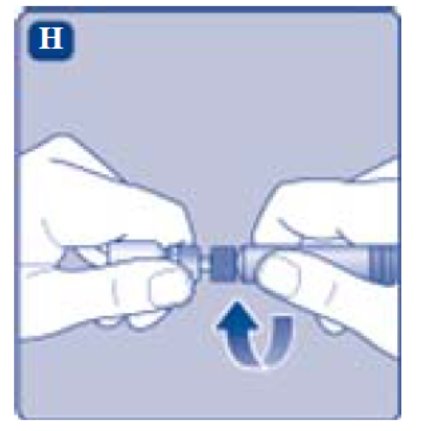
- Connect the pre-filled diluent syringe to the vial adapter by turning it clockwise until it is secured.
- Push the plunger rod to slowly inject all the diluent into the vial.
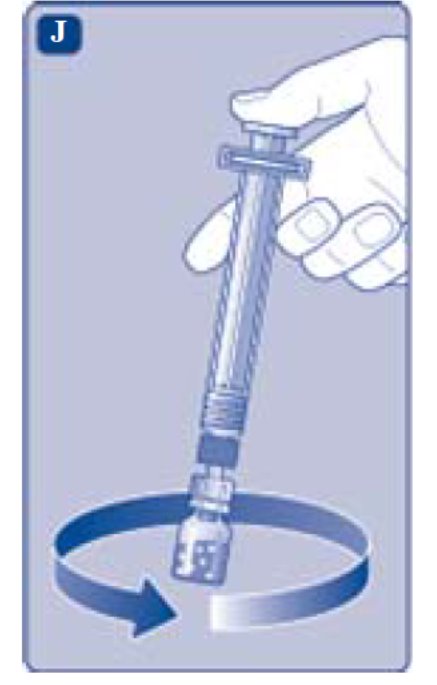
- Without removing the syringe, gently swirl the REBINYN vial until all of the powder is dissolved.
- Administer the REBINYN solution immediately [see Administration (2.3 )]. If not used immediately after reconstitution, store the solution in the vial with the vial adapter and the syringe attached, at room temperature ≤ 86°F (30°C). Do not store for longer than 4 hours.
Administration
For intravenous infusion only.
- Accidental needle stick with a needle contaminated with blood can transmit infectious viruses including HIV (AIDS) and hepatitis. If a needle stick occurs, obtain immediate medical attention. Place needles in a sharps container after single use.
- Inspect the reconstituted REBINYN solution visually prior to administration [ see Description (11 ) ]. The solution should be clear and have no particles. Do not use if particulate matter or discoloration is observed.
- Do not administer REBINYN in the same tubing or container with other medicinal products.
- Invert the REBINYN vial and slowly draw the solution into the syringe.
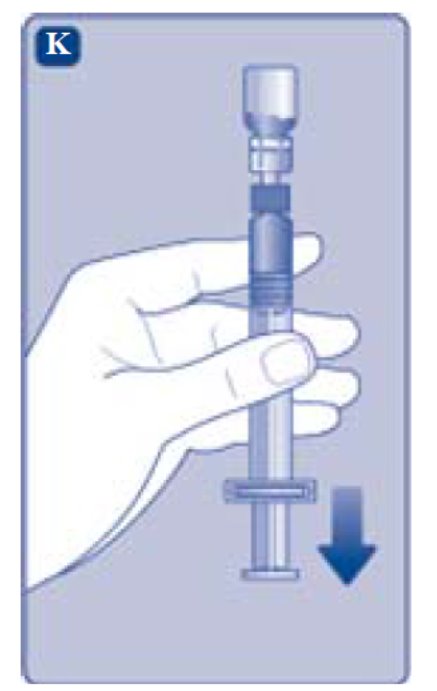
- Detach the syringe from the vial adapter by turning the syringe counterclockwise.
- Attach the syringe to the luer end of an infusion needle set.
- Infuse the reconstituted REBINYN intravenously slowly over 1 to 4 minutes.
- After infusion, safely dispose of the syringe with the infusion set, the vial with the vial adapter, any unused REBINYN, and other waste materials.
Caution: The pre-filled diluent syringe is made of glass with an internal tip diameter of 0.037 inches, and is compatible with a standard Luer-lock connector.
Some needleless connectors for intravenous catheters are incompatible with the glass diluent syringes (for example, certain connectors with an internal spike, such as Clave ® /MicroClave ® , InVision-Plus ® , InVision-Plus CS ® , Invision-Plus Junior ® , Bionector ® ), and their use can damage the connector and affect administration. To administer REBINYN through incompatible needleless connectors, withdraw the reconstituted product into a standard 10 mL sterile Luer-lock plastic syringe.
If you encounter any problems with attaching the pre-filled histidine-diluent syringe to any Luer‐lock compatible device, please contact Novo Nordisk at (844) 303-4448.
DOSAGE FORMS AND STRENGTHS
REBINYN is available as a white to off-white lyophilized powder in single-dose vials containing nominally 500, 1000, 2000, or 3000 IU per vial. Each carton and vial label for REBINYN states the actual Factor IX potency in IU.
After reconstitution with 4 mL of histidine diluent, the reconstituted solution contains approximately 125, 250, 500, or 750 IU per mL of REBINYN respectively.
USE IN SPECIFIC POPULATIONS
Pediatric Use: No dose adjustment is needed (8.4 ).
Pregnancy
Risk Summary
There are no data with REBINYN use in pregnant women to determine whether there is a drug-associated risk. Animal reproduction studies have not been conducted with REBINYN. It is unknown whether REBINYN can cause fetal harm when administered to a pregnant woman or can affect fertility. In the U.S. general population, the estimated background risk of major birth defect and miscarriage in clinically recognized pregnancies is 2-4% and 15-20%, respectively.
Lactation
Risk Summary
There is no information regarding the presence of REBINYN in human milk, the effect on the breastfed infant, and the effects on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for REBINYN and any potential adverse effects on the breastfed infant from REBINYN or from the underlying maternal condition.
Pediatric Use
Safety and efficacy of REBINYN were evaluated in four clinical trials that included 43 PTPs and in one clinical trial that included 50 pediatric PUPs [ see Adverse Reactions (6 ) and Clinical Studies (14 ) ]. Twelve of these subjects were ≤ 6 years of age; 13 subjects were 7 to 12 years of age; and 18 subjects were 13 to 17 years of age. Pharmacokinetic parameters were evaluated for 28 of the pediatric PTPs who were treated with REBINYN 40 IU/kg [ see Clinical Pharmacology (12.3 ) ].
Body weight-adjusted clearance was observed to be higher for pediatric subjects than for adult subjects. However, in clinical trials, no dose adjustment was needed in pediatric subjects who received a fixed dose of 40 IU/kg every week for routine prophylaxis.
Juvenile Animal Toxicity Data
A juvenile animal neurotoxicity study was conducted to evaluate the potential neurotoxicity of REBINYN when intravenously administered 120-1200 IU/kg/twice weekly in immature male rats from 3 to 13 weeks of age, followed by a 13-week treatment-free period. Accumulation of PEG was observed in the choroid plexus, pituitary, circumventricular organs, and the cranial motor neurons. PEG levels in these tissues increased with dose and dose duration (10 weeks) and remained detectable after the 13-week treatment-free period. Treatment-related PEG-positive vacuolated macrophages were observed in the pituitary. The accumulation of PEG was not associated with neurobehavioral changes, fertility, or functional effects.
Geriatric Use
Clinical studies of REBINYN did not include sufficient numbers of subjects age 65 and over to determine whether or not they respond differently than younger subjects.
Animals administered repeat doses of REBINYN showed accumulation of PEG in the choroid plexus, pituitary, circumventricular organs, and cranial motor neurons. [ see Use in Specific Populations (8.4 ) and Animal Toxicology and/or Pharmacology (13.2 ) ]. The potential clinical implications of these animal findings are unknown. No adverse neurologic effects of PEG have been reported in adults exposed to REBINYN during clinical trials, however, use in older adults with baseline cognitive dysfunction has not been fully evaluated [ see Neurologic Considerations (6.3 ) ].
CONTRAINDICATIONS
REBINYN is contraindicated in patients who have known hypersensitivity to REBINYN or its components (including hamster proteins) [ see Warnings and Precautions (5.1 ) and Description (11 ) ]
WARNINGS AND PRECAUTIONS
- Hypersensitivity reactions, including anaphylaxis, have occurred. Should hypersensitivity reactions occur, discontinue REBINYN and administer appropriate treatment (5.1 ).
- Neutralizing antibodies (inhibitors) to Factor IX have occurred following administration of REBINYN. Perform an assay that measures Factor IX inhibitor concentration if bleeding is not controlled with the recommended dose of REBINYN or if plasma Factor IX activity level fails to increase as expected (5.2 , 5.5 ).
- The use of Factor IX- products has been associated with the development of thromboembolic complications (5.3 ).
- Nephrotic syndrome has been reported following immune tolerance induction with Factor IX-containing products in hemophilia B patients with Factor IX inhibitors and a history of allergic reactions to Factor IX. (5.4 )
- Factor IX activity assay results may vary with the type of activated partial thromboplastin time reagent used (5.5 ).
Hypersensitivity Reactions
Allergic-type hypersensitivity reactions, including anaphylaxis, have occurred with REBINYN. The product may contain traces of hamster proteins which in some patients may cause allergic reactions. Signs of allergic reactions, which can progress to anaphylaxis, may include angioedema, chest tightness, difficulty breathing, wheezing, urticaria, and itching. Observe patients for signs and symptoms of acute hypersensitivity reactions, particularly during the early phases of exposure to the product. Discontinue use of REBINYN if allergic- or anaphylactic - type reactions occur, and initiate appropriate treatment.
Inhibitors
The formation of inhibitors (neutralizing antibodies) to Factor IX has occurred following REBINYN. If expected plasma factor IX activity levels are not attained, or if bleeding is not controlled as expected with the administered dose, perform an assay that measures Factor IX inhibitor concentration. Monitor all patients using clinical observations and laboratory tests for the development of inhibitors [ see Warnings and Precautions (5.5) ].
An association between the development of Factor IX inhibitors and allergic reactions has been reported. Evaluate patients experiencing allergic reactions for the presence of an inhibitor. Patients with Factor IX inhibitors may be at an increased risk of severe allergic reactions with subsequent exposure to Factor IX.
Thrombotic Events
The use of Factor IX-containing products has been associated with thromboembolic complications. Due to the potential risk of thromboembolic complications, monitor patients for early signs of thrombotic and consumptive coagulopathy when administering this product to patients with liver disease, post-operatively, to newborn infants, or to patients at risk of thrombosis or disseminated intravascular coagulation (DIC). In each of these situations, the benefit of treatment with REBINYN should be weighed against the risk of these complications.
Nephrotic Syndrome
Nephrotic syndrome has been reported following immune tolerance induction therapy with Factor IX products in hemophilia B patients with Factor IX inhibitors, often with a history of allergic reactions to Factor IX. The safety and efficacy of using REBINYN for immune tolerance induction have not been established.
Monitoring Laboratory Tests
If monitoring of Factor IX activity is performed, use a chromogenic assay or selected one-stage clotting assay validated for use with REBINYN [ see Dosage and Administration (2 ) ].
The one-stage clotting assay results can be significantly affected by the type of activated partial thromboplastin time (aPTT) reagent used, which can result in over- or under-estimation of Factor IX activity. Avoid the use of silica-based reagents, as some may overestimate the activity of REBINYN. If a validated one-stage clotting or chromogenic assay is not available locally, then use of a reference laboratory is recommended.
If bleeding is not controlled with the recommended dose of REBINYN, or if the expected Factor IX activity levels in plasma are not attained, then perform a Bethesda assay to determine if Factor IX inhibitors are present.
ADVERSE REACTIONS
Common adverse reactions (incidence ≥ 1%) in PTPs reported in clinical trials for REBINYN were itching and injection site reactions. Common adverse reactions (incidence ≥ 1%) in PUPs reported in clinical trials for REBINYN were rash, FIX inhibitors, hypersensitivity, itching, injection site reaction, and anaphylactic reaction.
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in clinical trials of another drug and may not reflect the rates observed in clinical practice.
Previously Treated Patients (PTPs)
In five multicenter, prospective, non-controlled, open-label clinical trials, 115 PTPs [0 to 6 years old: 12 subjects (10%); 7 to 12 years old: 13 subjects (11%); 13 to 17 years old: 18 subjects (16%); ≥18 years old: 72 subjects (63%)] received at least one dose of REBINYN as part of routine prophylaxis, on-demand treatment of bleeding episodes, perioperative management of major and minor surgery, or pharmacokinetic evaluation [ see Clinical Studies (14) ]. A PTP was defined as a subject with a history of at least 150 exposure days to other Factor IX products (adolescent/adult subjects) or 50 exposure days to other Factor IX products (pediatric subjects), and no history of inhibitors. A total of 15,167 injections were administered over a median of 733 days (range: 29- 2951 days), equivalent to 15,137 exposure days and 292 patient-years.
Adverse reactions in PTPs are listed in Table 3.
- Table 3: Summary of Adverse Reactions in Previously Treated Patients
System Organ Class | Adverse Reaction | Number of subjects (%) N=115 |
General disorders and administration site conditions | Injection site reactions | 4 (4) |
Immune system disorders | Hypersensitivity | 1 (1) |
Skin and subcutaneous tissue disorders | Itching | 3 (3) |
Previously Untreated Patients (PUPs)
In one multicenter, prospective, non-controlled, open-label clinical trial conducted in PUPs, 50 subjects (≤6 years of age) received at least one dose of REBINYN [see Clinical Studies (14) ]. A PUP was defined as a subject previously untreated or exposed to FIX-containing products less than or equal to 3 exposure days (5 previous exposures to blood components was acceptable). A total of 6,737 injections were administered over a median of 996 days (range: 61- 2,233 days), equivalent to 6,709 exposure days and 142 patient-years.
Adverse reactions in PUPs are listed in Table 4.
Table 4: Summary of Adverse Reactions in Previously Untreated Patients
System Organ Class | Adverse Reaction | Number of subjects (%) N=50 |
Blood and lymphatic system disorders | Factor IX inhibition | 4 (8) |
General disorders and administration site conditions | Injection site reaction | 1 (2) |
Immune system disorders | Anaphylactic reaction Hypersensitivty | 1 (2) 3 (6) |
Skin and subcutaneous tissue disorders | Rash Itching | 9 (18) 2 (4) |
6.2 Immunogenicity
Subjects were monitored for inhibitory antibodies to factor IX prior to dosing, on a monthly basis for the first three months, every two months up to one year, every three months for an additional year, and then every 6 months until end of trial.
No inhibitors were reported in the clinical trials in previously treated patients.
In an ongoing trial in previously untreated patients, one anaphylactic reaction has occurred with development of a factor IX inhibitor following treatment with REBINYN. Inhibitor development and anaphylactic reactions are more likely to occur during the early phases of factor IX replacement therapy [ see Warnings and Precautions (5.1 , 5.2 ) ].
The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors, including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease.
Neurologic Considerations
Animals administered repeat doses of REBINYN showed accumulation of PEG in the choroid plexus, pituitary, circumventricular organs, and cranial motor neurons [ see Use in Specific Populations (8.4 ) and Animal Toxicology and/or Pharmacology (13.2 ) ]. The potential clinical implications of these animal findings are unknown.
In the pediatric studies, 47 PUPs and 25 PTPs receiving routine prophylaxis with REBINYN at a weekly dose of 40 IU/kg were followed for central nervous system (CNS)-related ADRs for 6 and 8 years, respectively. The median duration of follow up of ADRs in the PUP and PTP studies were 2 and 7 years, respectively. Furthermore, neurological examinations were prospectively conducted in 44 PUPs and 17 PTPs with a median follow up of 2 years, and neurocognitive assessments were prospectively performed in 38 PUPs and 16 PTPs with a median follow up of 1 year.
Although no clear clinical implications of the animal findings are known and no clear clinical neurologic or neurocognitive safety signal has emerged, the physician should consider whether the patient is vulnerable to cognitive impairment, such as infants and children who have developing brains, and patients who are cognitively impaired. Factors such as duration of use, cumulative dose, age of the patient and co-morbidities that may increase risk of adverse neurologic and/or neurocognitive events should be considered when prescribing REBINYN. Report adverse neurocognitive and neurologic reactions.
Postmarketing Experience
The following adverse reactions have been identified during post-approval use of REBINYN. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Blood and lymphatic system disorders: Factor IX inhibitor development.
DESCRIPTION
REBINYN is a sterile, non-pyrogenic, white to off-white lyophilized powder for reconstitution with the provided histidine diluent for intravenous infusion. After reconstitution, the solution appears as a clear and colorless to slightly yellow liquid, free from visible particles and contains the following excipients per mL: sodium chloride, 2.34 mg; histidine, 3.10 mg; sucrose, 10 mg; mannitol, 25 mg; polysorbate 80, 0.05 mg. REBINYN is available in single-dose vials containing the labeled amount of Factor IX activity, expressed in IU. Each vial contains nominally 500 IU, 1000 IU, 2000, or 3000 IU. REBINYN potency is assigned using an in vitro , activated partial thromboplastin time (aPTT)-based, one-stage clotting assay calibrated against the World Health Organization (WHO) international standard for Factor IX concentrates. REBINYN contains no preservatives.
REBINYN is a purified recombinant human Factor IX (rFIX) with a 40 kilodalton (kDa) polyethylene-glycol (PEG) conjugated to the protein. The 40 kDa PEG group is selectively attached to specific -N-linked glycans in the rFIX activation peptide, with mono-PEGylated rFIX as the predominant form of REBINYN. The rFIX protein in REBINYN consists of a gamma-carboxylated (Gla) domain, two EGF-like (epidermal growth factor) domains, an activation peptide (which is cleaved off upon activation), and a protease domain. Once activated, the resulting rFIX has structural and functional properties similar to those of endogenous activated Factor IX. The primary amino acid sequence in REBINYN is identical to the Thr148 allelic form of human plasma-derived Factor IX and consists of 415 amino acids. The average molecular weight of REBINYN is approximately 98 kDa and the molecular weight of the protein moiety alone is 56 kDa. The nominal specific activity of REBINYN is 144 IU/mg protein.
REBINYN is produced by recombinant DNA technology in Chinese Hamster Ovary (CHO) cells. No additives of human or animal origin are used in the cell culture, purification, conjugation, or formulation of REBINYN. The rFIX protein is purified by a series of chromatographic steps, including an affinity chromatography step using a monoclonal antibody (produced in CHO cells), to selectively isolate rFIX from the cell culture medium. The production process includes two dedicated viral clearance steps, namely a detergent treatment step for inactivation and a 20 nm filtration step for removal of viruses. The conjugation of the PEG-group is done by an enzymatic reaction during the purification process, followed by final purification of REBINYN.
CLINICAL PHARMACOLOGY
Mechanism of Action
Patients with hemophilia B are deficient in coagulation Factor IX, which is required for effective hemostasis. Treatment with REBINYN temporarily replaces the missing coagulation Factor IX.
The Factor IX in REBINYN is conjugated to a 40-kDa polyethylene glycol molecule, which slows down its removal from the blood circulation.
Pharmacodynamics
The administration of REBINYN increases plasma levels of Factor IX and can temporarily correct the coagulation defect in hemophilia B patients, as reflected by a decrease in aPTT.
Pharmacokinetics
Pharmacokinetic (PK) parameters of REBINYN were evaluated in previously treated subjects, including a subset of subjects in the adult/adolescent trial and all subjects in the main phase of the pediatric trial [ see Clinical Studies (14) ]. PK samples were collected prior to dosing and at multiple time points up to 168 hours after dosing. The analysis of plasma samples was conducted using the one-stage clotting assay.
Steady state pharmacokinetic parameters for adolescents and adults following once-weekly prophylactic treatment of REBINYN 40 IU/kg are shown in Table 5.
Table 5: Steady-state pharmacokinetic parameters of REBINYN (40 IU/kg) in adolescents and adults (geometric mean (CV))
PK Parameter | 13-17 years N=3 | ≥ 18 years N=6 |
Half-life (hours) | 103.1 (14.2) | 114.9 (9.7) |
Incremental Recovery 30min (IU/dL per IU/kg) | 1.82 (28.2) | 1.92 (19.6) |
AUC 0-168 (IU•hours/dL) | 9072 (22) | 9280 (15) |
Clearance (mL/hour/kg) | 0.4 (16.7) | 0.4 (11.4) |
Mean residence time (hours) | 144.4 (15.3) | 158.1 (9.6) |
Vss (mL/kg) | 60.5 (31.1) | 65.8 (11.9) |
Factor IX activity 168 h after dosing (%) | 28.9 (18.6) | 32.4 (17.1) |
Abbreviations: AUC = area under plasma concentration-time curve; Vss= volume of distribution at steady state; CV=coefficient of variation.
The mean steady state pre-dose trough levels and post-dose peak levels across the clinical trials for all previously treated subjects are shown in Table 6.
Table 6: Factor IX peak and trough levels of REBINYN (40 IU/kg) by age at steady state
≤ 6 years N=12 | 7-12 years N=13 | 13-17 years N=9 | ≥18years N=20 | |
Mean Factor IX peak level (%) (95% CI) | 65.5 (60.6; 70.7) | 71.4 (66.3; 77.0) | 82.8 (70.7; 96.9) | 97.9 (87.7; 109.3) |
Mean Factor IX trough level• (%) (95% CI) Min, Max•• | 15.4 (13.2; 17.9) 9.2; 24.5 | 18.7 (16.2; 21.6) 8.3; 28.3 | 23.7 (19.9; 28.2) 18.6; 34.6 | 29.3 (26.0; 33.0) 21.3; 42.2 |
• Factor IX activity from samples collected at clinical site visits just prior to administration of next weekly dose
••Individual geometric mean trough values
Single-dose pharmacokinetic parameters of REBINYN in children, adolescents and adults are listed in Table 7.
Table 7: Single Dose Pharmacokinetic Parameters of REBINYN (40 IU/kg) in children, adolescents and adults (geometric mean (CV))
PK Parameter | ≤ 6 years N=12 | 7-12 years N=13 | 13-17 years N=3 | ≥ 18 years N=6 |
Half-life (hours) | 69.6 (15.8) | 76.3 (25.5) | 89.4 (24.1) | 83.0 (22.5) |
Incremental Recovery 30min (IU/dL per IU/kg) | 1.51 (7.31) | 1.59 (16.2) | 1.96 (14.7) | 2.34 (11.3) |
AUC inf (IU•h/dL) | 4617 (14) | 5618 (19) | 7986 (35) | 9063 (16) |
Clearance (mL/hour/kg) | 0.8 (13.0) | 0.6 (21.9) | 0.5 (30.4) | 0.4 (14.7) |
Mean residence time (hours) | 95.4 (15.3) | 105.1 (24.2) | 124.2 (24.4) | 115.5 (21.8) |
Vss (mL/kg) | 72.3 (14.8) | 68.3 (21.7) | 58.6 (7.8) | 47.0 (15.9) |
Factor IX activity 168 h after dosing (%) | 8.4 (16.3) | 10.9 (18.9) | 14.6 (59.6) | 16.8 (30.6) |
Abbreviations: AUC = area under plasma concentration-time curve; Vss = volume of distribution at steady state; CV = coefficient of variation.
Pharmacokinetics were investigated in 9 subjects in the adult/adolescent trial, of which 5 were normal weight (body mass index (BMI) 18.5 to 24.9 kg/m 2 ) and 4 were overweight (BMI 25 to <29.9 kg/m 2 ). The pharmacokinetic parameters were not affected by BMI.
The Factor IX activity following 80 IU/kg infusion in major surgery is shown in Table 8.
Table 8: Factor IX activity following 80 IU/kg bolus for major surgery
30 minutes | 8 hours 1 | 24 hours 1 | 48 hours 2 | |
N=13 | N=12 | N=12 | N=7 | |
Factor IX activity (%) Median (Range) | 143 (123-224) | 138 (101-175) | 112 (62-146) | 73 (40-110) |
1 Excludes one subject with no Factor IX activity measurement obtained.
2 Excludes two subjects with no Factor IX activity measurement obtained and additionally 4 subjects re-dosed prior to second day after surgery for whom the Factor IX activity at 24 hours were 84%, 112%, 131% and 134%. The 48 hours measurement reflects a measurement on the 2nd day after surgery (range 47-57 hours).
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Studies in animals to evaluate the carcinogenic or genotoxic potential of REBINYN, or dedicated studies to determine the effects of REBINYN on fertility, have not been performed. In a juvenile rat study (3 to 13 week old male rats), fertility was unaffected following 9 weeks of twice weekly administrations of up to 1200 IU/kg [ see Use in Specific Populations (8.4 ) ].
Animal Toxicology and/or Pharmacology
REBINYN was intravenously administered in repeat-dose toxicity studies in adult immune-deficient rats (40-1200 IU/kg/week for 26 weeks), immune-competent monkeys (350-3750 IU/kg/week for 4 weeks), and juvenile immune-competent rats (120‑1200 IU/kg/twice weekly for 10 weeks). Accumulation of PEG was detected in epithelial cells of the choroid plexus in the brain of the adult rats and monkeys. This finding was not associated with morphological changes or abnormal clinical signs. In juvenile rats, more comprehensive assessment of brain tissues demonstrated PEG accumulation in the choroid plexus, pituitary, circumventricular organs, and the cranial motor neurons [ see Use in Specific Populations (8.4 ) ].
CLINICAL STUDIES
Safety and efficacy of REBINYN was evaluated in five multicenter, non-controlled, open-label trials in on-demand treatment of bleeding episodes, perioperative management of major and minor surgery, and routine prophylaxis or pharmacokinetic evaluation in PTPs with hemophilia B (Factor IX activity ≤ 2%). The efficacy evaluation included 105 PTPs [62 adults (18 to 65 years old), 18 adolescents (13 to 17 years old), and 25 children (1 to 12 years old)].
- Adult/adolescent trial: The trial included 74 adolescent and adult subjects. There were two routine prophylaxis arms, with single-blind randomization to either 10 IU/kg or 40 IU/kg once-weekly for approximately 52 weeks, and an open-label on-demand treatment arm for approximately 28 weeks.
- Surgery trial: The surgery trial included 13 adolescent and adult subjects who received one infusion of REBINYN 80 IU/kg on the day of surgery, and post-operatively received infusions of 40 IU/kg, at the investigator’s discretion, for up to 3 weeks after surgery.
- Pediatric trial: The main phase of the pediatric trial included 25 PTPs (1 to 12 years old) in which subjects received routine prophylaxis with REBINYN 40 IU/kg once weekly for approximately 52 weeks until 50 EDs were reached.
Treatment of Bleeding Episodes
Previously Treated Patients
A total of 250 bleeding episodes were reported in 45 out of 69 PTPs receiving either REBINYN 40 IU/kg prophylaxis or on-demand treatment in the clinical program. Bleeding episodes were treated with REBINYN at 40 IU/kg for minor or moderate bleeds or 80 IU/kg for major bleeds, with additional doses of 40 IU/kg as needed. The median dose to treat a bleeding episode was 42 IU/kg.
An overall assessment of efficacy was performed by the subject (for home treatment) or the study site investigator (for treatment under medical supervision) using a 4-point scale of excellent, good, moderate, or poor. The overall success rate (defined as excellent or good) for treatment of bleeding episodes was 95% as shown in Table 9.
The success rate and dose needed for treatment of bleeding episodes were independent of the location of the bleeding. The success rate for treatment of bleeding episodes was also independent of whether the bleed was traumatic or spontaneous.
Table 9: Treatment of Bleeding Episodes in PTPs Receiving Either 40 IU/kg Prophylaxis or
On-Demand Treatment
Treatment | Prophylaxis with 40 IU/kg | On-Demand | Total |
New Bleeding Episodes | 107 | 143 | 250 |
Efficacy assessment• | |||
Excellent or Good | 101 (95%) | 135 (95%) | 236 (95%) |
Moderate or Poor | 5 (5%) | 7 (5%) | 12 (5%) |
Number of injections to treat a bleeding episode | |||
1 injection | 100 (93%) | 120 (84%) | 220 (88%) |
2 injections | 5 (5%) | 20 (14%) | 25 (10%) |
>2 injections | 2 (2%) | 3 (2%) | 5 (2%) |
•Efficacy assessment was based on 248 evaluated bleeding episodes (data missing for two bleeding episodes). Efficacy was assessed according to a four-point scale using:
Excellent: Abrupt pain relief and/or clear improvement in objective signs of bleeding within 8 hours after a single injection; Good: Noticeable pain relief and/or improvement in signs of bleeding within 8 hours after a single injection;
Moderate: Probable or slight beneficial effect within the first 8 hours after the first injection but requiring more than one injection within 8 hours;
Poor: No improvement, or worsening of symptoms within 8 hours after the second of two injections.
Perioperative Management
In the surgery trial, the efficacy analysis of REBINYN in perioperative management included 13 surgical procedures of which 9 were major and performed in 13 previously treated adolescent and adult patients. The procedures included 9 orthopedic, 1 gastrointestinal and 3 in the oral cavity.
The hemostatic effect during surgery was evaluated on a four-point scale of excellent, good, moderate, or poor. The intraoperative hemostatic effect was rated as excellent or good for the 13 surgeries, for a success rate of 100%. A pre-operative dose of 80 IU/kg REBINYN was effective, and no subjects required additional doses on the day of surgery. The median number of additional 40 IU/kg doses in the post-operative period was 2.0 for Days 1 to 6, 1.5 for Days 7-13, and 3.0 for Days 1 to 13. The mean total consumption of REBINYN in the pre- and post-operative period was 241 IU/kg (range: 81 to 460 IU/kg). There was no unexpected postoperative bleeding.
Three additional major surgeries and 18 minor surgery procedures were evaluated in the extension trial for REBINYN in previously treated patients. The hemostatic effect during major and minor surgery was confirmed with a success rate of 100%.
Routine Prophylaxis
Adult/Adolescent PTP Trial
In the main phase of the adult/adolescent PTP trial, 29 subjects (13 to 65 years old) received REBINYN 40 IU/kg once
weekly for approximately 52 weeks. The annualized bleeding rate for these subjects in the main phase is presented in Table 10. Eighteen of 20 (90%) target joints per ISTH definition (≥ 3 spontaneous bleeds into a single joint within a consecutive 6-month period) reported in 13 subjects in the 40 IU/kg once weekly arm at baseline were considered resolved at the end of the main phase.
Table 10: Annualized Bleeding Rate (ABR) in the Adult/Adolescent PTP Trial (40 IU/kg Once Weekly Arm) –
Main Phase
Main Phase | |||
Age of patient | 13-17 years N=9 | 18-65 years N=20 | Overall ≥ 13 years N=29 |
Total ABR | |||
Poisson-estimated mean (95% CI) | 2.19 (0.73 ; 6.54) | 2.68 (1.34 ; 5.35) | 2.52 (1.40; 4.52) |
Median (Q1; Q3) | 1.93 (0.00 ; 4.01) | 1.03 (0.00 ; 4.01) | 1.04 (0.00; 4.01) |
ABR for spontaneous bleeds | |||
Poisson-estimated mean (95% CI) | 0.11 (0.00; 13.23) | 1.77 (0.77; 4.07) | 1.22 (0.46; 3.25) |
Median (Q1; Q3) | 0.00 (0.00; 0.00) | 0.00 (0.00; 1.51) | 0.00 (0.00; 0.99) |
ABR for traumatic bleeds | |||
Poisson-estimated mean (95% CI) | 2.08 (0.98; 4.42) | 0.91 (0.41; 2.02) | 1.29 (0.74; 2.25) |
Median (Q1; Q3) | 1.93 (0.00; 3.87) | 0.00 (0.00; 1.01) | 0.00 (0.00; 2.05) |
ABR for joint bleeds | |||
Poisson-estimated mean (95% CI) | 1.42 (0.36; 5.57) | 2.19 (1.02; 4.73) | 1.94 (0.97; 3.88) |
Median (Q1; Q3) | 0.97 (0.00; 2.17) | 0.51 (0.00; 2.04) | 0.97 (0.00; 2.07) |
CI = confidence interval; Q1 = first quartile; Q3 = third quartile.
Pediatric PTP Trial
In the main phase of the pediatric PTP trial, 25 subjects 0 to 12 years of age received routine prophylactic administration of REBINYN 40 IU/kg once weekly for 52 weeks. The patients were stratified into two age groups: 0 to 6 years and 7 to 12 years, with a least 10 subjects in each arm. Two target joints in 2 subjects in the 7 to 12 years age group at baseline were considered resolved during the main phase.
Table 11: Annualized Bleeding Rate (ABR) in the Pediatric PTP Trial - Main Phase
| ||
Age of patient |
|
|
Mean treatment period (years) |
|
|
Total ABR | ||
Poisson-estimated mean (95% CI) | 0.90 (0.43 ; 1.89) | 2.06 (1.31 ; 3.24) |
Median (Q1; Q3) | 0.00 (0.00 ; 1.98) | 2.00 (0.96 ; 3.00) |
ABR for spontaneous bleeds | ||
Poisson-estimated mean (95% CI) | 0.27 (0.06 ; 1.26) | 0.61 (0.24 ; 1.57) |
Median (Q1; Q3) | 0.00 (0.00 ; 0.00) | 0.00 (0.00 ; 0.96) |
ABR for traumatic bleeds | ||
Poisson-estimated mean (95% CI) | 0.63 (0.28 ; 1.43) | 1.14 (0.65 ; 2.01) |
Median (Q1; Q3) | 0.00 (0.00 ; 1.00) | 0.98 (0.00 ; 1.93) |
ABR for joint bleeds | ||
Poisson-estimated mean (95% CI) | 0.18 (0.04 ; 0.72) | 0.92 (0.52 ; 1.62) |
Median (Q1; Q3) | 0.00 (0.00 ; 0.00) | 0.96 (0.00 ; 1.93) |
CI = confidence interval; Q1 = first quartile; Q3 = third quartile.
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
- REBINYN is supplied in packages comprised of a single-dose vial containing nominally 500, 1000, 2000, or 3000 IU of Factor IX potency; a MixPro ® pre-filled diluent syringe containing 10 mM histidine solution (1.6 mg/mL), and a sterile vial adapter with 25 micrometer filter, which serves as a needleless reconstitution device.
- The actual Factor IX potency in IU is stated on each REBINYN carton and vial.
Table 12: REBINYN Presentations
Presentation (Nominal Product Strength; IU) | Cap Color Indicator | Carton NDC Number | Components |
500 | Red | NDC 0169 7905 01 |
|
1000 | Green | NDC 0169 7901 01 |
|
2000 | Yellow | NDC 0169 7902 01 |
|
3000 | Dark Gray | NDC 0169 7903 01 |
|
- The REBINYN vials are made of glass, closed with a chlorobutyl rubber stopper (not made with natural rubber latex), and sealed with an aluminum cap.
- The pre-filled diluent syringes are made of glass, with a siliconised bromobutyl rubber plunger (not made with rubber latex).
- The closed vials and pre-filled diluent syringes are equipped with a tamper-evident snap-off cap which is made of polypropylene.
Storage and Handling
- Store REBINYN in the original package in order to protect from light.
- Store REBINYN under refrigeration at a temperature of 36°F-46°F (2°C – 8°C) for up to 24 months from the date of manufacture until the expiration date stated on the label.
- REBINYN may be stored at room temperature not to exceed 86°F (30°C) for up to 6 months within the 24-month time period. Record the date when the product was removed from the refrigerator in the space provided on the outer carton. The total time of storage at room temperature should not exceed 6 months. Do not return the product to the refrigerator.
- Do not use REBINYN after the end of the 6-month period at room temperature storage, or after the expiration date stated on the vial, whichever occurs earlier.
- Do not freeze REBINYN.
- Use REBINYN within 4 hours after reconstitution when stored at room temperature. Store the reconstituted product in the vial.
- Discard any unused reconstituted product.
Mechanism of Action
Patients with hemophilia B are deficient in coagulation Factor IX, which is required for effective hemostasis. Treatment with REBINYN temporarily replaces the missing coagulation Factor IX.
The Factor IX in REBINYN is conjugated to a 40-kDa polyethylene glycol molecule, which slows down its removal from the blood circulation.