Get your patient on Tazarotene - Tazarotene cream (Tazarotene)
Tazarotene - Tazarotene cream prescribing information
INDICATIONS AND USAGE
Plaque Psoriasis
Tazarotene cream, 0.1% is indicated for the topical treatment of patients with plaque psoriasis.
Acne Vulgaris
Tazarotene cream, 0.1% is also indicated for the topical treatment of patients with acne vulgaris.
DOSAGE AND ADMINISTRATION
Important Administration Instructions
Tazarotene cream is for topical use only. Tazarotene cream is not for ophthalmic, oral, or intravaginal use. If contact with mucous membranes occurs, rinse thoroughly with water [see Warnings and Precautions (5.2) ] . Wash hands thoroughly after application.
Psoriasis
It is recommended that treatment starts with tazarotene cream, 0.05%, with strength increased to 0.1% if tolerated and medically indicated. Apply a thin film (2 mg/cm 2 ) of tazarotene cream once per day, in the evening, to cover only the psoriatic lesions. If a bath or shower is taken prior to application, the skin should be dry before applying the cream. If emollients are used, they should be applied at least an hour before application of tazarotene cream. Because unaffected skin may be more susceptible to irritation, application of tazarotene cream to these areas should be carefully avoided.
Acne
Cleanse the face gently. After the skin is dry, apply a thin layer (2 mg/cm 2 ) of tazarotene cream 0.1% once per day, in the evening, to the skin areas where acne lesions appear. Use enough to cover the entire affected area.
Use effective sunscreens and wear protective clothing while using tazarotene cream [see Warnings and Precautions (5.3) ].
DOSAGE FORMS AND STRENGTHS
Cream, 0.1%. Each gram of tazarotene cream, 0.1% contains 1 mg of tazarotene in a white cream base.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary
Based on data from animal reproduction studies, retinoid pharmacology, and the potential for systemic absorption, tazarotene cream may cause fetal harm when administered to a pregnant female and is contraindicated during pregnancy. Safety in pregnant females has not been established. The potential risk to the fetus outweighs the potential benefit to the mother from tazarotene cream during pregnancy; therefore, tazarotene cream should be discontinued as soon as pregnancy is recognized [see Contraindications (4) , Warnings and Precautions (5.1) , Clinical Pharmacology (12.3) ]. Limited case reports of pregnancy in females enrolled in clinical trials for tazarotene cream have not established a clear association with tazarotene and major birth defects or miscarriage risk. Because the exact timing and extent of exposure in relation to the gestational age are not certain, the significance of these findings is unknown.
In animal reproduction studies with pregnant rats, tazarotene dosed topically during organogenesis at 2 times the maximum systemic exposure in subjects treated with the maximum recommended human dose (MRHD) of tazarotene cream, 0.1% resulted in reduced fetal body weights and reduced skeletal ossification. In animal reproduction studies with pregnant rabbits dosed topically with tazarotene gel at 26 times the maximum systemic exposure in subjects treated with the MRHD of tazarotene cream, 0.1%, there was a single incident of known retinoid malformations, including spina bifida, hydrocephaly, and heart anomalies.
In animal reproduction studies with pregnant rats and rabbits, tazarotene dosed orally during organogenesis at 2 and 52 times, respectively, the maximum systemic exposure in subjects treated with the MRHD of tazarotene cream, 0.1% resulted in malformations, fetal toxicity, developmental delays, and/or behavioral delays. In pregnant rats, tazarotene dosed orally prior to mating through early gestation resulted in decreased litter size, decreased numbers of live fetuses, decreased fetal body weights, and increased malformations at doses approximately 7 times higher than the maximum systemic exposure in subjects treated with the MRHD of tazarotene cream, 0.1% [see Data ] .
The background risk of major birth defects and miscarriage for the indicated population is unknown. Adverse outcomes in pregnancy occur regardless of the health of the mother or the use of medications. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Data
Animal Data
In rats, a tazarotene gel, 0.05% formulation dosed topically during gestation days 6 through 17 at 0.25 mg/kg/day, which represented 2 times the maximum systemic exposure in subjects treated with the MRHD of tazarotene cream, 0.1% (i.e., 2 mg/cm 2 over a 15% body surface area), resulted in reduced fetal body weights and reduced skeletal ossification. Rabbits dosed topically with 0.25 mg/kg/day tazarotene gel, which represented 26 times the maximum systemic exposure in subjects treated with MRHD of tazarotene cream, 0.1%, during gestation days 6 through 18, had a single incident of known retinoid malformations, including spina bifida, hydrocephaly, and heart anomalies.
When tazarotene was given orally to animals, developmental delays were seen in rats, and malformations and post-implantation loss were observed in rats and rabbits at doses representing 2 and 52 times, respectively, the maximum systemic exposure seen in subjects treated with the MRHD of tazarotene cream, 0.1%.
In female rats orally administered 2 mg/kg/day of tazarotene from 15 days before mating through gestation day 7, which represented 7 times the maximum systemic exposure in subjects treated with the MRHD of tazarotene cream, 0.1%, classic developmental effects of retinoids were observed including decreased number of implantation sites, decreased litter size, decreased numbers of live fetuses, and decreased fetal body weights. A low incidence of retinoid-related malformations was observed at that dose.
In a pre-and postnatal development toxicity study, topical administration of tazarotene gel (0.125 mg/kg/day) to pregnant female rats from gestation day 16 through lactation day 20 reduced pup survival, but did not affect the reproductive capacity of the offspring. Based on data from another study, the maximum systemic exposure in the rat would be equivalent to the maximum systemic exposure in subjects treated with the MRHD of tazarotene cream, 0.1%.
Lactation
Risk Summary
There is no information regarding the presence of tazarotene in human milk, the effects on the breastfed infant, or the effects on milk production. After single topical doses of 14 C-tazarotene gel to the skin of lactating rats, radioactivity was detected in rat milk. The lack of clinical data during lactation precludes a clear determination of the risk of tazarotene cream to an infant during lactation; therefore, the developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for tazarotene cream and any potential adverse effects on the breastfed child from tazarotene cream or from the underlying maternal condition.
Females and Males of Reproductive Potential
Pregnancy Testing
Pregnancy testing is recommended for females of reproductive potential within 2 weeks prior to initiating tazarotene cream therapy which should begin during a menstrual period.
Contraception
Females
Based on animal studies, tazarotene cream may cause fetal harm when administered to a pregnant woman [see Use in Specific Populations (8.1) ]. Advise females of reproductive potential to use effective contraception during treatment with tazarotene cream.
Pediatric Use
The safety and efficacy of tazarotene cream have not been established in patients with psoriasis under the age of 18 years, or in patients with acne under the age of 12 years.
Geriatric Use
Tazarotene cream for the treatment of acne has not been clinically tested in persons 65 years of age or older.
Of the total number of subjects in clinical trials of tazarotene cream for plaque psoriasis, 120 were over the age of 65. No overall differences in safety or effectiveness were observed between these subjects and younger subjects. Currently there is no other clinical experience on the differences in responses between the elderly and younger subjects, but greater sensitivity of some older individuals cannot be ruled out.
CONTRAINDICATIONS
Tazarotene cream is contraindicated in:
- Pregnancy. Retinoids may cause fetal harm when administered to a pregnant female [see Warnings and Precautions (5.1) , Use in Specific Populations (8.1 , 8.3) ] .
- Individuals who have known hypersensitivity to any of its components [see Warnings and Precautions (5.2) ].
WARNINGS AND PRECAUTIONS
- Embryofetal Toxicity: Tazarotene cream contains tazarotene, which is a teratogenic substance. Tazarotene cream is contraindicated in pregnancy. Females of child-bearing potential should have a negative pregnancy test within 2 weeks prior to initiating treatment and use an effective method of contraception during treatment. (5.1 )
- Local Irritation: Some individuals may experience excessive pruritus, burning, skin redness or peeling. If these effects occur, discontinue until the integrity of the skin has been restored, or reduce dosing interval, or in the case of psoriasis, may switch to the lower concentration. Tazarotene cream should not be used on eczematous skin, as it may cause severe irritation. (5.2 )
- Photosensitivity and Risk for Sunburn: Avoid exposure to sunlight, sunlamps, and weather extremes. Wear sunscreen daily. Tazarotene cream should be administered with caution if the patient is also taking drugs known to be photosensitizers. (5.3 )
Embryofetal Toxicity
Systemic exposure to tazarotenic acid is dependent upon the extent of the body surface area treated. In patients treated topically over sufficient body surface area, exposure could be in the same order of magnitude as in orally treated animals. Although there may be less systemic exposure in the treatment of acne of the face alone due to less surface area for application, tazarotene is a teratogenic substance, and it is not known what level of exposure is required for teratogenicity in humans [see Clinical Pharmacology (12.3) ] .
There were thirteen reported pregnancies in subjects who participated in the clinical trials for topical tazarotene. Nine of the subjects were found to have been treated with topical tazarotene, and the other four had been treated with vehicle. One of the subjects who was treated with tazarotene cream elected to terminate the pregnancy for non-medical reasons unrelated to treatment. The other eight pregnant women who were inadvertently exposed to topical tazarotene during clinical trials subsequently delivered apparently healthy babies. As the exact timing and extent of exposure in relation to the gestation times are not certain, the significance of these findings is unknown.
Females of Child-bearing Potential
Females of child-bearing potential should be warned of the potential risk and use adequate birth-control measures when tazarotene cream is used. The possibility that a female of child-bearing potential is pregnant at the time of institution of therapy should be considered.
A negative result for pregnancy test should be obtained within 2 weeks prior to tazarotene cream therapy. Tazarotene cream therapy should begin during a menstrual period [see Use in Specific Populations (8.1) ] .
Local Irritation and Hypersensitivity Reactions
Local tolerability reactions (including blistering and skin desquamation) and hypersensitivity adverse reactions (including urticaria) have been observed with topical tazarotene. Application of tazarotene cream may cause excessive irritation in the skin of certain sensitive individuals. Some individuals may experience excessive pruritus, burning, skin redness or peeling. If these effects occur, the medication should either be discontinued until the integrity of the skin is restored, or the dosing should be reduced to an interval the patient can tolerate. However, efficacy at reduced frequency of application has not been established. Alternatively, patients with psoriasis who are being treated with the 0.1% concentration can be switched to the lower concentration. Frequency of application should be closely monitored by careful observation of the clinical therapeutic response and skin tolerance. Therapy can be resumed, or the drug concentration or frequency of application can be increased as the patient becomes able to tolerate treatment.
Concomitant topical medications and cosmetics that have a strong drying effect should be avoided. It is also advisable to "rest" a patient's skin until the effects of such preparations subside before use of tazarotene cream is begun.
Tazarotene cream should not be used on eczematous skin, as it may cause severe irritation.
Weather extremes, such as wind or cold, may be more irritating to patients using tazarotene cream.
Photosensitivity and Risk for Sunburn
Because of heightened burning susceptibility, exposure to sunlight (including sunlamps) should be avoided unless deemed medically necessary, and in such cases, exposure should be minimized during the use of tazarotene cream. Patients must be warned to use sunscreens and protective clothing when using tazarotene cream. Patients with sunburn should be advised not to use tazarotene cream until fully recovered. Patients who may have considerable sun exposure due to their occupation and those patients with inherent sensitivity to sunlight should exercise particular caution when using tazarotene cream.
Tazarotene cream should be administered with caution if the patient is also taking drugs known to be photosensitizers (e.g., thiazides, tetracyclines, fluoroquinolones, phenothiazines, sulfonamides) because of the increased possibility of augmented photosensitivity.
ADVERSE REACTIONS
The following serious adverse reactions are discussed in more detail in other sections of the labeling:
- Embryofetal toxicity [see Warnings and Precautions (5.1) ]
- Photosensitivity and Risk of Sunburn [see Warnings and Precautions (5.3) ]
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice. In human dermal safety trials, tazarotene cream, 0.05% and 0.1% did not induce allergic contact sensitization, phototoxicity, or photoallergy.
Psoriasis
The most frequent adverse reactions reported with tazarotene cream, 0.05% and 0.1% occurring in 10 to 23% of subjects, in descending order, included pruritus, erythema, and burning. Reactions occurring in greater than 1 to less than 10% of subjects, in descending order, included irritation, desquamation, stinging, contact dermatitis, dermatitis, eczema, worsening of psoriasis, skin pain, rash, hypertriglyceridemia, dry skin, skin inflammation, and peripheral edema.
Tazarotene cream, 0.1% was associated with a greater degree of local irritation than the 0.05% cream. The rates of irritation adverse reactions reported during psoriasis trials with tazarotene cream, 0.1% were 0.1 to 0.4% higher than those reported for tazarotene cream, 0.05%.
Acne
The most frequent adverse reactions reported during clinical trials with tazarotene cream 0.1% in the treatment of acne, occurring in 10 to 30% of subjects, in descending order included desquamation, dry skin, erythema, and burning sensation. Reactions occurring in 1 to 5% of subjects included pruritus, irritation, face pain, and stinging.
Postmarketing Experience
The following adverse reactions have been identified during postapproval use of tazarotene. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Skin and subcutaneous tissue disorders: blister, dermatitis, urticaria, skin exfoliation, skin discoloration (including skin hyperpigmentation or skin hypopigmentation), swelling at or near application sites, and pain.
DRUG INTERACTIONS
No formal drug-drug interaction studies were conducted with tazarotene cream.
In a trial of 27 healthy female subjects between the ages of 20 to 55 years receiving a combination oral contraceptive tablet containing 1 mg norethindrone and 35 mcg ethinyl estradiol, concomitant use of tazarotene administered as 1.1 mg orally (mean ± SD C max and AUC 0-24 of tazarotenic acid were 28.9 ± 9.4 ng/mL and 120.6 ± 28.5 ng∙hr/mL) did not affect the pharmacokinetics of norethindrone and ethinyl estradiol over a complete cycle.
The impact of tazarotene on the pharmacokinetics of progestin only oral contraceptives (i.e., minipills) has not been evaluated.
DESCRIPTION
Tazarotene cream, 0.1% is for topical use and contains the active ingredient, tazarotene. Each gram of tazarotene cream, 0.1% contains 1 mg of tazarotene in a white cream base.
Tazarotene is a member of the acetylenic class of retinoids. Chemically, tazarotene is ethyl 6-[(4,4-dimethylthiochroman-6-yl)ethynyl]nicotinate. The compound has an empirical formula of C 21 H 21 NO 2 S and molecular weight of 351.46. The structural formula is shown below:
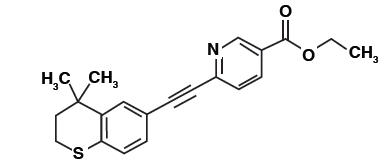
Tazarotene cream contains the following inactive ingredients: benzyl alcohol 1%, carbomer copolymer type B, carbomer homopolymer type B, edetate disodium, medium-chain triglycerides, mineral oil, purified water, sodium hydroxide (to adjust pH), sodium thiosulfate, and sorbitan monooleate.
CLINICAL PHARMACOLOGY
Mechanism of Action
Tazarotene is a retinoid prodrug which is converted to its active form, the carboxylic acid of tazarotene, by deesterification. Tazarotenic acid binds to all three members of the retinoic acid receptor (RAR) family: RARα, RARβ, and RARγ, but shows relative selectivity for RARβ, and RARγ and may modify gene expression. The clinical significance of these findings is unknown.
Pharmacokinetics
Following topical application, tazarotene undergoes esterase hydrolysis to form its active metabolite, tazarotenic acid. Little parent compound could be detected in the plasma. Tazarotenic acid was highly bound to plasma proteins (greater than 99%). Tazarotene and tazarotenic acid were metabolized to sulfoxides, sulfones and other polar metabolites which were eliminated through urinary and fecal pathways. The half-life of tazarotenic acid was approximately 18 hours, following topical application of tazarotene to normal, acne or psoriatic skin.
In a multiple dose trial with a once daily dose for 14 consecutive days in 9 psoriatic subjects (male=5; female=4), measured doses of tazarotene cream, 0.1% were applied by medical staff to involved skin without occlusion (5 to 35% of total body surface area: mean ± SD: 14 ± 11%). The C max of tazarotenic acid was 2.31 ± 2.78 ng/mL occurring 8 hours after the final dose, and the AUC 0-24h was 31.2 ± 35.2 ng∙hr/mL on day 15 in the five subjects who were administered clinical doses of 2 mg cream/cm 2 .
During clinical trials with tazarotene cream, 0.05% or 0.1% treatment for plaque psoriasis, three out of 139 subjects with their systemic exposure monitored had detectable plasma tazarotene concentrations, with the highest value at 0.09 ng/mL. Tazarotenic acid was detected in 78 out of 139 subjects (LLOQ = 0.05 ng/mL). Three subjects using tazarotene cream 0.1% had plasma tazarotenic acid concentrations greater than 1 ng/mL. The highest value was 2.4 ng/mL. However, because of the variations in the time of blood sampling, the area of psoriasis involvement, and the dose of tazarotene applied, actual maximal plasma levels are unknown.
Tazarotene cream 0.1% was applied once daily to either the face (N=8) or to 15% of body surface area (N=10) of female subjects with moderate to severe acne vulgaris. The mean C max and AUC values of tazarotenic acid peaked at day 15 for both dosing groups during a 29 day treatment period. Mean C max and AUC 0-24h values of tazarotenic acid from subjects in the 15% body surface area dosing group were more than 10 times higher than those from subjects in the face-only dosing group. The single highest C max throughout the trial period was 1.91 ng/mL on day 15 in the exaggerated dosing group. In the face-only group, the mean ± SD values of C max and AUC 0-24h of tazarotenic acid on day 15 were 0.10 ± 0.06 ng/mL and 1.54 ± 1.01 ng∙hr/mL, respectively, whereas in the 15% body surface area dosing group, the mean ± SD values of C max and AUC 0-24h of tazarotenic acid on day 15 were 1.20 ± 0.41 ng/mL and 17.01 ± 6.15 ng∙hr/mL, respectively. The steady state pharmacokinetics of tazarotenic acid had been reached by day 8 in the face-only and by day 15 in the 15% body surface area dosing groups.
In a Phase 3 clinical trial, tazarotene cream, 0.1% was applied once daily for 12 weeks to each of 48 subjects (22 females and 26 males) with facial acne vulgaris. The mean ± SD values of plasma tazarotenic acid at weeks 4 and 8 were 0.078 ± 0.073 ng/mL (N=47) and 0.052 ± 0.037 ng/mL (N=42), respectively. The highest observed individual plasma tazarotenic acid concentration was 0.41 ng/mL at week 4 from a female subject. The magnitude of plasma tazarotenic acid concentrations appears to be independent of gender, age, and body weight.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
A long-term study of tazarotene following oral administration of 0.025 mg/kg/day, 0.050 mg/kg/day, and 0.125 mg/kg/day to rats showed no indications of increased carcinogenic risks. Based on pharmacokinetic data from a shorter term study in rats, the highest dose of 0.125 mg/kg/day was anticipated to give systemic exposure in the rat equivalent to 0.6 times that seen in a psoriatic patient treated with 0.1% tazarotene cream at 2 mg/kg/cm 2 over a 35% body surface area in a controlled pharmacokinetic study. This estimated systemic exposure in rats was 2 times the maximum systemic exposure in acne patients treated with tazarotene cream, 0.1% cream at 2 mg/cm 2 over a 15% body surface area.
A long-term topical application study of up to 0.1% of tazarotene in a gel formulation in mice terminated at 88 weeks showed that dose levels of 0.05 mg/kg/day, 0.125 mg/kg/day, 0.25 mg/kg/day, and 1 mg/kg/day (reduced to 0.5 mg/kg/day for males after 41 weeks due to severe dermal irritation) revealed no apparent carcinogenic effects when compared to vehicle control animals. Systemic exposures at the highest dose was 3.9 times that seen in a psoriatic patient treated with 0.1% tazarotene cream at 2 mg/cm 2 over a 35% body surface area in a controlled pharmacokinetic study, and 13 times the maximum systemic exposure in acne patients treated with tazarotene cream, 0.1% at 2 mg/cm 2 over a 15% body surface area.
In evaluation of photo co-carcinogenicity, median time to onset of tumors was decreased, and the number of tumors increased in hairless mice following chronic topical dosing with intercurrent exposure to ultraviolet radiation at tazarotene concentrations of 0.001%, 0.005%, and 0.01% in a gel formulation for up to 40 weeks.
Mutagenesis
Tazarotene was found to be non-mutagenic in the Ames assay and did not produce structural chromosomal aberrations in a human lymphocyte assay. Tazarotene was non-mutagenic in the CHO/HGPRT mammalian cell forward gene mutation assay and was non-clastogenic in the in vivo mouse micronucleus test.
Impairment of Fertility
No impairment of fertility occurred in rats when male animals were treated for 70 days prior to mating and female animals were treated for 14 days prior to mating and continuing through gestation and lactation with topical doses of tazarotene gel up to 0.125 mg/kg/day. Based on data from another study, the systemic drug exposure in the rat would be equivalent to 0.6 times that observed in a psoriatic patient treated with 0.1% tazarotene cream at 2 mg/cm 2 over a 35% body surface area in a controlled pharmacokinetic study, and 2 times the maximum systemic exposure in acne patients treated with tazarotene cream, 0.1% at 2 mg/cm 2 over a 15% body surface area.
No impairment of mating performance or fertility was observed in male rats treated for 70 days prior to mating with oral doses of up to 1 mg/kg/day tazarotene. That dose produced a systemic exposure that was 1.9 times that observed in a psoriatic patient treated with 0.1% tazarotene cream at 2 mg/cm 2 over a 35% body surface area, and 6.3 times the maximum systemic exposure in acne patients treated with tazarotene cream, 0.1% at 2 mg/cm 2 over a 15% body surface area.
No impairment of mating performance or fertility was observed in female rats treated for 15 days prior to mating and continuing through gestation day 7 with oral doses up to 2 mg/kg/day of tazarotene. However, there was a significant decrease in the number of estrous stages and an increase in developmental effects at that dose [see Use in Specific Populations (8.1) ] . That dose produced a systemic exposure that was 3.4 times that observed in a psoriatic patient treated with 0.1% tazarotene cream at 2 mg/cm 2 over a 35% body surface area and 11 times the maximum systemic exposure in acne patients treated with tazarotene cream, 0.1% at 2 mg/cm 2 over a 15% body surface area.
Reproductive capabilities of F1 animals, including F2 survival and development, were not affected by topical administration of tazarotene gel to female F0 parental rats from gestation day 16 through lactation day 20 at the maximum tolerated dose of 0.125 mg/kg/day. Based on data from another study, the systemic drug exposure in the rat would be equivalent to 0.6 times that observed in a psoriatic patient treated with 0.1% tazarotene cream at 2 mg/cm 2 over a 35% body surface area, and 2 times the maximum systemic exposure in acne patients treated with tazarotene cream, 0.1% at 2 mg/cm 2 over a 15% body surface area.
CLINICAL STUDIES
In two 12-week vehicle-controlled clinical trials, tazarotene cream, 0.05% and 0.1% was significantly more effective than vehicle in reducing the severity of stable plaque psoriasis. Tazarotene cream, 0.1% and 0.05% demonstrated superiority over vehicle cream as early as 1 week and 2 weeks, respectively, after starting treatment.
In these trials, the primary efficacy endpoint was "clinical success," defined as the proportion of subjects with none, minimal, or mild overall lesional assessment at Week 12, and shown in Table 1. "Clinical success" was also significantly greater with tazarotene cream, 0.05% and 0.1% versus vehicle at most follow-up visits.
| Tazarotene Cream, 0.05% | Tazarotene Cream, 0.1% | Vehicle Cream | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Trial 1 N=218 | Trial 2 N=210 | Trial 1 N=221 | Trial 2 N=211 | Trial 1 N=229 | Trial 2 N=214 | ||||||||||
| Score | BL | Wk 12 | Wk 24 | BL | Wk 12 | BL | Wk 12 | Wk 24 | BL | Wk 12 | BL | Wk 12 | Wk 24 | BL | Wk 12 |
| |||||||||||||||
| None (0) | 0 | 1 (0.5%) | 1 (0.5%) | 0 | 2 (1%) | 0 | 0 | 0 | 0 | 6 (3%) | 0 | 0 | 1 (0.4%) | 0 | 1 (0.5%) |
| Minimal (1) | 0 | 11 (5%) | 12 (6%) | 0 | 7 (3%) | 0 | 12 (5%) | 14 (6%) | 0 | 11 (5%) | 0 | 7 (3%) | 6 (3%) | 0 | 1 (0.5%) |
| Mild (2) | 0 | 79 (36%) | 60 (28%) | 0 | 76 (36%) | 0 | 75 (34%) | 53 (24%) | 0 | 90 (43%) | 0 | 49 (21%) | 43 (19%) | 0 | 54 (25%) |
| Moderate (3) | 141 (65%) | 86 (39%) | 90 (41%) | 100 (48%) | 74 (35%) | 122 (55%) | 97 (44%) | 107 (48%) | 96 (45%) | 62 (29%) | 139 (61%) | 119 (52%) | 114 (50%) | 97 (45%) | 99 (46%) |
| Severe (4) | 69 (32%) | 39 (18%) | 51 (23%) | 80 (38%) | 36 (17%) | 91 (41%) | 36 (16%) | 46 (21%) | 86 (41%) | 29 (14%) | 81 (35%) | 51 (22%) | 61 (27%) | 93 (44%) | 47 (22%) |
| Very Severe (5) | 8 (4%) | 2 (0.9%) | 4 (2%) | 30 (14%) | 15 (7%) | 8 (4%) | 1 (0.5%) | 1 (0.5%) | 29 (14%) | 13 (6%) | 9 (4%) | 3 (1%) | 4 (2%) | 24 (11%) | 12 (6%) |
| "Clinical Success" | 0 | 91 (42% Denotes statistically significant difference for "Clinical Success" compared with vehicle. ) | 73 (33%) | 0 | 85 (40%) | 0 | 87 (39%) | 67 (30%) | 0 | 107 (51%) | 0 | 56 (24%) | 50 (22%) | 0 | 56 (26%) |
At the end of 12 weeks of treatment, tazarotene cream, 0.05% and 0.1% was consistently superior to vehicle in reducing the plaque thickness of psoriasis. Improvements in erythema and scaling were generally significantly greater with tazarotene cream, 0.05% and 0.1% than with vehicle. Tazarotene Cream, 0.1% was also generally more effective than tazarotene cream, 0.05% in reducing the severity of the individual signs of disease. However, tazarotene cream, 0.1% was associated with a greater degree of local irritation than tazarotene cream, 0.05%.
| Tazarotene Cream, 0.05% | Tazarotene Cream, 0.1% | Vehicle Cream | |||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Lesion | Trunk/Arm/Leg lesions | Knee/Elbow lesions | All Treated | Trunk/Arm/Leg lesions | Knee/Elbow lesions | All Treated | Trunk/Arm/Leg lesions | Knee/Elbow lesions | All Treated | ||||||||||
| Trial 1 | Trial 2 | Trial 1 | Trial 2 | Trial 1 | Trial 2 | Trial 1 | Trial 2 | Trial 1 | Trial 2 | Trial 1 | Trial 2 | Trial 1 | Trial 2 | Trial 1 | Trial 2 | Trial 1 | Trial 2 | ||
| N=218 | N=210 | N=218 | N=210 | N=218 | N=210 | N=221 | N=211 | N=221 | N=211 | N=221 | N=211 | N=229 | N=214 | N=229 | N=214 | N=229 | N=214 | ||
| Plaque elevation, scaling and erythema scored on a 0-4 scale with 0=none, 1=mild, 2=moderate, 3=severe and 4=very severe. | |||||||||||||||||||
| B#=Mean Baseline Severity; | |||||||||||||||||||
| C-12=Mean Change from Baseline at end of 12 weeks of therapy; | |||||||||||||||||||
| C-24=Mean Change from Baseline at week 24 (12 weeks after the end of therapy). | |||||||||||||||||||
| Plaque elevation | B# | 2.29 | 2.50 | 2.40 | 2.52 | 2.28 | 2.51 | 2.34 | 2.52 | 2.35 | 2.49 | 2.32 | 2.51 | 2.28 | 2.51 | 2.35 | 2.51 | 2.29 | 2.51 |
| C-12 | -0.83 Denotes statistically significant difference compared with vehicle. | -0.98 | -0.91 | -1.04 | -0.75 | -0.90 | -1.08 | -1.25 | -0.96 | -1.21 | -0.83 | -1.08 | -0.59 | -0.69 | -0.57 | -0.68 | -0.48 | -0.61 | |
| C-24 | -0.75 | -0.73 | -0.60 | -0.87 | -0.73 | -0.63 | -0.57 | -0.49 | -0.42 | ||||||||||
| Scaling | B# | 2.26 | 2.45 | 2.47 | 2.60 | 2.32 | 2.47 | 2.37 | 2.45 | 2.40 | 2.57 | 2.36 | 2.53 | 2.34 | 2.46 | 2.45 | 2.61 | 2.31 | 2.53 |
| C-12 | -0.75 | -0.90 | -0.78 | -0.98 | -0.67 | -0.80 | -0.84 | -1.06 | -0.76 | -1.13 | -0.73 | -1.03 | -0.66 | -0.79 | -0.62 | -0.76 | -0.46 | -0.70 | |
| C-24 | -0.68 | -0.62 | -0.51 | -0.79 | -0.61 | -0.59 | -0.56 | -0.45 | -0.34 | ||||||||||
| Erythema | B# | 2.26 | 2.51 | 2.17 | 2.40 | 2.23 | 2.48 | 2.25 | 2.53 | 2.17 | 2.42 | 2.21 | 2.51 | 2.24 | 2.47 | 2.17 | 2.34 | 2.24 | 2.47 |
| C-12 | -0.49 | -0.65 | -0.44 | -0.66 | -0.40 | -0.62 | -0.49 | -0.82 | -0.57 | -0.82 | -0.42 | -0.78 | -0.42 | -0.46 | -0.38 | -0.44 | -0.37 | -0.47 | |
| C-24 | -0.52 | -0.44 | -0.41 | -0.55 | -0.52 | -0.39 | -0.43 | -0.34 | -0.33 | ||||||||||
Acne:
In two large vehicle-controlled trials, subjects age 12 years and over with facial acne vulgaris of a severity suitable for monotherapy with a topical agent were enrolled. After face cleansing in the evening, tazarotene cream, 0.1% was applied once daily to the entire face as a thin layer. Tazarotene cream, 0.1% was significantly more effective than vehicle in the treatment of facial acne vulgaris. Efficacy results after 12 weeks of treatment are shown in Table 3:
| Tazarotene Cream, 0.1% | Vehicle Cream | |||
|---|---|---|---|---|
| Trial 1 N=218 | Trial 2 N=206 | Trial 1 N=218 | Trial 2 N=205 | |
| Median Percent Reduction in | ||||
| 46% Denotes statistically significant difference compared with vehicle. 41% 44% | 41% 44% 42% | 27% 27% 24% | 21% 25% 21% |
| Percent of Subjects with No Acne or Minimal Acne | 18% | 20% | 11% | 6% |
| Percent of Subjects with No Acne, or Minimal Acne, or Mild Acne | 55% | 53% | 36% | 36% |
HOW SUPPLIED/STORAGE AND HANDLING
Tazarotene cream is a white cream available in a concentration of 0.1%. It is supplied in a collapsible aluminum tube with a tamper-evident aluminum membrane over the opening and a white polypropylene screw cap, in 30 g and 60 g sizes.
Tazarotene Cream, 0.1%
30 gram NDC 51672-1373-2
60 gram NDC 51672-1373-3
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature].
Mechanism of Action
Tazarotene is a retinoid prodrug which is converted to its active form, the carboxylic acid of tazarotene, by deesterification. Tazarotenic acid binds to all three members of the retinoic acid receptor (RAR) family: RARα, RARβ, and RARγ, but shows relative selectivity for RARβ, and RARγ and may modify gene expression. The clinical significance of these findings is unknown.