Get your patient on Tacrolimus - Tacrolimus Extended - Release Capsules capsule, Coated, Extended Release (Tacrolimus Extended-Release Capsules)
Tacrolimus - Tacrolimus Extended - Release Capsules capsule, Coated, Extended Release prescribing information
WARNING: MALIGNANCIES AND SERIOUS INFECTIONS IN TRANSPLANT PATIENTS; AND INCREASED MORTALITY IN FEMALE LIVER TRANSPLANT PATIENTS
- Increased risk for developing serious infections and malignancies with tacrolimus extended-release capsulest or other immunosuppressants that may lead to hospitalization or death. [see Warnings and Precautions (5.1 , 5.2 )]
- Increased mortality in female liver transplant patients with tacrolimus extended-release capsulest. Tacrolimus extended-release capsulest is not approved for use in liver transplantation. [see Warnings and Precautions (5.3 )]
INDICATIONS AND USAGE
Tacrolimus extended-release capsules is indicated for the prophylaxis of organ rejection in kidney transplant patients in combination with other immunosuppressants in adult patients who can swallow capsules intact [see Clinical Studies (14.1 ), (14.2 )] .
Pediatric use information is approved for Astellas Pharma US, Inc.'s ASTAGRAF XL (tacrolimus extended-release capsules). However, due to Astellas Pharma US, Inc.'s marketing exclusivity rights, this drug product is not labeled with that information.
DOSAGE AND ADMINISTRATION
- Capsules must be taken whole. (2.1 )
- Take consistently every morning at the same time on an empty stomach at least 1 hour before a meal or at least 2 hours after a meal. (2.1 )
- Avoid eating grapefruit or drinking grapefruit juice or alcohol. (2.1 )
- African-American patients and patients with severe hepatic impairment may require dosing adjustments. (2.3 )
- Frequent monitoring of trough concentrations is recommended. (2.4 )
- For complete dosing information, see Full Prescribing Information.
| MMF = Mycophenolate mofetil | ||
Recommended Tacrolimus Extended-Release Capsules Initial Dosage | ||
Patient Population | Initial Oral Dosage | Whole Blood Trough Concentration Range |
ADULT | ||
With basiliximab, MMF and steroids | 0.15 mg/kg to 0.2 mg/kg once daily prior to reperfusion or within 48 hours of completion of transplant |
|
With MMF and steroids, without basiliximab induction |
|
|
Important Administration Instructions
- Tacrolimus extended-release capsules should not be used without the supervision by a physician with experience in immunosuppressive therapy.
- Tacrolimus extended-release capsules is not interchangeable or substitutable for tacrolimus extended-release tablets, tacrolimus immediate-release capsules or tacrolimus for oral suspension. Under or overexposure to tacrolimus may result in graft rejection or other serious adverse reactions. Changes between tacrolimus immediate-release and extended-release dosage forms must occur under physician supervision [see Warnings and Precautions (5.4 )].
- Advise patients to swallow tacrolimus extended-release capsules whole with liquid; patients must not chew, divide, or crush the capsules.
- Tacrolimus extended-release capsules should be taken consistently every morning at the same time to ensure consistent and maximum possible drug exposure, on an empty stomach at least 1 hour before a meal, or at least 2 hours after a meal [see Clinical Pharmacology (12.3 )].
- If a dose is missed, the dose may be taken up to 14 hours after the scheduled time (i.e., for a missed 8:00 AM dose, a dose may be taken by 10:00 PM). Beyond the 14-hour time frame, the patient should wait until the usual scheduled time the following morning to take the next regular daily dose. Instruct the patient not to double the next dose.
- Advise patients to avoid eating grapefruit or drinking grapefruit juice or alcoholic beverages while taking tacrolimus extended-release capsules [see Drug Interactions (7.2 )].
- Therapeutic drug monitoring is recommended for all patients receiving tacrolimus extended-release capsules [see Dosage and Administration (2.4 )] .
Dosage Recommendations for Kidney Transplant Patients
Table 1 includes the recommended starting tacrolimus extended-release capsules dosages and whole blood trough concentration ranges; the observed trough concentrations are shown in another section of the Full Prescribing Information [see Clinical Studies (14 )] . Titrate the tacrolimus extended-release capsules dosage based on clinical assessments of rejection and tolerability, and to achieve target trough concentration ranges [see Dosage and Administration (2.4 ) and Warnings and Precautions (5.6 , 5.7 , 5.10 , 5.11 )] .
| MMF = mycophenolate mofetil | ||
Recommended Tacrolimus Extended-Release Capsules Initial Dosage• | ||
Patient Population | Initial Oral Dosage | Whole Blood Trough Concentration Range |
ADULT | ||
With basiliximab, MMF and steroids | 0.15 mg/kg to 0.2 mg/kg once daily prior to reperfusion or within 48 hours of completion of transplant | • Month 1: 7 ng/mL to 15 ng/mL • Month 2 to Month 6: 5 ng/mL to 15 ng/mL • More than 6 Months: 5 ng/mL to 10 ng/mL |
With MMF and steroids, without basiliximab induction | • First dose (pre-operative): 0.1 mg/kg, within 12 hours prior to reperfusion • Subsequent doses (post-operative): 0.2 mg/kg once daily at least 4 hours after pre-operative dose and within 12 hours after reperfusion | • Month 1: 10 ng/mL to 15 ng/mL • Month 2 to Month 6: 5 ng/mL to 15 ng/mL • More than 6 Months: 5 ng/mL to 10 ng/mL |
Pediatric use information is approved for Astellas Pharma US, Inc.'s ASTAGRAF XL (tacrolimus extended-release capsules). However, due to Astellas Pharma US, Inc.'s marketing exclusivity rights, this drug product is not labeled with that information.
Dosage Modifications for African-American Patients, Patients with Hepatic Impairment, and Drug Interactions
African-American patients, compared to Caucasian patients, may need to be titrated to higher tacrolimus extended-release capsules dosages to attain comparable trough concentrations [see Clinical Pharmacology (12.3 ) and Clinical Studies (14 )] .
Patients with severe hepatic impairment (Child-Pugh ≥ 10) may require a lower starting dosage of tacrolimus extended-release capsules, due to the reduced clearance and prolonged half-life [see Clinical Pharmacology (12.3 )].
Dose adjustments of tacrolimus extended-release capsules may be necessary when administered concomitantly with CYP3A inducers or CYP3A inhibitors or cannabidiol [see Warnings and Precautions (5.10 , 5.15 ) and Drug Interactions (7.2 , 7.3 )].
Therapeutic Drug Monitoring
Measure tacrolimus whole blood trough concentrations at least two times on separate days during the first week after initiation of dosing and after a change in dosage, after a change in co-administration of CYP3A4 inducers and/or inhibitors or cannabidiol [see Drug Interactions (7.2 , 7.3 )] , or after a change in renal or hepatic function. When interpreting measured concentrations, consider that the time to achieve tacrolimus steady state is approximately 7 days after initiating or changing the tacrolimus extended-release capsules dose.
Monitor tacrolimus whole blood trough concentrations using a validated assay [e.g., immunoassays or high performance liquid chromatography with tandem mass spectrometric detection (HPLC/MS/MS)]. The immunosuppressive activity of tacrolimus is mainly due to the parent drug rather than to its metabolites. Immunoassays may react with metabolites as well as the parent drug. Therefore, whole blood tacrolimus trough concentrations obtained with immunoassays may be numerically higher than concentrations obtained with an assay using HPLC/MS/MS. Comparison of the whole blood tacrolimus trough concentrations of patients to those described in the prescribing information and other published literature must be made with knowledge of the assay method(s) employed.
DOSAGE FORMS AND STRENGTHS
Tacrolimus extended-release capsules:
- 0.5 mg: opaque yellowish pink cap and opaque light orange body branded with dull red “SD-TC” on the capsule body and dull red “0.5 mg” on the capsule cap.
- 1 mg: opaque light yellow cap and opaque light orange body branded with dull red “SD-TC” on the capsule body and dull red “1 mg” on the capsule cap.
- 5 mg: opaque red-orange cap and opaque orange body branded with dull red “SD-TC” on the capsule body and dull red “5 mg” on the capsule cap.
USE IN SPECIFIC POPULATIONS
Pregnancy: Can cause fetal harm. Advise pregnant women of the potential risk to the fetus. (8.1 , 8.3 )
Pediatric use information is approved for Astellas Pharma US, Inc.'s ASTAGRAF XL (tacrolimus extended-release capsules). However, due to Astellas Pharma US, Inc.'s marketing exclusivity rights, this drug product is not labeled with that information.
Pregnancy
Pregnancy Exposure Registry
There is a pregnancy registry that monitors pregnancy outcomes in women exposed to tacrolimus extended-release capsules during pregnancy. The Transplantation Pregnancy Registry International (TPRI) is a voluntary pregnancy exposure registry that monitors outcomes of pregnancy in female transplant recipients and those fathered by male transplant recipients exposed to immunosuppressants including tacrolimus. Healthcare providers are encouraged to advise their patients to register by contacting the Transplantation Pregnancy Registry International at 1-877-955-6877 or https://www.transplantpregnancyregistry.org/ .
Risk Summary
Tacrolimus can cause fetal harm when administered to a pregnant woman. Data from postmarketing surveillance and TPRI suggest that infants exposed to tacrolimus in utero are at a risk of prematurity, birth defects/congenital anomalies, low birth weight, and fetal distress [see Human Data]. Advise pregnant women of the potential risk to the fetus.
Administration of oral tacrolimus to pregnant rabbits and rats throughout the period of organogenesis was associated with maternal toxicity/lethality, and an increased incidence of abortion, malformation and embryofetal death at clinically relevant doses [0.5 the maximum recommended clinical dose (0.2 mg/kg/day), on a mg/m 2 basis]. Administration of oral tacrolimus to pregnant rats after organogenesis and throughout lactation produced maternal toxicity, effects on parturition, reduced pup viability and reduced pup weight at clinically relevant doses (0.8 the maximum recommended clinical dose, on a mg/m 2 basis). Administration of oral tacrolimus to rats prior to mating, and throughout gestation and lactation produced maternal toxicity/lethality, marked effects on parturition, embryofetal loss, malformations, and reduced pup viability at clinically relevant doses (0.8 times the maximum recommended clinical dose, on a mg/m 2 basis). Interventricular septal defects, hydronephrosis, craniofacial malformations and skeletal effects were observed in offspring that died [see Animal Data].
The background risk of major birth defects and miscarriage in the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Clinical Considerations
Disease-Associated Maternal and/or Embryo-Fetal Risk
Risks during pregnancy are increased in organ transplant recipients. The risk of premature delivery following transplantation is increased. Pre-existing hypertension and diabetes confer additional risk to the pregnancy of an organ transplant recipient. Pre-gestational and gestational diabetes are associated with birth defects/congenital anomalies, hypertension, low birth weight and fetal death.
Cholestasis of pregnancy (COP) was reported in 7% of liver or liver-kidney (LK) transplant recipients, compared with approximately 1% of pregnancies in the general population. However, COP symptoms resolved postpartum and no long-term effects on the offspring were reported.
Maternal Adverse Reactions
Tacrolimus extended-release capsules may increase hyperglycemia in pregnant women with diabetes (including gestational diabetes). Monitor maternal blood glucose levels regularly [see Warnings and Precautions (5.5 )] .
Tacrolimus extended-release capsules may exacerbate hypertension in pregnant women and increase pre-eclampsia. Monitor and control blood pressure [see Warnings and Precautions (5.8 , 5.9 )] .
Fetal/Neonatal Adverse Reactions
Renal dysfunction, transient neonatal hyperkalemia and low birth weight have been reported at the time of delivery in infants of mothers taking tacrolimus extended-release capsules.
Labor or Delivery
There is an increased risk for premature delivery (less than 37 weeks) following transplantation and maternal exposure to tacrolimus extended-release capsules.
Data
Human Data
There are no adequate and well-controlled studies on the effects of tacrolimus in human pregnancy. Safety data from the TPRI and postmarketing surveillance suggest infants exposed to tacrolimus in utero have an increased risk for miscarriage, pre-term delivery (less than 37 weeks), low birth weight (less than 2,500 gram), birth defects/congenital anomalies and fetal distress.
TPRI reported 450 and 241 total pregnancies in kidney and liver transplant recipients exposed to tacrolimus, respectively. The TPRI pregnancy outcomes are summarized in Table 6 . In the table below, the number of recipients exposed to tacrolimus concomitantly with mycophenolic acid (MPA) products during the preconception and first trimester periods is high (27% and 29% for kidney and liver transplant recipients, respectively). Because MPA products may also cause birth defects, the birth defect rate may be confounded and this should be taken into consideration when reviewing the data, particularly for birth defects. Birth defects observed include cardiac malformations, craniofacial malformations, renal/urogenital disorders, skeletal abnormalities, neurological abnormalities and multiple malformations.
Kidney | Liver | |
Pregnancy Outcomes Includes multiple births and terminations. | 462 | 253 |
Miscarriage | 24.5% | 25% |
Live births | 331 | 180 |
Pre-term delivery (less than 37 weeks) | 49% | 42% |
Low birth weight (less than 2,500 gram) | 42% | 30% |
Birth defects | 8% Birth defect rate confounded by concomitant MPA products exposure in over half of offspring with birth defects. | 5% |
Additional information reported by TPRI in pregnant transplant patients receiving tacrolimus included diabetes during pregnancy in 9% of kidney recipients and 13% of liver recipients and hypertension during pregnancy in 53% of kidney recipients and 16.2% of liver recipients.
Animal Data
Administration of oral tacrolimus to pregnant rabbits throughout organogenesis produced maternal toxicity and abortion at 0.32 mg/kg (0.5 times the maximum recommended clinical dose [0.2 mg/kg/day], on a mg/m 2 basis). At 1 mg/kg (1.6 times the maximum recommended clinical dose), embryofetal lethality and fetal malformations (ventricular hypoplasia, interventricular septal defect, bulbous aortic arch, stenosis of ductus arteriosus, omphalocele, gallbladder agenesis, skeletal anomalies) were observed. Administration of 3.2 mg/kg oral tacrolimus (2.6 times the maximum recommended clinical dose) to pregnant rats throughout organogenesis produced maternal toxicity/lethality, embryofetal lethality and decreased fetal body weight in the offspring of C-sectioned dams; and decreased pup viability and interventricular septal defect in offspring of dams that delivered.
In a peri-/postnatal development study, oral administration of tacrolimus to pregnant rats during late gestation (after organogenesis) and throughout lactation produced maternal toxicity, effects on parturition, and reduced pup viability at 3.2 mg/kg (2.6 times the maximum recommended clinical dose); among these pups that died early, an increased incidence of kidney hydronephrosis was observed. Reduced pup weight was observed at 1 mg/kg (0.8 times the maximum recommended clinical dose).
Administration of oral tacrolimus to rats prior to mating, and throughout gestation and lactation produced maternal toxicity/lethality, embryofetal loss and reduced pup viability at 3.2 mg/kg (2.6 times the maximum recommended clinical dose range). Interventricular septal defects, hydronephrosis, craniofacial malformations and skeletal effects were observed in offspring that died. Effects on parturition (incomplete delivery of nonviable pups) were observed at 1 mg/kg (0.8 times the maximum recommended clinical dose) [see Nonclinical Toxicology (13.1 )].
Lactation
Risk Summary
Controlled lactation studies have not been conducted in humans; however, tacrolimus has been reported to be present in human milk. The effects of tacrolimus on the breastfed infant, or on milk production, have not been assessed. Tacrolimus is excreted in rat milk and in peri-/postnatal rat studies; exposure to tacrolimus during the postnatal period was associated with developmental toxicity in the offspring at clinically relevant doses [see Pregnancy (8.1 ) and Nonclinical Toxicology (13.1 )] .
The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for tacrolimus extended-release capsules and any potential adverse effects on the breastfed child from tacrolimus extended-release capsules or from the underlying maternal condition.
Females and Males of Reproductive Potential
Contraception
Tacrolimus extended-release capsules can cause fetal harm when administered to pregnant women. Advise female and male patients of reproductive potential to speak to their healthcare provider on family planning options including appropriate contraception prior to starting treatment with tacrolimus extended-release capsules [see Use in Specific Populations (8.1 ) and Nonclinical Toxicology (13.1 )] .
Infertility
Based on findings in animals, male and female fertility may be compromised by treatment with tacrolimus extended-release capsules [see Nonclinical Toxicology (13.1 )].
Pediatric Use
Pediatric use information is approved for Astellas Pharma US, Inc.’s ASTAGRAF XL (tacrolimus extended-release capsules). However, due to Astellas Pharma US, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
Geriatric Use
Clinical studies of tacrolimus extended-release capsules did not include sufficient numbers of patients aged 65 and over to determine whether they respond differently from younger patients. In Studies 1 and 2, 29 patients were 65 years of age and older, and 3 patients were 75 years of age and over [see Clinical Studies (14 )] . Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Renal Impairment
The pharmacokinetics of tacrolimus in patients with renal impairment was similar to that in healthy subjects with normal renal function. However, due to its potential for nephrotoxicity, monitoring of renal function in patients with renal impairment is recommended; tacrolimus dosage should be reduced if indicated [see Warnings and Precautions (5.6 ) and Clinical Pharmacology (12.3 )] .
Hepatic Impairment
The mean clearance of tacrolimus was substantially lower in patients with severe hepatic impairment (mean Child-Pugh score: more than 10) compared to healthy subjects with normal hepatic function [see Clinical Pharmacology (12.3 )] . With greater tacrolimus whole blood trough concentrations in patients with severe hepatic impairment, there is a greater risk of adverse reactions and dosage reduction is recommended [see Dosage and Administration (2.3 )]. For patients with moderate hepatic impairment, monitor tacrolimus whole blood trough concentrations. For patients with mild hepatic impairment, no dosage adjustments are needed.
Race or Ethnicity
African-American patients may need to be titrated to higher dosages to attain comparable trough concentrations compared to Caucasian patients [see Dosage and Administration (2.3 ), Clinical Pharmacology (12.3 ), and Clinical Studies (14 )].
African-American and Hispanic patients are at increased risk for new onset diabetes after transplant. Monitor blood glucose concentrations and treat appropriately [see Warnings and Precautions (5.5 )].
CONTRAINDICATIONS
Tacrolimus extended-release capsules is contraindicated in patients with known hypersensitivity to tacrolimus [see Adverse Reactions (6.2 )] .
WARNINGS AND PRECAUTIONS
- Not Interchangeable with Other Tacrolimus Products-Medication Errors: Instruct patients or caregivers to recognize the appearance of tacrolimus extended-release capsules. (5.4 )
- New onset diabetes after transplant: Monitor blood glucose. (5.5 )
- Nephrotoxicity (acute and/or chronic): May occur due to tacrolimus extended-release capsules, drug interactions, concomitant nephrotoxic drugs. Monitor renal function; consider dosage reduction. (5.6 )
- Neurotoxicity: Including risk of posterior reversible encephalopathy syndrome (PRES), monitor for neurologic abnormalities; reduce dosage or discontinue tacrolimus extended-release capsules. (5.7 )
- Hyperkalemia: Risk may be increased with other agents associated with hyperkalemia; monitor serum potassium levels. (5.8 )
- Hypertension: May require antihypertensive therapy; monitor relevant drug interactions. (5.9 )
- QT prolongation: Consider obtaining electrocardiograms and monitoring electrolytes in patients at high risk. (5.11 )
- Immunizations: Avoid live vaccines. (5.12 )
- Pure red cell aplasia: Consider discontinuation of tacrolimus extended-release capsules. (5.13 )
- Thrombotic Microangiopathy, Including Hemolytic Uremic Syndrome and Thrombotic Thrombocytopenic Purpura: May occur, especially in patients with infections and certain concomitant medications. (5.14 )
Lymphoma and Other Malignancies
Immunosuppressants, including tacrolimus extended-release capsules, increase the risk of developing lymphomas and other malignancies, particularly of the skin . The risk appears to be related to the intensity and duration of immunosuppression rather than to the use of any specific agent. Examine patients for skin changes and advise to avoid or limit exposure to sunlight and UV light by wearing protective clothing and using a broad-spectrum sunscreen with a high protection factor.
Post-transplant lymphoproliferative disorder (PTLD), associated with Epstein-Barr Virus (EBV), has been reported in immunosuppressed organ transplant patients. The risk of PTLD appears greatest in patients who are EBV seronegative, a population which includes many young children. Monitor EBV serology during treatment.
Serious Infections
Immunosuppressants, including tacrolimus extended-release capsules, increase the risk of developing bacterial, viral, fungal, and protozoal infections, including opportunistic infections. These infections may lead to serious, including fatal, outcomes. Serious viral infections reported include:
- Polyomavirus-associated nephropathy (especially due to BK virus infection)
- JC virus-associated progressive multifocal leukoencephalopathy (PML)
- Cytomegalovirus (CMV) infections: CMV seronegative transplant patients who receive an organ from a CMV seropositive donor are at highest risk of CMV viremia and CMV disease.
Monitor for the development of infection and adjust the immunosuppressive regimen to balance the risk of rejection with the risk of infection [see Adverse Reactions (6.1 , 6.2 )] .
Increased Mortality in Female Liver Transplant Patients
In a clinical trial of 471 liver transplant patients randomized to tacrolimus extended-release capsules or tacrolimus immediate-release product, mortality at 12 months was 10% higher among the 76 female patients (18%) treated with tacrolimus extended-release capsules compared to the 64 female patients (8%) treated with tacrolimus immediate-release product. Tacrolimus extended-release capsules is not approved for the prophylaxis of organ rejection in patients who received a liver transplant.
Not Interchangeable with Other Tacrolimus Products - Medication Errors
Medication errors, including substitution and dispensing errors, between tacrolimus immediate-release products and tacrolimus extended-release capsules were reported outside the U.S. This led to serious adverse reactions, including graft rejection, or other adverse reactions due to under- or over-exposure to tacrolimus. Tacrolimus extended-release capsules is not interchangeable or substitutable for tacrolimus extended-release tablets, tacrolimus immediate-release capsules or tacrolimus for oral suspension. Changes between tacrolimus immediate-release and extended-release dosage forms must occur under physician supervision. Instruct patients and caregivers to recognize the appearance of tacrolimus extended-release capsules [see Dosage Forms and Strengths (3 )] and to confirm with the healthcare provider if a different product is dispensed or if dosing instructions have changed.
New Onset Diabetes After Transplant
Tacrolimus extended-release capsules caused new onset diabetes after transplant (NODAT) in kidney transplant patients, which may be reversible in some patients. African-American and Hispanic kidney transplant patients are at an increased risk. Monitor blood glucose concentrations and treat appropriately [see Adverse Reactions (6.1 ) and Use in Specific Populations (8.8 )] .
Nephrotoxicity due to Tacrolimus Extended-Release Capsules and Drug Interactions
Tacrolimus extended-release capsules, like other calcineurin-inhibitors, can cause acute or chronic nephrotoxicity in transplant patients due to its vasoconstrictive effect on renal vasculature, toxic tubulopathy and tubular-interstitial effects. Acute renal impairment associated with tacrolimus toxicity can result in high serum creatinine, hyperkalemia, decreased secretion of urea and hyperuricemia, and is usually reversible. In patients with elevated serum creatinine and tacrolimus whole blood trough concentrations greater than the recommended range, consider dosage reduction or temporary interruption of tacrolimus administration.
The risk for nephrotoxicity may increase when tacrolimus extended-release capsules is concomitantly administered with CYP3A inhibitors (by increasing tacrolimus whole blood concentrations) or drugs associated with nephrotoxicity (e.g., aminoglycosides, ganciclovir, amphotericin B, cisplatin, nucleotide reverse transcriptase inhibitors, protease inhibitors). When tacrolimus is used concurrently with other known nephrotoxic drugs, monitor renal function and tacrolimus blood concentrations, and adjust dose of both tacrolimus and/or concomitant medications during concurrent use [see Adverse Reactions (6.1 , 6.2 ) and Drug Interactions (7.2 )].
Neurotoxicity
Tacrolimus extended-release capsules may cause a spectrum of neurotoxicities. The most severe neurotoxicities include posterior reversible encephalopathy syndrome (PRES), delirium, seizure and coma; others include tremors, paresthesias, headache, mental status changes, and changes in motor and sensory functions [see Adverse Reactions (6.1 , 6.2 )] . As symptoms may be associated with tacrolimus whole blood trough concentrations at or above the recommended range, monitor for neurologic symptoms and consider dosage reduction or discontinuation of tacrolimus extended-release capsules if neurotoxicity occurs.
Hyperkalemia
Mild to severe hyperkalemia, which may require treatment, has been reported with tacrolimus including tacrolimus extended-release capsules. Concomitant use of agents associated with hyperkalemia (e.g., potassium-sparing diuretics, ACE inhibitors, angiotensin receptor blockers) may increase the risk for hyperkalemia [see Adverse Reactions (6.1 )] . Monitor serum potassium levels periodically during treatment.
Hypertension
Hypertension is a common adverse reaction of tacrolimus extended-release capsules therapy and may require antihypertensive therapy [see Adverse Reactions (6.1 )] . Some antihypertensive drugs can increase the risk for hyperkalemia [see Warnings and Precautions (5.8 )] . Calcium-channel blocking agents may increase tacrolimus blood concentrations and require dosage reduction of tacrolimus extended-release capsules [see Drug Interactions (7.2 )] .
Risk of Rejection with Strong CYP3A Inducers and Risk of Serious Adverse Reactions with Strong CYP3A Inhibitors
The concomitant use of strong CYP3A inducers may increase the metabolism of tacrolimus, leading to lower whole blood trough concentrations and greater risk of rejection. In contrast, the concomitant use of strong CYP3A inhibitors may decrease the metabolism of tacrolimus, leading to higher whole blood trough concentrations and greater risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation) [see Warnings and Precautions (5.7 , 5.11 )] . Therefore, adjust tacrolimus extended-release capsules dose and monitor tacrolimus whole blood trough concentrations when co-administering tacrolimus extended-release capsules with strong CYP3A inhibitors (e.g., including, but not limited to, telaprevir, boceprevir, ritonavir, ketoconazole, itraconazole, voriconazole, clarithromycin) or strong CYP3A inducers (e.g., including, but not limited to, rifampin, rifabutin) [see Dosage and Administration (2.4 ) and Drug Interactions (7.2 )] . A rapid, sharp rise in tacrolimus levels has been reported after co-administration with a strong CYP3A4 inhibitor, clarithromycin, despite an initial reduction of tacrolimus dose. Early and frequent monitoring of tacrolimus whole blood trough levels is recommended [see Drug Interactions (7.2) ] .
QT Prolongation
Tacrolimus extended-release capsules may prolong the QT/QTc interval and cause Torsades de pointes . Avoid tacrolimus extended-release capsules in patients with congenital long QT syndrome. Consider obtaining electrocardiograms and monitoring electrolytes (magnesium, potassium, calcium) periodically during treatment in patients with congestive heart failure, bradyarrhythmias, those taking certain antiarrhythmic medications or other products that lead to QT prolongation, and those with electrolyte disturbances (e.g., hypokalemia, hypocalcemia, or hypomagnesemia).
When co-administering tacrolimus extended-release capsules with other substrates and/or inhibitors of CYP3A, especially those that also have the potential to prolong the QT interval, a reduction in tacrolimus extended-release capsules dosage, monitoring of tacrolimus whole blood concentrations, and monitoring for QT prolongation is recommended [see Dosage and Administration (2.4 ) and Drug Interactions (7.2 )] .
Immunizations
Whenever possible, administer the complete complement of vaccines before transplantation and treatment with tacrolimus extended-release capsules.
Avoid the use of live attenuated vaccines during treatment with tacrolimus extended-release capsules (e.g., intranasal influenza, measles, mumps, rubella, oral polio, BCG, yellow fever, varicella, and TY21a typhoid vaccines).
Inactivated vaccines noted to be safe for administration after transplantation may not be sufficiently immunogenic during treatment with tacrolimus extended-release capsules.
Pure Red Cell Aplasia
Cases of pure red cell aplasia (PRCA) have been reported in patients treated with tacrolimus. All of these patients reported risk factors for PRCA such as parvovirus B19 infection, underlying disease, or concomitant medications associated with PRCA. A mechanism for tacrolimus-induced PRCA has not been elucidated. If PRCA is diagnosed, consider discontinuation of tacrolimus extended-release capsules.
Thrombotic Microangiopathy (TMA) Including Hemolytic Uremic Syndrome and Thrombotic Thrombocytopenic Purpura
Cases of thrombotic microangiopathy (TMA), including hemolytic uremic syndrome (HUS) and thrombotic thrombocytopenic purpura (TTP), have been reported in patients treated with tacrolimus extended-release capsules TMA may have a multifactorial etiology. Risk factors for TMA that can occur in transplant patients include, for example, severe infections, graft-versus-host disease (GVHD), Human Leukocyte Antigen (HLA) mismatch, the use of calcineurin inhibitors and mammalian target of rapamycin (mTOR) inhibitors. These risk factors may, either alone or combined, contribute to the risk of TMA.
In patients with signs and symptoms of TMA, consider tacrolimus as a risk factor. Concurrent use of tacrolimus and mTOR inhibitors may contribute to the risk of TMA.
Cannabidiol Drug Interactions
When cannabidiol and tacrolimus extended-release capsules are co-administered, closely monitor for an increase in tacrolimus blood levels and for adverse reactions suggestive of tacrolimus toxicity. A dose reduction of tacrolimus extended-release capsules should be considered as needed when tacrolimus extended-release capsules is co-administered with cannabidiol [see Dosage and Administration (2.4) and Drug Interactions (7.3) ] .
ADVERSE REACTIONS
The following clinically significant adverse drug reactions are discussed in greater detail in other sections of labeling:
- Lymphoma and Other Malignancies [see Warnings and Precautions (5.1 )]
- Serious Infections [see Warnings and Precautions (5.2 )]
- Increased Mortality in Female Liver Transplant Patients [see Warnings and Precautions (5.3 )]
- New Onset Diabetes after Transplant [see Warnings and Precautions (5.5 )]
- Nephrotoxicity due to Tacrolimus Extended-Release Capsules and Drug Interactions [see Warnings and Precautions (5.6 )]
- Neurotoxicity [see Warnings and Precautions (5.7 )]
- Hyperkalemia [see Warnings and Precautions (5.8 )]
- Hypertension [see Warnings and Precautions (5.9 )]
- QT Prolongation [see Warnings and Precautions (5.11 )]
- Pure Red Cell Aplasia [see Warnings and Precautions (5.13 )]
- Thrombotic Microangiopathy, Including Hemolytic Uremic Syndrome and Thrombotic Thrombocytopenic Purpura [see Warnings and Precautions (5.14) ]
Clinical Studies Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. In addition, the clinical trials were not designed to establish comparative differences across study arms with regards to the adverse reactions discussed below.
Kidney transplant patients were treated with tacrolimus extended-release capsules (N=214) or tacrolimus immediate-release product (N=212) and concomitant immunosuppressants (median duration of exposure of 12 months) in a randomized, open-label, active-controlled trial of mostly U.S. patients (Study 1) [see Clinical Studies (14.1 )] . The types of adverse reactions seen in Study 1 were similar to the adverse reactions seen in Study 2 [non-U.S. trial in kidney transplant patients treated with tacrolimus extended-release capsules (N=331) or tacrolimus immediate-release product (N=336) and concomitant immunosuppressants] [see Clinical Studies (14.2 )] .
In Study 1, the proportion of patients who discontinued treatment due to adverse reactions was 9% and 11% in the tacrolimus extended-release capsules and tacrolimus immediate-release treatment groups, respectively, through 12 months of treatment. The most common adverse reactions leading to discontinuation in tacrolimus extended-release capsules-treated patients were related to infections or renal/urinary disorders.
Infections The overall incidence of infections, serious infections, and infections with identified etiology reported in patients treated with the tacrolimus extended-release capsules or tacrolimus immediate-release product in Study 1 are shown in Table 2 .
Tacrolimus extended-release capsules, MMF, steroids, basiliximab induction N=214 | Tacrolimus immediate-release product, MMF, steroids, basiliximab induction N=212 | |
All Infections | 69% | 69% |
Respiratory Infections | 34% | 31% |
Urinary Tract Infections | 16% | 25% |
Cytomegalovirus Infections | 10% | 11% |
Bacterial Infections | 8% | 12% |
Gastroenteritis | 7% | 3% |
Polyomavirus Infections | 3% | 5% |
Serious Infections | 22% | 23% |
New Onset Diabetes After Transplant (NODAT) The incidence of new onset diabetes after transplantation (defined by the composite occurrence of ≥ 2 fasting plasma glucose values that were more than 126 mg/dL at ≥ 30 days apart, insulin use for ≥ 30 consecutive days, oral hypoglycemic use for ≥ 30 consecutive days, and/or HbA 1C ≥ 6.5%) is summarized in Table 3 below for Study 1 through one year post-transplant [see Warnings and Precautions (5.5 )] .
| Tacrolimus extended-release capsules, MMF, steroids, basiliximab induction N=162 | Tacrolimus immediate-release product, MMF, steroids, basiliximab induction N=151 | |
|---|---|---|
Composite NODAT | 36% | 35% |
≥ 2 Fasting Plasma Glucose Values ≥ 126 mg/dL ≥ 30 days apart | 26% | 23% |
HbA 1C ≥ 6.5% | 19% | 22% |
Oral hypoglycemic use ≥ 30 consecutive days | 14% | 9% |
Insulin use ≥ 30 consecutive days | 6% | 8% |
Hyperkalemia In Study 1 [see Clinical Studies (14.1 )] , 73 of 214 (34.1%) patients on tacrolimus extended-release capsules had a serum potassium level greater than 5.4 up to 6.4 mEq/L, and 8 out of 214 (3.7%) patients had a serum potassium level greater than 6.4 mEq/L [see Warnings and Precautions (5.8 )] .
Common Adverse Reactions The most common (≥ 30%) adverse reactions observed with tacrolimus extended-release capsules in Study 1 were: diarrhea, constipation, nausea, peripheral edema, tremor, and anemia. The incidence of adverse reactions that occurred in ≥ 15% of tacrolimus extended-release capsules-treated patients compared to tacrolimus immediate-release product through one year of treatment in Study 1 is shown by treatment groups in Table 4 .
Tacrolimus extended-release capsules, MMF, steroids, basiliximab induction N=214 | Tacrolimus immediate-release product, MMF, steroids, basiliximab induction N=212 | |
Diarrhea | 45% | 44% |
Constipation | 40% | 32% |
Nausea | 36% | 35% |
Peripheral Edema | 36% | 34% |
Tremor | 35% | 34% |
Anemia | 33% | 29% |
Hypertension | 28% | 30% |
Vomiting | 25% | 25% |
Hypomagnesemia | 24% | 27% |
Insomnia | 24% | 28% |
Hypophosphatemia | 23% | 28% |
Headache | 22% | 24% |
Hyperkalemia | 20% | 23% |
Increased Blood Creatinine | 19% | 23% |
Fatigue | 16% | 10% |
Leukopenia | 16% | 16% |
Hyperlipidemia | 16% | 17% |
Hyperglycemia | 16% | 18% |
Less Frequently Reported Adverse Reactions (less than 15% in tacrolimus extended-release capsules-treated patients) by System Organ Class
The following adverse reactions were reported in clinical studies of kidney transplant patients who were treated with tacrolimus extended-release capsules, MMF, and steroids (Studies 1 and 2):
- Blood and Lymphatic System Disorders: Hemolytic anemia, leukocytosis, neutropenia, thrombocytopenia, thrombotic microangiopathy
- Cardiac Disorders: Atrial fibrillation, atrial flutter, tachycardia
- Ear Disorders: Tinnitus
- Eye Disorders: Vision blurred, conjunctivitis
- Gastrointestinal Disorders: Abdominal distension, abdominal pain, aphthous stomatitis, dyspepsia, esophagitis, flatulence, gastritis, gastroesophageal reflux disease
- General Disorders and Administration Site Conditions: Anasarca, asthenia, edema, pyrexia
- Hepatobiliary Disorders: Abnormal hepatic function, cholestasis, hepatitis (acute and chronic), hepatotoxicity
- Infections and Infestations: Condyloma acuminatum, tinea versicolor
- Injury: Fall
- Investigations: Increased blood lactate dehydrogenase, increased blood urea, increased hepatic enzyme
- Metabolism and Nutrition Disorders: Anorexia, hyperphosphatemia, hyperuricemia, hypokalemia, hyponatremia, metabolic acidosis
- Musculoskeletal and Connective Tissue Disorders: Arthralgia, osteopenia, osteoporosis
- Neoplasms: Kaposi’s sarcoma
- Nervous System Disorders: Convulsion, dizziness, hypoesthesia, neurotoxicity, paresthesia, peripheral neuropathy
- Psychiatric Disorders: Agitation, anxiety, confusional state, depression, hallucination, mood swings, nightmare
- Renal and Urinary Disorders: Anuria, oliguria, proteinuria, renal failure, renal tubular necrosis, toxic nephropathy
- Respiratory, Thoracic and Mediastinal Disorders: Acute respiratory distress syndrome, dyspnea, pulmonary edema, productive cough
- Skin and Subcutaneous Tissue Disorders: Acne, alopecia, dermatitis, hyperhidrosis, hypotrichosis, pruritus, rash
- Vascular Disorders: Deep vein thrombosis, flushing
Pediatrics
Pediatric use information is approved for Astellas Pharma US, Inc.'s ASTAGRAF XL (tacrolimus extended-release capsules). However, due to Astellas Pharma US, Inc.'s marketing exclusivity rights, this drug product is not labeled with that information.
Postmarketing Experience
The following adverse reactions have been reported from marketing experience with tacrolimus in the U.S. and outside the U.S. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. These reactions have been chosen for inclusion due to either their seriousness, frequency of reporting or causal connection to tacrolimus extended-release capsules:
- Blood and Lymphatic System Disorders: Agranulocytosis, disseminated intravascular coagulation, hemolytic uremic syndrome, febrile neutropenia, pancytopenia, pure red cell aplasia [see Warnings and Precautions (5.13 )] , coagulopathy, thrombotic thrombocytopenic purpura, prolonged activated partial thromboplastin time, decreased blood fibrinogen
- Cardiac Disorders: Cardiac arrest, myocardial infarction, ventricular fibrillation, congestive cardiac failure, hypertrophic cardiomyopathy, pericardial effusion, angina pectoris, supraventricular extrasystoles, supraventricular tachycardia, bradycardia, Torsades de pointes , QT prolongation
- Ear Disorders: Hearing loss
- Eye Disorders: Blindness, optic neuropathy, optic atrophy, photophobia
- Gastrointestinal Disorders: Gastrointestinal hemorrhage, gastrointestinal perforation, pancreatitis, peritonitis, stomach ulcer, intestinal obstruction, ascites, colitis, ileus, impaired gastric emptying, dysphagia
- Hepatobiliary Disorders: Hepatic failure, hepatic necrosis, cirrhosis, cholangitis, venoocclusive liver disease, bile duct stenosis, hepatic steatosis, jaundice
- Hypersensitivity Reactions: Hypersensitivity, Stevens-Johnson syndrome, toxic epidermal necrolysis, urticaria
- Immune System Disorders: Graft versus host disease (acute and chronic)
- Investigations: Increased international normalized ratio
- Metabolism and Nutrition Disorders: Hypoproteinemia
- Musculoskeletal and Connective Tissue Disorders: Rhabdomyolysis, myalgia, polyarthritis, pain in extremity including Calcineurin-Inhibitor Induced Pain Syndrome (CIPS)
- Neoplasms: Lymphoma including EBV-associated lymphoproliferative disorder, hepatosplenic T-cell lymphoma, PTLD [see Warnings and Precautions (5.1 )] , leukemia, melanoma
- Nervous System Disorders: Cerebral infarction, progressive multifocal leukoencephalopathy (PML) sometimes fatal [see Warnings and Precautions (5.2 )] , posterior reversible encephalopathy syndrome (PRES) [see Warnings and Precautions (5.7 )] , coma, status epilepticus, quadriplegia, flaccid paralysis, hemiparesis, aphasia, syncope, carpal tunnel syndrome, nerve compression, mutism, dysarthria, somnolence
- Psychiatric Disorders: Mental status changes
- Renal and Urinary Disorders: Hemorrhagic cystitis, hematuria, urinary retention, urinary incontinence
- Respiratory, Thoracic and Mediastinal Disorders: Interstitial lung disease, pulmonary hypertension, lung infiltration, rhinitis allergic, hiccups
- Skin and Subcutaneous Tissue Disorders: Hyperpigmentation, photosensitivity
- Vascular Disorders: Hemorrhage
DRUG INTERACTIONS
- Risk of rejection with strong CYP3A inducers and risk of serious adverse reactions with strong CYP3A inhibitors: Adjust dose and monitor tacrolimus concentrations. (2.4 , 5.10 , 7.2 )
- Therapeutic drug monitoring and dose reduction for tacrolimus extended-release capsules should be considered when tacrolimus extended-release capsules is co-administered with cannabidiol. (2.4 , 5.15 , 7.3 )
- See Full Prescribing Information for clinically significant drug interactions. (7.1 , 7.2 , 7.3 )
Mycophenolic Acid
When tacrolimus extended-release capsules is prescribed with a given dose of a mycophenolic acid (MPA) product, exposure to MPA is higher with tacrolimus extended-release capsules co-administration than with cyclosporine co-administration with MPA, because cyclosporine interrupts the enterohepatic recirculation of MPA while tacrolimus does not. Monitor for MPA-associated adverse reactions and reduce the dose of concomitantly administered mycophenolic acid products as needed.
Effects of Other Drugs on Tacrolimus Extended-Release Capsules
Table 5 displays the effects of other drugs on tacrolimus extended-release capsules.
Drug/Substance Class or Name | Drug Interaction Effect | Recommendations |
Grapefruit or grapefruit juice High dose or double strength grapefruit juice is a strong CYP3A inhibitor; low dose or single strength grapefruit juice is a moderate CYP3A inhibitor. | May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation) [see Warnings and Precautions (5.7 , 5.10 , 5.11 )] . | Avoid grapefruit or grapefruit juice. |
Alcohol | May increase the rate of tacrolimus release and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation ) [see Warnings and Precautions (5.7 , 5.10 , 5.11 )] . | Avoid alcoholic beverages. |
Strong CYP3A Inducers Strong CYP3A inhibitor/inducer, based on reported effect on exposures to tacrolimus along with supporting in vitro CYP3A inhibitor/inducer data, or based on drug-drug interaction studies with midazolam (sensitive CYP3A probe substrate). : Antimycobacterials (e.g., rifampin, rifabutin), anticonvulsants (e.g., phenytoin, carbamazepine and phenobarbital), St John’s wort | May decrease tacrolimus whole blood trough concentrations and increase the risk of rejection [see Warnings and Precautions (5.10 )] . | Increase tacrolimus extended-release capsules dose and monitor tacrolimus whole blood trough concentrations [see Dosage and Administration (2.3 , 2.4 ) and Clinical Pharmacology (12.3 )] . |
Strong CYP3A Inhibitors: Protease inhibitors (e.g., nelfinavir, telaprevir, boceprevir, ritonavir), azole antifungals (e.g., voriconazole, posaconazole, itraconazole, ketoconazole), antibiotics (e.g., clarithromycin, troleandomycin, chloramphenicol), nefazodone, letermovir, Schisandra sphenanthera extracts | May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation). A rapid, sharp rise in tacrolimus levels may occur early, despite an immediate reduction of tacrolimus dose [see Warnings and Precautions (5.7 , 5.10 , 5.11 )] . | Reduce tacrolimus extended-release capsules dose (for voriconazole and posaconazole, give one-third of the original dose) and adjust dose based on tacrolimus whole blood trough concentrations [see Dosage and Administration (2.3 , 2.4 ) and Clinical Pharmacology (12.3 )] . Early and frequent monitoring of tacrolimus whole blood trough levels should start within 1-3 days and continue monitoring as necessary [see Warnings and Precautions (5.10) ] . |
Mild or Moderate CYP3A Inhibitors: Clotrimazole, antibiotics (e.g., verapamil, diltiazem, nifedipine, nicardipine), amiodarone, danazol, ethinyl estradiol, cimetidine, lansoprazole and omeprazole | May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation) [see Warnings and Precautions (5.7 , 5.10 , 5.11 )] . | Monitor tacrolimus whole blood trough concentrations and reduce tacrolimus extended-release capsules dose if needed [see Dosage and Administration (2.3 , 2.4 ) and Clinical Pharmacology (12.3 )] . |
Other drugs, such as: Magnesium and aluminum hydroxide antacids Metoclopramide | May increase tacrolimus whole blood trough concentrations and increase the risk of serious adverse reactions (e.g., neurotoxicity, QT prolongation) [see Warnings and Precautions (5.7 , 5.10 , 5.11 )] . | Monitor tacrolimus whole blood trough concentrations and reduce tacrolimus extended-release capsules dose if needed [see Dosage and Administration (2.3 , 2.4 ) and Clinical Pharmacology (12.3 )] . |
Mild or Moderate CYP3A Inducers Methylprednisolone, prednisone | May decrease tacrolimus whole blood trough concentrations. | Monitor tacrolimus whole blood trough concentrations and adjust tacrolimus extended-release capsules dose if needed [see Dosage and Administration (2.3 , 2.4 )] . |
Caspofungin | May decrease tacrolimus whole blood trough concentrations. | Monitor tacrolimus whole blood trough concentrations and adjust tacrolimus extended-release capsules dose if needed [see Dosage and Administration (2.3 , 2.4) ] . |
Direct Acting Antiviral (DAA) Therapy
The pharmacokinetics of tacrolimus may be impacted by changes in liver function during DAA therapy, related to clearance of HCV virus. Close monitoring and potential dose adjustment of tacrolimus extended-release capsules is warranted to ensure continued efficacy and safety [see Dosage and Administration (2.3 , 2.4 )] .
Cannabidiol
The blood levels of tacrolimus may increase upon concomitant use with cannabidiol. When cannabidiol and tacrolimus extended-release capsules are co-administered, closely monitor for an increase in tacrolimus blood levels and for adverse reactions suggestive of tacrolimus toxicity. A dose reduction of tacrolimus extended-release capsules should be considered as needed when tacrolimus extended-release capsules is co-administered with cannabidiol [see Dosage and Administration (2.4) and Warnings and Precautions (5.15) ] .
DESCRIPTION
Tacrolimus is the active ingredient in tacrolimus extended-release capsules. Tacrolimus is a calcineurin-inhibitor immunosuppressant produced by Streptomyces tsukubaensis . Chemically, tacrolimus is designated as [3 S – [3 R •[ E (1 S •, 3 S •, 4 S •)], 4 S •, 5 R •, 8 S •, 9 E , 12 R •, 14 R •, 15 S •, 16 R •, 18 S •, 19 S •, 26a R •]] – 5, 6, 8, 11, 12, 13, 14, 15, 16, 17, 18, 19, 24, 25, 26, 26a – hexadecahydro – 5, 19 – dihydroxy – 3 – [2 – (4 – hydroxy – 3 – methoxycyclo – hexyl) – 1 – methylethenyl] – 14, 16 – dimethoxy – 4, 10, 12, 18 – tetramethyl – 8 – (2 – propenyl) – 15, 19 – epoxy – 3H – pyrido[2, 1 – c ][1, 4]oxaazacyclotricosine – 1, 7, 20, 21(4H, 23H) – tetrone, monohydrate.
The chemical structure of tacrolimus is:
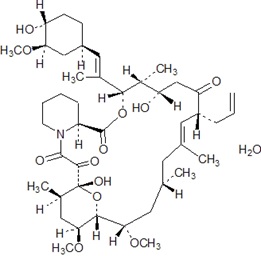
Tacrolimus has an empirical formula of C 44 H 69 NO 12 •H 2 O and a formula weight of 822.03. Tacrolimus appears as white crystals or crystalline powder. It is practically insoluble in water, freely soluble in ethanol, and very soluble in methanol and chloroform.
Tacrolimus extended-release capsules is available for oral administration as hard gelatin capsules containing the equivalent of 0.5 mg, 1 mg or 5 mg of anhydrous tacrolimus, USP. Inactive ingredients include ethylcellulose NF, hypromellose USP, magnesium stearate NF and lactose monohydrate NF. The ingredients are directly proportional across all capsule strengths. The capsule shell contains gelatin NF, ferric oxide red NF, ferric oxide yellow NF, and titanium dioxide USP.
CLINICAL PHARMACOLOGY
Mechanism of Action
Tacrolimus binds to an intracellular protein, FKBP-12. A complex of tacrolimus-FKBP-12, calcium, calmodulin, and calcineurin (a ubiquitous mammalian intracellular enzyme) is then formed and the phosphatase activity of calcineurin is inhibited. Such inhibition prevents the dephosphorylation and translocation of various factors such as the nuclear factor of activated T-cells (NF-AT), and nuclear factor kappa-light-chain-enhancer of activated B-cells (NF-κB).
Tacrolimus inhibits the expression and/or production of several cytokines that include interleukin (IL)-1 beta, IL‑2, IL-3, IL-4, IL-5, IL-6, IL-8, IL-10, gamma interferon, tumor necrosis factor-alpha, and granulocyte macrophage colony-stimulating factor. Tacrolimus also inhibits IL-2 receptor expression and nitric oxide release, induces apoptosis and production of transforming growth factor-beta that can lead to immunosuppressive activity. The net result is the inhibition of T-lymphocyte activation and proliferation as well as T-helper-cell-dependent B-cell response (i.e., immunosuppression).
Pharmacokinetics
Table 7 summarizes the pharmacokinetic (PK) parameters of tacrolimus following oral administration of tacrolimus extended-release capsules in healthy subjects and in kidney transplant patients. Whole blood tacrolimus concentrations in these PK studies were measured using validated HPLC/MS/MS assays.
Population | Tacrolimus Extended-Release Capsules Dose Healthy adult subjects (actual administered dose of tacrolimus extended-release capsules); adult de novo kidney transplant patients (actual group mean dose of tacrolimus extended-release capsules). | Day Day of tacrolimus extended-release capsules treatment and PK profiling. | PK Parameters of Tacrolimus Extended-Release Capsules | |||
C max Arithmetic means ± S.D. (ng/mL) | T max Median [range]. (hr) | AUC 24 (ng•hr/mL) | C 24 Tacrolimus trough concentration before the next dose. (ng/mL) | |||
Healthy Subjects (N=24) | 4 mg 4 mg | Day 1 Day 10 | 6.2 ± 2.1 11.6 ± 3.4 | 2 [1 to 5] 2 [1 to 3] | 74 ± 22 155 ± 46 | 2.3 ± 0.8 4.7 ± 1.5 |
Adult Kidney De novo “De novo” refers to immunosuppression starting at the time of transplantation; data from PK substudy of Study 2. (N=17) | 0.2 mg/kg 0.19 mg/kg 0.18 mg/kg 0.18 mg/kg | Day 1 Day 3 Day 7 Day 14 | 26 ± 13.7 31 ± 13.9 32.2 ± 10.2 32.7 ± 9 | 3 [2 to 24] 2 [0.5 to 2] 2 [1 to 6] 2 [1 to 4] | 372 ± 202 437 ± 175 405 ± 117 412 ± 109 | 12.1 ± 7.2 13.5 ± 5.6 11.4 ± 4 11.2 ± 3.9 |
Adult Kidney (6 months or greater post-transplant) (N=60) | 5.2 mg/day Same daily dose of tacrolimus extended-release capsules for 14-day period. | Day 14 | 16.1 ± 5.3 | 2 [1 to 6] | 222 ± 64 | 6.7 ± 1.9 Correlation coefficient of AUC 24 to C min r = 0.88. |
In de novo adult kidney transplant patients, the tacrolimus systemic exposure, as assessed by AUC 24 , for tacrolimus extended-release capsules 0.2 mg/kg once daily on Day 1 post-transplant was 18% (Ratio [SD]: 0.822 [1.647]) lower when compared with Prograf (tacrolimus immediate-release) 0.2 mg/kg/day given twice daily. By Day 3 post-transplant, the AUC 24 was similar between the two formulations. On Day 14 (steady state), the AUC 24 for tacrolimus extended-release capsules was 21% (Ratio [SD]: 1.207 [1.326]) higher than that of Prograf (tacrolimus immediate-release), at comparable trough concentrations (C 24 ).
Due to intersubject variability in tacrolimus PK, individualization of dosing regimen is necessary for optimal therapy [see Dosage and Administration (2.3 , 2.4 )] .
Pharmacokinetic data indicate that whole blood concentrations rather than plasma concentrations serve as the more appropriate sampling compartment to describe tacrolimus PK. Absorption
In healthy subjects, the administration of escalating tacrolimus extended-release capsules doses ranging from 1.5 mg to 10 mg resulted in dose-proportional increases in tacrolimus AUC and C 24h , and no change in elimination half-life.
Food Effects
The presence of a meal affects the absorption of tacrolimus; the rate and extent of absorption is greatest under fasted conditions. In 24 healthy subjects, administration of tacrolimus extended-release capsules immediately following a high-fat meal (150 protein calories, 250 carbohydrate calories, and 500 to 600 fat calories) reduced the C max , AUC t , and AUC inf of tacrolimus by approximately 25% compared with fasting values. Food delayed the median T max from 2 hours in the fasted state to 4 hours in the fed state; however, the terminal half-life remained 36 hours regardless of dosing conditions. The time when a meal is consumed also affected tacrolimus bioavailability. In 24 healthy subjects, when tacrolimus extended-release capsules was administered 1.5 hours after consumption of a high-fat breakfast, tacrolimus exposure was decreased approximately 35%. Administration of tacrolimus extended-release capsules 1 hour prior to a high-fat breakfast reduced tacrolimus exposure by 10%. Tacrolimus extended-release capsules should be taken, preferably on an empty stomach, at least 1 hour before a meal or at least 2 hours after a meal.
Chronopharmacokinetic Effect
In 23 healthy subjects, a diurnal effect on the absorption of tacrolimus was observed. Evening dosing of tacrolimus extended-release capsules reduced AUC inf by 35% relative to morning dosing. Tacrolimus extended-release capsules should be taken consistently at the same time every morning. Distribution
The plasma protein binding of tacrolimus is approximately 99% and is independent of concentration over a range of 5 ng/mL to 50 ng/mL. Tacrolimus is bound mainly to albumin and alpha-1-acid glycoprotein, and has a high level of association with erythrocytes. The distribution of tacrolimus between whole blood and plasma depends on several factors, such as hematocrit, temperature at the time of plasma separation, drug concentration, and plasma protein concentration. In a U.S. trial in which tacrolimus was administered as tacrolimus immediate-release, the ratio of whole blood concentration to plasma concentration averaged 35 (range 12 to 67).
Elimination
Metabolism
The desired pharmacological activity of tacrolimus is primarily due to the parent drug. Tacrolimus is extensively metabolized by the mixed-function oxidase system, primarily the cytochrome P-450 system (CYP3A4 and CYP3A5). A metabolic pathway leading to the formation of 8 possible metabolites has been proposed. Demethylation and hydroxylation were identified as the primary mechanisms of biotransformation in vitro . The major metabolite identified in incubations with human liver microsomes is 13-demethyl tacrolimus. In in vitro studies, a 31-demethyl metabolite has been reported to have the same activity as tacrolimus.
Excretion
In a mass balance study of orally-administered radiolabeled tacrolimus to 6 healthy subjects, the mean recovery of the radiolabel was 94.9 ± 30.7%. Fecal elimination accounted for 92.6 ± 30.7% and urinary elimination accounted for 2.3 ± 1.1% of the total radiolabel administered. The elimination half-life based on radioactivity was 31.9 ± 10.5 hours, whereas it was 48.4 ± 12.3 hours based on tacrolimus concentrations. The mean clearance of radiolabel was 0.226 ± 0.116 L/hr/kg and the mean clearance of tacrolimus was 0.172 ± 0.088 L/hr/kg.
The elimination half-life of tacrolimus after oral administration of 4 mg tacrolimus extended-release capsules daily for 10 days was 38 ± 3 hours in 24 healthy subjects.
Specific Populations
Pediatric Patients
Pediatric use information is approved for Astellas Pharma US, Inc.’s ASTAGRAF XL (tacrolimus extended-release capsules). However, due to Astellas Pharma US, Inc.’s marketing exclusivity rights, this drug product is not labeled with that information.
Patients with Renal Impairment
Tacrolimus pharmacokinetics following a single administration of tacrolimus immediate-release injection (administered as a continuous IV infusion) were determined in 12 patients (7 not on dialysis and 5 on dialysis, serum creatinine of 3.9 ± 1.6 and 12 ± 2.4 mg/dL, respectively) prior to their kidney transplant. The mean clearance of tacrolimus in patients with renal dysfunction given tacrolimus IV was similar to that in healthy subjects given tacrolimus IV and in healthy subjects given oral tacrolimus immediate-release [see Use in Specific Populations (8.6 )] .
Patients with Hepatic Impairment
Tacrolimus pharmacokinetics have been determined in six patients with mild hepatic impairment (mean Child-Pugh score: 6.2) following single oral administration of tacrolimus immediate-release. The mean clearance of tacrolimus in patients with mild hepatic impairment was not substantially different from that in healthy subjects. Tacrolimus pharmacokinetics were studied in six patients with severe hepatic impairment (mean Child-Pugh score: more than 10). The mean clearance was substantially lower in patients with severe hepatic impairment [see Dosage and Administration (2.3 ) and Use in Specific Populations (8.7 )].
Racial or Ethnic Groups
The pharmacokinetics of tacrolimus was studied following single oral administration of tacrolimus immediate-release (5 mg) in 10 African-American, 12 Latino-American, and 12 Caucasian healthy subjects [see Dosage and Administration (2.2 ), Use in Specific Populations (8.8 ) and Clinical Studies (14 )]:
- The mean (± SD) tacrolimus C max in African-Americans (23.6 ± 12.1 ng/mL) was lower than in Caucasians (40.2 ± 12.6 ng/mL) and Latino-Americans (36.2 ± 15.8 ng/mL).
- Mean AUC 0-inf tended to be lower in African-Americans (203 ± 115 ng∙hr/mL) than Caucasians (344 ± 186 ng∙hr/mL) and Latino-Americans (274 ± 150 ng∙hr/mL).
- The mean (± SD) absolute oral bioavailability (F) in African-Americans (12 ± 4.5%) and Latino-Americans (14 ± 7.4%) was lower than in Caucasians (19 ± 5.8%).
- There was no significant difference in mean terminal half-life among the three ethnic groups (range from approximately 25 to 30 hours).
Male and Female Patients
A formal trial to evaluate the effect of gender on tacrolimus pharmacokinetics has not been conducted; however, there was no difference in total mg daily dosages between male and female patients receiving tacrolimus extended-release capsules in the kidney transplant trials. A retrospective comparison of pharmacokinetics in healthy subjects, and in kidney transplant patients indicated no gender-based differences.
Drug Interaction Studies
Because tacrolimus is metabolized mainly by CYP3A enzymes, drugs or substances known to inhibit these enzymes and/or are known CYP3A substrates may increase tacrolimus whole blood concentrations. Drugs known to induce CYP3A enzymes may decrease tacrolimus whole blood concentrations [see Warnings and Precautions (5.10 ) and Drug Interactions (7.2 )] .
Figure 1 and Figure 2 summarize the PK data from drug interaction studies of tacrolimus extended-release capsules or tacrolimus immediate-release capsules. These studies assessed the effect of co-administered drugs on tacrolimus PK in healthy subjects. Dosing adjustments, when using drugs that inhibit or increase CYP3A enzymes, may be necessary [see Drug Interactions (7.2 )] .
Figure 1: Effect of Co-administered Drugs on the Pharmacokinetics of Tacrolimus (when Given as Tacrolimus Extended-Release Capsules)
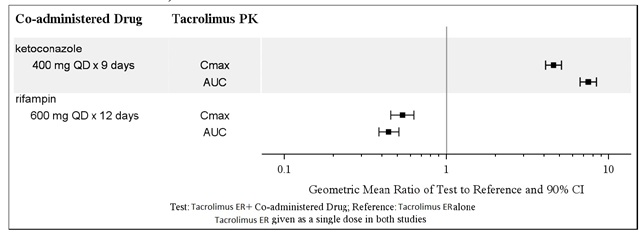
Figure 2: Effect of Co-administered Drugs on the Pharmacokinetics of Tacrolimus (when Given as Immediate-Release Tacrolimus)
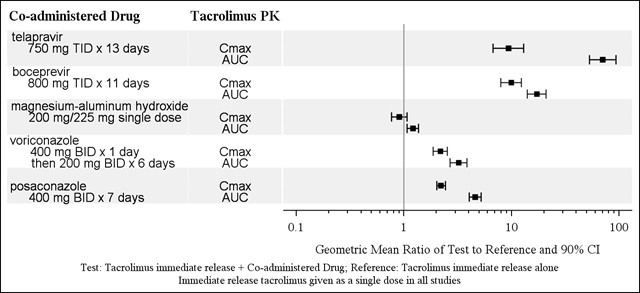
Other Drug Interaction Studies
- Caspofungin (see complete prescribing information for CANCIDAS): Caspofungin reduced the blood AUC 0-12 of tacrolimus by approximately 20%, peak blood concentration (C max ) by 16%, and 12-hour blood concentration (C 12hr ) by 26% in healthy adult subjects when tacrolimus (2 doses of 0.1 mg/kg 12 hours apart) was administered on the 10th day of CANCIDAS 70 mg daily, as compared to results from a control period in which tacrolimus was administered alone [see Drug Interactions (7.2) ] . The mechanism of interaction has not been confirmed.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Carcinogenicity studies were conducted in male and female rats and mice. In the 80-week mouse oral study and in the 104-week rat oral study, no relationship of tumor incidence to tacrolimus dosage was found. The highest dose used in the mouse was 3 mg/kg/day (0.49 times the AUC at the maximum clinical dose of 0.2 mg/kg/day) and in the rat was 5 mg/kg/day (0.14 times the AUC at the maximum clinical dose of 0.2 mg/kg/day) [see Warnings and Precautions (5.1 )] .
A 104-week dermal carcinogenicity study was performed in mice with tacrolimus ointment (0.03% to 3%), equivalent to tacrolimus doses of 1.1mg/kg/day to 118 mg/kg/day or 3.3 mg/m 2 /day to 354 mg/m 2 /day. In the study, the incidence of skin tumors was minimal and the topical application of tacrolimus was not associated with skin tumor formation under ambient room lighting. However, a statistically significant elevation in the incidence of pleomorphic lymphoma in high-dose male (25/50) and female animals (27/50), and in the incidence of undifferentiated lymphoma in high-dose female animals (13/50), was noted in the mouse dermal carcinogenicity study. Lymphomas were noted in the mouse dermal carcinogenicity study at a daily dose of 3.5 mg/kg (0.1% tacrolimus ointment; 2.4-fold the human exposure in stable adult kidney transplant patients more than 6 months post-transplant). No drug-related tumors were noted in the mouse dermal carcinogenicity study at a daily dose of 1.1 mg/kg (0.03% tacrolimus ointment). The relevance of topical administration of tacrolimus in the setting of systemic tacrolimus use is unknown.
The implications of these carcinogenicity studies are limited; doses of tacrolimus were administered that likely induced immunosuppression in these animals, impairing their immune system’s ability to inhibit unrelated carcinogenesis.
Mutagenesis
No evidence of genotoxicity was seen in bacterial ( Salmonella and E. coli ) or mammalian (Chinese hamster lung-derived cells) in vitro assays of mutagenicity, the in vitro CHO/HGPRT assay of mutagenicity, or in vivo clastogenicity assays performed in mice; tacrolimus did not cause unscheduled DNA synthesis in rodent hepatocytes.
Impairment of Fertility
Tacrolimus subcutaneously administered to male rats at paternally toxic doses of 2 mg/kg/day [1.6 times the maximum recommended clinical dose (0.2 mg/kg/day) on a mg/m 2 basis] or 3 mg/kg/day (2.4 times the maximum recommended clinical dose) resulted in a dose-related decrease in sperm count.
Tacrolimus administered orally at 1 mg/kg (0.8 times the maximum clinical dose) to male and female rats, prior to and during mating, as well as to dams during gestation and lactation, was associated with embryolethality and adverse effects on female reproduction. Effects on female reproductive function (parturition) and embryolethal effects were indicated by a higher rate of pre- and post-implantation loss and increased numbers of undelivered and nonviable pups. When administered at 3.2 mg/kg (2.6 times the maximum clinical dose range based on body surface area), tacrolimus was associated with maternal and paternal toxicity as well as reproductive toxicity including marked adverse effects on estrus cycles, parturition, pup viability, and pup malformations.
CLINICAL STUDIES
14.1 Tacrolimus Extended-Release Capsules with Basiliximab Induction
Study 1 was a 12-month, randomized, open-label trial of tacrolimus extended-release capsules (N=214) compared to active-control of tacrolimus (Prograf) immediate-release (N=212), conducted primarily in the U.S. in patients who were a recipient of a primary or retransplanted non-HLA-identical living or deceased donor kidney transplant. All patients received basiliximab induction and concomitant mycophenolate mofetil (MMF) and corticosteroids. The study population was 17 to 77 years of age, the mean age was 48 years; 64% were male and 36% were female; 73% were Caucasian, 22% were African-American, 2% were Asian, and 3% were categorized as other races. Living donors provided 49% of the organs and 51% of patients received a kidney transplant from a deceased donor with a mean cold ischemia time of 19 hours. The most frequent diseases leading to transplantation were balanced between the groups and included nephrosclerosis/hypertensive nephropathy, diabetic nephropathy, glomerulonephritis, and polycystic kidney disease. In the study, 97% of patients had no previous transplant and 3% had a previous transplant.
Study Medications
Tacrolimus Extended-Release Capsules or Control [Prograf (tacrolimus) capsules]
The initial dose of tacrolimus extended-release capsules was administered prior to reperfusion or within 48 hours after completion of the transplant procedure. The protocol-defined initial post-operative daily doses were 0.15 to 0.2 mg per kg given as a single dose in the morning for tacrolimus extended-release capsules and 0.075 to 0.1 mg per kg twice daily for control. The tacrolimus extended-release capsules and control dosage was then adjusted on the basis of safety and efficacy and a target whole blood tacrolimus trough concentration range of 7 ng/mL to 16 ng/mL for the first 90 days post-transplant and 5 ng/mL to 15 ng/mL thereafter.
The average recorded starting tacrolimus daily dose, given any time up to day 2 post-transplant, was higher for tacrolimus extended-release capsules than for control (0.14 mg per kg per day versus 0.1 mg per kg per day). Thereafter, to achieve comparable mean tacrolimus trough concentrations, on average 15% higher total mean daily doses of tacrolimus were required for tacrolimus extended-release capsules than for control.
Tacrolimus whole blood trough concentrations were monitored on Day 3, Day 7, Day 10, Day 14, and Day 21, then Month 1, Month 2, Month 4, Month 6, Month 8, Month 10, and Month 12. Table 10 shows the tacrolimus whole blood trough concentrations measured at protocol-specified time points for tacrolimus extended-release capsules. Approximately 80% of tacrolimus extended-release capsules-treated patients maintained tacrolimus whole trough blood concentrations between 5 ng/mL to 17 ng/mL during Month 1 through Month 2 and between 4 ng/mL to 12 ng/mL from Month 3 through Month 12.
Scheduled Visit | Tacrolimus Whole Blood Trough Concentrations (ng/mL) Immunoassay was used in most laboratories. [Median (10 th to 90 th Percentile)] |
Day 3 | 9.6 (4.9 to 20.2) |
Day 7 | 9.1 (4.4 to 16.8) |
Day 14 | 10 (5.7 to 16.9) |
Month 1 | 10.5 (5.6 to 17.1) |
Month 2 | 9.4 (6.1 to 14.2) |
Month 6 | 7.7 (4.4 to 11.5) |
Month 12 | 7.2 (3.8 to 10.4) |
African-American patients required higher tacrolimus extended-release capsules dosages to attain similar trough concentrations as Caucasian patients (see Table 11 ).
Time After Transplant | Caucasian Patients N=160 | African-American Patients N=41 | ||
Dose (mg/kg) | Mean Trough Concentration (ng/mL) | Dose (mg/kg) | Mean Trough Concentration (ng/mL) | |
Day 7 | 0.14 | 10.65 | 0.14 | 7.78 |
Month 1 | 0.14 | 11.11 | 0.17 | 10.92 |
Month 6 | 0.1 | 7.95 | 0.13 | 8.42 |
Month 12 | 0.09 | 7.53 | 0.12 | 7.33 |
MMF
The initial dose of MMF was 1 gram administered orally or intravenously prior to or within 48 hours of completion of the transplant procedure. Subsequent MMF was administered orally 1 gram twice daily or up to 1.5 grams twice daily in African-American patients. Dose-equivalent three times daily or four times daily dosing was permitted if MMF tolerability was a concern.
The MMF dosages administered by time period in tacrolimus extended-release capsules-treated patients are shown in Table 12 . The MMF dosage was reduced to less than 2 grams per day by month 12 in 56% of tacrolimus extended-release capsules-treated patients. Approximately 57% of the MMF dose reductions were because of adverse reactions in the tacrolimus extended-release capsules group [see Adverse Reactions (6.1 )] .
Time period (Days) | Patients on MMF | Time-averaged MMF dosage Time-averaged MMF dosage is the total MMF dosage per day divided by the duration of treatment. A time-averaged MMF dosage of 2 grams per day means that the MMF dosage was not reduced in those patients during the time period. | ||
N | Less than 2 grams per day | 2 grams per day | Greater than 2 grams per day | |
1 to 30 | 211 | 30% | 64% | 6% |
31 to 90 | 208 | 38% | 57% | 5% |
91 to 180 | 205 | 49% | 48% | 3% |
181 to 365 | 201 | 51% | 47% | 3% |
Basiliximab Induction
All patients were administered 2 doses of basiliximab induction therapy (20 mg intravenously) with the first dose on Day 0 before skin closure and the second dose between Day 3 and Day 5.
Steroids
All patients were administered an intravenous bolus of 500 to 1,000 mg of methylprednisolone (or an equivalent steroid dose) on Day 0 followed by oral administration of 200 mg methylprednisolone (or an equivalent dose of steroid) on Day 1 and subsequent tapering to achieve a targeted mean prednisone dose of 5 to 10 mg/day after the first 3 months.
Efficacy Results
The efficacy failure rate, defined as the percentage of patients with biopsy-proven acute rejection (BPAR), graft failure, death, and/or lost to follow at 12 months, is shown in Table 13 for the intent-to-treat population, as well as the rates of the individual events.
Tacrolimus extended-release capsules + MMF, steroids, basiliximab induction (N=214) | Prograf + MMF, steroids, basiliximab induction (N=212) | |
Efficacy Failure | 30 (14%) | 32 (15.1%) |
Treatment Difference (95% CI 95% confidence interval calculated using normal approximation. ) | -1.1% (-7.8%, +5.6%) | |
Efficacy Failure Endpoints | ||
Biopsy-Proven Acute Rejection | 22 (10.3%) | 16 (7.5%) |
Graft Loss | 5 (2.3%) | 9 (4.2%) |
Death | 3 (1.4%) | 9 (4.2%) |
Lost to follow-up | 3 (1.4%) | 4 (1.9%) |
Glomerular Filtration Rate
The estimated mean glomerular filtration rates, using the Modification of Diet in Renal Disease (MDRD) formula, by treatment group at Month 12 in the intent-to-treat population is shown in Table 14 .
Tacrolimus extended-release capsules + MMF, steroids, basiliximab induction (N=201) | Prograf + MMF, steroids, basiliximab induction (N=202) | |
Month 1 Baseline Mean (SD) Month 12 LOCF Last observation carried forward (LOCF); patients who died, lost the graft, or were lost to follow-up are imputed as zeroes. Mean (Standard deviation) Mean Difference Tacrolimus Extended-Release Capsules minus Prograf (tacrolimus immediate-release) Results from analysis of covariance model with Month 1 baseline as a covariate. | 56 (20) 58 (21) +2.3 (-1.2, +5.8) | 56 (21) 56 (23) |
Clinical Study of Tacrolimus Extended-Release Capsules without Induction
Study 2 was a 12-month, randomized, double-blind trial of tacrolimus extended-release capsules (N=331) compared to active control of tacrolimus (Prograf) immediate-release (N=336), in non-U.S. patients who received a primary or retransplanted non-HLA-identical living or deceased donor kidney transplant. This trial was designed to remain double-blind until the last patient enrolled had completed 24 weeks on study treatment. Patients with a high immunologic risk defined as a panel reactive antibody (PRA) grade more than 50% in the previous 6 months and/or with a previous graft survival of less than 12 months due to immunologic reasons were excluded, as were patients of donor kidneys with cold ischemia time more than 30 hours, or donor kidneys from a non heart-beating donor. The patient treatment assignments remained blinded for 12 months for 96% of the patients participating in the trial.
All patients received concomitant MMF and corticosteroids without induction. The population was 18 to 65 years of age; the mean age was 48 years; 63% of the study population was male; 82% were Caucasian, 5% were African-American, 2% were Asian, and 11% were categorized as other races. Living donors provided 27% of the organs and 73% of patients received a kidney transplant from a deceased donor with a mean cold ischemia time of 17 hours. The most frequent diseases leading to transplantation were balanced between the groups and included nephrosclerosis/hypertensive nephropathy, diabetic nephropathy, glomerulonephritis, and polycystic kidney disease.
Study Medication
Tacrolimus Extended-Release Capsules or Control [Prograf (tacrolimus) capsules]
The protocol-specified initial preoperative dose for both tacrolimus extended-release capsules and control was 0.1 mg per kg given orally in one dose within 12 hours prior to reperfusion, given at any time of the day. The initial post-operative tacrolimus daily dose (0.2 mg per kg per day) was given orally in one dose, preferably in the morning for tacrolimus extended-release capsules, and was given as 0.1 mg/kg twice daily for control. Subsequent doses of tacrolimus extended-release capsules and control were adjusted on the basis of clinical evidence of efficacy, occurrence of adverse events and according to whole blood tacrolimus trough concentration target ranges of 10 ng/mL to 15 ng/mL for the first 28 days post-transplant, 5 ng/mL to 15 ng/mL from Day 29 to Day 168, 5 ng/mL to 10 ng/mL thereafter.
The actual tacrolimus doses on Day 0 (0.1 mg per kg per day preoperative) and Day 1 (0.2 mg per kg per day post-operative) were comparable between tacrolimus extended-release capsules and control. Thereafter, to achieve comparable mean tacrolimus trough concentrations, on average, 25% higher total mean daily doses of tacrolimus were required for tacrolimus extended-release capsules than for control.
Tacrolimus whole blood trough concentrations were monitored on Day 1, Day 3, Day 7, Day 14, then Month 1, Month 2, Month 3, Month 6, Month 11, Month 12, and then every 3 months.
Table 15 shows the tacrolimus whole blood trough concentrations measured at protocol-specified time points for tacrolimus extended-release capsules. Approximately 80% of tacrolimus extended-release capsules-treated patients maintained tacrolimus whole trough blood concentrations between 6 ng/mL to 20 ng/mL during Month 1 through Month 2, and between 6 ng/mL to 14 ng/mL from Month 3 through Month 12.
Scheduled Visit | Tacrolimus Whole Blood Trough Concentrations (ng/mL) Immunoassay was used in most laboratories. [Median (10 th to 90 th Percentile)] |
Day 3 | 13.8 (6.5 to 25.5) |
Day 7 | 10.1 (5.5 to 17.3) |
Day 14 | 10.8 (6.7 to 17.9) |
Month 1 | 12 (7.5 to 17.6) |
Month 2 | 11.1 (6.6 to 17.3) |
Month 6 | 9.2 (5.7 to 13.5) |
Month 12 | 8 (5.1 to 13.8) |
MMF
The initial dose of MMF was 1 gram orally twice daily starting preoperatively and given for the first 14 days of the study. Thereafter the MMF dose was reduced to 0.5 grams twice daily to be maintained throughout the study.
The MMF dosages administered by time period in tacrolimus extended-release capsules-treated patients are shown in Table 16 . The MMF dosage was reduced to 0.5 grams twice daily starting after Day 14 in the majority of patients.
Time period (Days) | Patients on MMF | Time-averaged MMF dosage Time-averaged MMF dosage is the total MMF dosage per day divided by the duration of treatment. A time-averaged MMF dosage of 2 grams per day means that the MMF dosage was not reduced in those patients during the time period. , One patient had a time-averaged dose during the first and last period of more than 2 gram/day. | ||
N | Less than 1 gram per day | 1 gram to less than 2 grams per day | 2 grams per day | |
1 to 30 | 331 | 1% | 78% | 21% |
31 to 90 | 303 | 8% | 87% | 6% |
91 to 180 | 281 | 12% | 85% | 3% |
181 to 365 | 258 | 15% | 83% | 2% |
Steroids
An intravenous (IV) bolus of up to 1,000 mg methylprednisolone (or equivalent) was administered perioperatively (Day 0) with a second IV bolus of 125 mg being administered 1 day after reperfusion (Day 1). On Day 2, oral prednisone was started at 20 mg per day. Thereafter, the dose of oral prednisone (or equivalent) was tapered to a dose of 0 to 5 mg/day.
No Antibody Induction
Antibody induction therapy was not allowed.
Efficacy Results
The efficacy failure rate, defined as the percentage of patients with biopsy-proven acute rejection (BPAR), graft failure, death, and/or lost to follow at 12 months, is shown in Table 17 for the intent-to-treat population, as well as the rates of the individual events. About 1% of randomized patients were not transplanted and were not included in the ITT analysis.
Tacrolimus extended-release capsules + MMF and steroids (N=331) | Prograf + MMF and steroids (N=336) | |
Efficacy Failure | 93 (28.1%) | 78 (23.2%) |
Treatment Difference (95% CI 95% confidence interval calculated using normal approximation. ) | +4.9% (-1.7%, +11.5%) | |
Efficacy Failure Endpoints | ||
Biopsy-Proven Acute Rejection | 68 (20.5%) | 54 (16.1%) |
Graft loss | 28 (8.5%) | 24 (7.1%) |
Death | 10 (3%) | 8 (2.4%) |
Lost to follow-up | 4 (1.2%) | 7 (2.1%) |
Glomerular Filtration Rate
The estimated mean glomerular filtration rates, using the Modification of Diet in Renal Disease (MDRD) formula, by treatment group at Month 12 in the intent-to-treat population in Study 2 is shown in Table 18 .
Tacrolimus extended-release capsules + MMF and steroids (N=287) | Prograf + MMF and steroids (N=300) | |
Month 1 Baseline Mean (SD) Month 12 LOCF Last observation carried forward (LOCF); patients who died, lost the graft or were lost to follow-up are imputed as zeroes. Mean (Standard deviation) Mean Difference Tacrolimus Extended-Release Capsules minus Prograf (tacrolimus immediate-release) Results from analysis of covariance model with Month 1 baseline as a covariate. | 51 (19) 52 (20) -1.8 (-4.6, +0.8) | 52 (20) 55 (19) |
HOW SUPPLIED/STORAGE AND HANDLING
Tacrolimus extended-release capsules are supplied as listed in Table 19 .
0.5 mg | Oblong capsule with opaque yellowish pink cap and opaque light orange body. Capsule is branded with dull red “SD-TC” on capsule body and dull red “0.5 mg” on the capsule cap.
|
1 mg | Oblong capsule with opaque light yellow cap and opaque light orange body. Capsule is branded with dull red “SD-TC” on capsule body and dull red “1 mg” on the capsule cap.
|
5 mg | Oblong capsule with an opaque red-orange cap and opaque orange body. Capsule is branded with dull red “SD-TC” on capsule body and dull red “5 mg” on the capsule cap.
|
Store and Dispense
Store at 25°C (77°F); excursions permitted from 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature].
Mechanism of Action
Tacrolimus binds to an intracellular protein, FKBP-12. A complex of tacrolimus-FKBP-12, calcium, calmodulin, and calcineurin (a ubiquitous mammalian intracellular enzyme) is then formed and the phosphatase activity of calcineurin is inhibited. Such inhibition prevents the dephosphorylation and translocation of various factors such as the nuclear factor of activated T-cells (NF-AT), and nuclear factor kappa-light-chain-enhancer of activated B-cells (NF-κB).
Tacrolimus inhibits the expression and/or production of several cytokines that include interleukin (IL)-1 beta, IL‑2, IL-3, IL-4, IL-5, IL-6, IL-8, IL-10, gamma interferon, tumor necrosis factor-alpha, and granulocyte macrophage colony-stimulating factor. Tacrolimus also inhibits IL-2 receptor expression and nitric oxide release, induces apoptosis and production of transforming growth factor-beta that can lead to immunosuppressive activity. The net result is the inhibition of T-lymphocyte activation and proliferation as well as T-helper-cell-dependent B-cell response (i.e., immunosuppression).
Tacrolimus - Tacrolimus Extended - Release Capsules capsule, Coated, Extended Release PubMed™ news
- Journal Article • 2026 MayIatrogenic Immunodeficiency-associated Polymorphic Lymphoproliferative Disorder Resulting in Complete Remission After Tacrolimus Withdrawal in Systemic Lupus Erythematosus: A Case Report.
- Journal Article • 2026 MayPatient-centric capillary dried blood spot sampling for tacrolimus and creatinine monitoring in clinical practice.
- Journal Article • 2026 MayEfficacy and Safety of a Tacrolimus Lipid Suspension Enema in Mild-to-Moderate Ulcerative Colitis: A Multicenter, Prospective, Double-Blind, Phase II Randomized Controlled Trial.
- Journal Article • 2026 MayEvaluation of Ease of Use for Pediatric Medications Requiring Decapsulation, Dissolution, or Partial Dosing: A Questionnaire-Based Study in Japan.
- Journal Article • 2026 MayIntraocular Pressure During Short-Term Topical or Systemic Corticosteroid Treatment: Analysis of 3 Randomized Clinical Trials.