Triamterene And Hydrochlorothiazide - Triamterene And Hydrochlorothiazide tablet prescribing information
INDICATIONS AND USAGE
This fixed combination drug is not indicated for the initial therapy of edema or hypertension except in individuals in whom the development of hypokalemia cannot be risked.
- Triamterene and hydrochlorothiazide tablets are indicated for the treatment of hypertension or edema in patients who develop hypokalemia on hydrochlorothiazide alone.
- Triamterene and hydrochlorothiazide is also indicated for those patients who require a thiazide diuretic and in whom the development of hypokalemia cannot be risked (e.g., patients on concomitant digitalis preparations, or with a history of cardiac arryhthmias, etc.).
Triamterene and hydrochlorothiazide may be used alone or in combination with other antihypertensive drugs, such as beta-blockers. Since triamterene and hydrochlorothiazide may enhance the actions of these drugs, dosage adjustments may be necessary.
Usage in Pregnancy
The routine use of diuretics in an otherwise healthy woman is inappropriate and exposes mother and fetus to unnecessary hazard. Diuretics do not prevent development of toxemia of pregnancy, and there is no satisfactory evidence that they are useful in the treatment of developed toxemia.
Edema during pregnancy may arise from pathological causes or from the physiologic and mechanical consequences of pregnancy. Thiazides are indicated in pregnancy when edema is due to pathologic causes, just as they are in the absence of pregnancy. Dependent edema in pregnancy, resulting from restriction of venous return by the expanded uterus, is properly treated through elevation of the lower extremities and use of support hose; use of diuretics to lower intravascular volume in this case is illogical and unnecessary. There is hypervolemia during normal pregnancy which is harmful to neither the fetus nor the mother (in the absence of cardiovascular disease), but which is associated with edema, including generalized edema, in the majority of pregnant women. If this edema produces discomfort, increased recumbency will often provide relief. In rare instances, this edema may cause extreme discomfort which is not relieved by rest. In these cases, a short course of diuretics may provide relief and may be appropriate.
DOSAGE AND ADMINISTRATION
Note: 37.5 mg/25 mg = 37.5 mg triamterene and 25 mg hydrochlorothiazide
75 mg/50 mg = 75 mg triamterene and 50 mg hydrochlorothiazide
The usual dose of Triamterene and Hydrochlorothiazide 37.5 mg/25 mg is one or two tablets daily, given as a single dose, with appropriate monitoring of serum potassium (see WARNINGS ). The usual dose of Triamterene and Hydrochlorothiazide 75 mg/50 mg is one tablet daily, with appropriate monitoring of serum potassium (see WARNINGS ). There is no experience with the use of more than one 75 mg/50 mg tablet daily or more than two 37.5 mg/25 mg tablets daily. Clinical experience with the administration of two 37.5 mg/25 mg tablets daily in divided doses (rather than as a single dose) suggests an increased risk of electrolyte imbalance and renal dysfunction.
Patients receiving 50 mg of hydrochlorothiazide who become hypokalemic may be transferred to 75 mg/50 mg product directly. Patients receiving 25 mg hydrochlorothiazide who become hypokalemic may be transferred to a 37.5 mg triamterene/25 mg hydrochlorothiazide directly.
In patients requiring hydrochlorothiazide therapy and in whom hypokalemia cannot be risked, therapy may be initiated with 37.5 mg/25 mg of triamterene and hydrochlorothiazide. If an optimal blood pressure response is not obtained with 37.5 mg/25 mg of triamterene and hydrochlorothiazide, the dose should be increased to two 37.5 mg/25 mg tablets daily as a single dose, or one 75 mg/50 mg tablet daily. If blood pressure still is not controlled, another antihypertensive agent may be added (see PRECAUTIONS, Drug Interactions ).
Clinical studies have shown that patients taking less bioavailable formulations of triamterene and hydrochlorothiazide in daily doses of 25 mg to 50 mg hydrochlorothiazide and 50 mg to 100 mg triamterene may be safely changed to one 37.5 mg/25 mg of triamterene and hydrochlorothiazide daily. All patients changed from less bioavailable formulations to triamterene and hydrochlorothiazide should be monitored clinically and for serum potassium after the transfer.
CONTRAINDICATIONS
Hyperkalemia
Triamterene and hydrochlorothiazide should not be used in the presence of elevated serum potassium levels (greater than or equal to 5.5 mEq/liter). If hyperkalemia develops, this drug should be discontinued and a thiazide alone should be substituted.
Antikaliuretic Therapy or Potassium Supplementation
Triamterene and hydrochlorothiazide should not be given to patients receiving other potassium-conserving agents such as spironolactone, amiloride hydrochloride or other formulations containing triamterene. Concomitant potassium supplementation in the form of medication, potassium-containing salt substitute or potassium-enriched diets should also not be used.
Impaired Renal Function
Triamterene and hydrochlorothiazide is contraindicated in patients with anuria, acute and chronic renal insufficiency or significant renal impairment.
Hypersensitivity
Triamterene and hydrochlorothiazide should not be used in patients who are hypersensitive to triamterene or hydrochlorothiazide or other sulfonamide-derived drugs.
ADVERSE REACTIONS
Side effects observed in association with the use of triamterene and hydrochlorothiazide tablets, other combination products containing triamterene/hydrochlorothiazide, and products containing triamterene or hydrochlorothiazide include the following:
Gastrointestinal: jaundice (intrahepatic cholestatic jaundice), pancreatitis, nausea, appetite disturbance, taste alteration, vomiting, diarrhea, constipation, anorexia, gastric irritation, cramping.
Central Nervous System: drowsiness and fatigue, insomnia, headache, dizziness, dry mouth, depression, anxiety, vertigo, restlessness, paresthesias.
Cardiovascular: tachycardia, shortness of breath and chest pain, orthostatic hypotension (may be aggravated by alcohol, barbiturates or narcotics).
Renal: acute renal failure, acute interstitial nephritis, renal stones composed of triamterene in association with other calculus materials, urine discoloration.
Hematologic: leukopenia, agranulocytosis, thrombocytopenia, aplastic anemia, hemolytic anemia and megaloblastosis.
Ophthalmic: xanthopsia, transient blurred vision.
Hypersensitivity: anaphylaxis, photosensitivity, rash, urticaria, purpura, necrotizing angiitis (vasculitis, cutaneous vasculitis), fever, respiratory distress including pneumonitis.
Other: muscle cramps and weakness, decreased sexual performance and sialadenitis.
Whenever adverse reactions are moderate to severe, therapy should be reduced or withdrawn.
Altered Laboratory Findings
Serum Electrolytes: hyperkalemia, hypokalemia, hyponatremia, hypomagnesemia, hypochloremia (see WARNINGS and PRECAUTIONS ).
Creatinine, Blood Urea Nitrogen: Reversible elevations in BUN and serum creatinine have been observed in hypertensive patients treated with triamterene and hydrochlorothiazide.
Glucose: hyperglycemia, glycosuria and diabetes mellitus (see PRECAUTIONS ).
Serum Uric Acid, PBI and Calcium: (see PRECAUTIONS ).
Other: Elevated liver enzymes have been reported in patients receiving triamterene and hydrochlorothiazide.
Postmarketing Experience
Non-melanoma Skin Cancer
Hydrochlorothiazide is associated with an increased risk of non-melanoma skin cancer. In a study conducted in the Sentinel System, increased risk was predominantly for squamous cell carcinoma (SCC) and in white patients taking large cumulative doses. The increased risk for SCC in the overall population was approximately 1 additional case per 16,000 patients per year, and for white patients taking a cumulative dose of ≥ 50,000 mg the risk increase was approximately 1 additional SCC case for every 6,700 patients per year.
Drug Interactions
Thiazides may add to or potentiate the action of other antihypertensive drugs.
The thiazides may decrease arterial responsiveness to norepinephrine. This diminution is not sufficient to preclude effectiveness of the pressor agent for therapeutic use. Thiazides have also been shown to increase the responsiveness to tubocurarine.
Lithium generally should not be given with diuretics because they reduce its renal clearance and add a high risk of lithium toxicity. Refer to the package insert on lithium before use of such concomitant therapy.
Acute renal failure has been reported in a few patients receiving indomethacin and formulations containing triamterene and hydrochlorothiazide. Caution is therefore advised when administering non-steroidal anti-inflammatory agents with triamterene and hydrochlorothiazide.
Potassium-sparing agents should be used very cautiously, if at all, in conjunction with angiotensin-converting enzyme (ACE) inhibitors due to a greatly increased risk of hyperkalemia. Serum potassium should be monitored frequently.
Rx Only DESCRIPTION
Triamterene and hydrochlorothiazide combines triamterene, a potassium-conserving diuretic, with the natriuretic agent, hydrochlorothiazide.
Each Triamterene and Hydrochlorothiazide 37.5 mg/25 mg Tablet, USP contains 37.5 mg of Triamterene, USP and 25 mg of Hydrochlorothiazide, USP.
Each Triamterene and Hydrochlorothiazide 75 mg/50 mg Tablet, USP contains 75 mg of Triamterene, USP and 50 mg of Hydrochlorothiazide, USP.
Triamterene and hydrochlorothiazide tablets for oral administration contains the following inactive ingredients: lactose monohydrate, magnesium stearate, microcrystalline cellulose, and sodium starch glycolate. In addition, the 37.5 mg/25 mg tablets contain D&C Yellow No.10 Aluminum Lake and FD&C Blue No.1 Aluminum Lake.
Triamterene is 2,4,7-triamino-6-phenylpteridine. Triamterene is practically insoluble in water, benzene, chloroform, ether and dilute alkali hydroxides. It is soluble in formic acid and sparingly soluble in methoxyethanol. Triamterene is very slightly soluble in acetic acid, alcohol and dilute mineral acids. The following is the structural formula:
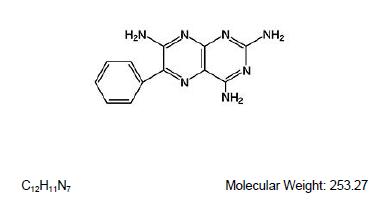
Hydrochlorothiazide is 6-chloro-3,4-dihydro-2H -1,2,4, benzothiadiazine-7-sulfonamide 1,1-dioxide. Hydrochlorothiazide is slightly soluble in water and freely soluble in sodium hydroxide solution, n-butylamine and dimethylformamide. It is sparingly soluble in methanol and insoluble in ether, chloroform and dilute mineral acids. Its molecular weight is 297.73. The following is the structural formula:
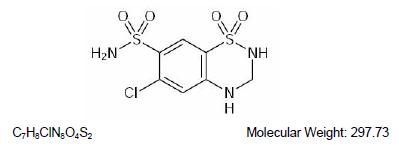
CLINICAL PHARMACOLOGY
Triamterene and hydrochlorothiazide is a diuretic, antihypertensive drug product, principally due to its hydrochlorothiazide component; the triamterene component reduces the excessive potassium loss which may occur with hydrochlorothiazide use.
Hydrochlorothiazide
Hydrochlorothiazide is a diuretic and antihypertensive agent. It blocks the renal tubular absorption of sodium and chloride ions. This natriuresis and diuresis is accompanied by a secondary loss of potassium and bicarbonate. Onset of hydrochlorothiazide's diuretic effect occurs within 2 hours and the peak action takes place in 4 hours. Diuretic activity persists for approximately 6 to 12 hours.
The exact mechanism of hydrochlorothiazide's antihypertensive action is not known although it may relate to the excretion and redistribution of body sodium. Hydrochlorothiazide does not affect normal blood pressure.
Following oral administration, peak hydrochlorothiazide plasma levels are attained in approximately 2 hours. It is excreted rapidly and unchanged in the urine.
Well controlled studies have demonstrated that doses of hydrochlorothiazide as low as 25 mg given once daily are effective in treating hypertension, but the dose-response has not been clearly established.
Triamterene
Triamterene is a potassium-conserving (antikaliuretic) diuretic with relatively weak natriuretic properties. It exerts its diuretic effect on the distal renal tubule to inhibit the reabsorption of sodium in exchange for potassium and hydrogen. With this action, triamterene increases sodium excretion and reduces the excessive loss of potassium and hydrogen associated with hydrochlorothiazide. Triamterene is not a competitive antagonist of the mineralocorticoids and its potassium-conserving effect is observed in patients with Addison's disease, i.e., without aldosterone. Triamterene's onset and duration of activity is similar to hydrochlorothiazide. No predictable antihypertensive effect has been demonstrated with triamterene.
Triamterene is rapidly absorbed following oral administration. Peak plasma levels are achieved within one hour after dosing. Triamterene is primarily metabolized to the sulfate conjugate of hydroxytriamterene. Both the plasma and urine levels of this metabolite greatly exceed triamterene levels.
The amount of triamterene added to 50 mg of hydrochlorothiazide in triamterene and hydrochlorothiazide tablets was determined from steady-state dose-response evaluations in which various doses of liquid preparations of triamterene were administered to hypertensive persons who developed hypokalemia with hydrochlorothiazide (50 mg given once daily). Single daily doses of 75 mg triamterene resulted in greater increases in serum potassium than lower doses (25 mg and 50 mg), while doses greater than 75 mg of triamterene resulted in no additional elevations in serum potassium levels. The amount of triamterene added to the 25 mg of hydrochlorothiazide in triamterene and hydrochlorothiazide tablets was also determined from steady-state dose-response evaluations in which various doses of liquid preparations of triamterene were administered to hypertensive persons who developed hypokalemia with hydrochlorothiazide (25 mg given once daily). Single daily doses of 37.5 mg triamterene resulted in greater increases in serum potassium than a lower dose (25 mg), while doses greater than 37.5 mg of triamterene, i.e., 75 mg and 100 mg, resulted in no additional elevations in serum potassium levels. The dose-response relationship of triamterene was also evaluated in patients rendered hypokalemic by hydrochlorothiazide given 25 mg twice daily. Triamterene given twice daily increased serum potassium levels in a dose-related fashion. However, the combination of triamterene and hydrochlorothiazide given twice daily also appeared to produce an increased frequency of elevation in serum BUN and creatinine levels. The largest increases in serum potassium, BUN and creatinine in this study were observed with 50 mg of triamterene given twice daily, the largest dose tested. Ordinarily, triamterene does not entirely compensate for the kaliuretic effect of hydrochlorothiazide and some patients may remain hypokalemic while receiving triamterene and hydrochlorothiazide. In some individuals, however, it may induce hyperkalemia (see WARNINGS ).
The triamterene and hydrochlorothiazide components of this product are well absorbed and are bioequivalent to liquid preparations of the individual components administered orally. Food does not influence the absorption of triamterene or hydrochlorothiazide from BluePoint’s triamterene and hydrochlorothiazide 37.5 mg/25 mg or 75 mg/50 mg tablets. The hydrochlorothiazide component of triamterene and hydrochlorothiazide tablets is bioequivalent to single entity hydrochlorothiazide tablet formulations.
HOW SUPPLIED
Triamterene and Hydrochlorothiazide Tablets, USP, 37.5 mg/ 25 mg are available for oral administration as green, oval bioconvex tablets, scored and engraved “37.5” bisect “25” on one side, “APO” on the other side. They are supplied as follows:
NDC 68001-327-00 bottles of 100
NDC 68001-327-03 bottles of 500
Triamterene and Hydrochlorothiazide Tablets, USP, 75 mg/50 mg are available for oral administration as yellow, oval bioconvex tablets, scored and engraved “75” bisect “50” on one side, “APO” on the other side. They are supplied as follows:
NDC 68001-328-00 bottles of 100
NDC 68001-328-03 bottles of 500
Dispense with a child-resistant closure in a tight, light-resistant container.
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature].
Protect from light.
TRIAMTERENE HYDROCHLOROTHIAZIDE TABLETS, USP
37.5 mg/25 mg and 75 mg/50 mg
Manufactured by:
Piramal Pharma Limited,
Plot No. 67-70, Sector - 2,
Pithampur 454775, Dist. Dhar, Madhya Pradesh, INDIA Mfg Lic. No.: 25/10/92
For BluePoint Laboratories
Revised 02/2025
Rev. 3a